Smoking behaviours of Australian adults in 1995: trends and concerns
David J Hill, Victoria M White and Michelle M Scollo
MJA 1998; 168: 209-213
For editorial comment see Gray
Abstract -
Introduction -
Methods -
Results -
Discussion -
References -
Authors' details
-
-
©MJA1998
Abstract |
Objectives: To estimate the prevalence of smoking
among Australian men and women in 1995 and to examine trends in smoking
prevalence in Australia over the past 10 years. Design: A representative sample of adults participated in face-to-face interviews conducted by a large market research company. Participants: 2819 men and 2880 women over the age of 16. Main outcome measure: Self-reported smoking behaviours assessed by standard questions. Results: Overall, 27.1% of men and 23.2% of women were smokers of tobacco (factory-made cigarettes, pipes, cigars or roll-your-own cigarettes). This difference in smoking prevalence of men and women was significant. More men (32.1%) than women (21.7%) were past smokers and more women (53.4%) than men (39.3%) had never been regular smokers. On average, male smokers smoked about 20 factory-made cigarettes a day, while women smoked about 18. Occupation and education levels were inversely related to smoking prevalence. Comparisons with earlier data suggest that the decline in smoking prevalence seen in previous surveys has ceased. However, the number of cigarettes consumed daily decreased between 1992 and 1995. In the period between 1983 and 1989, when per capita expenditure on adult antismoking campaigns rose, smoking prevalence declined, but levelled off thereafter in a period when expenditure on campaigns fell. Conclusion: Failure to find a continuing decline in prevalence of smoking among the Australian population is of great concern and indicates the importance of continuing and extending antismoking programs. |
Introduction | Cigarette smoking is still the most important preventable cause of premature death in Australia. Reducing the prevalence of smoking rightly remains a high priority on Australia's public health agenda.1,2 As such, it is important to collect and publish estimates of the prevalence of smoking and its sociodemographic correlates at regular intervals, as indicators of progress towards controlling the virtual epidemic of tobacco-related disease,3 and as a basis for public decisions on action to take. We have published data on national smoking prevalence for the years 1974,4 1976,5 1980,6 1983,7 1986,8 19899 and 1992,10 using a standard method of data collection. Here we report data for 1995. |
Methods |
Survey method: A large market research company carried out the sampling and interviewing as part of an omnibus survey in September/October 1995. Procedures were the same as in our previous surveys. In brief, interviews were conducted on the weekend, with respondents within a census collector's district selected at random within specified strata, including State and rural or urban divisions. Within each collector's district an individual residence was chosen at random for the first contact and the adjacent house was contacted next. Further adjacent households were approached until the required number of interviews for that collector's district were obtained (usually eight from about 200 households in each census collector's district). Response rate: Of the households contacted 47% agreed to participate in the survey, 42% refused, and in the remaining 11% either the residents were too old or ill or could not speak English, or call-back was unsuccessful. The response rate for this survey was similar to the rates for the 1992 and 1989 surveys, but it was lower than response rates in earlier years. Thus, if variable response rates influence reported prevalences, this could only have occurred for the period before 1989; recent comparisons are not confounded by response rates. Data collected: Respondents indicated their smoking status by choosing a category from the following list:
Current smokers of factory-made cigarettes indicated the brand usually smoked, the size of the pack usually bought and the number of cigarette packets usually smoked in a week. Respondents' sex, age (in five-year age groups), country of birth, highest level of education achieved, and occupation were recorded, as well as the occupation of the household's main income earner. Analysis of data: We calculated 95% confidence intervals (95% CI) associated with estimates of smoking prevalence among men and women and the difference between estimates. Confidence intervals around prevalence estimates for particular subgroups (eg, men aged 50-59 years) are not given. We used chi-squared tests of association to examine differences in the prevalence of smoking between groups, and logistic regression analyses to explore whether associations between smoking prevalence, educational level, occupation and, for women, country of birth were independent of associations between age and smoking. We used analyses of variance and t tests to examine whether the mean number of cigarettes smoked differed between groups. Finally, to compare the prevalence of smoking across recent years, we age-standardised the data from the 1995, 1992 and 1989 surveys to the age distribution of the 1986 sample. |
Results |
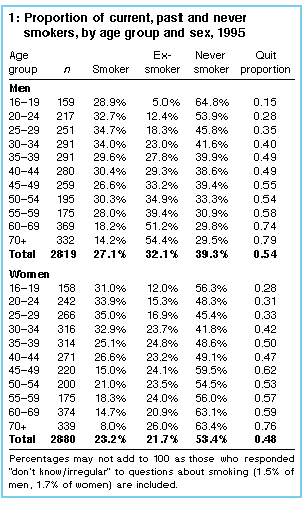
Smoking status: Of the 5699 participants, 51% (2880) were women and 49% (2819) were men. A comparison of the distributions of age, occupation, education and country of birth in the sample data with those in the census data indicated no bias in the socio demographic variables in the dataset. Eighty-two per cent of respondents were interviewed on the first visit to their home. The smoking status of these respondents was similar to that of the more hard-to-reach respondents (those who were interviewed on the second or third contact). Cigarettes dominated tobacco use, with only 1% of men and less than 1% of women indicating that they smoked only pipes or cigars. Only 8% of men and 4% of women had smoked roll-your-own cigarettes in the month before the survey. The smoking status of the males and females in the sample is shown in Table 1.
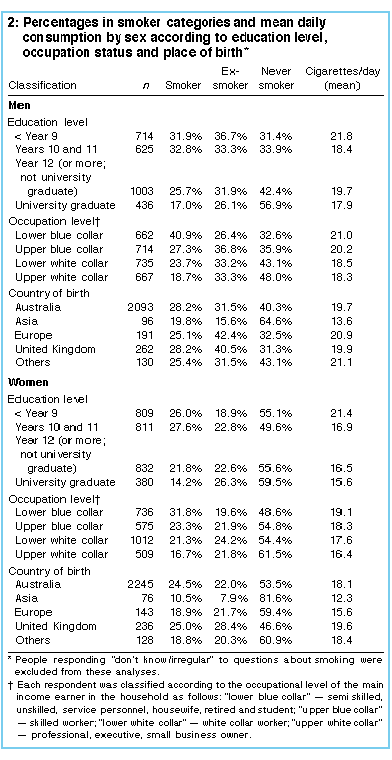
Smoking prevalence: In 1995, the estimated prevalence of smoking among Australian men aged 16 years and over was 27.1% (95% CI, 25.6%-28.7%), while among women the prevalence was estimated to be 23.2% (95% CI, 21.7%-24.7%); this difference was significant (3.9%; 95% CI, 1.6%-6.2%). The prevalence of smoking peaked between the ages of 25 and 29 in men (34.7%) and in women (35%), after which age smoking generally decreased among both men and women. Past smoking or non-smoking: More men (32.1%; 95% CI, 30.4%-33.8%) than women (21.7%; 95% CI, 20.2%-23.2%) were past smokers, a highly significant difference (10.4%; 95% CI, 8.1%-12.7%). More women (53.4%; 95% CI, 51.6%-55.2%) than men (39.3%; 95% CI, 37.5%-41.1%) had never been regular smokers, and again this difference was highly significant (14.1%; 95% CI, 11.5%-16.7%). Men and women differed in their age-related patterns of past smoking. Among men, the proportion of past smokers increased with age to reach a peak of 54.4% in those over 70. Although among women the proportion of past smokers peaked at 26% for those over 70, the proportion of past smokers in the other age groups showed little variation from the overall rate of 21.7%. The proportion who had ever smoked was calculated by adding the percentage of those who had smoked in the past to the percentage of current smokers. Overall, 59.2% (95% CI, 57.4%-61.0%) of men and 44.9% (95% CI, 43.1%-46.7%) of women had smoked at some stage in their life. The association between age and ever having smoked differed for men and women. While among men the proportion who had ever smoked increased with increasing age, for women the proportions of ever smokers began to decrease after the age of 35. Quit proportions: The quit proportion (ie, proportion of ever smokers who had given up smoking in each age and sex group) is also shown in Table 1. The overall quit proportion for men (0.54) was slightly higher than that among women (0.48). However, as Table 1 shows, there is little difference in the quit proportions for men and women in most age groups, except for the 16 to 19 years and 60 to 69 years age groups. Factory-made cigarettes: The mean number of factory-made cigarettes smoked per day by smokers was 19.7 (SD, 11.6) for men and 18.1 (SD, 10.8) for women; this difference was statistically significant (t=2.55, df=1238, P=0.01). In 1995, the cigarettes smoked by women had a lower average tar content than the cigarettes smoked by men (t=5.56, df=1022, P<0.001). The average tar content of cigarettes smoked by men was 8.2 mg (SD, 2.8), while for women it was 7.2 mg (SD, 3.0). Education: As in previous reports of this survey series, the prevalence of smoking and the mean number of cigarettes smoked per day differed for people in various sociodemographic groups. As Table 2 shows, smoking prevalence decreased with increased education, so that only 17.0% of men and 14.2% of women who were university graduates smoked. The association between education level and smoking prevalence was significant for both sexes, but was stronger for men (chi-squared=91.3, df=6, P<0.001) than women (chi-squared=35.5, df=6, P<0.001). The proportions of ex-smokers in the different education levels indicate that quitting was common in all groups. However, the greater proportion of never smokers in the better-educated groups indicates that the lower prevalence of smoking among this group was due to their never having smoked in the first place. For both men and women, smokers with more years of formal education smoked fewer cigarettes per day than did those who had fewer years of education (men: F3,618 = 3.15, P<0.05; women: F3,614=8.92, P<0.001).
Occupational levels: Respondents were classified into one of four occupation levels based on the occupation of the household's main income earner. Occupational levels differed in the level of skill required for the job, such that unskilled workers (eg, labourers) were classified as "lower blue collar", while skilled workers (eg, plumbers) were classified as "upper blue collar". As occupation status increased, the prevalence of smoking decreased (Table 2). Among men from "upper white collar" households, 18.7% smoked compared with 40.9% of men from "lower blue collar" households. The association between occupation status and smoking was significant for both men (chi-squared=102.3, df=6, P<0.001) and women (chi-squared=46.8, df=6, P<0.001). Among men, the proportion of ex-smokers was slightly lower among "lower blue collar" households than other groups . Among women, the proportion of ex-smokers was similar among all occupation groups. The proportion of never smokers was greatest among higher occupation levels. This pattern of results indicates that the lower prevalence of smoking seen in higher occupation groups is due to the relatively lower rate of taking up smoking among these groups rather than their greater success at quitting. The differences in the mean number of cigarettes consumed per day between occupation groups was not statistically significant for men (F3,618 = 2.0, P=0.12) or women (F3,614=1.4, P=0.24). Country of birth: The prevalence of smoking was lowest among both men and women born in Asian countries. However, while the prevalence of 19.8% among Asian-born men was not significantly different from that found for groups born elsewhere, the prevalence of smoking among Asian-born women was significantly lower than the prevalence of smoking among women born in Australia (chi-squared=7.2, df=1, P<0.01) or the United Kingdom (chi-squared=6.6, df=1, P<0.01). The number of cigarettes smoked per day showed little variation according to place of birth. The overall association between place of birth and cigarette consumption was not significant for either men (F4,617=1.3, P=0.26) or women (F4,614=1.0, P=0.40). However, Asian-born men consumed significantly fewer cigarettes per day than did men born elsewhere (t=2.14, df=620, P<0.05). Logistic regression analyses of demo graphic data: In separate analyses, age was entered before the predictor variable of education level, occupational status or country of birth (for women only), and in each case the association between smoking prevalence and the predictor variable remained significant. Pack size and number of cigarettes smoked: The cigarette packet size most commonly used was 25 (by 36% of smokers), followed by packets of 30 and 40 (19% each), 50 (17%), 20 (6%) and 35 (4%). The number of cigarettes smoked per day was related to packet size (F5,1205=34.93, P<0.001). The mean number of cigarettes smoked per day by those who used packets of 20 was 13, for packets of 25 it was 16, for packets of 30 it was 17, for packets of 40 the mean was 23, and for packets of 50 it was 25. Except for women from lower blue collar households, the packet of 25 cigarettes was the most popular size for all occupation and education groups. After collapsing pack-size categories and combining sexes, 55% of blue collar smokers used pack sizes of 20, 25 or 30 compared with 68% of white collar smokers, and 32% of white collar smokers used packs of 35, 40 or 50 compared with 45% of blue collar smokers (chi-squared=20.0, df=1, P<0.001). |
Comparisons with previous years |
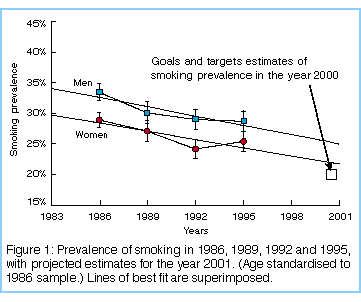
Smoking prevalences in Australia from 1986 to 1995 are shown in Figure 1, with a line of best fit superimposed.
Of concern from a public health point of view is that the observed
prevalence in 1995 is no lower than that in 1992, necessitating an
upward adjustment of the projection to 2001 compared with our
projection based on the four triennial surveys up to 1992. It was
expected that the national prevalence targets for the year 2000 would
be bettered.10 Now the
trends suggest they will not be met, either for men or women. The
results of the 1995 survey also show 5% more men and 3% more women
smoking than would have been expected on the basis of the trends to
1992, and, by extrapolation, this means that in 1995, 356 000 more men
and 384 500 more women were smoking in Australia than expected .
The mean number of cigarettes smoked by men in 1995 was lower than the 22.1 cigarettes smoked per day by men in 1992 (t=3.39, df=1348, P<0.001). Among women, however, the average number of cigarettes smoked per day in 1995 was not significantly less than the number smoked in 1992 (19.1) (t=1.59, df=1322, P=0.113). The legislative and other activity to restrict advertising and promotion of tobacco, as well as expenditure on adult-directed antismoking campigns, between 1989 and 1995 are outlined in Box 1. |
Discussion |
This is the first time in eight successive surveys that the reported
prevalence of smoking in men was no lower than the previous survey and
the first time since 1983 that this was also the case for prevalence of
smoking in women. If these data signal an underlying change and the
previously falling prevalence of smoking has indeed stabilised, a
major public health response is indicated. Attainment of what is
arguably the nation's primary public health target1 -- reducing the prevalence of
smoking in men and women to 20% by 2000 -- is clearly under threat. Given
that this target was and still may be seen as modest, this would be a
major public health failure, as the following calculations show.
For every percentage point smoking prevalence in Australia exceeds the national goal, nearly 140 000 people are smoking who, had the goal been met, would not have been. So, if the goal is missed by 3%, which would be the case if the prevalence remains stable, nearly 420 000 more people than expected will be smoking. If they remain smokers, according to estimates of Doll et al,15 210 000 will die prematurely as a result of their smoking. Against the above fairly alarming observations must be set some auspicious trends -- smokers are smoking less and are probably less exposed to inhaled carcinogens and this should flow through to modest public health gains. As well as benefiting themselves, it seems plausible that a lower daily consumption by smokers is reducing the passive exposure of others to cigarette smoke, as forgone cigarettes may be some of those previously smoked at work or in public places where others would be exposed to sidestream smoke. Assuming these data indicate a slow-down or stalling in the previous reduction in smoking prevalence, why has this occurred and what needs to be done? Figure 2 suggests one explanation for influences on smoking prevalence. At times when antismoking activity is high, whether it be in the form of policy or programs, smoking declines, but when these abate prevalence stagnates. Clearly, these data call for more extensive and rigorous analysis which might incorporate, in a multivariate analysis, other factors such as price, regulations and pro-cigarette promotions. This could determine the extent to which program expenditure affects smoking prevalence. The trends are extremely worrying. Stasis in public policy and prevention programs paralleled by static smoking levels suggest the importance of continuing to extend antismoking programs in order to restart the reduction in smoking prevalence. The experience of some Scandinavian countries shows that public health authorities cannot rest on their laurels.16 Much remains to be done (Box 2). |
References |
(Received 11 Aug 1997, accepted 27 Jan, 1998) |
Authors' details
Centre for Behavioural Research in Cancer, Anti-Cancer Council of Victoria, Melbourne, VIC.David J Hill, PhD, Director;
Victoria M White, MA, Behavioural Scientist;
Michelle M Scollo, BBSc, GradDipCommHlth, Public Health Consultant.
Reprints will not be available from the authors.
Correspondence:
David J Hill, Director, Centre for Behavioural Research in Cancer,
Anti-Cancer Council of Victoria, 1 Rathdowne Street, Carlton South,
VIC 3053.
E-mail: davidh AT accv.org.au
Readers may print a single copy for personal use. No further
reproduction or distribution of the articles
should proceed without the permission of the publisher. For
permission, contact the
Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
Received 29 May 2026, accepted 29 May 2026
- David J Hill
- Victoria M White
- Michelle M Scollo