A large proportion of accidental paediatric exposures and deliberate self-poisoning incidents involve paracetamol; it is the leading pharmaceutical agent responsible for calls to Poisons Information Centres in Australia and New Zealand. Management of paracetamol poisoning has altered since the previous guidelines were published in 2008, so that they do not reflect current practice by clinical toxicologists. The key changes from the previous guidelines concern the indications for administration of activated charcoal; the management of patients taking large or massive overdoses; modified-release and supratherapeutic ingestions; and paediatric liquid paracetamol ingestion.
Main recommendations
The management of patients with paracetamol overdose is usually straightforward. Acute deliberate self-poisoning, accidental paediatric exposure and inadvertent repeated supratherapeutic ingestions all require specific approaches to risk assessment and management.
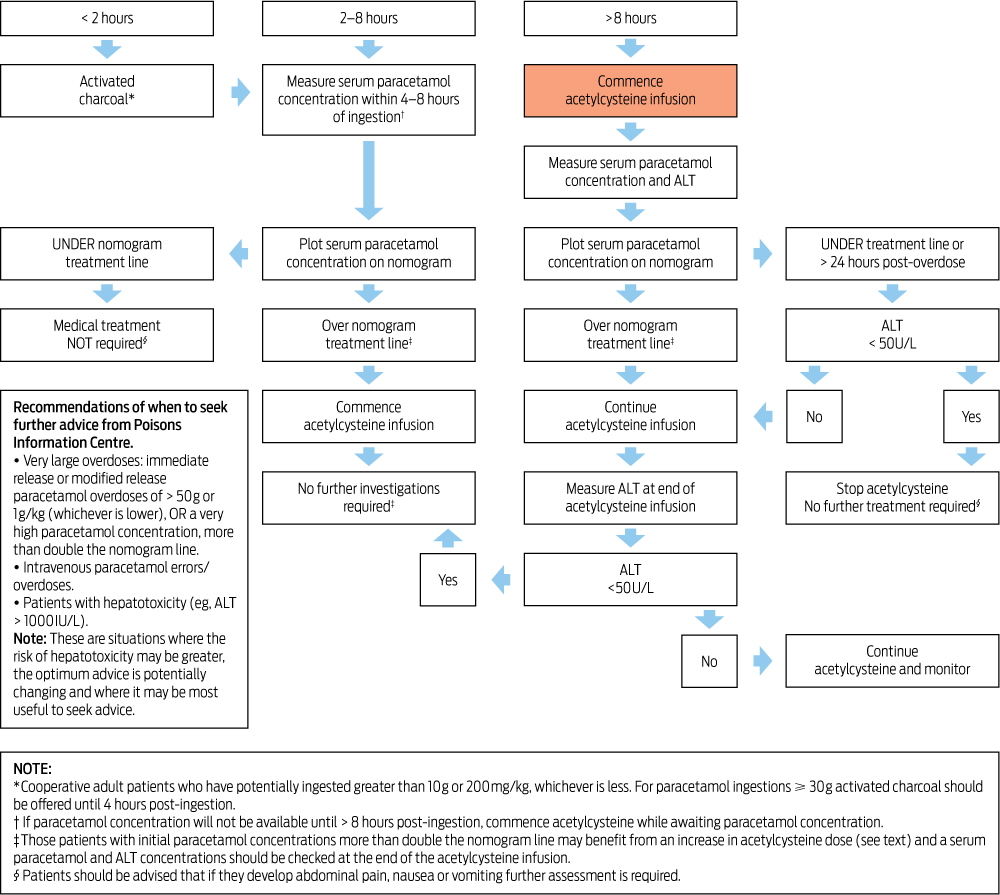
Each initially involves a risk assessment (Box 1). The key factors to consider in paracetamol poisoning are the ingested dose and serum paracetamol concentration (early), or clinical and laboratory features suggesting liver damage (late). Serum paracetamol concentration should be used to assess the need for acetylcysteine administration in all patients presenting with deliberate self-poisoning with paracetamol, regardless of the stated dose. The management of acute paracetamol exposure with known time of ingestion is summarised in a management flow chart (Box 2) and the management of supratherapeutic ingestion is shown in Box 3.
It is important to note that the paracetamol treatment nomogram has not changed, and that the acetylcysteine regimen remains the same as in the previous guidelines.
Changes in management
Gastric decontamination
It was previously recommended that activated charcoal be administered within 1 hour of paracetamol ingestion. The current guideline advises that 50 g activated charcoal should be administered to a cooperative, awake adult within 2 hours of ingestion of a toxic dose of immediate-release paracetamol, and within 4 hours of modified-release paracetamol ingestion (Box 2).
For immediate-release paracetamol overdoses of greater than 30 g, activated charcoal should be administered up to 4 hours after ingestion. For massive modified-release paracetamol overdoses, absorption may continue until 24 hours after ingestion, and patients may still benefit from activated charcoal treatment after more than 4 hours.
Modified-release paracetamol
As per the previous guideline, acetylcysteine treatment should be started immediately if more than 200 mg/kg or 10 g (whichever is lower) has been ingested. Two assessments of serum paracetamol concentration 4 hours apart are required, the first at least 4 hours after ingestion.
The recommendation about when to discontinue acetylcysteine infusion has changed. Serial paracetamol concentrations, measured 4 hours apart, must be below the nomogram line and decreasing. Further, near the completion of acetylcysteine infusion (ie, 2 hours before completion of infusion), serum alanine aminotransferase (ALT) and paracetamol concentrations should be measured. Acetylcysteine infusion should be continued if the ALT level is increasing (greater than 50 U/L) or the paracetamol concentration is greater than 10 mg/L (66 μmol/L).
Large or massive paracetamol overdoses
Patients who ingest large or massive doses of paracetamol were not discussed in previous versions of the guidelines. Most patients ingest less than 30 g of paracetamol, with only a small percentage of overdoses having a paracetamol concentration greater than double the nomogram line. Those who ingest greater doses may have decreased paracetamol clearance and increased risk of hepatotoxicity despite treatment, and may benefit from modifying the standard paracetamol management. Patients considered at high risk of hepatotoxicity are those with high initial paracetamol concentrations.
Although no randomised control trials have investigated optimum acetylcysteine dosage in these patients, it is the practice of many clinical toxicologists to adjust the dose in large paracetamol overdoses. Who might benefit from an increase in acetylcysteine dose and the optimum dose have not yet been determined. One approach, in patients with a paracetamol concentration more than double the nomogram line, is to double the concentration of the 16-hour infusion of acetylcysteine from 100 mg/kg (current standard acetylcysteine third-bag infusion) to 200 mg/kg intravenous acetylcysteine. Serum ALT and paracetamol levels should be checked near the completion of acetylcysteine infusion. Acetylcysteine should be continued if the ALT level is increasing (greater than50 U/L) or the paracetamol concentration is greater than 10 mg/L (66 μmol/L). The Poisons Information Centre or a clinical toxicologist may be consulted for the most current advice on managing these patients, including the optimal acetylcysteine regimen.
Liquid paracetamol ingestion by children under 6 years of age
No recommendations were made in the previous guideline. When ingestion of more than 200 mg/kg of liquid paracetamol by a child under 6 years of age is suspected (in obese children, this should be based on an ideal body weight), serum paracetamol concentration should be measured at least 2 hours after ingestion. If the concentration 2 to 4 hours after ingestion is less than 150 mg/L (1000 μmol/L), acetylcysteine is not required. If the 2-hour paracetamol concentration is greater than 150 mg/L (1000 μmol/L), it should be measured again 4 hours after ingestion, and acetylcysteine infusion commenced if the value is still greater than 150 mg/L (1000 μmol/L), as per the paracetamol nomogram.
The 2-hour paracetamol concentration should only be used to guide management in a healthy child less than 6 years of age, after an isolated liquid paracetamol ingestion. In all other cases, such as children who present later than 4 hours after ingestion, and children who are older than 6 years of age, treatment is the same as that for acute paracetamol exposure in adults.
Repeated supratherapeutic ingestion
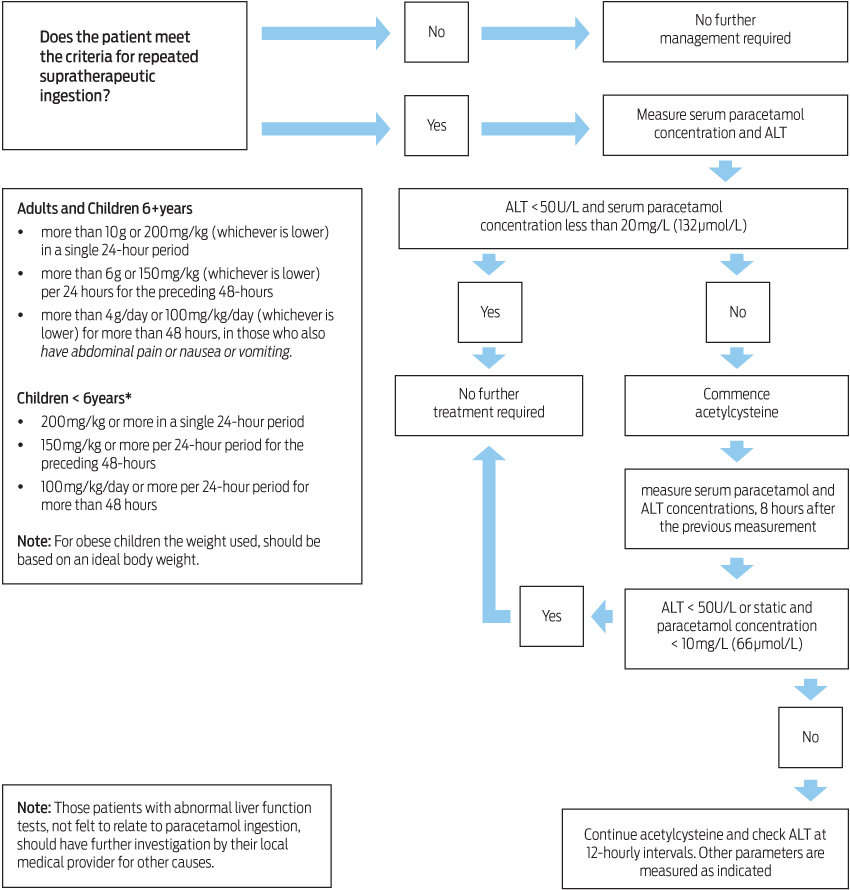
Patients should have serum paracetamol and ALT concentrations measured if they meet the criteria for supratherapeutic ingestion (Box 1). The main changes in the guidelines concern the criteria for assessment in those who have ingested more than 100 mg/kg/day or 4 g/day (whichever is lower) per 24-hour period for longer than 48 hours. Patients only require assessment if they have symptoms such as abdominal pain or nausea or vomiting. Management is outlined in Box 3.
Acetylcysteine dosing recommendation
The guideline essentially remains unchanged, except that dosing should be based on actual body weight rounded up to the nearest 10 kg, with a ceiling weight of 110 kg.
Hepatotoxicity
This was not discussed in detail in the previous guidelines. Acetylcysteine should be continued until the patient is clinically improving, ALT levels are decreasing, the international normalised ratio (INR) is improving and less than 2, and the paracetamol concentration is less than 10 mg/L (66 μmol/L). Regular clinical review and 12-hourly (or more frequent) blood tests are recommended if there is clinical deterioration.
A liver transplant unit should be consulted if any of the following criteria are met:
-
INR >3.0 at 48 hours or >4.5 at any time;
-
oliguria or creatinine >200 μmol/L;
-
persistent acidosis (pH < 7.3) or arterial lactate >3 mmol/L;
-
systolic hypotension with blood pressure less than 80 mmHg, despite resuscitation;
-
hypoglycaemia;
-
severe thrombocytopenia;
-
encephalopathy of any degree, or any alteration of consciousness (Glasgow coma scale <15) not associated with co-ingestion of sedatives.
Conclusions
This is a summary of the updated guidelines for the management of paracetamol poisoning in Australia and New Zealand. The full guidelines are available on the website of the Medical Journal of Australia (www.mja.com.au/sites/default/files/issues/203_05/Guidelines_paracetamol_Aus_NZ_2015.pdf).
Where there are any concerns regarding the management of paracetamol ingestion, advice can always be sought from a clinical toxicologist or the Poisons Information Centre (telephone: 13 1126 in Australia, 0800 764 766 [0800 POISON] in New Zealand).
Box 1 Paracetamol dosing that may be associated with hepatic injury
|
|
Adults and children >6 years of age |
Children (aged 0–6 years)∗ |
|||||||||||||
|
|
|||||||||||||||
|
Acute single ingestion |
>200 mg/kg or 10 g (whichever is lower) over a period of <8 hours |
>200 mg/kg over a period of <8 hours |
|||||||||||||
|
Repeated supratherapeutic ingestion |
>200 mg/kg or 10 g (whichever is lower) over a single 24-hour period |
>200 mg/kg over a single 24-hour period |
|||||||||||||
|
|
>150 mg/kg or 6 g (whichever is lower) per 24-hour period for the preceding 48 hours |
>150 mg/kg per 24-hour period for the preceding 48 hours |
|||||||||||||
|
|
>100 mg/kg or 4 g (whichever is lower) per 24-hour period, for more than 48 hours in those who also have symptoms indicating possible liver injury (eg, abdominal pain, nausea or vomiting) |
>100 mg/kg per 24-hour period for more than 48 hours |
|||||||||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
Provenance: Commissioned; not externally peer reviewed.





We thank Clinical Associate Professor Simone Strasser (Royal Prince Alfred Hospital) and transplant hepatologists from around Australia and the Kingboyuan;rsquo;s College, London, for their input regarding patients requiring discussion with a liver transplant unit.
No relevant disclosures.