Use of systematic reviews of randomised trials by Australian neonatologists and obstetricians
Christopher F C Jordens, Penelope Hawe, Les M Irwig, David J Henderson-Smart, Margaret Ryan, Deborah A Donoghue, Roger G Gabb and Ian S Fraser
MJA 1998; 168: 267-270
For editorial comment see Phillips
Abstract - Introduction - Methods - Results - Discussion - Acknowledgements - References - Authors' details
Abstract |
Objective: To determine what proportion of
Australian neonatologists and obstetricians report using
systematic reviews of randomised trials. Design: Cross-sectional survey using structured telephone interviews. Setting: Australian clinical practice in 1995. Participants: 103 of the 104 neonatologists in Australia (defined as clinicians holding a position in a neonatal intensive care unit); a random sample of 145 members of the Royal Australian College of Obstetricians and Gynaecologists currently practising in Australia. Main outcome measures: Information sources used in clinical practice; reported awareness of, access to and use of systematic reviews, and consequent practice changes. Results: Response rates were 95% (neonatologists) and 87% (obstetricians); 71 neonatologists (72%) and 55 obstetricians (44%) reported using systematic reviews, primarily for individual patient care. Databases of systematic reviews were used with a median frequency of once per month. Among neonatologists, systematic reviews were used more commonly by those who were familiar with computers, attended professional meetings, and had authored research papers. Among obstetricians, they were used more commonly by those who were familiar with computers, had less than 10 years' clinical experience, attended more deliveries, and were full-time staff specialists in public hospitals. Of neonatologists who reported using systematic reviews, 58% attributed some practice change to this use. For obstetricians, the corresponding figure was 80%. Conclusions: There is evidence that Australian neonatologists and obstetricians use systematic reviews and modify their practice accordingly. Dissemination efforts can benefit from knowledge of factors that predict use of systematic reviews. |
Introduction |
Randomised controlled trials are widely accepted as the best method
of evaluating the effectiveness of medical interventions. However,
their findings are slow to change medical opinion and practice.1,2 The communication of
clinically important research findings is hampered by the volume and
geometric growth of the medical literature.3 Reviews address this problem, but conventional review methodology is unscientific4,5 and open to selection biases inherent in the publication process.5,6 This has led to the development of systematic reviews. A properly conducted systematic review begins with an exhaustive search for published and unpublished randomised trials addressing a well defined research question. The second step is to identify trials of adequate quality to contribute to decision-making. The results of included trials are then pooled, or "meta-analysed", to arrive at a quantitative estimate of the benefits and harms of treatment. Systematic reviews published by the Cochrane Collaboration are also continuously updated by specialist review groups.7 Systematic reviews in pregnancy and childbirth have been available for some years. In 1988 a comprehensive trial register became commercially available in database form as the Oxford database of perinatal trials.8 Effective care in pregnancy and childbirth, 9 a textbook based on this research synthesis, was published the following year, with a guide for non- specialist readers.10 A companion textbook, Effective care of the newborn infant,11 appeared in 1992. From 1993, systematic reviews relating to pregnancy and childbirth were available electronically in the Cochrane pregnancy and childbirth database.12 All these reviews are currently being updated for The Cochrane library.13 These new publications represent prototypes for future publications in other fields of practice. However, their impact on clinical practice remains uncertain, despite several surveys to ascertain the extent of their dissemination and uptake.14-18 To make a practical difference, systematic reviews must be readily available to clinicians who are aware of them, who use them, and who implement their findings. To ascertain whether this is occurring in Australia, we conducted a survey of neonatologists and obstetricians with the aims:
|
Methods | |
Participants |
Clinicians who held a position in one of Australia's 23 neonatal
intensive care units were eligible for the survey. The Australian and
New Zealand Neonatal Network (ANZNN), which covers all
neonatologists, provided a current listing. The Royal Australian
College of Obstetricians and Gynaecologists (RACOG) drew a simple
random sample of 20% of Fellows from its membership. Those sampled
were eligible if they were currently practising obstetrics. Any
clinicians not currently practising in Australia, not on the
telephone network, or who were involved in designing this survey,
were ineligible.
Eligible clinicians were sent an introductory letter, telephoned, and invited to schedule a confidential, 10-minute telephone interview about information sources used in clinical practice. Systematic reviews were not mentioned until the interview was under way. |
Interviews |
An existing interview schedule15,16 was modified in consultation
with the ANZNN and the RACOG. Respondents were first asked to name the
three main sources of information they used for keeping up with new
developments in their field, and for dealing with uncertainty about a
specific treatment decision. They were also asked which of the three
information sources they considered the most important or useful for
each task.
Respondents were then asked about their access to and use of computers, and asked directly whether they had heard of, had access to, and used the Cochrane database, Oxford database, and Effective care of the newborn infant (neonatologists) or Effective care in pregnancy and childbirth (obstetricians). Those who reported using any of these resources were asked what a systematic review was, how often they consulted that resource, what they used it for, whether they thought using it had made any difference to their clinical practice and, if so, whether they could name a treatment policy they had altered in response to evidence from a systematic review. To count as users of systematic reviews, respondents had to mention randomised trials or meta-analysis in their description of a systematic review. The final questions sought demographic information on clinical experience, place of education, attendance at professional meetings, research publications, academic appointments, and qualifications. A research degree was defined as a doctorate, relevant master's degree, or bachelor's degree of science in medicine, held in addition to basic medical and specialty qualifications. Reports of authorship were verified by searching MEDLINE and by screening abstracts. For neonatologists it was noted whether they held full- or part-time positions, whether they worked in a hospital with an obstetric unit, whether they headed a neonatal unit, and in which unit they worked. For obstetricians, it was noted whether they held a position as a full-time staff specialist in a public hospital. They were asked how many deliveries they attended each year, and whether they worked at any hospital with an accredited RACOG training post. The interview schedule was modified after a pilot study with seven neonatologists in New Zealand. The main survey was conducted between August and December 1995, with ethics approval from the ANZNN, RACOG and the University of Sydney. All interviews were conducted by the first author (C F C J). |
Analysis | Confidence intervals for the proportion of obstetricians who reported using systematic reviews were calculated with a finite population correction. Confidence intervals were not calculated for the corresponding proportion of neonatologists, as this was ascertained for all Australian neonatologists. Descriptive and c 2 analyses were conducted. Then, using a backwards stepwise modelling procedure, a multivariate logistic regression analysis was used to determine which study factors predicted the reported use of systematic reviews. With the neonatology data, this modelling procedure was repeated using binomial generalised estimating equations to adjust for clustering of respondents within neonatal units.19 |
Results |
Of 106 listed neonatologists, three were ineligible (one had
retired, one was not practising in Australia, and one was involved in
designing this survey). Of the 103 eligible clinicians remaining, 98
completed interviews (95% response). From a sample of 210
obstetricians, 65 were ineligible for the survey (51 no longer
practised obstetrics, 13 were not practising in Australia, and one
could not be located on the telephone network). Of 145 eligible
obstetricians, 126 completed interviews (87% response).
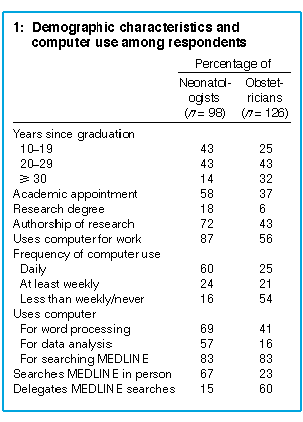
Respondent characteristics are shown in Box 1, with comparative data
on computer use.
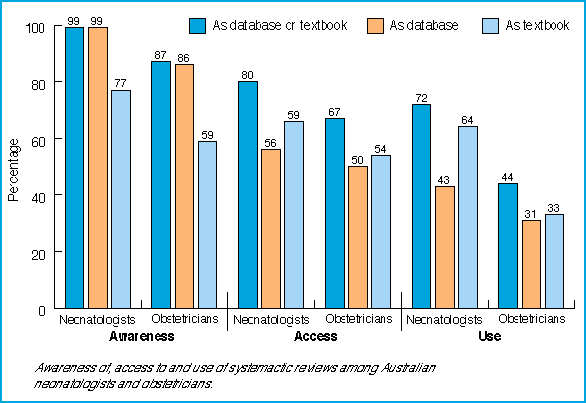
For the purpose of keeping up with new clinical developments, respondents favoured journals, conferences and meetings, colleagues and MEDLINE (in that order) over systematic reviews. For the purpose of clinical problem-solving, colleagues, MEDLINE, journals, and other printed medical literature were favoured over systematic reviews as sources of information. Although the percentages favouring each source varied between the two specialties and according to whether the respondent was simply nominating the resource or nominating it as the most important resource, the rank order of the resources remained consistent. In each specialty, 21% of respondents mentioned systematic reviews without prompting from the interviewer when naming the information sources they used, or when describing their computer use. When questioned directly about systematic reviews, 71 neonatologists (72%) and 55 obstetricians (44%; 95% confidence interval, 36%-51%) reported using them in either electronic database or textbook form. The confidence interval indicates the reliability of the sample prevalence as an estimate of the population prevalence. The Figure shows reported levels of awareness of, access to and use of systematic reviews by specialty. |
 | |
Predictors of |
Results of the multivariate analysis are shown in Box 2. Among
neonatologists, three factors significantly (P<0.05)
and independently predicted use of systematic reviews: attendance
at meetings of the Australian Perinatal Society, authorship of at
least one research paper, and familiarity with computers (our index
of this was use of a computer for word-processing). Results from
cluster analysis agreed with those from logistic regression.
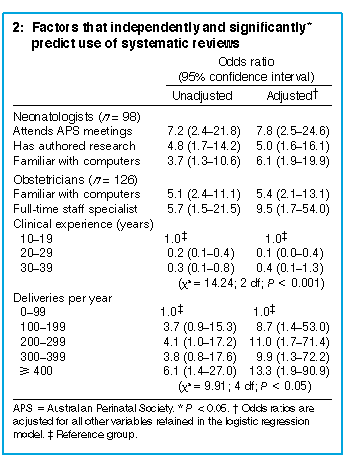 Among obstetricians, four factors sig nificantly and independently predicted use of systematic reviews: familiarity with computers, mode of practice (full-time staff specialists were more likely to use systematic reviews than others), clinical experience (recent graduates were more likely to use systematic reviews), and number of deliveries per year (likelihood of using systematic reviews increased with this number). |
Descriptors of |
Both neonatologists and obstetricians reported using databases of
systematic reviews with a median frequency of once per month. The main
purpose for using systematic reviews (irrespective of their format)
reported by respondents from both specialties was individual
patient care. Systematic reviews were also said to be used for (in rank
order of frequency of reporting) teaching, preparing a pre
sentation, reviewing current management or developing
evidence-based protocols or guidelines, settling disputes,
background information, reviewing a topic, research, as a source of
references, and patient information.
Of the 71 neonatologists who reported using systematic reviews, 58% said that this had changed their clinical practice in some way, and 44% gave at least one example of a treatment policy they had altered in response to a systematic review. The most common examples were treatment of respiratory disorders, and use of steroids and indomethacin. Corresponding percentages for obstetricians who reported using systematic reviews were 80% (reported a change in practice) and 71% (gave at least one example). The most common example was use of steroids in management of preterm rupture of membranes. |
Discussion |
We found that 72% of neonatologists and 44% of obstetricians reported
consulting systematic reviews, primarily for the purpose of
individual patient care. Databases of systematic reviews were used
at a median frequency of once per month. Systematic reviews were used
more commonly by those who were familiar with computers in both
specialties, by those who attended professional meetings and had
authored research papers among neonatologists, and by those who had
had less than 10 years' clinical experience, attended more
deliveries, and who had a position as a full-time staff specialist
among obstetricians.
The findings of this survey are based on self-reporting. Although the survey was designed to minimise over-reporting, it was still subject to imprecision in respondents' recall about (for example) the frequency with which they used systematic reviews, and to difficulties in attributing practice changes to their use. Nevertheless, this was the first study of the use of systematic reviews by Australian clinicians, and the findings have immediate and practical relevance for organisations such as universities, government agencies and specialty colleges that are trying to improve access to the best available evidence and to promote its use.20-23 The association between use of systematic reviews and attendance at Australian Perinatal Society meetings among neonatologists could reflect greater receptiveness to innovations among clinicians who attend professional meetings. However, it also supports the perception (reported elsewhere13 ) that professional organisations play an important role in disseminating research findings. Future dissemination efforts could usefully concentrate on these organisations. In both specialties, familiarity with computers predicted use of systematic reviews. Better access to digital information technology and training in its use is therefore likely to enhance uptake of these reviews. This might include improved access to The Cochrane library and the Internet, and training workshops for searching specialist databases. The remaining predictors of use of systematic reviews, as well as the overall contrast between neonatology and obstetrics, suggest that specialists practising primarily in public hospitals are more likely to use systematic reviews than those working primarily in private practice. Special efforts are therefore needed to reach the latter. As systematic reviews do not appear to rank highly among the information sources used in clinical practice, it is important to stress their relative advantages. Uptake of this innovation appears more likely among recent graduates, with senior clinician researchers acting as "product champions".24 Although debate persists as to whether practising clinicians accept the innovations of evidence-based medicine,25 our survey found evidence that Australian neonatologists and obstetricians use systematic reviews, and appear to modify their practice accordingly. Efforts are needed to enhance the use of these reviews, and to conduct further evaluations of their influence on clinical practice. In attempting to improve practice standards, it is important to pursue methods which have been shown to be effective.26 |
Acknowledgements | We would like to thank the many clinicians who gave up their time to participate in this survey. Infrastructure support for this project was provided by the Department of Public Health and Community Medicine at the University of Sydney. Special thanks are due to Petra Macaskill, who conducted the cluster analysis, and Jeanette Ward and Mary Osborne, from the Central Sydney Area Health Service Needs Assessment and Health Outcomes Unit, who provided helpful advice on survey procedures. |
References |
(Received 11 Jun, accepted 11 Sep, 1997) |
Authors' details
University of Sydney, Sydney, NSW.Christopher F C Jordens, MPH, Postgraduate Student, Department of Public Health and Community Medicine; now Researcher, Centre for Values, Ethics and the Law in Medicine, Department of Surgery, University of Sydney;
Penelope Hawe, MPH, Senior Lecturer, Department of Public Health and Community Medicine;
Les M Irwig, FFPHM, PhD, Associate Professor, Department of Public Health and Community Medicine;
David J Henderson-Smart, PhD, FRACP, Professor, and Director, NSW Centre for Perinatal Health Services Research, and Department of Neonatal Medicine, Royal Prince Alfred Hospital, Sydney, NSW;
Deborah A Donoghue, RN, BSocSc, Senior Research Assistant, Australian Institute of Health and Welfare National Perinatal Statistics Unit;
Ian S Fraser, MD, FRACOG, Professor in Reproductive Medicine, Department of Obstetrics and Gynaecology, Queen Elizabeth II Research Institute for Mothers and Infants.
Royal Australian College of Obstetricians and Gynaecologists,
Melbourne, VIC.
Margaret Ryan, MSW, PhD, Research Officer.
Centre for Professional Development, Victoria University of
Technology, Melbourne, VIC.
Roger G Gabb, PhD, Professor, and Director.
Reprints: Mr C F C Jordens, Department of Surgery, Blackburn
Building D06, University of Sydney, NSW 2006.
E-mail: cjordens AT surgery.usyd.edu.au
Readers may print a single copy for personal use. No further
reproduction or distribution of the articles
should proceed without the permission of the publisher. For
permission, contact the
Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
Received 25 May 2026, accepted 25 May 2026
- Penelope Hawe
- Les M Irwig
- David J Henderson-Smart
- Margaret Ryan
- Deborah A Donoghue