Abstract
Objectives: To estimate the number of pregnant women in New South Wales who had not been tested for gestational diabetes mellitus (GDM) during the period 1991-1994.Design: The number of women not tested for GDM was estimated from the recorded data available in the NSW Midwives Data Collection (MDC) annual reports and compared with three incidence surveys.
Main outcome measure: The number of pregnant women not tested for GDM.
Results: Over the four-year period, the average annual recorded MDC incidence of GDM was 2.2%. This percentage was adjusted up to 3.3% after review of the MDC validation study and an incidence study. However, the expected incidence of GDM from three incidence surveys was 6.6%. Thus, half of the pregnant women in NSW do not appear to have been tested for GDM.
Conclusion: For the four-year period 1991-1994, an estimated 50% of women in NSW were probably not tested for GDM.
MJA 1997; 167: 14-16
Introduction
Following the Australasian Diabetes in Pregnancy Society's (ADIPS) 1991 recommendation that all pregnant women should be tested for GDM in every pregnancy,5 the NSW Midwives Data Collection (MDC) recorded a gradual increase in the number of women with GDM from 1.5% in 1991 to 2.7% in 1994. In contrast, from surveys in other Australian centres since 1991, the incidence of GDM ranges from 5.5%-8.8%.4,6-8
The difference between these rates and those recorded by the MDC suggests that many women are still not being tested for GDM in NSW and are at risk of complications which could either be prevented or substantially reduced. The purpose of our study was to estimate the extent of undiagnosed GDM in NSW for the period 1991-1994 by estimating the number of pregnant women who had not been tested for GDM.
Methods
We obtained data from the NSW MDC annual reports for 1991-1994. It is a statutory requirement under the Public Health Act 1991 (NSW) that all births (including home births) are reported to the MDC, which records information on maternal medical and obstetric conditions, delivery and infant characteristics.Incidence of GDM recorded on the MDC was compared with the incidence of GDM found in three different Australian surveys. The sources of these data are shown in Box 1. The three surveys used the 75 g oral glucose tolerance test for the diagnosis of GDM based on the ADIPS criteria.5 According to these criteria, GDM is diagnosed if the fasting plasma glucose level is ≥ 5.5 mmol/L and/or the two-hour plasma glucose level is ≥ 8.0 mmol/L. By combining these data, we obtain an average incidence of GDM, which we refer to as the expected incidence.

At the Mercy Hospital for Women in Melbourne, a 50 g glucose load is used and capillary blood samples taken for plasma glucose measurement; a diagnosis of GDM is made if the glucose level at one hour is ≥ 9.0 mmol/L and the glucose level at two hours is ≥ 7.0 mmol/L. The incidence of GDM during the period 1991-1994 was 8.8%.4 While the glucose load and diagnostic criteria are different, a comparison of the Mercy Hospital and ADIPS criteria found that they diagnosed similar women and in the same proportion.9
While the incidence of GDM will vary depending on the ethnic composition of the population being examined, these surveys all included a majority of people of European extraction.
Validation of the NSW Midwives Data Collection
A 1990 validation study of the MDC, using a 1% sample, found that the recording of data relating to GDM had a sensitivity of 66.7% and a specificity of 99.6%.10 That is, when a case of GDM was recorded it was accurate, but only two-thirds of the known cases were recorded. Therefore, by increasing the recorded MDC incidence by 50% (representing the underestimation of GDM according to the sensitivity data), we are likely to obtain the actual MDC incidence, which we refer to as the estimated incidence.
A 1993 survey carried out in the Wollongong area to determine the incidence of GDM was compared with the recorded MDC incidence of GDM in the area.6 The MDC recorded a rate of 5.0%, while the survey found a rate of 7.2%. A 50% addition to the recorded MDC incidence (as indicated by the validation study) gave a figure of 7.5%, which is similar to the 7.2% found in the survey. Therefore, the addition of a 50% correction factor to the recorded MDC incidence of GDM is a reasonable approximation.
Results
The proportion of women with a diagnosis of GDM recorded by the MDC for each different Area Health Service in NSW between 1991 and 1994 is shown in Box 2. It was assumed that the accuracy of data recording in all Area Health Services was equal and had not changed over the four-year period.
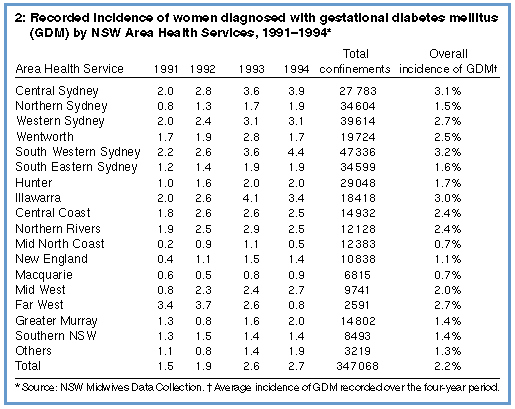
For the whole of NSW, the percentage of women diagnosed with GDM increased from 1.5% in 1991 to 1.9% in 1992 (P < 0.001) and from 1.9% in 1992 to 2.6% in 1993 (P < 0.001). There was no significant change between 1993 and 1994. For the four-year period, the overall recorded MDC incidence of GDM was 2.2%.
In the Sydney metropolitan area, the incidence of GDM ranged from a high of 3.1% in the Central Sydney Area Health Service to a low of 1.5% in the Northern Sydney Area Health Service. The incidence of GDM in the main metropolitan areas of Sydney, Newcastle and Wollongong was 2.4%, which was significantly higher than the country areas (1.6%) (P < 0.001). Some country areas also showed marked changes over the four-year period. For example, the proportion of women diagnosed with GDM increased from 0.8% to 2.7% in the Mid West Area Health Service and declined from 3.4% to 0.8% in the Far West Area Health Service.
By applying the 50% correction factor to the recorded MDC incidence of 2.2%, the estimated incidence of GDM is 3.3%. However, the expected incidence of GDM is 6.6% (Box 1). Therefore, half of the pregnant women in NSW during the period 1991-1994, or 173 534 women, were probably not tested for GDM.
Discussion
The expected incidence of GDM was derived from pooled incidence data from the three surveys where the diagnosis had been based on the ADIPS criteria. The lowest incidence was reported in the two surveys which used data gathered from prenatal clinics.7,8 A higher incidence was reported in the survey which included private patients in the data collection.6 The higher rate found in the survey which included private patients could be anticipated, as private patients are older than clinic patients and increasing age is a high risk factor for developing GDM.4 Thus, the expected incidence of GDM of 6.6% is likely to be conservative.The recorded MDC incidence of GDM for 1991-1994 was lower than the expected incidence. With the application of the 50% correction factor to the recorded MDC incidence (as suggested by the MDC validation study and by data collection in the Wollongong area6 ) and a conservative estimate for the expected incidence of GDM, it is possible that half of all the women who delivered in NSW between 1991 and 1994 were not tested for GDM.
Some women may have decided not to be tested for GDM. Others may not have been able to tolerate the glucose solution. In most cases, however, the decision not to test would have undoubtedly been made by the clinician responsible.
Box 2 shows that testing for GDM is not evenly distributed, with a recorded MDC incidence range of 0.7%-3.2%. Of particular concern is that lower than average rates of testing were found in areas where a higher than average rate of GDM could be anticipated. In metropolitan Sydney, the lowest number of recorded cases of GDM were from the Northern Sydney Area Health Service. The MDC has shown that this is also the Area Health Service with the highest proportion of women aged 35 years or over at the time of delivery, a risk factor for GDM. An incidence of GDM of at least 10%4 could be anticipated in this age group.
Women with an Aboriginal background have a high incidence of GDM.8 The New England and Macquarie Area Health Service, with a high proportion of Aboriginal Australians, had a rate of GDM less than the non-metropolitan average. The Far West Area Health Service also has a high proportion of Aboriginal Australians, and the recorded incidence of GDM there fell over the four-year period from 3.4% to 0.8%.
Observational studies of women with untreated GDM have found a higher perinatal mortality rate than that found in glucose-tolerant women.2,3 At the Mercy Hospital for Women in Melbourne, Beischer et al. showed that, despite a steady reduction in the overall perinatal mortality rate, women who were not tested for GDM (and therefore not treated) had a significantly higher perinatal mortality rate than women who were tested.4 An estimate can be made of the excess perinatal mortality rate for women in NSW who have not been tested for GDM ( Box 3).
Although the recorded incidence of GDM has increased (particularly in the two years after the ADIPS recommendation for universal testing was made), our results confirmed our belief that not all pregnant women in NSW are being tested for GDM. This may have implications for perinatal mortality rates.
References
- Metzger BE. Summary and recommendations of the Third International Workshop-Conference on Gestational Diabetes Mellitus; 1991 Dec. Diabetes 1991; 40 Suppl 2: 197-201.
- O'Sullivan JB, Charles D, Mahan CM, et al. Gestational diabetes and perinatal mortality rate. Am J Obstet Gynecol 1973; 116: 901-904.
- Pettitt DJ, Knowler WC, Baird R, et al. Gestational diabetes: infant and maternal complications of pregnancy in relation to third-trimester glucose tolerance in the Pima Indians. Diabetes Care 1980; 3: 458-464.
- Beischer NA, Wein P, Sheedy MT, et al. Identification and treatment of women with hyperglycaemia diagnosed during pregnancy can significantly reduce perinatal mortality rates. Aust N Z J Obstet Gynaecol 1996; 36: 239-247.
- Martin FIR. The diagnosis of gestational diabetes. Med J Aust 1991; 155: 112.
- Moses R, Griffiths R, McPherson S. The incidence of gestational diabetes in the Illawarra area of New South Wales. Aust N Z J Obstet Gynaecol 1994; 34: 425-427.
- Martin FIR, Ratnaike S, Wootton A, et al. The 75 g oral glucose tolerance in pregnancy. Diabetes Res Clin Pract 1995; 27: 147-151.
- Yue DK, Molyneaux LM, Ross GP, et al. Why does ethnicity affect prevalence of gestational diabetes? The underwater volcano theory. Diabet Med 1996; 13: 748-752.
- Henry OA, Shelley-Jones DC, Oats JN, et al. Comparison of the 50 g capillary plasma glucose tolerance test with the 75 g venous plasma glucose tolerance test in pregnancy. J Obstet Gynecol Res 1996; 22: 215-219.
- Epidemiology and Health Services Evaluation Branch, Public Health Division, NSW Health Department. Validation Study of the New South Wales Midwives Data Collection 1990. Public Health Bull 1993; 4 Suppl 8: S5.
(Received 15 Jan, accepted 8 May, 1997)
Authors' details
Illawarra Area Health Service, NSW.Robert G Moses, FRACP, Clinical Director of Diabetes Services.
Prince of Wales Hospital, Sydney, NSW.
Stephen Colagiuri, FRACP, Director of Diabetes Services.
Received 25 May 2026, accepted 25 May 2026
- Robert G Moses
- Stephen Colagiuri




