End-of-life decisions in Australian medical practice
Helga Kuhse, Peter Singer, Peter Baume, Malcolm Clark and Maurice Rickard
MJA 1997; 166: 191
For editorial comment see Van Der Weyden
and Ashby
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Results - Discussion - Acknowledgement - References - Authors' details
- - - ©MJA1997
Abstract |
Objective: To estimate the proportion of medical
end-of-life decisions in Australia, describe the characteristics
of such decisions and compare these data with medical end-of-life
decisions in the Netherlands, where euthanasia is openly practised. Design: Postal survey, conducted between May and July 1996, using a self-administered questionnaire based on the questionnaire used to determine medical end-of-life decisions in the Netherlands in 1995. Participants: A random sample of active medical practitioners from all Australian States and Territories selected from medical disciplines in which there were opportunities to be the attending doctor at non-acute patient deaths, and hence to make medical end-of-life decisions. Main outcome measure: Proportion of Australian deaths that involved a medical end-of-life decision, using ratio-to-size estimation based on the sampled doctors' responses to the questionnaire. The response rate was 64%. Results: The proportion of all Australian deaths that involved a medical end-of-life decision were: euthanasia, 1.8% (including physician-assisted suicide, 0.1%); ending of patient's life without patient's concurrent explicit request, 3.5%; withholding or withdrawing of potentially life-prolonging treatment, 28.6%; alleviation of pain with opioids in doses large enough that there was a probable life-shortening effect, 30.9%. In 30% of all Australian deaths, a medical end-of-life decision was made with the explicit intention of ending the patient's life, of which 4% were in response to a direct request from the patient. Overall, Australia had a higher rate of intentional ending of life without the patient's request than the Netherlands. Conclusions: Australian law has not prevented doctors from practising euthanasia or making medical end-of-life decisions explicitly intended to hasten the patient's death without the patient's request. |
Introduction |
In Australia, the practice of euthanasia or physician-assisted
suicide (Box 1) is unlawful, except in the Northern Territory. It is,
however, widely recognised in common law (in some Australian States
and Territories in statute law) that mentally competent patients
have a right to refuse medical treatment, and that doctors who comply
with a patient's request for non-treatment are not generally deemed
to have acted unlawfully or to have practised euthanasia or
physician-assisted suicide, even if their action or omission was
foreseen to lead to the patient's death.
Before the Northern Territory Rights of the Terminally Ill Act 1995, the only country where doctors could openly practise euthanasia was the Netherlands. Although this practice is subject to criminal law in the Netherlands, it has been long accepted by strong public support, and the Dutch Parliament has recognised that doctors practising it should not be prosecuted if they comply with certain guidelines.1,2 In 1990, the Dutch Government appointed the Remmelink Commission to review the nationwide practice of euthanasia and other end-of-life medical practices. The investigators used three different methods to ascertain the incidence of these practices. In order to facilitate comparisons with our study, we summarise the findings of their questionnaire study.3 Of all deaths in the Netherlands in 1990 (approximately 129 000), 1.7% were the result of euthanasia and 0.2% were the result of physician-assisted suicide; these deaths complied with Royal Dutch Medical Association guidelines on euthanasia. However, in a clear violation of the guidelines, 1000 deaths (0.8%) involved the administration of drugs with the explicit intention of ending the patient's life, but without the patient's explicit request. In a second nationwide study of medical end-of-life practices in the Netherlands in 1995, by van der Maas et al.,4 the corresponding findings were: euthanasia, 2.3%; physician-assisted suicide, 0.2%; and ending of life without the explicit concurrent request of the patient, 0.7%. Although recent Australian surveys have reported on doctors' attitudes about medical end-of-life decisions,5 and doctors' attitudes to and practice of voluntary euthanasia,6,7 no study has examined the number of deaths in Australia involving medical end-of-life decisions. In this study, we sought to estimate the number of deaths involving a medical end-of-life decision in Australia, to describe the characteristics of such decisions, and to compare these data with those of the Dutch studies. A comparison of medical end-of-life decisions in the Netherlands with a country where euthanasia cannot be practised openly, such as Australia, would indicate whether the Netherlands has a higher rate of ending of life without the patient's explicit request. Australia and the Netherlands have a similar population size (18 million and 15.3 million, respectively) and comparable annual death rates (7.1 and 8.7 per thousand, respectively).8 In the Netherlands in 1995 there were 135 546 deaths,3 while in Australia there were 125 771 deaths from July 1994 to June 1995.9 |
Methods | |
Ethical approval |
Ethical approval for this study was obtained from the Monash University Standing Committee on Ethics in Research on Humans. |
Questionnaire |
We used an English version of the retrospective questionnaire used by
van der Maas et al.4 Our
questionnaire was based on an authoritative translation provided by
the Dutch researchers, so the terminology and meanings of the
questions were comparable, and contained the original 24 items used
in their survey. We considered anonymity to be essential because we
were seeking information about conduct for which doctors would be
liable to prosecution. Therefore, unlike the study by van der Maas et
al.,4 we did not conduct
interviews.
Grouping euthanasia and physician-assisted suicide together, our questionnaire addressed all medical end-of-life decisions, as defined in Box 1. The questionnaire examined the medical action that preceded the death, the doctor's intention, whether an explicit request from the patient was involved, whether a wish had been expressed to hasten death, whether discussion took place with the patient or others, whether the patient was competent when making the request or when participating in discussions, and the estimated length of life shortened. Most questionnaires were completed carefully and consistently. (Copies of the questionnaire are available from the authors.) |
Medical practitioner sample |
We received the addresses of 3000 doctors taken at random from a list of
27000 Australian doctors that had been extracted from the Australian
Medical Masterfile Database (Australasian Medical Publishing
Company, Sydney). Each doctor on the list belonged to one of 27 medical
disciplines where there would be the possibility of making a medical
end-of-life decision (i.e., being the attending doctor at a
non-acute death) (Box 2). The sample of doctors in the study by van der
Maas et al.4 consisted of
those who had attended deaths where the cause of death was highly
likely to have involved making a medical end-of-life decision (as
determined from death certificates).
Australia does not have a national Death Certificate Register for identifying causes of death and attending doctors, as in the Netherlands. Therefore, the 27 medical disciplines (also extracted from the Australian Medical Masterfile Database) in our study were chosen to be as comparable as possible with the broader categories of doctors (cardiology, surgery, internal medicine, respiratory medicine [pulmonology], neurology, general practitioners and nursing home physicians) who were attendant to 87% of hospital deaths and nearly all deaths outside hospitals in the Netherlands.4 Between May 1996 and July 1996, we sent questionnaires to the random sample of 3000 doctors in the selected medical disciplines. The sampling method was chosen to reflect the wider distribution of doctors in Australia with regard to sex, age, medical discipline and State or Territory of residence. The response rate, after a second mailing to non-respondents, was 1918 questionnaires (64%). The initial questions on the questionnaire narrowed the field of respondents to include the 1361 doctors who had attended a death within the last 12 months. These doctors were asked to recall the most recent death they had attended during that period. The field was further narrowed by excluding doctors who, in respect of that death, had had no contact with the patient until after death or where the death had been sudden and totally unexpected. Of the remaining field of 1112 doctors who had attended a death where there was an opportunity to make a medical end-of-life decision (i.e., a non-acute death), 800 doctors made a decision intended either to shorten life or foreseen as probably or certainly shortening life, and 312 doctors did not make such a decision. |
Statistical analysis |
The percentages and confidence intervals regarding doctors
were computed using standard formulas for the estimation of
proportions under simple random sampling.10 The sampling scheme regarding deaths was equivalent to two-stage cluster sampling. Each
selected doctor was asked for details regarding only the most recent
death he or she had attended in the past 12 months. Thus, the
percentages of deaths and corresponding confidence intervals were
computed using the usual ratio-to-size estimator for such sampling.10,11 The virtue of the ratio-to-size estimator was that it could take into account differences in the rates of death that the different doctors in our sample attended in the normal course of their duties (each doctor was asked to indicate the number of deaths they would attend on average within a certain period). For example, oncologists and general practitioners in our sample were each asked about only one death, but the differences in the number of deaths they normally attend were taken into account by the ratio-to-size method when extra polated to percentages of Australian deaths. Surveyed doctors' responses were weighted in these statistical extrapolations in proportion to the number of deaths they normally attend. A consequence of the differential weightings involved in the ratio-to-size method, however, is that there is no simple way of deriving the proportion of deaths in Australia that were preceded by a medical end-of-life decision from our sample of doctors who reported on their decision with regard to the most recent death they had attended. Furthermore, the confidence intervals take into account possible differences in attitudes towards end-of-life decisions between doctors and the fact that each respondent was asked about only one death. |
Results | |
Survey response rates | From the 3000 doctors who were sent questionnaires, we received responses from 1918 doctors (64%). There was no significant difference in response rate for men versus women (chi-squared test, 3.03; 1 degree of freedom [df]), nor between the States and Territories (chi-squared test, 1.94; 7 df). The response rate did, however, differ significantly with age, ranging from 74.9% for the under-35 years age group to 50.5% for the 56-65 years age group (chi-squared test, 26.73; 4 df). The response rate also differed significantly between different categories of medical discipline: there was a higher response rate from doctors in Groups A and B (116 and 340 doctors, respectively), and a lower response rate from doctors in Group C (1265 doctors) (chi-squared test, 160.4; 2 df). One hundred and ninety-seven doctors either did not state their medical discipline or indicated that it did not fall into one of these groups. (Further data on respondents' medical discipline, age, sex and State or Territory of residence are available from the authors.) |
Medical end-of-life decisions: medical practitioner sample |
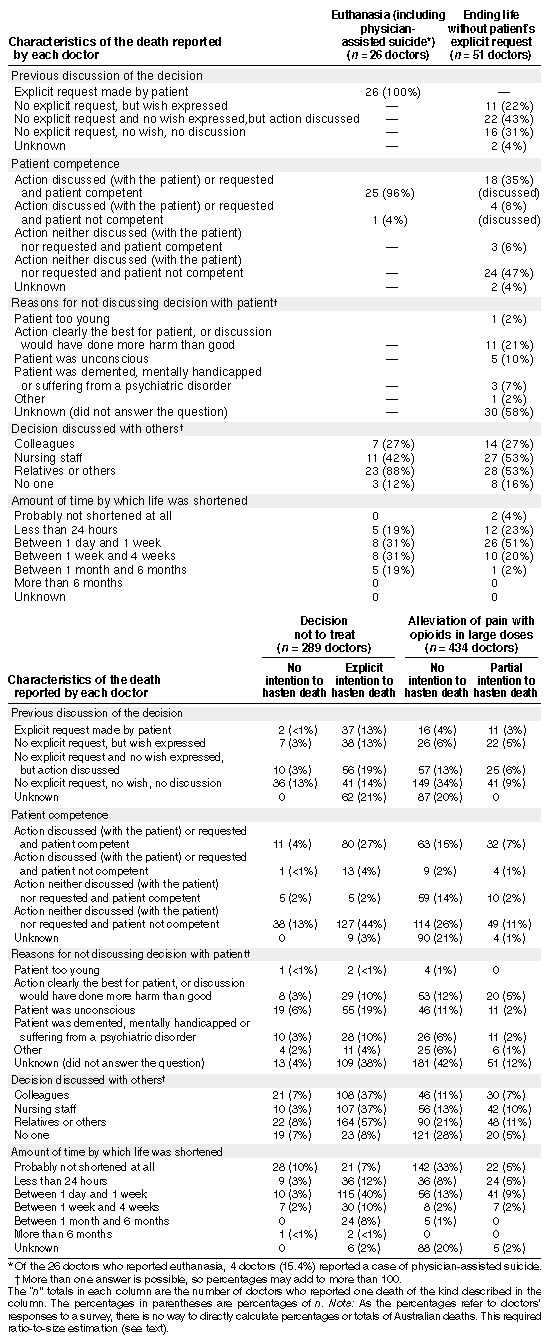
Box 3 shows the characteristics of the deaths reported by the 800
doctors in our study who made medical end-of-life decisions. There were no significant differences with regard to sex (chi-squared test, 0.94; 1 df), State or Territory
of residence (chi-squared test, 1.07; 7
df) or medical discipline (chi-squared test, 4.06; 3 df) between the 800 doctors who made medical end-of-life
decisions and the 312 who did not make such a decision. There was,
however, a marginally significant difference in the age
distribution (chi-squared test,
11.50; 4 df; P=0.02). There was a higher than expected number
of doctors aged between 56-65 years who did not make such a decision.
The medical end-of-life decisions reported by the 800 doctors were as follows: 26 doctors (3.2%) reported euthanasia; 51 doctors (6.4%) reported ending the patient's life without the patient's explicit request; 289 doctors (36.1%) reported making a decision not to treat, of which 55 doctors (19%) reported no intention to hasten death, and 234 doctors (81%) reported an explicit intention to hasten death; and 434 doctors (54.2%) reported alleviating the patient's pain with opioids in large doses, of which 335 doctors (77.2%) reported no intention to hasten death, and 99 doctors (22.8%) reported a partial intention to hasten death (Box 3). We are planning to publish further analysis of the data at a later date. |
Medical end-of-life decisions: proportions of Australian deaths |
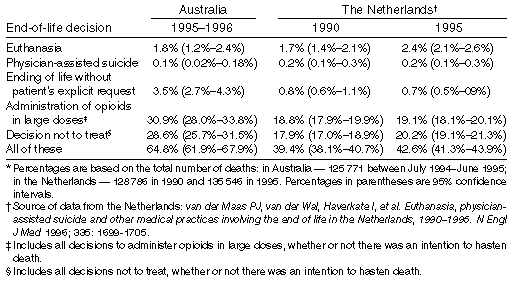
Box 4 shows the proportion of Australian deaths (acute and non-acute)
that involved a medical end-of-life decision. The results in Box 4 and
the results discussed below are based on an extrapolation of the data
from Box 3 by means of ratio-to-size estimation (see Methods). A
medical decision either partly or explicitly intended to hasten
death or not prolong life occurred in 36.5% (±3.5%) of all Australian
deaths. In almost half (17.8% [±2.9%]), there had been no explicit
request from the patient, nor had there been any discussion of ending
the patient's life, and the doctor did not believe that the patient had
expressed a wish for death to be hastened.
Euthanasia and physician-assisted suicide Ending of life without an explicit request from the patient
In 0.7% of all Australian deaths, attending doctors (who were asked to give as many reasons as applied) stated that they did not discuss with the patient the possible hastening of death by prescribing, supplying or administering drugs because the patient was unconscious, demented or mentally handicapped. In 0.5% of all Australian deaths, attending doctors felt that the act of hastening death was "clearly the best one for the patient", or that "discussion would have done more harm than good". Decisions not to treat Therefore, in 14.3% (±2.8%) of all Australian deaths, the death was preceded by a medical decision to withhold or withdraw treatment with the explicit intention of not prolonging life or of hastening death, despite the fact that the decision was not based on an explicit request from a patient, there was no discussion with the patient about whether to hasten death by the omission of treatment, and the doctor did not believe that the patient had expressed a wish for death to be hastened. In almost all of these cases (14.1% of all deaths) the doctor did not consider the patient capable of assessing his or her situation and making a decision about it. In 0.16% of all Australian deaths, the doctor did consider the patient capable of assessing his or her situation and making a decision about it, but intentionally hastened death by forgoing treatment, without discussing this with the patient. In 10.5% (±2.7%) of all Australian deaths, attending doctors (who were asked to give as many reasons as applied) stated that they did not discuss with the patient the possible hastening of death by withholding or withdrawing treatment because the patient was unconscious. Dementia or mental handicap was offered as the reason in 2.6% of all Australian deaths. In 1.6% of all Australian deaths, the attending doctor felt that the decision "was clearly the best one for the patient" or "discussion would have done more harm than good". Alleviation of pain and/or symptoms with opioids Amount of time by which life was shortened
|
Discussion |
One of the main findings of our study was that 30% (±3.3%) of all
Australian deaths were preceded by a medical decision explicitly
intended to hasten the patient's death: doctors prescribed,
supplied or administered drugs with the explicit intention of ending
the patient's life in 5.3% (±1%) of these deaths, and withdrew or
withheld life-prolonging treatment with the explicit intention of
not prolonging life or of hastening death in 24.7% (±3.1%) of these
deaths.
Our study shows that Australia had a significantly higher rate of intentional ending of life without the patient's consent, both through the administration of drugs and by withholding or withdrawing treatment, than the Netherlands. Overall, 36.5% (±3.5%) of all Australian deaths involved a medical decision either partly or explicitly intended to hasten death or not prolong life, compared with 19.5% of deaths in the Netherlands.4 Further comparisons with the data from the Netherlands are shown in Box 5. The difference in the rates of euthanasia between the two countries was not statistically significant. However, the rates of intentionally ending life without an explicit request from the patient were significantly higher in Australia than in the Netherlands (P < 0.0001). In 22.5% (±3.1%) of all Australian deaths, doctors withheld or withdrew treatment from patients, without the patient's explicit request, with the explicit intention of ending life. No comparable 1995 figure for the Netherlands was available (the 1991 figure was 5.3%), but the 1995 figure for all decisions to forgo treatment with an explicit intention of hastening death or not prolonging life in the Netherlands was 13.3%.4 If we classify euthanasia as all cases in which death is "intentionally accelerated by a doctor,"12 30% of all Australian deaths (or 37000 cases) would be cases of euthanasia. The comparable 1995 figure for the Netherlands was 16.6%. The response rate of 64% to our questionnaire was adequate to give a broad picture of medical end-of-life decisions in Australia, but all postal surveys are subject to some degree of non-response bias. The validity of our observations and comparisons is limited by the degree to which our study can be compared with the studies from the Netherlands. Although we strove to obtain a sample population of Australian doctors as comparable as possible to the sample in the study by van der Maas et al.,4 the 27 medical disciplines we selected may not have matched exactly the groups of doctors in their study. Furthermore, in our study there was a higher response rate from doctors whose medical discipline belonged to Groups A and B, and a lower response rate from those in Group C (Box 2). An analysis of the responses of doctors in each of these categories indicates that, in so far as this response bias had any effect on our results, this effect would have been to reduce the reported rate of euthanasia and ending of a patient's life without an explicit request. Cultural differences between Australia and the Netherlands could have accounted for some of the differing responses to the questionnaire. In the Netherlands, the community has a different relationship with primary care doctors compared with Australians, which may account for some of the differences in results. In the Netherlands, most primary care is provided by the huisarts ("home doctor"), the general practitioner or family doctor, either in the patient's home or in the doctor's home surgery. All Dutch patients have a personal huisart, who usually serves a practice of about 2300 people, lives in the area and makes frequent house calls when a patient is ill. This allows for close and enduring contact between the doctor and the patient, and distinguishes the delivery of primary care in the Netherlands from the increasingly institutionalised delivery of primary care in Australia. However, our study undermines suggestions that the rate at which doctors intentionally end patients' lives without an explicit request is higher in a country where euthanasia is practised openly (the Netherlands) than in a comparable country which has not allowed euthanasia to be practised openly, such as Australia. Although Australian law recognises a right to refuse treatment, it generally prohibits the intentional termination of life, whether by act or omission.13 Our findings, together with the previously cited studies of doctors in Victoria and New South Wales,6,7 suggest that Australian law has not prevented the practice of euthanasia or the intentional ending of life without the patient's consent. Our study shows that, while 30% (±3.3%) of all Australian deaths were preceded by an action or omission explicitly intended to end the patient's life, in only 4% was the decision taken in response to an explicit request from the patient. Far more doctors in our sample intentionally hastened death by forgoing (withholding or withdrawing) treatment than by prescribing, supplying or administering drugs with the explicit intention of ending life. For the purposes of this comparative study, we used the same narrow definition of euthanasia (the administration of drugs with the explicit intention of ending the patient's life, at the patient's request) that was used by van der Maas et al.4 Traditionally, "euthanasia" has been defined more broadly: "an action or an omission which of itself or by intention causes death, in order that all suffering may in this way be eliminated."14 This study suggests that the contemporary focus on euthanasia in the narrow sense may be too limited, at least if the aim is to prevent patients having their lives shortened by medical end-of-life decisions being made without their consent. Our study raises the question of why some Australian doctors choose intentionally to end the lives of some of their patients without the patients' consent, especially in situations where the patient is competent and could be consulted. While this issue remains the subject of further empirical research, it may be that, because existing laws prohibit the intentional termination of life, doctors are reluctant to discuss medical end-of-life decisions with their patients lest these decisions be construed as collaboration in euthanasia or in the intentional termination of life. |
Acknowledgement | This study was supported by a grant from the National Health and Medical Research Council. Responsibility for the views expressed is that of the authors alone. |
References |
|
Authors' details
Centre for Human Bioethics, Monash University, Clayton, VIC.Helga Kuhse, PhD, Director; Peter Singer, FAHA, FASSA, Deputy Director; Maurice Rickard, PhD, NHMRC Research Officer.
School of Community Medicine, University of New South Wales, Sydney, NSW.
Peter Baume, MD, FAFPHN, Professor.
Department of Mathematics, Monash University, Clayton, VIC.
Malcolm Clark, PhD, Senior Lecturer.
No reprints will be available from the author.
Correspondence: Associate Professor H Kuhse, Centre for Human Bioethics, Monash University, Clayton, VIC 3168.
E-mail: helga.kuhse AT arts.monash.edu.au
- - - To top of article - ©MJA 1997
<URL: http://www.mja.com.au/>
© 1997 Medical Journal of Australia.
1: Definitions of medical end-of-life decisions4
Euthanasia:
The administration of drugs with the explicit
intention of ending the patient's life, at the patient's request.
Physician-assisted suicide:
The prescription or supplying
of drugs with the explicit intention of enabling the patient to end his
or her own life.
Ending of life without the patient's explicit request:
The
administration of drugs with the explicit intention of ending the
patient's life, without a concurrent, explicit request by the
patient.
Alleviation of pain and symptoms with opioids:
The
administration of doses large enough so that there was a probable
life-shortening effect.
A decision not to treat:
The withholding or withdrawing of
potentially life-prolonging treatment.
2: Medical disciplines in Australia that involve the possibility of doctors making medical end-of-life decisions*
Group A:
Emergency medicine, intensive care, neonatology, medical oncology, palliative care, renal medicine, cardiothoracic surgery.
Group B:
Cardiology, clinical haematology, geriatric medicine, general medicine/general physician, immunology, infectious diseases, radiation oncology, respiratory medicine, abdominal surgery, neurosurgery, vascular surgery, gynaecological oncology, otorhinolaryngology.
Group C:
Breast surgery, endocrinology, gastroenterology, general practice, general surgery, neurology, urological surgery
* Participating doctors were asked to nominate the group containing the medical discipline in which they practise. Medical disciplines were extracted from the Australasian Medical Masterfile Database.
Received 9 June 2026, accepted 9 June 2026
- Helga Kuhse
- Peter Singer
- Peter Baume
- Malcolm Clark
- Maurice Rickard