Hyponatraemia and death after "ecstasy" ingestion
Michael J A Parr, Heather M Low and Paull Botterill
A 15-year-old girl collapsed with respiratory arrest after taking "ecstasy" at a "dance party". She presented to hospital with hyponatraemia and cerebral oedema and later died. We postulate that ingestion of large amounts of water contributed to the hyponatraemia. Advice to those using ecstasy at dance parties should be modified to suggest moderate fluid intake only and to emphasise the need to seek prompt medical attention for non-resolving symptoms.
MJA 1997; 166: 136
For comment see White et al.
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Introduction - Clinical record - Discussion - Acknowledgements - References - Authors' details
- ©MJA1997
Introduction | Recent deaths associated with ingestion of the illicit drug "ecstasy" have attracted widespread publicity and debate about the cause of death. Ecstasy (3,4-methylenedioxymethamphetamine; MDMA) is an ampheta mine derivative which has short-term hallucinogenic and stimulant effects, but in the long term may deplete brain serotonin by reducing numbers of serotonergic nerve terminals.1 Previous ecstasy-related deaths have involved hyperthermia, rhabdomyolysis, coagulopathy and cardiac toxicity.2 We report a death after ecstasy ingestion associated with hyponatraemia, a less well known complication. |
Clinical record |
A previously healthy 15-year-old girl was admitted to the Intensive
Care Department in coma after a respiratory arrest.
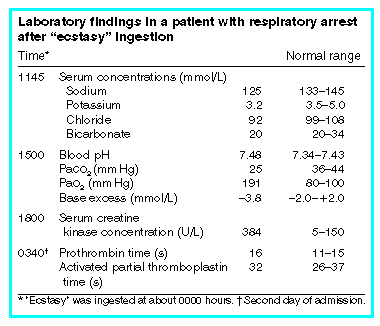
The evening before admission, she had been at a "dance party", where she had taken MDMA at about midnight. She was also believed to have drunk large quantities of water at the party, as then advised by health authorities (e.g., United Kingdom Health Education Authority, and National Poisons Unit), to counteract the hyperthermic effects of MDMA. About 0500, while still at the dance party, she began to vomit. After leaving the party she rested at a friend's house, where she had episodes of dry retching, impaired consciousness, confusion and some abnormal twitching movements. At 1000, about ten hours after ingestion of the MDMA, she was still drowsy and confused, and then collapsed with respiratory arrest while being walked downstairs. There was an estimated 12 minutes of hypoventilation and apnoea, with no cardiopulmonary resuscitation until an ambulance crew arrived. At 1023, on arrival of the ambulance crew, she was found to be in sinus tachycardia with palpable pulses, and she was intubated and ventilated by the crew. Spontaneous cardiac output was maintained throughout. She received naloxone, Hartmann's solution (1000 mL) and polygeline (Haemaccel, Hoechst) (500 mL) before arrival at hospital. At 1118, in the Emergency Department she was found to have: Glasgow Coma Scale score, 3; heart rate, 110 bpm; blood pressure, 80/50 mmHg; temperature, 32.8oC. She had bilateral papilloedema, fixed dilated pupils, no eye movements, no corneal, gag or cough reflexes and no reactions to pain. The hypotension did not respond to a further 1000 mL of 0.9% saline, and a noradrenaline infusion was started. This corrected the hypotension but did not improve the neurological status. At 1145, results of biochemical tests of blood taken before treatment in the Emergency Department showed reduced concentrations of serum electrolytes, suggesting haemodilution (see Box [below]). The haemodilution was corrected within six hours with infusion of 0.9% saline, moderate fluid restriction (total fluids, 60 mL/hour) and diuresis with frusemide and mannitol.
At 1205, a chest x-ray revealed changes consistent with pulmonary oedema, and at 1245 computed tomography of the brain showed cerebral oedema with marked effacement of basal cisterns and inferior displacement of the brainstem. An electrocardiogram at 1400 was normal. Blood-gas analysis at 1500 showed respiratory alkalosis. Maximum serum creatine kinase level was raised, and there was no sign of coagulopathy (see Box [above]). On the second day of admission, the patient was making spontaneous efforts to breathe (on the ventilator) but otherwise her neurological status had not changed. She required noradrenaline to maintain blood pressure but had no cardiac arrhythmias. A nuclear magnetic resonance scan confirmed diffuse cerebral oedema, with decreased blood flow within the major cerebral vessels. Overnight, the patient deteriorated, developing diabetes insipidus and ceasing to breathe spontaneously. On the third day of admission, results of clinical examination were consistent with a diagnosis of brain death, and a cerebral angiogram confirmed this diagnosis. Postmortem findings showed diffuse brain swelling, with cerebellar tonsillar herniation and pituitary necrosis. Analysis of antemortem urine and blood revealed MDMA at levels of 430 ng/mL and 0.05 mg/L, respectively. No other drugs were detected. |
Discussion |
We report the death of a previously well young girl after ingestion of
MDMA. The cause of death was thought to be hypoxic encephalopathy
after respiratory arrest following acute water intoxication
secondary to ingestion of MDMA. It would seem likely that
hyponatraemia and cerebral oedema before the respiratory arrest
were major factors in her death.
The cerebral oedema is unlikely to have resulted from hypoxia after the respiratory arrest, as it would then usually be accompanied by bradycardia or asystole, neither of which was present. In addition, there was no evidence that the patient suffered cardiac arrhythmia, toxicity or infarction, which have caused other amphetamine-related deaths.3 The contribution of intravenous therapy to the hyponatraemia, fluid overload and cerebral and pulmonary oedema is unclear. Given the volumes (1500 mL) and osmotic concentrations (hypertonic or isotonic) of the solutions administered, any contribution is likely to have been small. The effects of MDMA are numerous and complex, and severe reactions are unpredictable.1 There have been many reports of MDMA-associated deaths caused by fulminant hyperthermia, coagulopathy and rhabdomyolysis,1 and clinical awareness of these problems seems high. However, many other complications of MDMA ingestion, such as hyponatraemia, may result in death or serious morbidity and have received less publicity. Instances of hyponatraemia after MDMA ingestion have been reported, with postulated causes that include ingestion of large quantities of water, the syndrome of inappropriate antidiuretic hormone secretion (SIADH) and contamination of the MDMA with other chemicals.4-9 Hyponatraemia raises a diagnostic dilemma, as its signs may be indistinguishable from those of MDMA intoxication. 10 There is evidence that morbidity associated with hyponatraemia is highest in children and women and is not related to either the magnitude or duration of the hyponatraemia.11 To our knowledge, this is the first Australian report of a fatality associated with ecstasy in which hyponatraemia and cerebral oedema appeared to be the main pathological processes. However, dissecting out the various factors involved in the death is extremely difficult. The roles of MDMA, the dance party environment, water ingestion, hyponatraemia, cerebral oedema, hypoxia, hypotension and SIADH are intertwined. The dance party environment encourages heavy exercise in a hot environment, with the advice to drink plenty of water. In the presence of high salt losses, this may produce hyponatraemia. Water ingestion may become uncontrolled as the individual attempts to treat symptoms or as the MDMA impairs rational judgement or possibly stimulates compulsive repetitive behaviour.12 Cerebral oedema as a result of hyponatraemia is well recognised and may result in tentorial herniation, respiratory arrest and cerebral hypoxia.11 SIADH has also been implicated in ecstasy-associated hyponatraemia.9 Although the mechanism is unclear, animal research suggests that serotonin increases secretion of antidiuretic hormone.13 Given the many people who take ecstasy without apparent ill-effect, it has acquired a safe reputation. Among the many adverse reactions, we must now include life-threatening hyponatraemia, which may have the same symptoms and signs as MDMA intoxication. To avoid adverse reactions, individuals using MDMA at dance parties are often advised to rest, avoid overheating, wear loose clothing and drink plenty of cool drinks.14 However, there is no evidence that this prevents adverse reactions. Furthermore, because of the possibility of hyponatraemia, this advice should be modified to suggest ingesting only moderate amounts of liquids. The importance of seeking medical attention promptly for non-resolving symptoms should also be emphasised. |
Acknowledgements | The authors would like to thank the NSW Senior Deputy State Coroner, Mr John Abernethy, for releasing this information for publication, and Dr John A Henry of the National Poisons Unit, Guy's Hospital, London (UK), for assistance with this case. |
References |
(Received 26 July, accepted 21 Nov, 1996) |
Authors' details
Intensive Therapy Unit, Royal North Shore Hospital, Sydney, NSW.Michael J A Parr, MRCP, FRCA, Senior Registrar; currently, Consultant in Anaesthesia and Intensive Care, Frenchay Hospital, Bristol, UK; Heather M Low, FRACP, Senior Staff Specialist.
NSW Institute of Forensic Medicine, Sydney, NSW.
Paull Botterill, FRCPA, Pathologist.
No reprints will be available. Correspondence: Dr H M Low, Intensive Therapy Unit, Royal North Shore Hospital, St Leonards, NSW 2065.
- To top of article - ©MJA 1997
<URL: http://www.mja.com.au/> © 1997 Medical Journal of Australia.
- Heather M Low
- Paull Botterill