Women's satisfaction with medical abortion with RU486
Pam M Mamers, Anna L Lavelle, Amanda J Evans, Sandra M Bell, Jen R Rusden and David L Healy
The combination of RU486 (mifepristone) and prostaglandin analogues has been used for medical abortion in several European centres. We surveyed 41 Australian women who successfully used this method of abortion in a World Health Organization-sponsored trial. Overall, the women were satisfied with the method and found the associated pain level acceptable. (MJA 1997; 167: 316-317)
For editorial comment, see Henshaw
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Introduction - Clinical record - Results - Discussion - Acknowledgements - References - Authors' details
- - ©MJA1997
Introduction |
A safe, reliable, non-invasive, but effective, method of fertility
control has been sought for many years. The combination of the
progesterone antagonist mifepristone (RU486) and prostaglandin E1 analogues has been used in several European countries
for medical abortion, and its efficacy has been extensively studied
for human fertility control. RU486 has been approved for use in the
United Kingdom, Sweden, China and France, and it is estimated that
over a million women have received RU486 in these countries since 1988
(Dr P Van Look, Associate Director, Special Program of Research,
Development and Research Training, World Health Organization,
personal communication).
Following approval from the Therapeutic Goods Administration in March 1994, the World Health Organization selected Monash University and Family Planning Victoria to participate in an international multicentre, double-blind, randomised controlled trial to test the efficacy and side effects of two doses of mifepristone (600 mg or 200 mg) followed by 400 mg of misoprostol 48 hours later for the termination of early pregnancy. Ethical approval to conduct the trial was obtained from the ethics committee of Family Planning Victoria. We thought it would be useful to know if the Australian women who participated in this WHO trial considered medical abortion an acceptable primary treatment and if their level of pain was acceptable. For women who had had a previous surgical termination, we were interested in how they felt the methods compared. |
Clinical record |
Fifty patients seeking legal abortion were admitted to the study on
satisfying the criteria of the WHO protocol, which were: women
seeking legal abortion, in good general health, over the age of
consent, with a menstrual delay of up 35 days, with uterine size equal
to that expected for the estimated duration of pregnancy, having had a
positive pregnancy test, and who gave informed consent. Each woman
received extensive counselling by the nurse coordinator (P M M) and
the investigator (D L H) before entering the trial. Women were
advised that further counselling would be available at any time.
According to the trial protocol, participants attended the clinic to receive mifepristone and returned after 48 hours to receive misoprostol. Women were offered paracetamol (500 mg) for mild to moderate pain or pethidine (50 mg intramuscularly) for severe pain. Analgesic preparations known to interfere with prostaglandin metabolism, such as salicylates and mefenamic acid, were not dispensed and women were advised not to take these. Patients returned for follow-up two weeks and six weeks after abortion. Five women were withdrawn from the trial because they needed surgical intervention. Four women who had a successful termination of pregnancy failed to attend for assessment at six weeks and were lost to follow-up. Thirty-eight of the remaining 41 women who completed the protocol agreed to complete a self-administered questionnaire to assess their satisfaction with medical abortion. The questionnaire included two visual analogue scales on which:
Further, the questionnaire included questions about cost, avoidance of anaesthesia, whether the procedure was considered more natural, and whether the pain and discomfort were acceptable. Women were also invited to make personal comments about why they chose a medical abortion and how they rated their experience. |
Results |
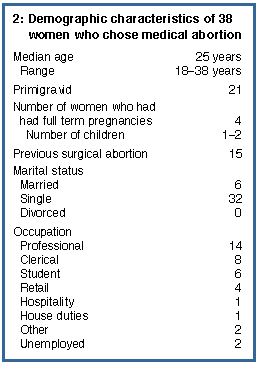
The demographic variables for the 38 women who completed the
questionnaire are shown in Box 2. The mean score for satisfaction with
medical termination of pregnancy was 4.5 (range, 1-5). The 15 women
who had previously had a surgical abortion found the medical approach
more acceptable (mean score, 4.5; range, 3-5).
The level of pain and discomfort was regarded as acceptable by 34 participants; 19 women experienced only mild discomfort, while one woman was pain free. Seventeen of these 20 women did not require analgesia. Only one patient required pethidine for severe pelvic cramping. The remaining women who required analgesia were satisfied with paracetamol. Cost was an important factor in the choice for seven of the 38 participants. There were no costs involved for trial patients. As public hospitals in Victoria are able to service only a small number of patients, most women seeking termination must attend private abortion clinics, so that cost becomes a factor in their choice of provider. The wish to avoid anaesthesia was important for 19 women, while 25 regarded medical abortion as more natural. Other factors in women's decisions to choose medical termination included preferring a less clinical atmosphere and finding research staff to be very supportive at a stressful time (nine women), considering a medical termination to be more emotionally acceptable (nine women), and fear of surgical operation (six women). Other factors included more autonomy (expressed as "a need to be in control of the situation") and the desire for a less invasive procedure. One woman stated: "I was much more able to cope with my decision to have a medical termination as I was conscious the whole time and did not feel that my body was invaded." Six women reported that the associated pain and the duration of bleeding was a drawback for medical abortion, but all six rated the procedure as acceptable. |
Discussion |
We acknowledge that our sample was biased, as the 38 women who
completed questionnaires sought out medical termination of
pregnancy. However, in terms of many demographic variables, our
participants were similar to a large sample of women who sought
surgical terminations in New South Wales surveyed by Adelson et al.1 Over half the women in both
groups were single, most were 25 years or under and they were generally
well educated.
Satisfaction with medical termination of pregnancy among the 38 women was evident. The factors involved in their choice of medical abortion were complex. Overall, medical abortion provided women with a more active role in the process, thus allowing them to achieve a certain degree of autonomy. Most of the women surveyed described the medical approach as more natural, and two women likened the procedure to having a miscarriage. The requirements for a medical abortion differ in many respects from those for a surgical abortion. In particular, partners, friends or family could be present at any time, and patients were not required to fast during the three hours they remained in the clinic after being given misoprostol. Many of the women who participated in the trial commented on the friendly, non-clinical approach, which they considered psychologically beneficial at a time when anxiety levels were increased. Similar psychological benefits of medical abortion have been noted by Henshaw and colleagues.2 Medical abortion as an alterative to surgical abortion has gained acceptance in countries in which it has become available. In a British study of 363 women undergoing first-trimester abortion, 20% of women chose medical abortion, 26% chose the surgical technique, and the remainder agreed to be randomised to either method.3 This finding concurs with earlier studies in France where one-fifth of women chose medical abortion.4 In a Chinese study, women who were likely to accept medical abortion were single, young, nulliparous and employed; these women were reportedly fearful of "trauma to the body" from surgical abortion.5 Significantly, all women who answered the questionnaire in that study said that they would choose medical termination again.5 As Baird6 has suggested, more studies are needed to establish the acceptability of mifepristone (RU486) for termination of pregnancy in different countries and different cultures. A further follow-up study in Australia with a larger sample of women would be useful in this regard. |
Acknowledgements | We thank our patients as well as Family Planning Victoria for their support and recruitment of women for this study. |
References |
(Received 17 Dec 1996, accepted 27 Jun, 1997) |
Authors' details
Monash University Department of Obstetrics and Gynaecology, Monash Medical Centre, Melbourne, VIC.Pam M Mamers, RN, BA, Clinical Research Nurse;
Amanda J Evans, FRACGP, CertFPA, Medical Director Family Planning, and Honorary Senior Lecturer;
David L Healy, FRACOG, PhD, Chairman.
Family Planning Victoria, Melbourne, VIC.
Anna L Lavelle, BSc(Hons), PhD, Executive Director;
Sandra M Bell, RN, RM, Research Nurse and Pregnancy Counsellor;
Jen R Rusden, RN, Research Nurse and Pregnancy Counsellor.
Reprints will not be available from the authors.
Correspondence: Ms P
M Mamers, Monash University Department of Obstetrics and
Gynaecology, Level 5, Monash Medical Centre, 246 Clayton Road,
Clayton, VIC 3168.
©MJA 1997
<URL: http://www.mja.com.au/>
© 1997 Medical Journal of Australia.
- Pam M Mamers
- Anna L Lavelle
- Amanda J Evans
- Sandra M Bell
- Jen R Rusden
- David L Healy