Routine pulmonary function tests in young adolescents with asthma in general practice
Peter H Hewson, Elizabeth A Tippett, Danny M Jones, Justin P Madden and Peter Higgs
For editorial comment, see Sawyer and Bowes
Readers may print a single copy for personal use. No further
reproduction or distribution of the articles in whole or in part
should proceed without the permission of the publisher. For
copyright permission, contact the
Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Results - Discussion - Acknowledgements - References - Authors' details
- - ©MJA1996
Abstract Objective: To assess the value of performing routine pulmonary function tests by flow-loop spirometry in young adolescents with asthma.
Design: A prospective clinical study comparing clinical assessment and patients' self- reporting of asthma severity with the results of pulmonary function tests.
Setting: General practice in a small rural community of about 30 000 people.
Patients: Young adolescents with asthma, aged 10-15 years, were enrolled in the study over a two-year period from July 1993 to June 1995 when they presented for either elective, interval assessments or with an acute exacerbation of asthma.
Main outcome measures: Discrepancy between (i) the doctor's and the patient's perception of asthma control (six scale measures) and the consequent management plans, and (ii) the results of pulmonary function tests that indicated less than adequate airway function (i.e., forced expiratory volume in one second as a percentage of predicted vital capacity for height and sex [FEV 1 %] less than 65% or average flow rate over the middle 50% of forced vital capacity as a percentage of predicted normal value [FEF 25%-75% ] less than 65%).
Results: Twenty-seven adolescents with asthma were assessed on a total of 37 occasions. The results of pulmonary function tests did not correlate with asthma symptoms and treatment in 11 of the 37 assessments (30%; 95% confidence interval [CI], 16%-47%). The 11 assessments were performed on eight patients.
Conclusions: This small community-based study of adolescents with asthma supports the view that pulmonary function testing by flow-loop spirometry should be part of the routine assessment of acute and chronic asthmatics. Further study in a larger community is needed to clarify the frequency of over- and underestimation of asthma severity in this difficult age group.
MJA 1996; 165: 469-472
Introduction
Older children and adolescents often have difficulty assessing the severity of their asthma, 1 and consequently pulmonary function tests have been recommended for those with frequent or chronic asthma who are able to perform spirometry adequately. 2-4 Pulmonary function testing by flow-loop spirometry allows measurement of forced expiratory volume in one second as a percentage of the predicted vital capacity for height and sex (FEV 1 %), and forced mid expiratory flow (FEF 25%-75% : the average flow rate over the middle 50% of forced vital capacity).While peak flow monitoring and FEV 1 % have been used for decades as a measure of pulmonary function, forced mid expiratory flow is not as well known a measure, but is more sensitive than FEV 1 in detecting small airways obstruction. 2 Pulmonary function tests have been shown to be useful in adults, but there are few studies of their useful ness in children and young adolescents with asthma. One study found that 17% of apparently well children with asthma had a low forced expiratory volume in one second / vital capacity ratio (FEV 1 /FVC) and 54% had low forced mid expiratory flow (FEF 25%-75% ), suggesting that, without these tests, both patients and doctors were unable to detect mild degrees of broncho constriction, especially of the smaller airways. 5
To date, no study has described the use of pulmonary function tests as part of routine community medical practice in young adolescents. In fact, in some centres, spirometry tests are not yet done routinely in chronic asthmatics in this age group. We performed pulmon ary function tests in adolescents with asthma in an Australian country setting, comparing patients' and doctors' clinical assessment of asthma severity with the results of routinely performed pulmonary function tests.
Methods This two-year study took place in Colac, Victoria (population, 14 000; regional population, 30 000) between July 1993 and June 1995. All young adolescents with asthma (recurrent wheeze responsive to bronchodilators) between the ages of 10 and 15 years pre senting to their general practitioner Monday to Friday either for an elective asthma management review, or because of an acute exacerbation of their asthma, were assessed by the general practitioner and included in the study. No adolescents were excluded from the study or refused to participate. Appointments for elective management reviews (interval assessments) had been made weeks in advance. An acute exacerbation of asthma was defined as an appreciably more severe wheeze and cough than usual (as assessed by the general practitioner).
The severity of symptoms and the perception of asthma control were assessed by the general practitioner, giving day and night symptom scores (0-5), and a wheeze description, based on questioning of the patient. The doctor and the patient then separately graded asthma control as excellent, very good, fair, poor, or very poor. (The scoring system is given in the footnote to the Table).
Forced expir atory volume in one second (FEV 1 ) and forced mid expiratory flow (FEF 25%-75% ) were measured -- on the same day if it was a daytime presentation (usually immediately after the clinical assessment) or the morning after if it was an evening presentation. An Alpha Vitalograph spirometer (Fisher & Paykel, Melbourne, Vic.) was used and the tests were conducted by the senior physiotherapist at Colac Hospital (E A T), who had attended the spirometry technician's course run by the Department of Respiratory Medicine, Alfred Hospital, Melbourne. The tests were repeated if the assessment was judged to be inadequate by the physiotherapist. The effect of bronchodilators on pulmonary function tests was determined in all patients, with recordings being taken 20 minutes (in one patient 25 minutes) after bronchodilator therapy.
The pulmonary function tests were done without knowledge of the clinical status of the patient and the results were made available to the treating doctor if requested. The patients' previous home peak expiratory flow measurements were also recorded, as was peak flow measured with the spirometer.
The results of the pulmonary function tests were considered not to correlate with asthma symptoms and treatment, and to be likely to lead to a change in asthma management, if:
During an interval assessment:
- The patient complained of no, few or only moderate symptoms, the doctor felt asthma control was excellent, very good or reasonable, respectively, and did not change treatment, but FEV 1 % (normal, > >80%) or FEF 25%-75% (normal, > >65%) was less than 65%.
- The patient and the doctor thought control was poor, the dose of maintenance asthma therapy was increased, but pulmonary function tests revealed no evidence of bronchospasm.
- The patient and the doctor felt current asthma control was excellent or very good, no increase in dose of inhaled steroids was suggested and no oral corticosteroids were prescribed, but FEV 1 % or FEF 25%-75% was less than 65%.
Of the 22 interval assessments, 16 (73%) were in patients taking inhaled corticosteroids (in 11 of these the patients were taking more than 700 µg inhaled corticosteroids per day, and in five FEF 25%-75% values were less than 65%). In two (9%) interval assessments peak expiratory flows were less than 300 L/min (in only one of the assessments with FEF 25%-75% less than 65% were peak flows less than 300 L/min).
Of the 15 acute exacerbation assessments, eight (53%) were in patients taking inhaled corticosteroids (in three of these the patients were taking more than 700 µg inhaled corticosteroids per day). In five (45%) acute exacerbation assessments peak expiratory flows were less than 300 L/min (four were unavailable).
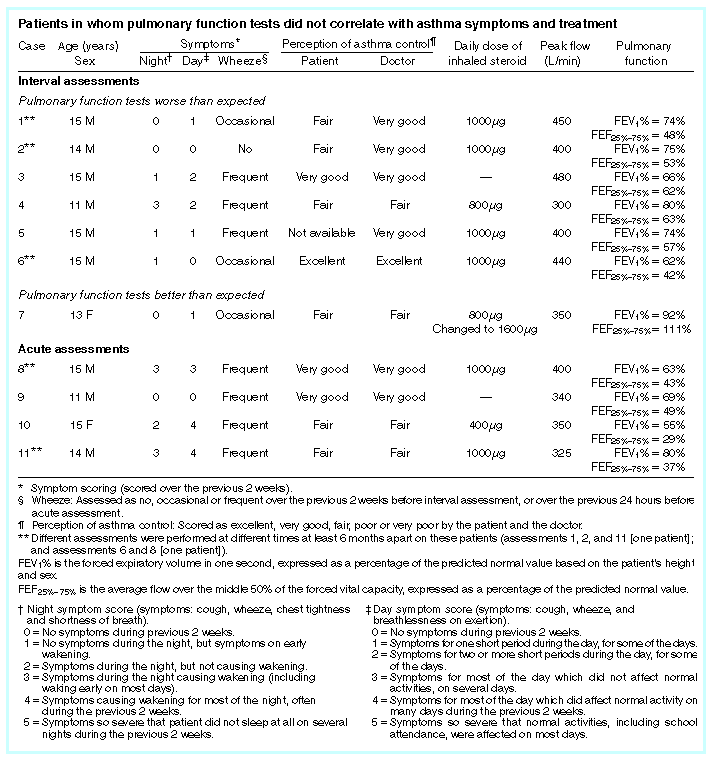
Details of the patients whose pulmonary function tests did not
correlate with asthma symptoms and treatment are given in the Table.
Overall, pulmonary function tests not correlating with clinical and
patient assessment of asthma severity were found in 11 of 37
assessments (30%; 95% confidence interval [CI], 16%-47%). If only
those tests performed within four hours of the clinical assessment
are included, pulmonary function tests in 10 of 33 assessments (30%;
95% CI, 15%-46%) did not correlate with asthma severity. Pulmonary
function tests in six of the 22 interval assessments (27%; 95% CI,
11%-50%) showed FEV 1 % or FEF 25%-75% to be less than 65% when
management had not been changed after clinical assessment (Cases
1-6). During acute exacerbations, four of 15 assessments (27%; 95%
CI, 8%-55%) showed FEV 1 % or FEF 25%-75% values to be less
than 65% when no change in treatment had been made on clinical grounds
(Cases 8-11). Tests in one patient (Case 7) showed normal pulmonary
function after clinical assessment had suggested poor asthma
control. Her pulmonary function tests were carried out within two
hours of the clinical evaluation; her inhaled cortico steroid dose
had been doubled.
Discussion This community-based study of all young adolescent asthmatics presenting to their general practitioners in a country town found that in 30% of assessment opportunities the results of pulmonary function tests were likely to change management. This proportion was maintained even if slightly delayed pulmonary function tests (4-14 hours) were excluded. This result is comparable with previously published findings that 54% of apparently well asthmatics had lower than expected FEF 25%-75% values at follow-up, despite being asymptomatic. 5
At interval assessments in which management had not been changed and the results of pulmonary function tests were low, three of five adolescents (Table: assessments 1, 3-6) reported frequent wheeze. The other two thought their asthma was well controlled; however, their FEF 25%-75% values were 62% and 42%, respectively. In these patients peak flows, measured at home and by spirometry, were all above 300 L/min and this may have accounted for ALIGN=TOP the reluctance to change therapy. However, it has been shown previously that peak flow results can be misleading, and widely varying optimal values can be expected. 3 A low expectation of what can be achieved in frequently symptomatic patients may contribute to a less aggressive approach in adolescents with asthma.
The rather frequent use of inhaled corticosteroids in relatively high doses in this small sample of asthmatics suggests that a more objective measure of asthma status should be used. Potential overuse of inhaled corticosteroids in these growing young people may not always safeguard those at risk of more severe asthma. Six of 11 patients (55%) taking more than 700 µg inhaled corticosteroids had FEF 25%-75% values less than 60%, suggesting that in these patients an even higher dose of inhaled corticosteroid may be required. More specific alterations to long term inhaled steroid use would be possible if pulmonary function tests were performed regularly.
During assessments for acute exacerbation the rate of pulmonary function tests not correlating with symptoms was still high (27%) and the FEF 25%-75% was worryingly low in three patients in whom management was not altered (Table: assessments 8, 9, 10, and 11). These three adolescents all had frequent wheeze, but presumably were not distressed, with peak flows (measured at home and by spirometry) above 320 L/min. Pulmonary function tests gave an indication of small airways disease which they were not aware of or was not revealed by their peak flow measurements.
Our study involved a small number of patients and the confidence intervals calculated suggest a larger study is necessary. Nevertheless, data on mortality in asthma indicate that underestimation of asthma severity can be extremely important. Robertson et al. found that about 35% of possibly preventable asthma deaths may have been related to medical practitioner underestimation of asthma severity. 6
The full implications of FEF 25%-75% values in the 55%-65% range is not yet certain. A long term follow-up of asymptomatic patients with values in this range has not yet been done. Most of our patients with low FEF 25%-75% values not correlating with symptoms had values below 55% (Table: 7 of 10 assessments). Thus, even if the implications of an FEF 25%-75% value between 55% and 65% is disputed, the frequency of the lower results suggests more aggressive treatment is required.
This relatively small study of asthmatic adolescents in a small country town strongly supports the view that pulmonary function tests need to be part of the routine assessment of acute and chronic asthmatics.
Acknowledgements
We thank Professor P D Phelan, Department of Paediatrics, University
of Melbourne, for his provocation, encouragement and support; and Mr
Ross Gollan, Senior Lecturer, Department Mathematics and
Statistics, Deakin University.
References
- Sly PD, Landau LI, Weymouth R. Home recording of peak expiratory
flow rates and perception of asthma. Am J Dis Child 1985; 139:
479-482.
-
Landau LI. The value of lung function in guiding drug therapy in
childhood asthma. Eur Respir Rev 1994; 4: 10-14.
-
Phelan PD, Olinsky A, Robertson CF. Respiratory illness in
children, 4th edition. Cambridge: Blackwell Scientific
Publications, 1994; 152-156.
-
Milner AD. Childhood asthma: diagnosis, treatment and
management. London: Martin Dunitz, 1987; 18-38.
-
Bye MR, Kerstein D, Barsh E. The importance of spirometry in the
assessment of childhood asthma. Am J Dis Child 1992; 146:
977-981.
-
Robertson CF, Rubinfeld AR, Bowes G. Deaths from asthma in
Victoria: a 12-month survey. Med J Aust 1990; 152: 511-517.
(Received 19 Sep 1995, accepted 4 Jul 1996)
Authors' details
106 McKillop Street, Geelong, VIC 3220.
Peter H Hewson, MD, FRACP, Consultant Paediatrician.
Colac Hospital, Corangamite Street, Colac, VIC.
Elizabeth A Tippett, DipPhys, Senior Physiotherapist.
2 Connor Street, Colac, VIC.
Danny M Jones, MB BS, DA, DipRACOG, General Practitioner;
Justin P Madden, MB BS, DA, DRCOG, General Practitioner;
Peter Higgs, MB BS, General Practitioner.
No reprints will be available. Correspondence: Dr P H Hewson.
- - To top of article - ©MJA 1996
<URL: http://www.mja.com.au/> © 1996 Medical Journal of Australia.
Received 25 May 2026, accepted 25 May 2026
- Peter H Hewson
- Elizabeth A Tippett
- Danny M Jones
- Justin P Madden
- Peter Higgs




