Age-specific HIV incidence among homosexually active men in Australia
Matthew G Law, Philip S Rosenberg, Ann McDonald and John M Kaldor
MJA 1996; 164: 715-718.
This article has been published in the Medical Journal of Australia. Readers may print a single copy for personal use. No further reproduction or distribution of the articles in whole or in part should proceed without the permission of the publisher. For copyright permission, contact the Australasian Medical Publishing Company
Abstract - Introduction - Methods - Results - Discussion - Acknowledgements - References - Author's Details - Table - Figure 1 - Figure 2
Register to be notified of new articles by email - To Current Issues list - ©MJA1996
Abstract Objective: To estimate age at HIV infection among homosexually active men in Australia.
Design: Age-specific back-projection estimates of HIV incidence.
Methods: Monthly counts of AIDS among homosexually active men diagnosed by 30 June 1994 and reported by 31 March 1995 were obtained from the National AIDS Registry and were adjusted for reporting delays. The progression rate to AIDS was estimated from a large cohort study of HIV-infected homosexual men, with adjustment for the effect of age at HIV infection and the effect of antiretroviral and prophylactic treatments.
Results: The median age at HIV infection was estimated to have decreased from 31 years of age between 1982 and 1984 to between 23 and 27 years in the periods 1987 to 1989 and 1990 to 1994. Despite the trend to a younger median age at HIV infection during the current epidemic, HIV incidence was estimated to have declined in all age groups from a peak in the mid-1980s. This decline was more pronounced in the older age groups, with more modest reductions in age groups under 30 years.
Conclusion: Most HIV infections among homosexually active men since 1987 appear to have occurred in men aged under 30 years. This has implications for education programs aimed at preventing HIV infection among homosexually active men.
MJA 1996; 164: 715-718
Introduction
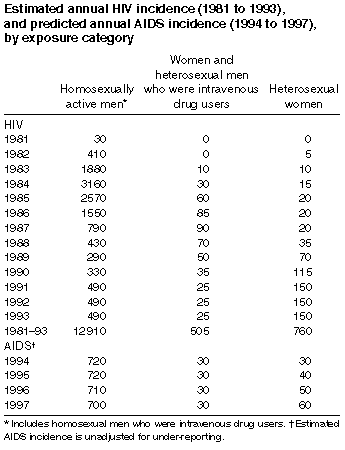
A rapid increase in HIV incidence in Australia in the early 1980s (with a peak of around 3300 cases per year in the mid-1980s, followed by a rapid decline) was reported by both the National Working Group on HIV Projections in 19921 and the Evaluation of the National HIV/AIDS Strategy in 1996.2Cumulative HIV incidence to the end of 1993 was estimated to be between 13 000 to 19 000 cases, with a preferred estimate of 15 200 cases. The estimated annual incidences of HIV infection from 1981 to 1993 for homosexually active men, for heterosexual women, and for women and heterosexual men who were intravenous drug users, are shown in the Box.3About 85% of both AIDS cases and diagnosed HIV infections in Australia have been in men who have had homosexual contact.4 Over the period of the current AIDS epidemic, it could be expected that a new generation of homosexual men has become sexually active and at risk of HIV infection. An important question, therefore, is whether and how HIV incidence among younger homosexually active men has changed over time. The method of back-projection has become the preferred method for estimating past HIV incidence, and for projecting future AIDS incidence, in most developed countries.5-7 Here, using an extension of the back-projection method,8 we estimate the age at HIV infection among homosexually active men in Australia.
Methods Our analyses were based on AIDS cases diagnosed by 30 June 1994 and reported to the National AIDS Registry (NAR) at the National Centre in HIV Epidemiology and Clinical Research by 31 March 1995 in men with a history of homosexual contact, including those who were intravenous drug users. These AIDS incidence data were adjusted for the reporting delay between the time of diagnosis to the time of entry of the case on the NAR.9 All estimates of HIV incidence were adjusted for underreporting of AIDS cases to the NAR, which is currently estimated to be about 10%.3
Age-specific HIV incidence was estimated using the back-projection method suggested by Rosenberg,8 in which the rate of progression to AIDS is assumed to be associated with age.10
To reflect the uncertainty in the rate of progression to AIDS, particularly beyond 10 years following HIV infection, we used two different progression-rate distributions derived from a large-cohort study of HIV-infected homosexual men.11 A faster progression-rate distribution was based on a median "time-to-AIDS" of nine years for people aged 30 at diagnosis of HIV infection, and the rate of progression to AIDS was taken to increase by 1.042 for each year the age at HIV infection was above 30, and to decrease by 1/1.042 for each year the age was below 30. A slower progression rate was based on a median "time-to-AIDS" of 9.8 years and an age-effect of 1.037. As the effect of age on modifying the progression rate to AIDS is uncertain and the assumption of an age-effect would lower the back-projection estimate of median age at HIV infection, we also analysed the progression rates with the age-effects at both zero and half of the above values.
The extended definition of AIDS adopted in Australia in January 1988 was assumed to result in a 10% increase in the rate of progression to AIDS.12 The effect of antiretroviral and prophylactic treatments on the progression rate was incorporated into the analysis by assuming that 20% of HIV-infected people were first diagnosed as HIV positive at diagnosis of AIDS and so would not have received treatment before the diagnosis of AIDS,13 and that zidovudine became available in Australia from mid-1987 and was accepted and tolerated by up to 90% of people with diagnosed HIV infection. The effect of treatment was assumed to be a modest 20% reduction in the rate of progression to AIDS and to gradually diminish during ex- tended use, consistent with randomised clinical trials of zidovudine.14-16 We also did further analyses assuming a stronger treatment effect which corresponded to a 50% reduction in the progression rate.
Back-projections were conducted for five time periods (early 1977 to mid-1981, mid-1981 to mid-1984, mid-1984 to mid-1986, mid-1986 to mid-1989 and mid-1989 to mid-1994) and for five age groups (17 to 20, 21 to 24, 25 to 29, 30 to 39 and 40 to 59 years). To allow direct comparison of estimates of HIV incidence in different age groups and time periods, estimates of HIV incidence in a given age group and time period were standardised by dividing the estimated total number of new HIV infections by the product of the number of age-years and calendar-years.
Results There were 4661 cases of AIDS diagnosed by 30 June 1994 and reported to the NAR by 31 March 1995 among homosexually active men. After adjusting for reporting delays, analyses were based on 4769 cases of AIDS. We did not analyse other exposure categories as there were too few AIDS cases in these categories.
The patterns of HIV incidence were similar for both the faster and the slower progression-rate distributions, with a rapid increase in the annual number of HIV infections in the early 1980s to a peak of between 2600 and 3100 per year in the mid-1980s, followed by a steep decline. The faster progression rate gave a smaller estimate of the cumulative HIV incidence to 30 June 1994 than the slower progression rate: 11 800 HIV infections, compared with 14 700, respectively. Both the pattern of HIV incidence and the cumulative HIV incidence estimated by the age-specific analysis are consistent with the non-age-specific back-projections for homosexually active men shown in the Box.
The median age at HIV infection was similar for both the faster and slower progression-rate distributions (Figures 1a and 1b). As the epidemic developed, there was a decline in the median age at HIV infection, from 31 years in 1982 to 1984, to 23 and 25 years for both the faster and slower progression-rate distributions, respectively, in 1987 to 1989, and to 25 and 27 years in 1990 to 1994. The age-effect of zero on the progression rate to AIDS gave similar results, showing a decline in median age at HIV infection from 34 and 33 years for both the faster and slower progression-rate distributions, respectively, in 1982 to 1984, to 24 and 26 years, respectively, in 1987 to 1989, and to 27 and 28 years, respectively, in 1990 to 1994. Analyses which assumed half the age-effect also gave similar results.
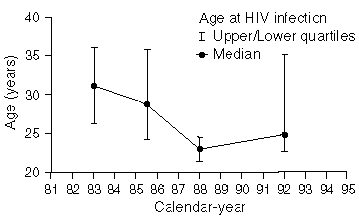
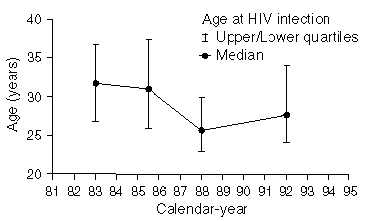
Figure 1: Estimated median age at HIV infection by calendar year (a) faster progression-rate distribution, (b) slower progression-rate ditribution (see text)
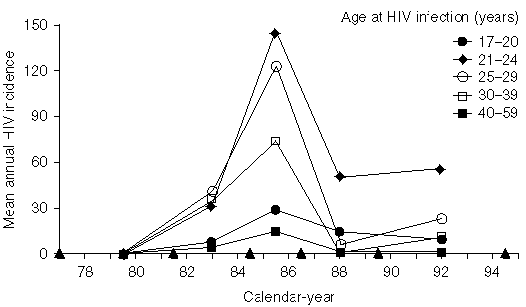
Although the median age at HIV infection has declined during the epidemic, HIV incidence has declined in all age groups from a peak in the mid-1980s (Figures 2a and 2b). However, this decline has been more pronounced in the older age groups; most HIV infections in recent years appear to have been in men under 30 years. HIV incidence was similar in the age groups 21 to 24, 25 to 29 and 30 to 35 years in 1982 to 1984, but by 1990 to 1994 HIV incidence was substantially higher in the 21 to 24 years age group.
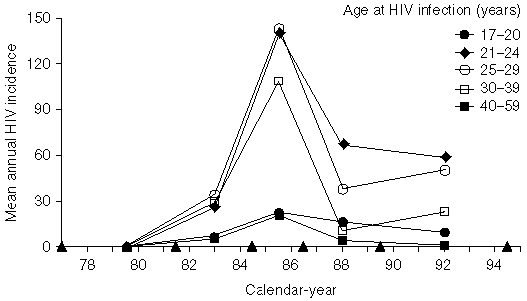
Figure 2: Estimated HIV incidence by age group at HIV infection and by calendar year (a) faster progression-rate distribution, (b) slower progression-rate ditribution (see text)
Sensitivity analyses which assumed a stronger treatment effect (a 50% reduction in the progression rate to AIDS) gave similar results and are not shown.
Discussion The decrease in the estimated median age at HIV infection among homosexually active men, as shown by our age-specific back-projection analysis, has previously been reported using similar methods in the United States,17 and has also been observed in open cohorts of homosexual men attending genitourinary medicine clinics in London between 1988 and 1994.18
Since 1991, another Australian source of information about new HIV infections has been reported cases to the NAR of newly acquired HIV infection. Diagnosed HIV infections are considered to be newly acquired if the person had a negative HIV test within a year of their positive HIV test or if a HIV seroconversion illness was diagnosed. About 200 newly acquired HIV infections are reported each year,4 and the median age of these people has been around 30 to 31 years since 1991 (more than the median age of between 25 and 27 years estimated by the age-specific back-projection analyses in our study). However, HIV incidence since 1991 has been estimated to be around 500 cases per year,3 so only about 40% of these cases are diagnosed each year as newly acquired. It is possible that this 40% is a biased sample of all new HIV infections and, in particular, slightly older than new HIV infections which are not diagnosed as newly acquired.
Back-projection analyses are based on assumptions that are subject to uncertainty, in particular the assumed progression-rate distributions. The available Australian data were part of a large- cohort study of HIV-infected homosexual men,11 and indicate that the overall progression rate in homosexually active men in Australia is broadly consistent with both the faster and slower progression-rate distributions that were assumed in the age-specific back-projections. Other major sources of uncertainty are in the modifying effect of age at HIV infection and the effect of antiretroviral and prophylactic treatments on the progression rate to AIDS. The general trend of decreasing age at HIV infection was, however, a robust feature of sensitivity analyses which investigated these uncertainties, suggesting that this trend is at least qualitatively correct.
Examining the history of the HIV epidemic among homosexually active men in Australia lends further support for a decreasing age at HIV infection. When the HIV epidemic began in Australia around 1980, homosexually active men of all ages were at risk of infection. As the epidemic progressed, new homosexual men were at risk of HIV infection as they became sexually active, generally at a younger age. Thus, the age distribution of homosexually active men at risk of HIV infection (and hence of those already infected) would be expected to have decreased as the epidemic progressed.
The estimates of HIV incidence were standardised for the number of calendar-years and age-years in each time period and age group. This allows direct comparison of HIV incidence if the number of homosexually active men can be assumed to be constant across different age groups over the time period of the epidemic. Based on the 1991 census,19 the resident male population in Australia was fairly uniformly distributed across the age range 15 to 44 years (at about 140 000 men per age-year) but there were fewer men in older age groups. In the age range 17 to 39 years, however, direct comparison of the standardised estimates of HIV incidence appears valid, provided that the proportion of homosexual men is constant over the age range.
One feature of our analyses which requires cautious interpretation is the apparent small increase in HIV infection in some age groups between 1987 to 1989 and 1990 to 1994. As few people infected with HIV in the most recent period would be expected to have progressed to AIDS, these figures are uncertain. The most appropriate interpretation is that the number of new HIV infections has been reasonably stable in all age groups between 1987 and 1994.
In conclusion, age-specific back-projections suggest that the median age at HIV infection among homosexually active men has decreased over the period 1982 to 1994, and that most HIV infections in more recent years have occurred in men aged under 30. These results suggest that education programs aimed at preventing HIV infections in homosexually active men should be targeted towards younger age groups, in particular homosexually active men in their early twenties.
Register to be notified of new articles by email - To Current Issues list - ©MJA1996
Acknowledgements
The National Centre in HIV Epidemiology and Clinical Research is
funded by the Australian National Council on AIDS through the
Commonwealth AIDS Research Grants Committee. The authors thank the
National HIV Surveillance Committee and the doctors who reported
AIDS cases under national surveillance procedures.
References
- National Working Group on HIV Projections. Estimates and
projections of the HIV epidemic in Australia, 1981-1994. Internal
technical report 1. Sydney: National Centre in HIV Epidemiology and
Clinical Research, April 1992.
-
Valuing the past . . . investing in the future. Evaluation of the
National HIV/AIDS Strategy 1993-94 to 1995-96. Canberra:
Commonwealth Department of Human Services and Health, 1995.
-
National Centre in HIV Epidemiology and Clinical Research.
Estimates and projections of the HIV epidemic in Australia,
1981-1997. In: Technical appendix no. 1: An epidemiological
assessment of the HIV epidemic in Australia. Evaluation of the
National HIV/AIDS Strategy 1993-94 to 1995-96. Canberra:
Commonwealth Department of Human Services and Health, 1996.
-
National Centre in HIV Epidemiology and Clinical Research.
Australian HIV Surveillance Report, Vol. 12, No. 1. Sydney: National
Centre in HIV Epidemiology and Clinical Research, 1996.
-
Brookmeyer R, Gail MH. A method for obtaining short-term
projections and lower bounds on the size of the AIDS epidemic. J Am
Stat Soc 1988; 3: 301-308.
-
Taylor JM. Models for the HIV infections and AIDS epidemic in the
United States. Stat Med 1989; 8: 45-58.
-
Becker NG, Watson LF, Carlin JB. A method of non-parametric
back-projection and its application to AIDS data. Stat Med
1991; 10: 1527-1542.
-
Rosenberg PS. Backcalculation models of age-specific HIV
incidence rates. Stat Med 1994; 13: 1975-1990.
-
Brookmeyer R, Liao J. The analysis of delays in disease reporting:
methods and results for the acquired immunodeficiency syndrome.
Am J Epidemiol 1990; 132: 355-365.
-
Rosenberg PS, Goedert JJ, Biggar RJ, for the multicenter
Hemophilia Cohort Study and the International Registry of
Seroconverters. Effect of age-at-seroconversion on the natural
AIDS incubation distribution. AIDS 1994; 8: 803-810.
-
Biggar RJ and the International Registry of Seroconverters. AIDS
incubation in 1891 HIV seroconverters from different exposure
groups. AIDS 1990; 4: 1059-1066.
-
Selik RM, Buelher JW, Karon JM, et al. Impact of the 1987 revision of
the case definition of Acquired Immune Deficiency Syndrome in the
United States. J AIDS 1990; 3: 73-82.
-
Kaldor JM, French MAK. When do patients present with HIV
infection? Med J Aust 1993; 158: 37-38.
-
Volberding PA, Lagakos SW, Koch MA, et al. Zidovudine in
asymptomatic human immunodeficiency virus infection: A controlled
trial in persons with fewer than 500 CD4-positive cells per cubic
millimeter. N Engl J Med 1990; 322: 941-949.
-
Cooper DA, Gatell JM, Kroon S, et al. Zidovudine in persons with
asymptomatic HIV infection and CD4+ cell counts greater than 400 per
cubic millimeter. N Engl J Med 1993; 329: 297-303.
-
Concorde Coordinating Commitee. Concorde: MRC/ANRS randomised
double-blind controlled trial of immediate and deferred zidovudine
in symptom-free HIV infection. Lancet 1994; 343: 871-881.
-
Rosenberg PS, Biggar RJ, Goedert JJ. Declining age at HIV
infection in the United States [letter]. N Engl J Med 1994;
330: 789-790.
-
Miller E, Waight PA, Tedder RS, et al. Incidence of HIV infection in
homosexual men in London, 1988-94. BMJ 1995; 311: 545.
-
Australian Bureau of Statistics. Australia in profile.
Canberra: ABS, 1993. (Catalogue No. 2821.0.)
(Received 13 Nov 1995, accepted 2 April 1996)
Authors' details
National Centre in HIV Epidemiology and Clinical Research, The University of New South Wales, Sydney, NSW.Matthew G Law, MSc, Statistician. Ann McDonald, MPH, Senior Research Assistant. John M Kaldor, PhD, Professor of Epidemiology.
National Cancer Institute, Rockville, USA.
Philip S Rosenberg, PhD, Biostatistician.
No reprints will be available. Correspondence: Mr M G Law, National Centre in HIV Epidemiology and Clinical Research, The University of New South Wales, 376 Victoria Street, NSW 2010.
E-mail: mlaw@nchecr.unsw.edu.au
Readers may print a single copy for personal use. No further
reproduction or distribution of the articles
should proceed without the permission of the publisher. For
permission, contact the
Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au>".
<URL: http://www.mja.com.au/>
© 1996 Medical Journal of Australia.
Received 25 May 2026, accepted 25 May 2026
- Matthew G Law
- Philip S Rosenberg
- Ann McDonald
- John M Kaldor