Abstract |
Objective: To define recent trends (1993-1996) in
incidence of endstage renal disease (ESRD) among Australian
Aboriginal people in the Top End of the Northern Territory
(NT). Design: Analysis of hospital and clinical records of the Darwin-based ESRD treatment program from 1993 to 1996 and comparison with data accumulated since 1978. Participants: All people entering the ESRD treatment program from 1978 to 1996. Main outcome measures: Number of patients treated for ESRD; their ethnicity, age and sex; comorbidities in Aboriginal patients; treatment methods and outcomes. Results: More Aboriginal people presented with ESRD between 1993 and 1996 (87) than in the previous 15 years of the program (68). The incidence of ESRD in Aboriginals reached 838 per million in 1996, and is doubling every 4 years. Aboriginal people presenting with ESRD are younger than non-Aboriginal people with ESRD, and, in contrast to non-Aboriginals, ESRD rates are higher in women than men. The numbers and proportions of Aboriginal ESRD patients who have hypertension, type 2 diabetes and cardiac disease are rising. Haemodialysis remains the most common form of treatment, and the number of dialysis treatments is doubling every 2.5 years. Only 9% of Aboriginal patients entering the program in 1993-1996 were treated with chronic ambulatory peritoneal dialysis and only 3% received transplants. Despite their younger age, survival of Aboriginal people on dialysis is low (median 3.3 years v. 6.5 years in non-Aboriginals), and graft survival after transplant is poor (37% at 5 years v. 88% in non-Aboriginals). Survival has not improved in the past 4 years, with fewer deaths from infection offset by more deaths from cardiovascular disease. Conclusions: The predicted doubling of ESRD incidence among Aboriginal people by the year 2000 will add an enormous burden to limited resources. Risk factors for renal disease underlie all the excess morbidity and mortality in NT Aboriginal adults, and arise out of accelerated lifestyle changes and socioeconomic disadvantage. Better living conditions and education, robust and integrated primary healthcare programs, and systematic screening for early renal disease and treatment of those with established disease are all matters of urgency. |
Introduction |
The high rate of endstage renal disease (ESRD) in Australian
Aboriginal people is attracting increased attention.1-4 The Northern Territory (NT) faces
particular challenges in dealing with this problem. It has the lowest
population (179 000 people) and tax base of any Australian State, and
the highest proportion of Aboriginal people (22% of the population,
compared with 5%-6% for Queensland and Western Australia -- the
States with the next-highest proportion). It has an area of 1 346 200
km2, and only two dialysis
centres, 1500 km apart (one in Darwin and one in Alice Springs), which
can scarcely accommodate the increasing numbers of Aboriginal
people needing treatment.
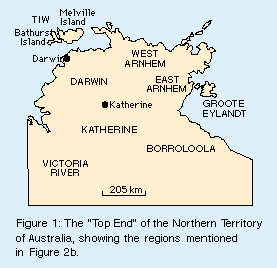
In a previous article,1 we reported the rising rates of ESRD among Aboriginal people in the Top End of the NT (Figure 1), with an average annual incidence of 440 per million from 1988 to 1993. Aboriginal patients were younger than their non-Aboriginal counterparts and, in contrast to the non-Aboriginal population, more women than men were affected. There was little use of chronic ambulatory peritoneal dialysis (CAPD), and the few transplants gave poor results. Comorbidities were high and there was a shorter survival time on treatment than in non-Aboriginal people. Tiwi people living on Bathurst and Melville islands had especially high rates of ESRD, but for other communities there were too few cases to allow calculation of population-adjusted rates. We present data for ESRD treatment in the Top End of the NT for the period 1993-1996, thus extending the period of analysed data to 19 years. The expanded data allow calculation of regional population-specific rates, and illuminate trends in diagnoses, comorbidities, treatment methods and survival. |
Methods | |
Study population | The total study population comprised all people entering the Top End ESRD treatment program from January 1978 to December 1996 inclusive. Our data sources were dialysis unit records and hospital files. We used Australian Bureau of Statistics aggregate and regional data from the 1987, 1991 and 1995 population censuses for the denominators for calculating ESRD rates for the 4-year intervals 1985-1988, 1989-1992, and 1993-1996.5The 1991 Aboriginal community census was used to calculate individual community rates for the three 4-year intervals. People moving to the NT from other countries or other States and becoming residents are potentially included in the census and thus the denominators. |
Statistical analysis | We calculated age-standardised rates of ESRD with Epi-Info6 using aggregate Australian non-Aboriginal data from the 1996 Australian and New Zealand Dialysis and Transplant Registry (ANZDATA) as the reference population.7χ2 tests with Yates' correction were used to examine differences between groups. Kaplan-Meier survival analyses were performed by SPSS for Windows,8 and the log-rank test was used to compare the differences between the groups. |
Results | In the period 1993-1996, 104 people entered the ESRD treatment program, making a total of 214 for the period 1978-1996. Of the total, 155 (72%) were Aboriginal, and 59 (28%) were non-Aboriginal. |
Incidence of treated ESRD |
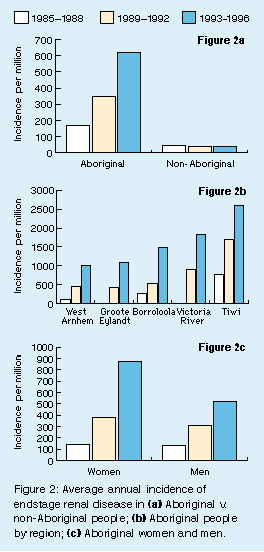
Figure 2a shows the dramatic increase in
incidence of ESRD in Aboriginal people over the three 4-year periods,
with an average doubling time of about 4 years. More Aboriginal people
(87) presented for treatment in the 4 years 1993-1996 than in the
previous 15 years of the program (68). Within this most recent 4-year
period, rates have continued to rise at an average of 22% per year,
peaking at 838 per million9 in
1996 (compared with 39 per million in non-Aboriginal people in the
NT). With age adjustment, the 1993-1996 average annual rate
represents a 15-fold increase and the 1996 rate a 21-fold increase
over ESRD rates in non-Aboriginal Australians nationwide. NT rates
for non-Aboriginals, which did not change over this time period, are
lower than Australian aggregate rates (62 per million from
1993-1996) because the NT has a younger population. All regions of the
Top End are experiencing the same phenomenon, although current rates
vary. Figure 2b shows the changes in
incidence in Aboriginal people in the five regions with the highest
current rates.
The number of Aboriginal people receiving ESRD treatment (the prevalence), including those with functioning transplants, peaked at 2871 per million in 1996 versus 377 per million for non-Aboriginals. Finally, the number of dialysis procedures (which accrue most of the costs) is rising by 28% per year, or doubling every 2.5 years.9 |
Sex and age distribution of ESRD patients |
Ninety-three (60%) of the 155 Aboriginals with ESRD were women and 62
(40%) were men, compared with 23 (39%) women and 36 (61%) men among the
59 non-Aboriginal patients. Figure 2c
shows the higher ESRD rates in Aboriginal women than men at each time
period, resulting, in 1993-1996, in an age-adjusted relative risk of
31 in women versus 16 in men.
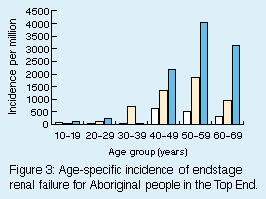
On average, Aboriginal people were 5 years younger than non-Aboriginal people on entering the program (44 v. 49 years). However, the age distributions were quite different, with Aboriginal people most commonly presenting between the ages of 30 and 49 years, and non-Aboriginals between 50 and 69 years. Figure 3 shows that ESRD rates in Aboriginal people rose in most age groups over the life of the program, so that the average age and age distribution did not change appreciably. The age-specific incidence of ESRD in Aboriginal people peaked at age 50-59 years, and in non-Aboriginals at over 70 years. |
Renal failure causes and comorbidities in Aboriginals |
The Table compares the distribution of "causes" of ESRD in the two most
recent 4-year intervals in those patients with documented causes.
The proportion of ESRD in Aboriginal people attributed to (but not
always solely due to) diabetes has almost doubled, that classified as
glomerulonephritis has fallen by more than half, and the proportion
in the "unknown" category has increased markedly.
Aboriginal people with ESRD are more likely than non-Aboriginal people to have type 2 diabetes (48% v. 24%; P = 0.002) and hypertension (52% v. 32%; P = 0.01). Furthermore, these proportions have increased recently: for diabetes from 37% pre-1993 to 60% in 1993-1996 (P < 0.005); and for hypertension from 43% to 57% (P = 0.1); and for people with both diabetes and hypertension from 19% to 38% (P = 0.011). |
Treatment for ESRD |
Fifty-one per cent (30) of non-Aboriginal people, but only 17% (26) of
Aboriginal people, have received transplants since 1978, and only 3%
in the period 1993-1996. Potential reasons for this discrepancy
include medical ineligibility, discouraging earlier results,
distance to the transplant centre (in Adelaide), underservicing and
difficulties in supervision of care in remote areas, lack of living
related donors, and difficulties in HLA matching with donor organs.
In 1996, only 11% of Aboriginal people with ESRD had functioning
transplants versus 65% for non-Aboriginal people.
Chronic ambulatory peritoneal dialysis (CAPD) rates in Aboriginal patients remain low, with only 5% of incident cases pre-1993 and 9% in 1993-1996 treated in this manner. |
Patient and graft survival |
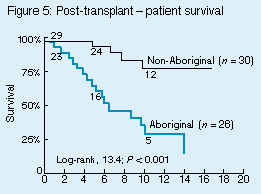
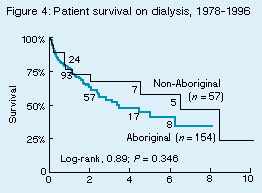 Despite the younger age of Aboriginal patients with ESRD, their "integrated" survival (with all forms of treatment, ie, dialysis and transplantation) was significantly worse than that of non-Aboriginal people, with median survival times of 3.6 versus 12.3 years (P = 0.0025). This difference was reflected in those with and without diabetes. While survival on dialysis (CAPD and haemodialysis), as shown in Figure 4, tended to be lower in Aboriginal people (median 3.3 v. 6.5 years; P = 0.34), both graft and patient survival after transplantation were clearly worse (Figures 5 and 6). Patient survival at 1 and 5 years after transplantation was 92% and 60% for Aboriginals, compared with 97% and 93% for non-Aboriginals (P < 0.001), and graft survival at 1 and 5 years was 73% and 37% for Aboriginal people, compared with 97% and 88% for non-Aboriginal people (P < 0.001). There has been no improvement in integrated survival, or in dialysis or transplant survival separately, in the period 1993-1996.
|
Causes of death | The causes of death in Aboriginal people have changed for the period 1993-1996. Deaths due to cardiac disease have increased from 33% before 1993 to 51% after 1993. Deaths due to voluntary withdrawal from treatment are unchanged (24% and 25%, respectively). In contrast, only one non-Aboriginal patient has ever withdrawn from treatment, and none in the past decade. |
Discussion |
These data for 1993-1996 confirm and further define the rise in
incidence of renal failure among Aboriginal people in the Top End of
the Northern Territory. No community is spared, and this pattern is
repeated in Central Australian Aboriginals, who have even higher
rates (1400 per million in 1996).4 Current incidence rates are now
comparable with those of Afro-Americans and Native Americans (800
and 744 per million, respectively, in 1995); however, age-adjusted
rates are much higher in Australian Aboriginals (due to their very
youthful population) and are increasing much faster, with a doubling
time less than 4 years versus 10 years for the US minority
groups.10 These alarming
figures are nonetheless underestimates, because some Aboriginal
people, especially older people and those from very remote
communities, decline treatment for ESRD or are medically unsuited.
Most of the increase is real. It is not due to ageing of the Aboriginal population, as it is reflected across every age group; and it is not due to improved ascertainment, at least in the major communities, as awareness has been high since the mid 1980s. The disability and the personal, family and community disruption are great, and the resource requirement will be truly formidable if current rates of increase, which project up to 500 new cases between 1997 and 2004 (exponential progression), are sustained. The data confirm the younger age and female predominance of Aboriginal people with ESRD. The latter might be due, in part, to lower birthweights and the relatively higher adult body weights in women, with more marked insulin resistance and earlier onset of type 2 diabetes.11,12 Both occur also in Central Australia.4 Some of the change in attributed cause of ESRD over the most recent 8-year period reflects subjectivity in assignment criteria, but much reflects reassignment of the common finding of bland glomerulomegaly with absent or minimal inflammation13-15 from the "glomerulonephritis" category to the "unknown" category. The rise in renal failure attributed to diabetes is compatible with the dramatic increase in rates of diabetes and its complications in all Aboriginal communities,16 but clinical and biopsy data show that diabetes is more often a facilitating factor for disease expression and progression rather than the prime or sole cause of the underlying nephropathy.11,14 The increased incidence in all communities of Syndrome X (obesity, hypertension, dyslipidaemia, dysglycaemia and predisposition to cardiovascular disease), which is attributed to insulin resistance, likewise explains the increasing proportions of Aboriginal people presenting for ESRD treatment with diabetes and hypertension as comorbidities.11,16-18 These conditions are already generating more heart attacks, strokes, coronary angioplasties, coronary artery bypass graft procedures and cardiovascular deaths among Aboriginal ESRD patients. As the epidemic grows and the Aboriginal population ages, these complications will become more common, and further increase costs, complicate treatment and compromise survival. The persistently high rate of withdrawal of Aboriginal people from ESRD treatment reflects difficulties with chronic disability, the complex treatment regimen, and loss of social and family support and "land identity" associated with relocation from their community to Darwin for treatment.19,20 Initiatives to move treatment closer to home include attempts to promote CAPD, which has low rates of technical failure and peritonitis, but major problems with exit-site infections;20 a renewed focus on transplant (seven Aboriginal people received transplants in 1997); construction of the first community-based dialysis unit with seven stations on the Tiwi islands; and the possibility of placing haemodialysis stations in clinics in high risk remote areas. However, deliberations about efficient and equitable delivery of ESRD treatment must no longer be allowed to dominate the dialogue. Dialysis in the Top End currently costs $496 per treatment, which is about $75 000 per patient per year. This cost does not include medicines, relocation and housing, transportation and hospitalisations.9 The allocation of resources of this magnitude to people with a median life expectancy of 3.3 years must be balanced by serious and sustained community-based initiatives to prevent and ameliorate the underlying problem. Most renal disease in Aboriginal communities is marked by albuminuria, and all renal failure arises in people with a history of progressive overt albuminuria.11Risk factors for renal failure include low birthweight and infant malnutrition, infections (scabies, poststreptococcal glomerulonephritis), increasing adult weight, high blood pressure, increasing glucose levels, insulin resistance, dyslipidaemia, and heavy drinking.11 Several risk factors can operate simultaneously, progressively compounding the decline in renal function that accompanies increasing age. The current epidemic is probably explained by the confluence of many risk factors over a short time period, associated with dramatic lifestyle changes and serious socioeconomic disadvantage. Ironically, the great fall in infant mortality between the late 1950s and late 1970s, a consequence of better hospital management of sick babies, means that those low birthweight babies now surviving to adult life are at high risk for renal and other chronic diseases.11,21 This multifactorial perspective on renal disease necessitates a rethinking of renal disease classifications.11 There is a need for a stronger focus on community and individual risk factor profiles and on pathophysiological interactions, and some de-emphasis of categorical definitions. It justifies a general preventive health services model, which will also reduce the diabetes, hypertension, cardiovascular disease, chronic lung disease and infections that contribute to the excess mortality in NT Aboriginal adults.17 In addition, screening programs to recognise early and established renal disease, and treatment (including angiotensin-converting enzyme inhibitors) to arrest disease progression, must be incorporated into regular adult healthcare in every Aboriginal community as a matter of urgency.22,23 |
Acknowledgements |
This study was supported by the National Health and Medical Research
Council of Australia, and the Australian Kidney Foundation.
We thank Dr David Pugsley, who led the way with renal services in the Northern Territory, and established the basis of these observations, and Dr Diane Howard and Dr Sid Selva-Nayagam, who have had the longest tenure of care of renal patients. We thank the staff of the Nightcliff Dialysis Unit and the Renal Unit at Royal Darwin Hospital for their excellent care and cooperation. Dr Zhiqiang Wang assisted with statistical analyses, and Ms Susan Jacups with clerical and graphic support. |
References |
(Received 5 Jan, accepted 10 Mar, 1998) |
Authors' details
Menzies School of Health Research, Darwin, NT.Janine L Spencer, FRACP, DTM&H(Lond), Paediatrician, Australian Kidney Foundation Research Fellow.
Wendy E Hoy, BScMed, FRACP, NHMRC Senior Research Fellow, Director of Renal Program; and Renal Community Services Specialist, Territory Health Service.
TVW Telethon Institute for Child Health Research, Perth, WA.
Desiree T Silva, FRACP, MPH, Paediatrician.
Royal Darwin Hospital, Darwin, NT.
Paul Snelling, FRACP, Nephrologist, Royal Darwin Hospital,
and Territory Health Service.
Reprints will not be available from the authors.
Correspondence: Dr W
E Hoy, Menzies School of Health Research, PO Box 41096, Casuarina, NT
0811.
E-mail: wendyATmenzies.su.edu.au
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia ".
Received 25 May 2026, accepted 25 May 2026
- Janine L Spencer
- Desiree T Silva
- Paul Snelling
- Wendy E Hoy