Reducing indigenous mortality in Australia: lessons from other countries
Ian T Ring and David Firman
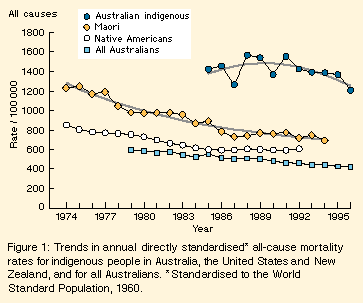
Mortality rates from all causes in Maori in New Zealand and Native Americans have fallen substantially since the early 1970s. Comparable mortality rates for Australian Aboriginals and Torres Strait Islanders in 1990-1994 were at or above the rates observed 20 years ago in Maori and Native Americans, being 1.9 times the rate in Maori, 2.4 times the rate in Native Americans, and 3.2 times the rate for all Australians. Circulatory diseases, respiratory diseases, injuries and endocrine diseases (mostly diabetes) are responsible for almost 70% of these excess deaths. Mortality rate trends in indigenous populations in other countries suggest the feasibility of substantial and rapid reductions in mortality rates of Australia's indigenous people.
MJA 1998; 169: 528-533
For editorial comment, see Mooney et al
Introduction -
Methods -
Results -
Discussion -
References -
Authors' details
-
-
More articles on Aboriginal health -
©MJA1998
Introduction |
The poor health of Australian Aboriginals and Torres Strait
Islanders is well known. Since the 1970s, indigenous infant
mortality rates have been declining, but life expectancy has not
changed because of continued high adult mortality rates,1 due largely to
high death rates from chronic diseases in middle age.2 This pattern
contrasts with that of the indigenous people of Canada, the United
States and New Zealand, where marked improvements in health have
occurred.3-5 While the health status of
Australians as a whole continues to improve, the all-cause death rate
for Aboriginal women is unchanged and the rate among men has decreased
only slightly.6 As a result, the gap between
the death rates for the Aboriginal population and the total
Australian population has widened.1,7 Relatively few causes
account for most of the mortality rate difference between indigenous
Australians and all Australians.
We report trends in mortality from these causes of death in indigenous people in Australia, New Zealand (NZ), and the United States (US). |
Methods |
Australian data
The accuracy of Aboriginal and Torres Strait Islander censuses has been investigated.8,9 Experimental, adjusted counts have been calculated by the Australian Bureau of Statistics (ABS) for 1986-199110 and for 199411 at the State level. Population counts of indigenous people in the 1996 Census were greater in every State than expected from the 1991 Census and adjusted counts, indicating that more people identified themselves as Aboriginal or Torres Strait Islander than in previous censuses. The 1985-1996 indigenous population counts we used for WA and the NT were based on ABS experimental counts, adjusted for the 1996 Census. In WA, adjusted 1996 population counts were greater than predictions based on experimental counts for earlier years. Consequently, ABS population counts for WA for 1985-1995 were adjusted upwards so that they were compatible with 1996 figures. In the NT, adjusted 1996 counts were consistent with predictions, and ABS experimental counts and predictions were used. Annual total numbers of deaths for all Australia and for WA and the NT, and corresponding populations, were obtained from the ABS for 1979-1996. ICD-9 coding to four digits was used for coding cause of death.12 US and NZ data
Annual numbers of deaths for Maori for 1974-1994 were obtained from the NZ Health Information Service, and corresponding population estimates were based on census data from Statistics NZ. Excess mortality
Standardised mortality rates
|
Results |
All-cause mortality rates
Death rates for NZ and US indigenous people fell relatively rapidly in the 1970s and more slowly thereafter. Between 1974 and 1984 mortality rates in Maori fell 32%, and a further 19% between 1984 and 1994. Mortality rates in Native Americans fell 17% between 1973 and 1982 from levels some 30% lower than those for Maori, and a further 11% between 1982 and 1992. Current mortality rates in Australian indigenous people are comparable with rates in Maori in the early 1970s. By 1990-1994, the average Australian indigenous all-cause mortality rate was 1.9 times the Maori rate, 2.4 times the US indigenous rate and 3.15 times the all-Australian rate. Main causes of excess mortality in Aboriginals and Torres Strait
Islanders
International comparisons of mortality trends for the major causes
of excess mortality
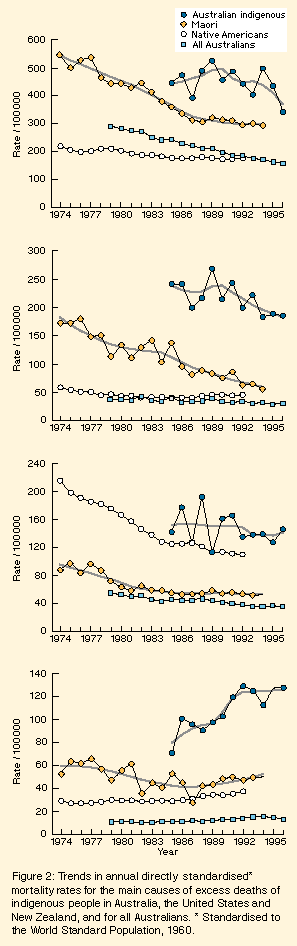
Circulatory disease: Current mortality rates for circulatory diseases in Aboriginals and Torres Strait Islanders were 50% higher than corresponding rates for Maori (the next-highest), and 2.5 times the all-Australian rate (Table, below). In the early 1970s, these mortality rates in Maori were above current Australian indigenous rates, but fell rapidly over the ensuing 20 years. Circulatory disease mortality rates in Native Americans have been lower than those in the other groups for the entire period, while the all-Australian mortality rates have held an intermediate course. Mortality rates from ischaemic heart disease in Maori fell in 1974 from above contemporary Australian indigenous rates to a third below by 1990-1994. By 1990-1994, mortality rates from cerebrovascular disease in Maori, after being equivalent in 1974, were down to less than half the corresponding Australian indigenous rates.
Respiratory diseases: Mortality trends in respiratory system diseases were generally similar to those of the circulatory system, with Maori rates being initially very high (at the level of current Aboriginal and Torres Strait Islander rates) and then falling rapidly to levels not greatly exceeding current all-Australian levels. The overall reductions in rates of diseases of the respiratory system in Maori have been due largely to reductions in asthma and pneumonia deaths, which accounted for most respiratory system deaths in 1990-1994. In Australian indigenous people, other chronic obstructive pulmonary diseases and pneumonia accounted for a similar proportion of respiratory disease deaths in the same period. Injury and poisoning: The pattern here has been somewhat similar, although the relative positions of Native Americans and Maori are reversed. Death rates in Native Americans and Alaskan Natives were one and a half times the Australian indigenous injury and poisoning death rates in the early 1970s, but US rates have now fallen to below the current Australian level. For Aboriginals and Torres Strait Islanders in WA and the NT, there is little evidence of an overall decline (Figure 2). The decline in mortality rates from injury and poisoning in Native Americans has been driven particularly by changes in transport accidents, but also changes in homicide and suicide rates. For Australian indigenous people in WA and the NT, there appear to have been some relatively small recent falls in homicides and transport accident deaths, but there is some evidence that suicide rates are rising. Endocrine diseases: There has been no substantial improvement in mortality from endocrine diseases (largely diabetes). Death rates from diabetes in Maori fell in the 1970s, but have been rising slowly since the mid 1980s. Diabetes mortality rates in Native Americans have been rising slowly for 20 years. The rate for Australian indigenous people has also risen since the mid 1980s, but much more rapidly. In 1990-1994, the average mortality rate in Australian indigenous people for endocrine diseases was 2.4 times the Maori rate, 3.2 times the Native American rate and eight times the Australian rate (Figure 2). |
Discussion |
The health of Aboriginal and Torres Stait Islanders in WA and the NT is
relatively poor compared with that of Maori and Native Americans,
and has shown little, if any, improvement over the past 20 years.
Although Australian mortality data cover only a 12-year period from
1985, there is no reason to believe that rates were much lower in the 10
years before 1985, and may have been somewhat higher.
Several factors may influence the validity of comparisons among these three indigenous groups. A fundamental cause of non-random variation in annual mortality rates for indigenous groups is differences in factors influencing identification of a death as an indigenous death, and those determining whether people identify themselves as indigenous at census time. Special efforts to increase completeness in the 1996 Census resulted in a sharp rise in Australian indigenous population counts. However, similar improvements in ethnic identification on death certificates had not occurred by 1996. Indigenous population sizes over the 12 years studied were adjusted upwards to reflect the 1996 Census increase, which means that the Australian indigenous rates are likely to be lower than their true values. For all three indigenous groups, deaths were grouped by year of registration rather than year of death, so that they could be compared on a common basis. The extent of year-to-year variation in the proportion of deaths in a given year that were also registered in that year is unknown for Maori and Native Americans. Such variation would add a component of extra-Poisson variability to annual rate figures, but is unlikely to influence long term trends. The degree of late registration of Australian indigenous deaths is known to be relatively large compared with non-indigenous deaths and to vary from year to year. For this reason, apparent trends in Australian indigenous rates may be influenced to some degree by error in endpoint rate values. Different cause-of-death coding practices may have existed in the three comparison countries over time, leading to different apparent mortality rates for certain diseases. However, comparability of New Zealand and Australian non-indigenous rates suggests that there has been little difference between coding practices in these two countries over time. Furthermore, all-cause rates, not subject to coding variations, display the same patterns and differentials between ethnic groups observed for the separate causes of death. Although the three indigenous groups each have a different heritage and cultures, they share common experiences in their history. They are minority cultures in affluent nations dispossessed of their country and marginalised. However, Maori and Native Americans have made rapid gains in health and life expectancy over the past two decades. This progress is characterised by an initial rapid fall in death rates, followed by a more gradual decline as levels of the non-indigenous population are approached. Australian indigenous mortality shows little or no evidence of this pattern for any of the major causes of excess deaths. For some causes there is evidence of a recent decline, but no significant trend has yet been established. The health problems of Australia's indigenous people, and the circumstances responsible, are not unique. Why, then, has the health of Australia's indigenous people failed to match the improvement seen in other countries? Kunitz14 identified several aspects of Australian postcolonial indigenous experience which he felt contributed to the lack of improvement in health. He argues that Aboriginal affairs have traditionally been first a colonial then a State responsibility; and that there has been constant tension between State interests, particularly relating to land and management of the indigenous population. Furthermore, an official policy of assimilation maintained over many decades discouraged the creation of specialised indigenous health programs. In more recent times, competition for federal health funding by State and non-State bodies has meant that efforts to improve indigenous health have lacked coordination. Another factor, he suggests, is a lack of a sense of a single identity in many present-day indigenous communities, which were created artificially by gathering together people from many different tribal groups. The Treaty of Waitangi has been central to the relationship between Maori and other New Zealanders, and in the United States treaties established some status for Native Americans in their relationships with the "invading" Europeans, although these treaties were often abused. It is therefore difficult to entirely discount the suggestion that the absence of a treaty is a factor in the relative lack of progress in improving Australian indigenous health. Treaties, no matter how loosely worded, have appeared to play a significant and useful role in the development of health services, and in social and economic issues, for the indigenous people of New Zealand, the United States and Canada. Syme15 has hypothesised that the sense of control that people have over their lives and the sense of hope that this creates are important determinants of health status. He links both of these factors to disadvantage. It is arguable that colonial paternalism, an official policy of assimilation, and a lack of formal recognition through treaties have together acted to create and reinforce a sense of powerlessness in Australian indigenous people which is relatively less in other indigenous groups. It may well be that these intangible factors are adversely affecting indigenous health in Australia. The experience of other indigenous people around the world generates considerable confidence that effective action in Australia will produce substantial changes in indigenous health. Progress is needed in five key areas: infrastructure (land, housing, water supply, education, income, etc), self-determination of health services, access to a network of community-controlled primary healthcare services delivering effective health services for priority issues, an adequate level of resources, and a skilled workforce.16 Future success requires much greater progress within each of these five areas than has occurred in the past. A greater sense of control may only come from a wider acceptance and recognition of a valued role for Australian indigenous people in Australian society. |
References |
|
Authors' details
School of Public Health and Tropical Medicine, James Cook University, Townsville, QLD.Ian T Ring, MB BS, MPH, MSc, Professor; and Head.
Health Information Centre, Queensland Health, Brisbane, QLD.
David Firman, MMath, Statistician.
Reprints: Professor T Ring, School of Public Health and
Tropical Medicine, James Cook University, Townsville, QLD 4811.
E-mail: ian.ringATjcu.edu.au
-
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
- Ian T Ring
- David Firman