Older people often live with several chronic conditions1 and take several medications to control the symptoms and reduce the risk of complications.2 Using several medicines concurrently — polypharmacy — places older people at risk of harm, including from adverse drug reactions,3 and is associated with poor clinical outcomes, including nutritional deficiencies, falls, frailty, impaired cognition, more frequent hospitalisation, and premature mortality.4,5 Reducing polypharmacy is one of the areas highlighted by the World Health Organization in its third global patient safety challenge, which aims to halve the global burden of iatrogenic medication‐related harm.6
Dramatic increases in rates of polypharmacy have been reported overseas,7 but the situation for older Australians is less well documented. The estimated prevalence of polypharmacy in different Australian settings range between 43% and 91%;3,8,9,10 the higher estimates are usually for people with greater needs, such as hospital inpatients and aged care home residents.
The heterogeneity of these estimates is also partially explained by how exposure to medicines is measured and polypharmacy is defined. Medicines exposure has been variously estimated on the basis of dispensing claims, prescribing data, medicine chart review, and self‐report by patients; further, some authors measure pill burden (the number of pharmaceutical preparations taken), others the total number of unique medicinal substances.11 There is no universally accepted definition of polypharmacy; current working definitions include four or more daily medicines (applied by the WHO)6 and five or more concurrent medicines, ten or more medicines (“hyperpolypharmacy”) or 15 or more medicines (“extreme hyperpolypharmacy”), as well as qualitative definitions such as “more medicines than necessary”.12
We estimated the extent of polypharmacy in a nationally representative sample of older Australians (70 years of age and older) on the basis of dispensing claims data for prescribed medicines. We applied several definitions of polypharmacy to determine the extent of polypharmacy among older Australians during the period 2006–2017.
Methods
Setting and data source
In Australia, prescribed medicines included in the Pharmaceutical Benefits Scheme (PBS) are publicly subsidised for Australian citizens and permanent residents. We analysed a 10% random sample of de‐identified dispensing data for PBS‐eligible people. This standard dataset extract, provided by the Australian Department of Human Services for analytic purposes, includes data for all PBS‐listed medicines dispensed in Australia.13 PBS dispensing records in the data extract for people aged 70 years or more from the period 1 January 2006 – 31 December 2017 were included in our analysis.
The PBS subsidises PBS‐listed medicines when their price exceeds a co‐payment threshold. PBS concessional beneficiaries (people with a health care card or receiving government welfare benefits, including low income, old age, sickness, unemployment, single parent, or disability support) pay a lower co‐payment than other PBS‐eligible people (general beneficiaries).13 The prices of many common medicines are below the general co‐payment threshold, but all are above the concessional co‐payment threshold. Since July 2012, all PBS‐listed medicines have been captured in the PBS dataset, regardless of price; prior to July 2012, only medicines above the co‐payment threshold were recorded, and ascertainment of PBS‐subsidised medicines was complete only for concessional beneficiaries. Further, the PBS dataset does not include medicines purchased without a prescription, such as over‐the‐counter and complementary medicines, or medicines dispensed on private prescriptions.
Medicines of interest
We examined medicines according to the Anatomic Therapeutic Chemical (ATC) classification system at the fifth level; that is, by chemical substance, not preparation. We included all dispensed items recorded in the PBS collection except topical and non‐therapeutic agents (such as plasters and creams) and medicines in ATC classification V (Various).14
Measurement of polypharmacy
We estimated continuous polypharmacy by counting the number of unique medicines dispensed during both of two time periods, 1 April – 30 June and 1 October – 31 December, in each calendar year;15 we separately counted each active ingredient in combination preparations. This measure of polypharmacy captures prescription medicines taken on a regular basis. We chose the specified exposure periods to avoid underestimating medicine exposure because people who reach the PBS “safety net” stockpile medicines at the end of the calendar year (once the total amount paid for medicines by an individual or family reaches a threshold level, further medicines can be acquired with reduced or [for concessional beneficiaries] without co‐payments).13 Our primary outcome was the prevalence of continuous polypharmacy of five or more unique medicines; as secondary outcomes, we report continuous polypharmacy of ten or more and 15 or more unique medicines.
Population prevalence of polypharmacy, 2017
We calculated the prevalence of polypharmacy in 2017, both overall and stratified by age and sex, using the mid‐calendar year estimated Australian residential population (Australian Bureau of Statistics16). As the dispensing data were derived from a 10% sample of all PBS beneficiaries (general and concessional), we multiplied counts by 10 to estimate the numbers of people affected by polypharmacy.
Prevalence of polypharmacy among concessional beneficiaries, 2006–2017
We calculated the annual prevalence of polypharmacy (five or more unique medicines) among PBS concessional beneficiaries for each entire calendar year.
Alternative measures of polypharmacy: cumulative polypharmacy and pill burden
We also estimated polypharmacy according to two alternative measures. We calculated cumulative polypharmacy,15 or the number of unique medicines dispensed during a single time period (1 April – 30 June) in a calendar year. The continuous polypharmacy approach is more conservative than the cumulative polypharmacy method; in addition to regular medicines, cumulative polypharmacy captures short courses of treatment and intermittently dispensed medications, and therefore provides an upper limit estimate of the prevalence of polypharmacy. Second, we calculated polypharmacy according to pill burden, based on the number of unique preparations dispensed; that is, combination therapies were counted as single entities. We included all oral and non‐oral formulations in the pill burden analyses.
Ethics and data access approval
This study was approved by the New South Wales Population and Health Services Research Ethics committee (reference, 2013/11/494). The Department of Human Services External Request Evaluation Committee approved access to PBS data (reference, MI8696).
Results
Population prevalence of continuous polypharmacy, 2017
Extrapolating data from the PBS sample (Supporting Information, table 1) to the Australian population, we estimated that continuous polypharmacy (five or more unique medicines) affected 935 240 older Australians (prevalence, 36.1%) in 2017. Rates of polypharmacy were higher for women than men (36.6% v 35.4%) and were highest among those aged 80–84 years (43.9%) or 85–89 years (46.0%). The prevalence of continuous polypharmacy with 10 or more unique medicines among older Australians was 5.9%, and with 15 or more medicines, 0.7% (Box 1).
Prevalence of continuous polypharmacy among concessional beneficiaries, 2006–2017
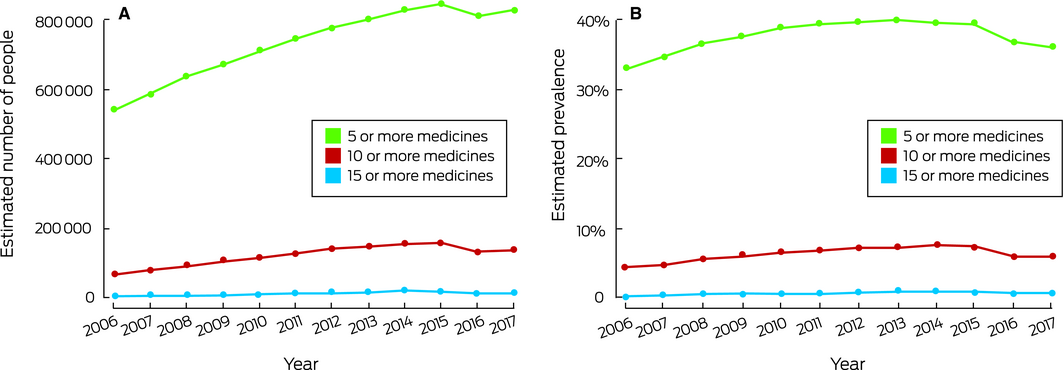
The number of concessional beneficiaries in the PBS sample aged 70 years or more was 163 725 in 2006 and 229 212 in 2017 (Supporting Information, table 2). The estimated number of people affected by polypharmacy with five or more unique medicines increased from 543 950 (prevalence, 33.2%) in 2006 to 829 830 (39.8%) in 2014, then declined to 814 470 (36.8%) in 2016 before rising to 828 950 (36.2%) in 2017; the overall increase in absolute numbers during 2006–2017 was 52% (Box 2). The estimated number of older concessional beneficiaries affected by hyperpolypharmacy increased from 71 550 in 2006 (prevalence, 4.1%) to 139 650 (6.1%) in 2017, an absolute increase of 95%.
Prevalence of cumulative polypharmacy, 2017
The proportion of older Australians (general and concessional beneficiaries) affected by cumulative polypharmacy with five or more unique medicines in 2017 was 52.7% (Supporting Information, table 1), corresponding to an estimated 1 366 590 people; this number is our upper estimate of polypharmacy among older Australians. Among concessional beneficiaries, annual estimates of the prevalence of cumulative polypharmacy were consistently higher than for continuous polypharmacy, but the changes over time were similar (Supporting Information, table 2 and figure 1.
Prevalence of polypharmacy according to pill burden
In 2017, 28.5% of older people regularly took five or more medical preparations concurrently, corresponding to an estimated 738 900 people. The estimated prevalence of polypharmacy based on pill burden was generally lower than that based on medicine burden (Supporting Information, table 3), but for PBS concessional beneficiaries aged 70 years or more it also increased during most of the study period (at a slower rate than medicine burden) before dipping in 2016. Estimates of polypharmacy based upon cumulative pill burden were consistently higher than those based upon continuous pill burden (Supporting Information, table 4 and figure 2).
Discussion
On the basis of our analysis of a nationally representative sample of PBS prescribing data, we estimate that about 935 000 Australians aged 70 years or more were using five or more medicines during both of two 3‐month periods of 2017. While the prevalence of polypharmacy grew modestly during 2006–2017 (by 9%), the growth of the population aged 70 years or more meant that the number of people affected by polypharmacy increased by 52%. Medical practitioners are increasingly aware of the high risk of harm for older people associated with polypharmacy, and the need for strategies for consolidating management of patients with chronic diseases and for deprescribing inappropriate medicines is recognised. The decline in polypharmacy at the end of our observation period may reflect a reduction in the total number of PBS‐listed medicines dispensed, but PBS policy changes at this time17 could also explain the apparent reduction in PBS‐relevant dispensing; that is, people may have continued to use medicines after they were no longer subsidised by the PBS.
Large increases in the prevalence of polypharmacy have been reported overseas: for example, from 24% in 1992 to 39% in 2012 among people over 65 years of age in the United States18 and from 11.4% in 1995 to 22.1% in 2010 in people over 70 in the United Kingdom.7 We did not find such a large increase during 2006–2017, but the prevalence of polypharmacy in comparable years was much higher in Australia than in the US or UK, despite our conservative measure of continuous polypharmacy. The reasons for these differences are unclear, but our findings suggest that levels of medicine use in Australia are not only relatively high, but have been for some time.
Earlier estimates of polypharmacy in community settings in Australia were similar to ours, ranging between 36% and 43%.10,19 Conversely, our estimates were lower than Australian estimates for older people in hospitals (75%),9 oncology outpatients (57%),3 and residents of aged care facilities (91%),8,20 probably because people receiving care have medication needs greater than those of the general population. Medicine use by older people receiving community care services in Australia has doubled over the past 20 years.21 This rapid increase may reflect the changing population of people who use these services as eligibility criteria for both community care services and residential aged care are modified.
Unlike other studies, we examined the prevalence of polypharmacy according to pill burden as well as the number of unique medicines. The increase in polypharmacy based on unique medicines over the past decade was more marked than for the estimate based on pill burden. The increased availability of combination products has probably contributed both to using more medicines and to lowering the pill burden. We recommend that future studies specify and distinguish between medicines use and pill burden, particularly as the difference between estimates of polypharmacy based on the two measures appears to be increasing.
Polypharmacy (both its prevalence and absolute numbers) steadily increased among older people in Australia from 2006 until 2015, then declined from 2016. An analysis of Medicare statistics22 indicates that this change in PBS dispensing involved all PBS‐listed medicines (data not shown), and it is likely that changes in PBS policies17 influenced dispensing rather than changed actual medicine use. For example, popular low cost medicines (eg, paracetamol, aspirin, iron, folic acid) were delisted by the PBS,23 and a new policy allowed pharmacists to opt to discount PBS co‐payments by $1 at their own expense. An expanded “early supply rule” was introduced so that medicines dispensed within a specified interval would not count towards the safety net threshold or be eligible for the $1 discount.24 The combination of these policy changes may have resulted in less dispensing throughout the year and fewer patients reaching the PBS safety net threshold.
Strengths and limitations
The strength of our study is that it was based on a nationally representative sample of PBS prescribing data for older Australians. It is the first to investigate patterns of polypharmacy across all older Australians rather than in specific subgroups. Analysing dispensing databases is an indirect, validated method for estimating medicines use.25
The data included in this study included only PBS‐subsidised medicines and excluded medicines not requiring prescriptions, complementary and alternative medicines, and medicines dispensed on private or non‐subsidised prescriptions. The continuous polypharmacy method may not capture medicines that were commenced or stopped between the two observation periods. Some regular medicines may not have been included in the continuous polypharmacy analysis, including infrequently dispensed medicines such as l‐thyroxine, iron infusions, some anti‐resorptive therapies, and vitamin B12 injections. These exclusions mean that our estimates of polypharmacy will be conservative. But by reporting several polypharmacy measures, we have provided a benchmark for future research, applying two different methods to derive comparable estimates of the prevalence of polypharmacy (continuous and cumulative) that provide realistic upper and lower estimates of medicine use and pill burden.
We analysed a large dispensing dataset, but did not have data on patient‐specific health parameters, including comorbid conditions and functional status. It was therefore not possible to assess whether individual medicine regimens were therapeutically appropriate. Similarly, we cannot ascertain whether changes in the prevalence of polypharmacy reflect improved treatment of comorbid conditions and reduced under‐prescribing of indicated therapies.
Conclusion
The prevalence of polypharmacy among older Australians is relatively high, affecting almost one million people in 2017. We found that the proportion of older PBS concessionary beneficiaries affected has increased since 2006 by 9%, and the absolute number of people by 52%, despite a small reduction since 2014. Polypharmacy can be appropriate, but this needs to be balanced against the risk that it may contribute to adverse health outcomes in older people. Translational research into strategies for reducing medicine use and complexity that target both health professionals and the public is needed. These strategies need to be effective and sustainable, and should include multidisciplinary approaches and system‐level interventions.26
Box 1 – Population prevalence of continuous polypharmacy in Australia and numbers of people affected among people aged 70 years or more, 2017
|
|
Estimated residential population16 |
Estimated number of people (prevalence) |
|||||||||||||
|
5 or more medicines |
10 or more medicines |
15 or more medicines |
|||||||||||||
|
|
|||||||||||||||
|
All people (70 years or more) |
2 593 514 |
935 240 |
153 040 |
17 220 |
|||||||||||
|
Age group |
|||||||||||||||
|
70–74 years |
958 102 |
269 800 |
38 400 |
4250 |
|||||||||||
|
75–79 years |
677 142 |
250 760 |
39 420 |
4660 |
|||||||||||
|
80–84 years |
469 203 |
205 790 |
36 850 |
4380 |
|||||||||||
|
85–89 years |
307 736 |
141 640 |
25 610 |
2660 |
|||||||||||
|
90–94 years |
144 551 |
55 790 |
10 610 |
1120 |
|||||||||||
|
95 years or more |
36 780 |
11 460 |
2150 |
150 |
|||||||||||
|
Sex |
|||||||||||||||
|
Women |
1 407 313 |
515 540 |
85 060 |
9360 |
|||||||||||
|
Men |
1 186 201 |
419 700 |
67 980 |
7860 |
|||||||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
Received 30 January 2019, accepted 6 May 2019
- Amy T Page1,2,3
- Michael O Falster4
- Melisa Litchfield4
- Sallie‐Anne Pearson4,5
- Christopher Etherton‐Beer6,7
- 1 Alfred Health, Melbourne, VIC
- 2 Centre for Medicine Use and Safety, Monash University, Melbourne, VIC
- 3 Centre for Optimisation of Medicines, University of Western Australia, Perth, WA
- 4 Centre for Big Data Research in Health, UNSW Australia, Sydney, NSW
- 5 Menzies Centre for Health Policy, University of Sydney, Sydney, NSW
- 6 WA Centre for Health and Ageing, University of Western Australia, Perth, WA
- 7 Royal Perth Hospital, Perth, WA
This investigation was supported by the National Health and Medical Research Council (NHMRC) Centre for Research Excellence in Medicines and Ageing (CREMA; 1060407). Michael Falster and Amy Page are supported by NHMRC Early Career Fellowships (1139133, 1156892). We thank the Department of Human Services for providing the data for our analysis.
Sallie Pearson and Christopher Etherton‐Beer are members of the Drug Utilisation Sub‐Committee of the Pharmaceutical Benefits Advisory Committee. The views expressed in this article do not represent those of the Committee.
- 1. Formiga F, Fort I, Robles MJ, et al. Comorbidity and clinical features in elderly patients with dementia: differences according to dementia severity. J Nutr Health Aging 2009; 13: 423–427.
- 2. Williams A, Manias E, Walker R. Interventions to improve medication adherence in people with multiple chronic conditions: a systematic review. J Adv Nurs 2008; 63: 132–143.
- 3. Turner JP, Shakib S, Singhal N, et al. Prevalence and factors associated with polypharmacy in older people with cancer. Support Care Cancer 2014; 22: 1727–1734.
- 4. Turner JP, Jamsen KM, Shakib S, et al. Polypharmacy cut‐points in older people with cancer: how many medications are too many? Support Care Cancer 2016; 24: 1831–1840.
- 5. Gnjidic D, Hilmer SN, Blyth FM, et al. Polypharmacy cutoff and outcomes: five or more medicines were used to identify community‐dwelling older men at risk of different adverse outcomes. J Clin Epidemiol 2012; 65: 989–995.
- 6. Sheikh A, Dhingra‐Kumar N, Kelley E, et al. The third global patient safety challenge: tackling medication‐related harm. Bull World Health Organ 2017; 95: 546–546A.
- 7. Guthrie B, Makubate B, Hernandez‐Santiago V, Dreischulte T. The rising tide of polypharmacy and drug‐drug interactions: population database analysis 1995–2010. BMC Med 2015; 13: 74.
- 8. Somers M, Rose E, Simmonds D, et al. Quality use of medicines in residential aged care. Aust Fam Physician 2010; 39: 413–416.
- 9. Hubbard RE, Peel NM, Scott IA, et al. Polypharmacy among inpatients aged 70 years or older in Australia. Med J Aust 2015; 202: 373–377. https://www.mja.com.au/journal/2015/202/7/polypharmacy-among-inpatients-aged-70-years-or-older-australia.
- 10. Morgan TK, Williamson M, Pirotta M, et al. A national census of medicines use: a 24‐hour snapshot of Australians aged 50 years and older. Med J Aust 2012; 196: 50–53. https://www.mja.com.au/journal/2012/196/1/national-census-medicines-use-24-hour-snapshot-australians-aged-50-years-and.
- 11. Balu S, Simko RJ, Quimbo RM, Cziraky MJ. Impact of fixed‐dose and multi‐pill combination dyslipidemia therapies on medication adherence and the economic burden of sub‐optimal adherence. Curr Med Res Opin 2009; 25: 2765–2775.
- 12. Masnoon N, Shakib S, Kalisch‐Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatr 2017; 17: 230.
- 13. Paige E, Kemp‐Casey A, Korda R, Banks E. Using Australian Pharmaceutical Benefits Scheme data for pharmacoepidemiological research: challenges and approaches. Public Health Res Pract 2015; 25: e2541546.
- 14. World Health Organization. ATC/DDD Index 2018. https://www.whocc.no/atc_ddd_index (viewed June 2018).
- 15. Fincke BG, Snyder K, Cantillon C, et al. Three complementary definitions of polypharmacy: methods, application and comparison of findings in a large prescription database. Pharmacoepidemiol Drug Saf 2005; 14: 121–128.
- 16. Australian Bureau of Statistics. Quarterly population estimates (ERP), by state/territory, sex and age. http://stat.data.abs.gov.au/Index.aspx?DataSetCode=ERP_QUARTERLY (viewed June 2018).
- 17. Australian Department of Health. PBS Access and Sustainability Package including the Sixth Community Pharmacy Agreement. Pharmaceutical Benefits Scheme; updated 13 July 2017. http://www.pbs.gov.au/info/general/pbs-access-sustainability-package (viewed May 2019).
- 18. Kantor ED, Rehm CD, Haas JS, et al. Trends in prescription drug use among adults in the United States from 1999–2012. JAMA 2015; 314: 1818–1830.
- 19. Beer C, Hyde Z, Almeida OP, et al. Quality use of medicines and health outcomes among a cohort of community dwelling older men: an observational study. Br J Clin Pharmacol 2011; 71: 592–599.
- 20. Poudel A, Peel NM, Mitchell CA, et al. Geriatrician interventions on medication prescribing for frail older people in residential aged care facilities. Clin Interv Aging 2015; 10: 1043–1051.
- 21. Elliott RA, Lee CY, Beanland C, et al. Medicines management, medication errors and adverse medication events in older people referred to a community nursing service: a retrospective observational study. Drugs Real World Outcomes 2016; 3: 13–24.
- 22. Australian Department of Human Services. Pharmaceutical Benefits schedule group reports. Updated 25 Mar 2019. http://medicarestatistics.humanservices.gov.au/statistics/pbs_group.jsp (viewed May 2019).
- 23. Australian Department of Human Services. Proposed listing changes for OTC items from 1 January 2016. http://www.pbs.gov.au/general/pbs-access-sustainability/otc-recommendations-for-1-january-2016.pdf (viewed May 2019).
- 24. Andrade SE, Kahler KH, Frech F, Chan KA. Methods for evaluation of medication adherence and persistence using automated databases. Pharmacoepidemiol Drug Saf 2006; 15: 565–574.
- 25. Australian Department of Health. Discounting PBS patient co‐payment. Updated 25 June 2015. http://www.pbs.gov.au/general/pbs-access-sustainability/fact-sheet-discounting-pbs-patient-co-payment.pdf (viewed May 2019).
- 26. Page AT, Cross AJ, Elliott RA, et al. Integrate health care to provide multidisciplinary consumer‐centred medication management: report from a working group formed from the National Stakeholders’ Meeting for the Quality Use of Medicines to Optimise Ageing in Older Australians. J Pharm Pract Res 2018; 48: 459–466.





Abstract
Objective: To estimate the prevalence of polypharmacy among Australians aged 70 years or more, 2006–2017.
Design, setting and participants: Analysis of a random 10% sample of Pharmaceutical Benefits Scheme (PBS) data for people aged 70 or more who were dispensed PBS‐listed medicines between 1 January 2006 and 31 December 2017.
Main outcome measures: Prevalence of continuous polypharmacy (five or more unique medicines dispensed during both 1 April – 30 June and 1 October – 31 December in a calendar year) among older Australians, and the estimated number of people affected in 2017; changes in prevalence of continuous polypharmacy among older concessional beneficiaries, 2006–2017.
Results: In 2017, 36.1% of older Australians were affected by continuous polypharmacy, or an estimated 935 240 people. Rates of polypharmacy were higher among women than men (36.6% v 35.4%) and were highest among those aged 80–84 years (43.9%) or 85–89 years (46.0%). The prevalence of polypharmacy among PBS concessional beneficiaries aged 70 or more increased by 9% during 2006–2017 (from 33.2% to 36.2%), but the number of people affected increased by 52% (from 543 950 to 828 950).
Conclusions: The prevalence of polypharmacy among older Australians is relatively high, affecting almost one million older people, and the number is increasing as the population ages. Our estimates are probably low, as we could not take over‐the‐counter or complementary medicines or private prescriptions into account. Polypharmacy can be appropriate, but there is substantial evidence for its potential harm and the importance of rationalising unnecessary medicines, particularly in older people.