TO THE EDITOR: Multisystem inflammatory syndrome in children (MIS‐C) or adults (MIS‐A) is a rare but severe systemic inflammatory syndrome,1 with an epidemiological peak occurring 4–6 weeks after severe acute respiratory syndrome coronavirus‐2 (SARS‐CoV‐2) outbreaks.2 Also known as paediatric inflammatory multisystem syndrome temporally associated with SARS‐CoV‐2, MIS‐C is the subject of active surveillance across paediatric centres.3 The peak age for the syndrome is 9 years,1 although cases have been reported in adults.4 We report, to our knowledge, the first Australian case of MIS‐A, diagnosed 2 months into the SARS‐CoV‐2 Delta outbreak in New South Wales, with 60 075 coronavirus disease 2019 (COVID‐19) notifications in the period 29 June to 4 October 2021.5
A 42‐year‐old woman presented with 7 days of subjective fevers, myalgia, light‐headedness, abdominal pain, nausea, palpitations and non‐pleuritic chest pain. Presentation occurred 27 days after acute COVID‐19 pneumonitis, confirmed by polymerase chain reaction and serology testing. The acute illness was mild, requiring neither oxygen nor hospitalisation, and the patient recovered fully 72 hours before onset of this new symptom complex. She was unimmunised against SARS‐CoV‐2.
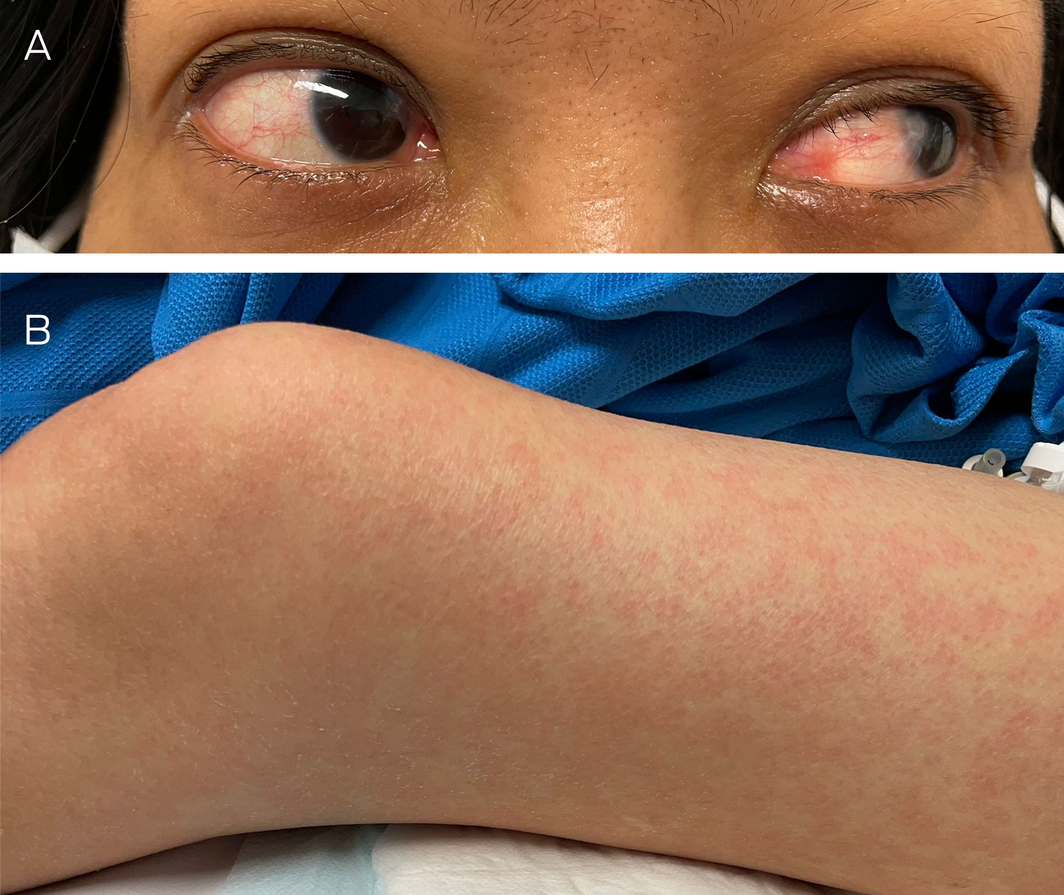
The patient was febrile (38.2°C), with tachycardia (114 beats per minute) and hypotension (79/56 mmHg) but no respiratory distress. She had bilateral conjunctival injection, a widespread blanching macular rash (Box), and oedema of the hands bilaterally. There was no lymphadenopathy or oral mucosal change.
Investigations revealed significant inflammation, with a raised C‐reactive protein level (119 mg/L; reference interval [RI], ≤ 4 mg/L), lymphopenia (0.5 × 109/L; RI, 1.0–4.0 × 109/L), thrombocytopenia (74 × 109/L; RI, 150‐400 × 109/L), neutrophilia (12.2 × 109/L; RI, 2.0–8.0 × 109/L), deranged liver function tests (alanine transaminase, 160 U/L; RI, 10–35 U/L), and hypoalbuminemia (20 g/L; RI, 35–50 g/L). Her D‐dimer level was raised (2.34 mg/L; RI, < 0.5 mg/L), as was her brain natriuretic peptide level (1660 ng/L; RI, ≤ 125 ng/L); troponin and creatine kinase levels were normal. Blood and urine cultures were negative, and anti‐streptolysin O and anti‐DNase B titres were not raised. No echocardiographic evidence of myocarditis was seen, and there was no coronary artery dilatation.
The patient responded to two doses of intravenous immunoglobulin (2 g/kg each) following 48 hours of inotropic support (metaraminol infusion then low dose noradrenaline). Aspirin (3 mg/kg daily) was administered, as well as intravenous antibiotics for 72 hours while cultures were pending.
MIS‐A was diagnosed on the basis of current case definitions,6,7 although the patient also fulfilled criteria for probable toxic shock syndrome, as described in other case series.8
Adults and adolescents with MIS‐A typically present with multisystem involvement, often incorporating myocarditis, shock and gastrointestinal features,4,9 whereas younger children present more commonly with a Kawasaki disease‐like illness.9 Given the absence of specific diagnostic markers, the overlapping phenotype with toxic shock syndrome and the poor sensitivity of cultures and serological markers for these alternative diagnoses, such differentials must be carefully considered in the early phase of illness.
Nonetheless, clinicians should be aware of MIS‐C or MIS‐A in patients presenting with shock, mucocutaneous changes and/or gastrointestinal symptoms, even without preceding symptomatic SARS‐CoV‐2 infection. Prompt treatment with intravenous immunoglobulin and/or steroids is essential to minimise long term morbidity from coronary artery dilatation.1 Although rare, further cases of MIS‐C and MIS‐A are anticipated following increasing COVID‐19 case notifications in NSW and Victoria.
This letter was published as a peer‐reviewed Accepted Article (prior to structural editing and typesetting) on 14 October 2021.
- 1. Whittaker E, Bamford A, Kenny J, et al. Clinical characteristics of 58 children with a pediatric inflammatory multisystem syndrome temporally associated with SARS‐CoV‐2. JAMA 2020; 324: 259–269.
- 2. Toubiana J, Poirault C, Corsia A, et al. Kawasaki‐like multisystem inflammatory syndrome in children during the COVID‐19 pandemic in Paris, France: prospective observational study. BMJ 2020; 369: m2094.
- 3. Paediatric Active Enhanced Disease Surveillance. COVID‐19, Kawasaki Disease (KD) and PIMS‐TS in children; 15 May 2020. https://www.paeds.org.au/covid‐19‐kawasaki‐disease‐kd‐and‐pims‐ts‐children (viewed Oct 2021).
- 4. Morris SB, Schwartz NG, Patel P, et al. Case series of multisystem inflammatory syndrome in adults associated with SARS‐CoV‐2 infection — United Kingdom and United States, March–August 2020. MMWR Morb Mortal Wkly Rep 2020; 69: 1450–1456.
- 5. New South Wales Government. NSW COVID‐19 cases by age range. https://data.nsw.gov.au/nsw‐covid‐19‐data/cases (viewed Oct 2021).
- 6. Centers for Disease Control and Prevention. Multisystem inflammatory syndrome in adults (MIS‐A) case definition information for healthcare providers. https://www.cdc.gov/mis/mis‐a/hcp.html (viewed Oct 2021).
- 7. Vogel TP, Top KA, Karatzios C, et al. Multisystem inflammatory syndrome in children and adults (MIS‐C/A): case definition and guidelines for data collection, analysis, and presentation of immunization safety data. Vaccine 2021; 39: 3037–3049.
- 8. Singh‐Grewal D, Lucas R, McCarthy K, et al. Update on the COVID‐19‐associated inflammatory syndrome in children and adolescents; paediatric inflammatory multisystem syndrome‐temporally associated with SARS‐CoV‐2. J Paediatr Child Health 2020; 56: 1173–1177.
- 9. Godfred‐Cato S, Bryant B, Leung J, et al. COVID‐19‐associated multisystem inflammatory syndrome in children — United States, March–July 2020. MMWR Morb Mortal Wkly Rep 2020; 69: 1074–1080.





We thank Philip Britton, Archana Koirala and Nicholas Wood for helpful discussions regarding this case.
No relevant disclosures.