Prevalence of hepatitis G virus in Queensland blood donors
Len D Moaven, Catherine A Hyland, Ian F Young, D Scott Bowden, Rhonda McCaw, Leigh Mison and Stephen A Locarnini
MJA 1996; 165: 369
Subsequently cited in Moaven L. Should we be screening blood donors for hepatitis G virus? The case for screening. MJA 1998; 169: 373-374
and Wong et al. Should we be screening blood donors for hepatitis G virus? The case against screening. MJA 1998; 169: 375-377
Readers may print a single copy for personal use. No further
reproduction or distribution of the articles in whole or in part
should proceed without the permission of the publisher. For
copyright permission, contact the
Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Blood donors - Serological and biochemical testing - Reverse transcription PCR testing - Results - Discussion - Box - References - Authors' details
- - ©MJA1996
Abstract Objective: To determine the prevalence of hepatitis G virus (HGV) carriage in Queensland blood donors.
Design: Cross-sectional survey with retrospective longitudinal study of HGV-positive donors.
Setting: Brisbane Red Cross Blood Bank, 1995.
Subjects: 100 consecutive blood donors attending the Blood Bank on two days in October 1995 and 20 blood donors with a raised plasma alanine aminotransferase (ALT) level on their last donation.
Outcome measures: Presence of HGV RNA by reverse transcription polymerase chain reaction (RT-PCR) in currently donated blood and in blood samples archived for up to 34 months. RT-PCR used two different reverse transcription methods and three different specific sets of primers and probes.
Results: Five of the 120 blood donors were positive for HGV RNA by all RT-PCR methods (four of the 100 with normal ALT levels [4%] and one of the 20 with raised ALT levels [5%]). Retrospective testing of archived samples showed that four of these five had been persistently HGV RNA-positive for at least two years, while the fifth had been HGV RNA-negative on two donations before becoming HGV RNA-positive. No risk factors were identified for this donor.
Conclusions: A relatively large number of Queensland blood donors (4%) are persistently HGV RNA-positive.
MJA 1996; 165: 369-371
Introduction
S ince the introduction of improved diagnostic assays for hepatitis C virus 1 and increased screening of blood donors, 2 the incidence of post-transfusion hepatitis has been reduced to low levels. However, there are still cases of post-transfusion hepatitis where an aetiological agent is not identified. 3While searching for novel agents that may be associated with post-transfusion hepatitis, two independent groups recently discovered an RNA virus that causes acute and chronic infection in man. 4,5 The two isolates, designated hepatitis G virus (HGV) and GB virus C, respectively, belong to the same species, 6 and findings for one seem applicable to the other. Currently, the only reliable method for determining the prevalence of infection with these viruses is specific reverse transcription polymerase chain reaction (RT-PCR) assay to detect viral RNA. A serological assay to detect carriers of HGV is unlikely to be available in the immediate future, and much of the epidemiology of HGV will rely on RT-PCR-based assays.
From the available RT-PCR data, it appears that HGV is transmitted parenterally, with increased prevalence in injecting drug users and patients who have received multiple transfusions. 4,7,8 HGV has a high prevalence in developed countries, with about 1.5% of volunteer blood donors from the United States and Europe being positive for HGV RNA. 4,8 It is not known whether these positive donors are transiently infected or chronic carriers of HGV.
We examined the prevalence of HGV in Queensland blood donors. As most donors had plasma stored from previous donations, we were also able to collect unique longitudinal data.
Methods
Blood donors
Consecutive blood donors at the Brisbane Red Cross Blood Bank over two
days in October 1995 were asked to participate. The first 100 to sign a
consent form agreeing to be tested for HGV were studied (compliance
was 100%). These donors all had normal plasma alanine
aminotransferase (ALT) levels.
Blood was also collected over a three-month period from 20 donors with a raised ALT level on their most recent donation. Six of the 20 had raised ALT levels on two or more previous donations.
All donors had signed the donor declaration form indicating they did not fall into an "at risk" group. All testing was performed with the approval of the Queensland Red Cross Blood Transfusion Service Ethics Committee.
Serological and biochemical testing All donors were tested for antibodies to hepatitis C virus (HCV), HIV 1, HIV 2 and human T-cell lymphotropic virus (HTLV) and for hepatitis B surface antigen (HBsAg) (Abbott Diagnostics, Chicago, Illinois, USA). They were also screened with a syphilis antibody assay, Sysmic RPR (Diagast, Lille, France). Plasma ALT levels were measured by a microtitre tray assay. 9 Samples positive for HGV RNA were also tested for hepatitis B core specific antibody (Abbott Diagnostics).
Reverse transcription PCR testing For RT-PCR testing, the recommendations of Kwok and Higuchi 10 were followed to prevent sample contamination. Blood samples were collected in acid-citrate-dextrose and plasma was stored at 2 70 o C within two hours of collection. RNA was subsequently extracted from these plasma samples with a guanidine thiocyanate and phenol-chloroform extraction procedure. 11
RT-PCR was performed with random hexamers and two sets of PCR primers from the 5 9 untranslated region and the region encoding the non-structural protein 5a of the HGV genome. These primers are part of an HGV primer and capture probe set commercially available from Boehringer Mannheim (Germany). In addition, RT-PCR was performed with primers from the region encoding the protein 5b, as described previously. 12
If a plasma sample was positive for HGV RNA, a separate aliquot of plasma was retrieved from frozen storage and RNA was extracted and tested with all three primer sets. Samples positive for HGV RNA were also tested for HCV RNA (Amplicor, Roche Diagnostic Systems, Branchberg, New Jersey, USA).
Donors positive for HGV RNA were tested retrospectively by recovering archived frozen plasma samples from previous donations. These samples had been frozen within two hours of collection and stored at 2 30 o C. As controls, archived plasma samples were also recovered from donors negative for HGV RNA. Archived samples were coded and tested blind. In addition, four of the five donors found to be positive for HGV RNA returned subsequently to donate blood and were retested for HGV RNA. These retrospective and prospective samples were tested with the NS5b primers alone.
Results Five of the 120 blood donors were HGV-positive by RT-PCR with all three of the primer sets. These positive donors comprised four of the 100 with normal ALT levels (4%; 95% confidence interval [CI], 1%-10%) and one of the 20 with raised ALT levels (5%; 95% CI, 0.1%-25%). This donor had not had raised ALT levels previously. The remaining 115 donors were negative by all three primer sets. Repeat PCR testing of a separate aliquot of each HGV-positive sample revealed complete concordance of results.
The five HGV-positive donors were negative for hepatitis B core-specific antibody and HCV RNA. All donors were negative for antibodies to HCV, HIV 1, HIV 2 and HTLV, for HBsAg and for syphilis RPR antibody.
Plasma samples from 22 previous donations given by the five HGV-positive donors were also tested for HGV RNA (see Box). Four donors were HGV-positive for all previous donations ( n = 18), made up to 22-34 months previously. The fifth, a 38-year-old man, was HGV-positive from August 1994, but two previous donations (May 1994 and November 1993) were HGV-negative. His ALT level was normal on each occasion and no risk factor or illness could be identified for this donor despite specific questioning about the period May 1994 to August 1994. Potential risk factors were noted for three of the other HGV carriers (see Box).
All HGV-positive donors were well. Four returned for further testing, including the donor who appeared to acquire HGV infection in 1994; they remained HGV-positive on all occasions (up to six months after initial tests).
The control archived plasma samples were tested blindly and found to be HGV-negative.
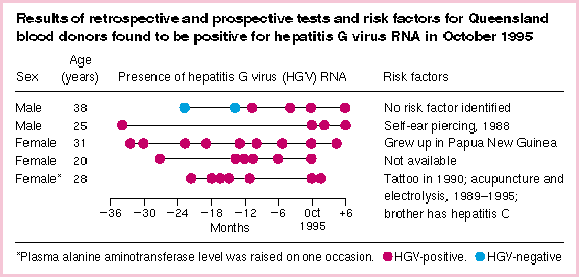
It has yet to be determined why this infection is so prevalent in a group normally assumed to be at low risk for exposure to blood-borne viruses. Mother-to-baby (and early horizontal) transmission may account for the pattern of distribution (analogously to HBV in developing countries). 12 One donor had grown up in a developing country and another had potential risk factors (e.g., tattooing). Even so, one of the donors appeared to acquire HGV infection recently, without evident risk factors. This suggests that there are multiple modes of transmission.
We found that only one of the HGV-positive donors had a raised ALT level, and on only one occasion. Although HGV infection is associated with an early and mild rise in results of liver function tests in some recipients of HGV-infected blood, 4 this is not unusual in acute viral infections. There is currently little evidence that HGV commonly causes chronic liver disease, but this does not preclude association with another disease. Indeed, we would argue that it is unlikely that a positive-strand RNA virus could cause chronic infection and not be associated with a disease syndrome. It is worth noting that with such a high prevalence of HGV in the general population the demonstration of a disease association will have to be particularly rigorous.
The strategy we developed for HGV testing is time consuming and expensive, but, without a reliable serological or alternative virological marker, nucleic acid amplification by PCR remains the method of choice. An alternative to our PCR strategy could be use of a single reliable primer set, with automation of RNA extraction and RT-PCR.
Blood donations may have to be tested for HGV RNA when suitable assays become available for mass screening, especially if evidence emerges that it causes significant disease. A National Health and Medical Research Council working party on novel viral hepatides has been set up in collaboration with the Red Cross Blood Transfusion Service to determine the significance of HGV in blood donations. In the meantime, it is important that recipients of donated blood continue to be advised of the potential complications of heterologous blood transfusion and, specifically, that they may acquire HGV infection. 2 However, currently the clinical significance of HGV infection is unclear and further clinical and epidemiological studies are needed on this new and emerging virus.
References
- Aach RD, Stevens CE, Hollinger B, et al. Hepatitis C virus infection
in post-transfusion hepatitis: an analysis with first and second
generation assays. N Engl J Med 1991; 325: 1325-1329.
-
Sloand EM, Pitt E, Klein HG. Safety of the blood supply. JAMA
1995; 274: 1368-1373.
-
Alter HJ. Transfusion transmitted hepatitis C and non-A, non-B,
non-C. Vox Sang 1994; 67: 19-24.
-
Linnen J, Wages J, Zhen-Yong ZK, et al. Molecular cloning and
disease association of hepatitis G virus: a
transfusion-transmissible agent. Science 1996; 271:
505-508.
-
Simons JN, Leary TP, Dawson JG, et al. Isolation of novel virus-like
sequences associated with human hepatitis. Nat Med 1995; 1:
564-569.
-
Zuckerman AJ. Alphabet of hepatitis viruses [editorial].
Lancet 1996; 347: 558-559.
-
Bowden DS, Moaven LD, Locarnini SA. New hepatitis viruses: are
there enough letters in the alphabet? Med J Aust 1996; 164:
87-89.
-
Dawson GJ, Schlauder GG, Coleman P, et al. Prevalence and clinical
significance of GBV-C [abstract]. Proceedings of the Ninth
Triennial International Symposium on Viral Hepatitis and Liver
Disease; 1996 April 21-25; Rome (Italy). Rome: CpA (Viale
delle Medaglie d'Oro, 342100136), 33: 116.
-
Hyland CA, Douglas R, Mazzocchi R, Young IF. Surrogate testing for
non-A, non-B hepatitis in Queensland, Australia, an ALT microtitre
tray method for screening blood donors. Pathology 1988; 20:
271-274.
-
Kwok S, Higuchi R. Avoiding false positives with PCR. Nature
1989; 339: 237-238.
-
Chemczynski P, Sacchi N. Single-step method of RNA isolation by
acid guanidinium thiocyanate phenol-chloroform extraction.
Anal Biochem 1987; 167: 156-159.
-
Moaven LD, Tennakoon PS, Bowden DS, Locarnini SA. Mother-to-baby
transmission of hepatitis G virus. Med J Aust 1996; 165:
84-85.
(Received 15 May, accepted 9 Aug 1996)
Authors details
Victorian Infectious Diseases Reference Laboratory, Fairfield
Hospital, Melbourne, VIC.
Len D Moaven, FRCPA, Senior Registrar in Virology; D Scott
Bowden, PhD, Senior Scientist (Molecular Virology); Rhonda
McCaw, BSc, Scientist (Molecular Virology); Stephen A
Locarnini, PhD, MRC(Path), Director.
Red Cross Blood Transfusion Service, Brisbane, QLD.
Catherine A Hyland, PhD, Scientist-in-Charge
(Viral Serology); Ian F Young, FRCPA, Director; Leigh
Mison, BSc, Scientist.
Reprints: Dr S A Locarnini, Victorian Infectious Diseases Reference
Laboratory, Fairfield Hospital, PO Box 65, Fairfield, VIC 3078.
E-mail: stephenL AT hna.ffh.vic.gov.au
<URL: http://www.mja.com.au/>
© 1997 Medical Journal of Australia.
We appreciate
your comments.
Received 25 May 2026, accepted 25 May 2026
- Len D Moaven
- Catherine A Hyland
- Ian F Young
- Rhonda McCaw
- Leigh Mison
- Stephen A Locarnini




