Four international studies have found that the youngest children in a school class are more likely than their classmates to receive pharmacological treatment for attention deficit/hyperactivity disorder (ADHD).1-4 We investigated whether this late birth date effect applies to children in Western Australia. We compared the proportions of WA children born in the early and late months of a recommended school-year intake who received at least one Pharmaceutical Benefits Scheme prescription for an ADHD medication in 2013 (Box).
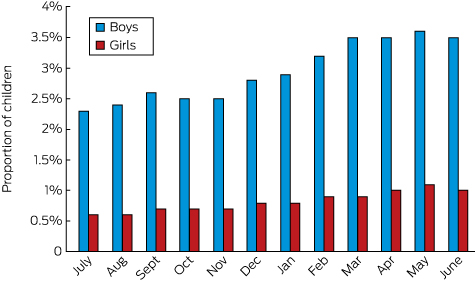
An estimated population of 311 384 children was included in our study, analysed by year and month of birth, sex, and in two 5-year bands: children aged 6–10 years (born July 2003 – June 2008) and children aged 11–15 years (born July 1998 – June 2003). A total of 5937 children (1.9%) received medication for ADHD; the proportion of boys receiving medication (2.9%) was higher than that of girls (0.8%).
Among children aged 6–10 years, those born in June (the last month of the recommended school-year intake) were about twice as likely to have received ADHD medication than those born in the first intake month (the previous July); the relative risks (RRs) were 1.93 for boys (95% confidence interval [CI], 1.53–2.38) and 2.11 for girls (95% CI, 1.57–2.53). For children aged 11–15 years, the effect was less marked, but still significant (RR: boys, 1.26; 95% CI, 1.03–1.52; girls, 1.43; 95% CI, 1.15–1.76). The RRs for the combined group (aged 6–15 years) were 1.52 (95% CI, 1.30–1.73) for boys and 1.73 (95% CI, 1.42–1.94) for girls. Similar differences were found when comparing children born in the first 3 (or 6) months and the last 3 (or 6) months of the school-year intake. These results are consistent with those of previous international studies.
As the data were de-identified, it was impossible to identify which students had commenced school outside their recommended starting year. However, in contrast to other mainland Australian states, fewer than 2% of children in WA start school outside the recommended school-year intake. Delayed entry is most common for children born in June; our study is therefore likely to underestimate the effect of birth date. Further research in states with greater flexibility for parents in deciding their child’s school starting age would help determine whether a broader age spread in school classes is associated with a reduction or increase in any late birthday effect on ADHD medication status.
Frances, who led the DSM-IV development taskforce of the American Psychiatric Association, argued that similar findings in North America indicated that developmental immaturity is mislabelled as a mental disorder and unnecessarily treated with stimulant medication. While he considers ADHD a legitimate diagnosis, he asserted that it is overdiagnosed and overmedicated, estimating that a “diagnostic rate of around 2% … would best balance harms and benefits”.5
The prescribing rate for children in our study was 1.9%, comparable with that reported by a Taiwanese study (1.6%).4 The late birth date effects identified in WA and Taiwan were of similar strength to those in the three North American studies, where the reported ADHD medication prescribing rates for the periods analysed were at least twice as high (4.5%,1 5.8%,2 3.6%3). This indicates that even at relatively low rates of prescribing there are significant concerns about the validity of ADHD as a diagnosis.
Received 6 April 2016, accepted 4 August 2016
- Martin Whitely1,2
- Leanne Lester3
- John Phillimore1
- Suzanne Robinson4
- 1 John Curtin Institute of Public Policy, Curtin University, Perth, WA
- 2 Sir Walter Murdoch School of Public Policy and International Affairs, Murdoch University, Perth, WA
- 3 University of Western Australia, Perth, WA
- 4 Curtin University, Perth, WA
No relevant disclosures.
- 1. Elder TE. The importance of relative standards in ADHD diagnoses: evidence based on exact birth dates. J Health Econ 2010; 29: 641-656.
- 2. Evans WN, Morrill MS, Parente ST. Measuring inappropriate medical diagnosis and treatment in survey data: the case of ADHD among school-age children. J Health Econ 2010; 29: 657-673.
- 3. Morrow RL, Garland J, Wright JM, et al. Influence of relative age on diagnosis and treatment of attention-deficit/hyperactivity disorder in children. CMAJ 2012; 184: 755-762.
- 4. Chen MH, Lan WH, Bai YM, et al. Influence of relative age on diagnosis and treatment of attention-deficit/hyperactivity disorder in Taiwanese children. J Pediatr 2016; 172: 162-167.e1.
- 5. Frances A. Don’t throw out the baby out with the bathwater. Aust N Z J Psychiatry 2015; 49: 577.





Saul Geffen
This assertion is not supported by the data. There are several other conclusions that could be drawn from the data, e.g. that younger children are more likely to be anxious and stressed by school and therefore more likely to exhibit ADHD symptoms, or that younger children are monitored more closely and their symptoms of ADHD are more likely to be identified.
Indeed maybe there is a seasonal effect on developing ADHD like there is for multiple sclerosis.
I note that the authors fail to explicitly state their stand on conventional medical treatment of a serious and well accepted condition such as ADHD.
Competing Interests: No relevant disclosures
Dr Saul Geffen
RACP
Rafael LBravo
This study reaches conclusions similar to those published in MJA and is available in PubMed with abstract in English although the complete original text is in Spanish
Librero J, Izquierdo-María R, García-Gil M, Peiró S. Children's relative age in class and medication for attention-deficit/hyperactivity disorder. A population-based study in a health department in Spain. Med Clin (Barc). 2015 Dec 7;145(11):471-6.
Competing Interests: No relevant disclosures
Dr Rafael LBravo
Centro de Slaud Linneo. SErMAS