Reported use of asthma management plans in South Australia
Justin J Beilby, Melanie A Wakefield and Richard E Ruffin
MJA 1997; 166: 298
For comment see Jenkins & Bauman
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Results - Asthma management plans - Good management - Discussion - References - Authors' details
- - ©MJA1997
Abstract |
Objective: To examine the use of asthma management
plans (AMPs) and specific elements of AMPs in a South Australian
community. Design: Cross-sectional questionnaire survey by experienced interviewers. Participants and Setting: 307 adults with current asthma, confirmed by a doctor, who were among 3001 respondents of a representative sample of 4065 South Australian adults recruited by multistage systematic clustered area sampling for a larger study in March 1995. Main Outcome Measures: Prevalence of reported use of AMPs and of specific elements of AMPs, such as knowledge of trigger factors and having an action plan, and the proportion of adults with asthma receiving what we defined as "good management". Results: 46% reported having an AMP; 63% had discussed trigger factors with their doctors and 39.5% had action plans. 82% had been told the severity of their asthma, and 23.3% were receiving good management. Conclusion: Less than half of people with asthma use AMPs, although certain elements within the AMPs are reportedly being used more frequently. More research is required on why AMPs are not more generally used and, more importantly, on what elements within the AMP model are useful and effective for people with asthma and likely to be used by their general practitioners (GPs). |
Introduction |
Asthma causes substantial morbidity1 and mortality,2 and costs -- in the range of $585-$720
million in Australia in 1991.3
Approximately 9% of Australians (over 1.4 million people)
have reported asthma as "either a recent or long term condition in the
last 12 months".4 There is
evidence that the prevalence of the disease is increasing,5 and that it is both undertreated and
underdiagnosed.6 The
variability of the condition in both adults and children further
complicates these concerns.
In an attempt to create a unified approach to the management of asthma, a group of "accepted experts" developed the Asthma Management Plan (AMP), a set of consensus guidelines for health professionals.7 The Australian AMP comprises six steps:
In this study we examine the current use of AMPs and determine the specific elements of the plan that have been adopted by people with asthma and their doctors. Such information is important in planning ongoing asthma management campaigns. |
Methods |
In March 1995, a representative population sample of adults in South
Australia was obtained for the Health Omnibus Survey,8 as follows. A multistage systematic
clustered area sample of households was used to give a sample
comprising 75% selected from the Adelaide metropolitan area and the
rem ainder from country centres with populations of 1000 or more. At
each household, one person aged 15 years or over (the person whose
birthday was last) was selected for interview. Interviews were
conducted in the respondent's home by trained interviewers, with up
to six call-back visits if the selected respondent was not at home.
For the purposes of our study, we included a number of questions in the Health Omnibus Survey. Respondents were asked whether they had asthma, and if they answered "yes" they were then asked to respond to the questions listed in Box 1. For the purposes of the interviews, we defined:
Finally, we considered that patients who reported having an AMP, being told about trigger factors and having an action plan were receiving "good management", and examined factors related to good management. We excluded the optimisation of pharmacological intervention from our definition. SPSS was used for all statistical analyses.9 |
Results |
3001 of a possible 4065 people responded (response rate, 73.8%). Of
these 3001 respondents, 558 (18.6%) indicated that they had ever had
asthma, and 521 (93.4%) of these had had their asthma confirmed by a
doctor. Of these 521, 307 (58.9%) indicated that they still had
asthma, representing 10.2% of the total sample and comprising 120 men
and 186 women (one respondent did not indicate sex), with a mean age of
39.4 years (SD, 18.3; range, 15-84 years).
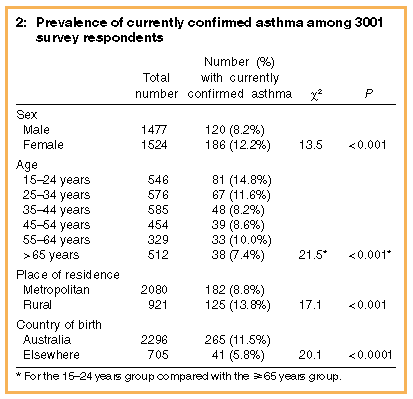
Box 2 (below) shows that current medically confirmed asthma was more common among women than men, and declined in prevalence with increasing age. It was also more common among rural than metropolitan respondents, and among Australian-born respondents than those born elsewhere; this difference remained significant after adjusting for age and sex in logistic regression analyses. There was no relationship between current confirmed asthma prevalence and post-secondary education or annual gross household income, even after adjusting for age and sex. |
Asthma management plans |
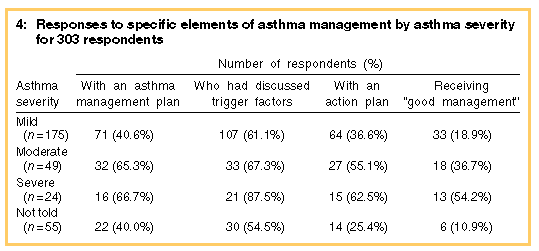
Box 3 (above) summarises our findings on asthma management among respondents
with currently confirmed asthma. Further analyses showed that
having an AMP was not related to age, sex, area of residence, or whether
people had been told their level of severity. However, those who had a
regular doctor were more likely to have an AMP (P = 0.03). Those
who saw both a general practitioner (GP) and specialist were
significantly more likely to have an AMP (81.7%) than those who saw a GP
only (47.6%), specialist only (41.1%) or no one (22.6%; P =
0.02). Among respondents who had been told their level of severity,
those with moderate or severe asthma were more likely to report having
an AMP than those with mild asthma (P < 0.01), after
adjustment for other covariates.
Women were more likely than men to have been told about their asthma severity (86.3% v. 75.0%; chi-squared = 6.1; P = 0.01), and those who had been told tended to be younger than those who had not (t = 3.1; P = 0.07). Among those who had been told, reported level of severity increased with advancing age (t = 5.3; P < 0.01). Severity did not vary by sex, but was greater among rural respondents than metropolitan respondents (chi-squared = 8.6; P = 0.01). The reported prevalence of discussing trigger factors and having an action plan increased with increasing asthma severity (see Box 4). It is notable that only 14 (25.4%) of those who had not been told their asthma severity had an action plan.
Men were more likely than women to have no regular doctor for asthma care (22.7% v. 12.4%; chi-squared = 5.7; P = 0.02); there was no difference by age. Overall, those who had discussed trigger factors did not differ by sex, area of residence or whether they had been told their level of severity. After adjustment for covariates, discussion of trigger factors was more likely among younger respondents (P < 0.05) and those who had a regular doctor (P < 0.01). Among those who had been told their level of severity, logistic regression analysis showed that those with severe asthma were more likely than those with moderate or mild asthma to have discussed trigger factors (P < 0.05). Of those with a regular doctor, source of care was unrelated to discussion of trigger factors. Respondents who reported having an action plan did not vary by age, area of residence or whether they had been told their level of severity. Action plans were more common among women (P < 0.05) and those who had a regular doctor (P < 0.05), and among those who had been told they had moderate or severe asthma than mild asthma (P < 0.01). For respondents with a regular doctor, source of care was unrelated to having an action plan. |
Good management | Seventy-one respondents with currently confirmed asthma (23.3%) were receiving "good management". Good management was unrelated to age, sex, area of residence or whether respondents had been told their level of severity, but was more likely among those who had a regular doctor (P < 0.05). Among those who had been told their level of severity, those with moderate or severe asthma were more likely to be receiving good management than those with mild asthma (P < 0.001). Of those with a regular doctor, source of care was unrelated to receiving good management. |
Discussion |
Given that the AMP model was initiated in 1989, our finding of a
prevalence of reported use of AMPs of 46%, with much higher
prevalences for certain elements of AMPs, is reassuring. It is
noteworthy that we found AMPs to be more common among people who had
been told their asthma was severe and those with a regular doctor.
Our finding that 39.5% of respondents had an action plan is a somewhat higher result than those of previous reports,10,11 possibly indicating an increase in their use. As we found that reported use of action plans did not vary by age, the different age profile of our study compared with that of Comino and colleagues10 (mean, 39.4 years; range, 15-84 years v. mean, 37.4 years; range, 18-50 years) is unlikely to have contributed to the apparent doubling in prevalence of action plan use that we observed. However, unlike the other study, we included verbal as well as written action plans, and this may have been responsible for the difference. Our study was based on self-report, and responses were not validated. However, our method of assessing self-reported asthma has been used in a previous validated epidemiological study.12 There may have been under-reporting in the responses to the questions, even though we used trained interviewers. However, despite these methodological problems, the key measure of the acceptability of the AMP and its elements is their reported use in the community. We are aware that the term "asthma management plan" may have introduced some problems in that our def inition of the AMP encompassed as - sessment of severity, trigger-factor discussions and the development of an action plan. Hence, it is possible that people who reported using an AMP may have been including the other three elements. However, as a main objective was to compare the uptake of the "complete" AMP with that of its individual elements, we believed it was important to include all these questions in the survey. We found that certain elements of the AMP are being adopted more frequently than others, which may indicate that patients find these steps more appropriate to their specific needs, or that doctors (GPs and specialists) find certain elements of the AMP easier to use or implement. GPs are the principal providers of asthma care in the community and it is probable that they have a considerable effect on the uptake of the AMP model. Developing a "complete" management plan may be too onerous a task for a busy GP. Conversely, GPs may find the AMP model does not satisfy their individual needs and, as a consequence, choose specific elements from the AMP model for their everyday practice.13 Over 80% of our respondents, most of whom had mild to moderate asthma, saw a GP for all or part of their asthma care. As there is evidence that GPs' management of asthma is very variable,14,15 it is important to concentrate on providing useful and focused education for GPs. Urgent clarification is needed of the key steps within the AMP model that will reduce mortality and morbidity in people with asthma and improve their quality of life. Interestingly, we found that only 41% of the respondents attending a specialist only had an AMP. As specialists spend more time with their patients and deal with people with more severe asthma, this finding requires further investigation. It has been suggested that some steps of the AMP may be inappropriate for general application. For example, peak flow meters are supposed to be used in both steps 2 and 3, but Ruffin and Pierce have proposed that aiming to have all asthmatic patients record peak expiratory flow over the long term may not be worthwhile,16 and that focusing on, for example, those at risk of dying, those in uncertain clinical situations (e.g., those with exercise-induced asthma) and those who are "particularly interested" in monitoring their asthma would be more cost effective. They emphasised the need for a more rigorous scientific approach to examining "the basis for and benefit of" peak expiratory flow.16 In a more recent paper Gibson et al. state that "action plans have received little controlled evaluation".17 Among 35 adult asthma patients, they found that the current increase in medication recommended in the AMP action plan had a high failure rate. On the other hand, there is evidence that regular review (step 6 of the AMP) can reduce days lost from work or school18 and home visits by GPs,19 and that patient education (step 5) improves symptom control20 and reduces visits to accident and emergency departments.21 The guidelines in the AMP model have come to be accepted as the "gold standard" of asthma management in most countries.22,23 However, what is needed now is a careful re-evaluation 24 to ensure that "unsound practice" does not become formalised.25 A new perspective may be required that embraces the variability in management and clinical encounters.26 Not surprisingly, we found that having a regular doctor is the main determinant of "good management" -- regular review is likely to allow time for the introduction of more steps in the AMP. The challenge in continuing to evaluate an introduced management program in clinical practice is substantial. If over half the population of asthmatic patients have already been exposed to the asthma management plan in part or in full, how can this be done? Small intensive clinical trials with objective outcomes such as peak flow measurements, or case-control studies comparing asthmatic patients with and without good quality of life, could be performed, but would have the disadvantage of not being generalisable to the population at large. Large population studies with specific outcome measures would rely on the outcome measures being validated against accepted criteria of asthma control. A national project that used specific health outcomes, such as prescriptions of reliever or preventer agents, and monitored hospital admissions for asthma could be used to evaluate interventions introduced on a State or regional basis. To coordinate and cooperate in such a project would present a challenge to organisations involved in asthma management. There is current interest in coordinated care programs for chronic diseases and the time is right to introduce an evaluation strategy for different interventions in asthma. |
References |
(Received 17 Apr, accepted 11 Nov, 1996) |
Authors' details
Research & Health Promotion Unit, Royal Australian College of General Practitioners, Adelaide, SA.Justin J Beilby, MPH, FRACGP, Director.
Behavioural Epidemiology Unit, South Australian Health Commission, Adelaide, SA.
Melanie A Wakefield, MA, PhD, Senior Behavioural Scientist.
Department of Thoracic Medicine, The Queen Elizabeth Hospital, Adelaide, SA.
Richard E Ruffin, MD, FRACP, Director.
No reprints will be available. Correspondence: Dr J J Beilby, Department of General Practice, University of Adelaide, Adelaide, SA 5005.
- - To top of article - ©MJA 1997
<URL: http://www.mja.com.au/>
© 1997 Medical Journal of Australia.
Received 25 May 2026, accepted 25 May 2026
- Justin J Beilby
- Melanie A Wakefield
- Richard E Ruffin