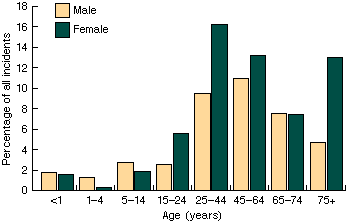Analysing potential harm in Australian general practice: an incident-monitoring study
Alice L Bhasale, Graeme C Miller, Sharon E Reid and Helena C Britt
MJA 1998; 169: 73-76
For editorial comment, see Kidd & Veale
Abstract -
Introduction -
Method -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
©MJA1998
Abstract |
Objective: To collect data on incidents of potential
or actual harm to general practice patients and to evaluate the
possible causes of these incidents. Design: An observational study of incidents of potential harm based on a modified critical incidents technique. A non-random sample of general practitioners (GPs) anonymously submitted incident reports contemporaneously. Setting and participants: Australian general practices between October 1993 and June 1995. During the study period, 324 GPs participated at some time. Main outcome measures: GP-reported free-text descriptions of incidents and structured responses for preventability, potential for harm, immediate consequences, predicted long-term outcomes, type of incident, contributing factors, mitigating factors, and additional resource use. Results: 805 incidents were reported -- 76% were preventable; 27% had potential for severe harm. No long term harm was predicted for 66% of incidents. Incidents could relate to pharmacological management (51 per 100 incidents), non-pharmacological management (42 per 100 incidents), diagnosis (34 per 100 incidents) or equipment (5 per 100 incidents). The most common contributory factors were poor communication between patients and healthcare professionals and actions of others (23 per 100 incidents each) and errors in judgement (22 per 100 incidents). Conclusion: Human errors and preventable system problems were identified. The incident monitoring technique provided useful data which could be applied to incident prevention strategies. |
Introduction |
Increased interest in quality improvement in healthcare has led to
greater recognition that errors occur. The Harvard Medical
Practice Study1,2 and the
Quality in Australian Health Care Study3 retrospectively reviewed hospital
medical records to identify and quantify adverse events caused by the
hospital care provided. These studies have provided important
insight into rates of adverse outcomes. In Australia, around 16% of
admissions studied were associated with an adverse event.3 Following the success of incident monitoring in anaesthetics,4,5 in 1993 the Commonwealth Review of Professional Indemnity Arrangements for Health Care Professionals initiated pilot incident-monitoring studies in six medical specialties. The aim of this study was to test the incident-monitoring method in general practice. An important difference between studies such as the Harvard Medical Practice Study and incident-monitoring studies is that no claims of generalisability are made in the latter. Incident monitoring cannot estimate prevalence. It provides detailed contextual information about specific processes and situations that can lead to adverse patient outcomes. Such information is then used to make specific recommendations. The objectives of this study were to test a mechanism for obtaining incident reports from GPs; to gain an understanding of the type of incidents occurring in general practice and hence areas of potential harm; and to identify areas which might benefit from intervention. |
Method |
The method has been described in detail elsewhere.6 Participating general
practitioners reported incidents contemporaneously, on
purpose-designed reporting forms. An incident was broadly defined
as "an unintended event, no matter how seemingly trivial or
commonplace, that could have harmed or did harm a patient". This
criterion included "near misses" -- where the harm may have been
averted, but the potential for harm existed.
All GP members of the Australian Sentinel Practice Research Network and the Central, Southern, Western and Wentworth Area Health Sentinel Networks in Sydney were asked by letter to participate. Others volunteered when reporting was offered as a Quality Assurance option through the Royal Australian College of General Practitioners (RACGP). Reports were anonymous and information was protected from subpoena by the Health Insurance Act 1973 (Cwlth).7 The reporting form included both free text and fixed-response questions. Information requested included GP characteristics and the patient's age, sex and health problems associated with the incident. Free text descriptions were elicited of the incident, its consequences, and contributing and mitigating factors; the outcome; and the GP's opinion of the incident's preventability. Fixed-choice responses included the type of incident, contributing factors, mitigating factors, potential for harm, immediate consequences, and predicted long term outcomes. All fixed-choice questions included an "other" category to allow continuing development of categories. Quantitative descriptive analysis was used to describe the main features of the data for all 805 incidents received, using SAS.8 No significance testing was carried out as it would have been invalid because of the nature of the study and sample. Qualitative analysis of textual data was carried out for 500 incidents. This analysis involved examination of groups of events for common causes, situations and contributing factors. |
Results | |
GP response |
Of 510 GPs initially approached, 214 accepted. A further 110 GPs
volunteered during the study. Between October 1993 and June 1995, 805
reports were received from 324 enrolled participants. As all reports
were anonymous, reporting rates could not be calculated. However, a
GP-generated personal identification number on most reports
allowed estimation of the number of reports received from each
identification number. There were 241 GPs who submitted at least one
report, and 82 unidentified reports.
The proportion of each sex and the proportion from rural practices among the respondents were equivalent to the overall GP population at that time.9 However, only 16% of respondents had less than 10 years' experience, whereas in a national sample in 1990-1991 about 30% of GPs had less than 10 years' experience.10 |
Patients |
Of the 805 incidents, 58% involved female patients. Almost one-third
of incidents involved patients over 65 years old (median age, 50
years; range, 0-98 years). Younger patients (0-24 years) were least
likely to be involved in incidents (Figure). Compared with the overall age-sex distribution of patients attending GP consultations, women older than 75 years and infants
were over-represented in the incidents reported.9
|
Incidents |
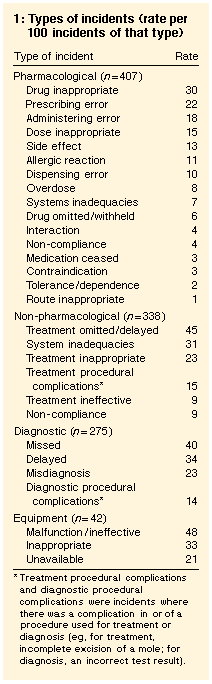
Incidents were categorised as pharmacological,
non-pharmacological, diagnostic or equipment events (Box 1).
Pharmacological events were most frequent. The most common incident
type overall was omitted or delayed treatment. A high degree of
overlap between non-pharmacological and diagnostic events was
noted -- 79 incidents involved both types.
GPs thought 76% of the incidents were preventable (Box 2) and 11% were unpreventable. They were undecided about the remaining 13%. More than one-third of the incidents resulted in additional use of resources. While pharmacological incidents were most often reported, they were also largely considered preventable (79%) and the least harmful potentially and in the long term. In contrast, diagnostic events were less preventable and more harmful (Box 2). Of the 38 deaths reported, 30 involved a diagnostic incident. |
 |
|
| Major immediate consequences were reported in 17% of incidents, and 4% resulted in the patient's death (Box 2). GPs predicted that most incidents would cause no long term harm, but that 7% would result in the future death of the patient. | |
Mitigating and contributing factors |
Incident outcomes were more frequently mitigated by chance factors
than through systematised fail-safe or preventive procedures. The
most frequently reported mitigating factors were good fortune,
early intervention by the GP, and the patient's good physical
condition (Box 3).
Ineffective communication and problems in coordination between healthcare services were frequent contributing factors (Box 4). Actions or involvement of others in caring for patients were also frequently cited. Assessment-related mistakes constituted another cluster of contributing factors (eg, errors in judgement, failure to recognise significant signs and symptoms, and inadequate patient assessment). Insufficient use of standard resources and protocols by the GP was also recognised. GPs reported being tired, rushed or late in 10% of incidents, but GP memory lapses and stressful situations were least frequently cited as contributing factors.
There were no obvious associations between specific contributing factors and incident type. |
Qualitative analysis |
Qualitative analysis of free-text responses identified four broad
problem groups: communication, procedural, clinical and external
problems. More comprehensive descriptions are available
elsewhere.11,12 Communication problems: Most communication problems between GPs and patients occurred when patients did not understand some aspect of their condition, the management plan or the treatment. Patients with mental health problems or lacking English language skills were particularly at risk. Some serious pharmacological incidents occurred when patients misunderstood instructions and took newly prescribed drugs in addition to, rather than instead of, a previously prescribed medication. Poor communication also manifested as clinical error in inadequate history taking. There were also problems with communication between healthcare providers. Clinical information about the outcomes of hospital referrals or admissions, the expected role of the GP in post-discharge care, specialists' recommendations for management and results of tests or investigations was often not communicated between GPs and other healthcare providers, or was too late to be of use. Unclear or uninformative medical records caused a number of incidents, and inadequate records resulted in poor communication within practices. Incorrect or unclear labelling of drugs resulted in administration of the wrong drug, and inappropriate drugs were dispensed because of poor handwriting on prescription forms. Such errors were often compounded by similar medication names (eg, Teldane/Feldene, Microlax/ Murelax). Procedural problems: The main procedural error was failure to check medical records. Diagnostically, procedural error manifested in poor application of the differential diagnosis, when the correct diagnosis was inappropriately rejected because of insufficient or incorrect examination, or was not included in the differential diagnoses and was therefore not evaluated. In non-pharmacological incidents, treatment procedures may have been neglected (eg, not checking for anaesthesia before an excision). In equipment incidents, machines were not properly checked before use (eg, leads or tubes were disconnected) or were not well maintained (eg, unfilled emergency oxyviva equipment). Lack of protocols for ensuring action on results of tests and investigations meant that important results were filed unseen or left until the GP who ordered the test was next in the surgery. Recall systems were often inadequate, preventing recall of patients for follow-up tests and investigations and resulting in missed or delayed diagnosis or management. Clinical problems: These consisted of incidents that could only be attributed to human error. In pharmacological incidents, clinical errors occurred where an inappropriate drug was chosen; in non-pharmacological incidents, where the wrong treatment was chosen; in diagnostic incidents, where symptoms and signs were not recognised (eg, chest pain considered to be musculoskeletal); and in equipment incidents, where equipment was used inappropriately. External problems: External problems involved factors outside the GP's control, such as actions of other healthcare providers, equipment faults or unavailability, disease-related factors, and unpredictable drug effects. Patient-related factors included non-compliance, age, level of comprehension, and psychological condition. |
Discussion |
The diversity of incidents reflects the heterogeneous nature of
general practice and its context within the healthcare system.
Nevertheless, it was possible to isolate recurrent themes and errors
and to identify incidents that occurred because of system problems or
other preventable factors.
Pharmacological incidents were most frequent and could be prevented through clearer prescription writing, double-checking of doses and potential interactions, and improved patient understanding. Unexpected drug reactions (eg, to previously well-tolerated drugs) and idiosyncratic complications were largely beyond GPs' control. However, compilation of this information may be useful to reinforce or add to data collected elsewhere. Diagnostic incidents had the most serious outcomes. While management of test results and lack of recall systems contributed to these incidents, many occurred while the patient was under another medical practitioner's care, or were caused by the diagnostic decision-making processes of GPs. Patient misunderstanding was a factor in many incidents. This might be addressed by improved GP awareness to ensure full patient understanding. However, information management problems require "hard-wired" solutions -- structures and systems that ensure better outcomes. In particular, opportunities for errors may be reduced by better recall systems for follow-up and for regular tests and screening,13 better transfer of medical information between healthcare providers, clearer writing of prescriptions, and better maintenance and use of medical records. Information technology could help by streamlining some of the administrative functions, particularly prescription writing, which appears to be adversely affected when GPs are tired, rushed, or running late. Limitations to the validity of our data include the non-random nature of the sample, limited recognition of incidents, selectivity in reporting incidents, and the lack of an alternative perspective. (We did not seek the patients' perspective because of the controversial nature of the data.) However, issues we identified as important have been described by other researchers. Many of the issues pertaining to pharmacological incidents have been described in a study of adverse drug events in United States hospitals.14 Similarly, the problems of multiple prescribing in the elderly have been well summarised, and opportunities for improvement in the management of polypharmacy have been identified.15 Prescription clarity has also been recognised as an area of potential misunderstanding.16 In critical incident studies, incidents are sampled until "saturation" (until no new incident types are reported).17 While these 805 incidents may not reach saturation, they demonstrate at least some of the types of incidents occurring in Australian general practice. Logically, where inadequate systems are widely used, similar events are likely to occur regularly rather than being related to individual characteristics or techniques. Continued collection and classification of events will elucidate more causal factors, particularly for the less common types of incidents. This study also resulted in a number of suggested interventions.18 Incident monitoring studies are intended to be continually used in improving systems. It is important to use the data for formulating interventions. This study has shown that such data can be collected in general practice, but the translation of findings into active change remains to be addressed. |
Acknowledgements | We gratefully acknowledge the funding provided by the Commonwealth Review of Professional Indemnity Arrangements for Health Care Professionals. The project was conducted under the auspices of the RACGP. Recruitment of GPs and administration of the GP participants was carried out jointly by the Family Medicine Research Unit and the RACGP Research and Health Promotion Unit, South Australia. Other members of the research team made considerable contributions to running the project. Thanks must go to the GP participants for so generously sharing their experiences with us. |
References |
(Received 4 Aug 1997, accepted 26 Mar 1998) |
Authors' details
Department of General Practice, University of Sydney, Sydney, NSW.Alice L Bhasale, BSc(Psychol), MSc(Med), Senior Research Assistant, Family Medicine Research Unit;
Graeme C Miller, MB BS, FRACGP, Medical Director, Family Medicine Research Unit;
Sharon E Reid, MB BS, MPH, Lecturer;
Helena C Britt, PhD, Director, Family Medicine Research Unit.
Reprints will not be available from the authors.
Correspondence: Ms A
L Bhasale, Acacia House, Westmead Hospital, Westmead, NSW
2145.
E-mail: alicebATgenprac.wsahs.nsw.gov.au
-
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
Received 25 May 2026, accepted 25 May 2026
- Alice L Bhasale
- Graeme C Miller
- Sharon E Reid
- Helena C Britt