headspace National Youth Mental Health Foundation is the Australian Government’s major investment in the area of youth mental health.1 The National Survey of Mental Health and Wellbeing (NSMHW) revealed that one in four young people experience a clinically relevant mental health problem within any 12-month period, compared with one in five in the general population.2 Half of a cohort of young people were shown to suffer diagnosable mental ill health at some point during the transition from childhood to adulthood, which reduces fulfilment of their potential and increases likelihood of disability and premature death.3 Australian data are consistent with international trends and the adolescent and early adult years are periods of peak prevalence and incidence for most mental disorders.4,5 Yet, despite having the highest prevalence, young people have the lowest level of professional help-seeking for mental health problems across the lifespan.2
headspace was initiated in 2006 to address the concerning mismatch between level of need and amount of mental health service use among adolescents and young adults.1 The initiative is innovative in targeting the age range from early adolescence through early adulthood, maintaining that the traditional child and adolescent versus adult service divide creates a disjunction at precisely the time when there is greatest need for continuity.6 There are now 55 headspace centres across Australia, scaling up to 100 centres in 2016.
The approach to service delivery has been described elsewhere,1,7 but briefly, headspace centres aim to create highly accessible, youth-friendly, integrated service hubs that provide evidence-based interventions and support to young people aged 12–25 years around their mental health, health and wellbeing needs. Each centre is directed by a lead agency on behalf of a local partnership of organisations responsible for the delivery of services, comprising mental health, alcohol and other drug, primary care, and vocational services. The main aim is to improve outcomes for young people by addressing the major barriers to service use for young people,8,9 and enabling better access to and engagement in early intervention services that provide holistic and integrated care.
Client clinical presentation characteristics were measured through self-reported reason for presentation, as well as by clinician diagnosis according to relevant World Health Organization ICD-10 classifications of mental and behavioural disorders. Level of psychological distress was measured by self-report using the 10-item Kessler Psychological Distress Scale (K10),10 while stage of illness was estimated by clinicians using the categories of no mental disorder, mild to moderate symptoms, subthreshold symptoms not reaching full diagnosis, diagnosed disorder, periods of remission, or serious and ongoing disorder without periods of remission.11 Days out of role were self-reported,12 and overall functioning was assessed by clinicians using the Social and Occupational Functioning Assessment Scale (SOFAS).13
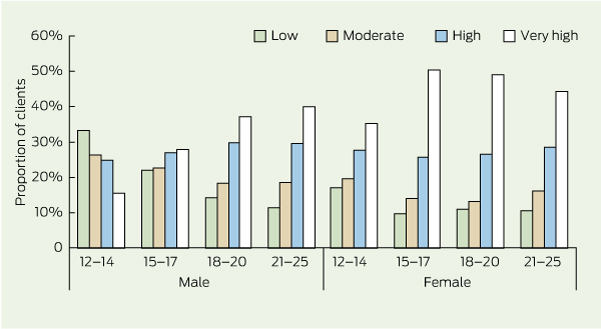
The proportion of male and female clients in each age group is shown in Box 1. The peak age of presentation was 15–17 years, and relatively more males presented in the youngest (12–14 years) and oldest (21–25 years) age groups. Overall, 63.7% of clients were female and 35.6% were male, with only 0.7% reporting that they were intersex, transgender or transsexual. The NSMHW showed that 30% of young women and 23% of young men had experienced mental disorder in the past 12 months.14
There were 7.7% of clients who identified as Aboriginal or Torres Strait Islander, compared with 2011 census data showing that 4.0% of Australians aged 12–25 years identify as Aboriginal or Torres Strait Islander.15
Clients who reported being born outside Australia comprised 7%, compared with 15% of the population aged 10–24 years in 2007–2008.16 Consistent with population trends, the most common places of birth outside Australia for headspace clients were England and New Zealand. Ninety-four per cent reported speaking only English at home, which compares with 80.3% in the general population aged over 5 years.17
Over half the clients (57.1%) lived in major cities, while 31.2% lived in inner regional areas, 9.6% in outer regional, and 2.1% in remote or very remote areas. This compares with 2012 estimates from the Australian Bureau of Statistics that 70% of the youth population lived in major cities, 18% in inner regional areas, 9% in outer regional and 2% in remote or very remote areas.18
Most headspace clients had stable accommodation (86.6%), but there were 10.3% for whom accommodation was an issue, 2.4% who reported that they were at risk of being homeless, and 0.7% who were currently homeless. This compares to 0.7% of the Australian population aged 12–24 years who were estimated as being homeless or in marginal housing in the 2011 census.19 Security of housing decreased markedly with age among headspace clients, from 94.0% of those aged 12–14 years to 81.5% of those aged 21–25 years.
Many clients were currently engaged in education, with 46.7% at school and 21.0% in higher education. Among those aged 18–25 years, 29.0% were not engaged in employment, education or training, which compares with 27.3% in the population.20
Overwhelmingly, the main self-reported reason for young people presenting at headspace centres was having problems with how they felt (71.6%); specifically, almost a quarter first presented feeling sad or depressed (24.9%) and 12.7% were feeling anxious. The next most common reason was having relationship problems (11.4%), followed by physical health issues (6.6%), school/work problems (6.0%), alcohol or other drug problems (1.7%), sexual health issues (1.6%) and vocational concerns (1.0%). Reasons for presenting varied by age and sex (Box 1). Relationship and school issues decreased with age, while problems with feelings increased, especially for males. For females, health and sexual health reasons for presentation increased with age, while alcohol and other drug and vocational issues become more pressing for males.
Over half (69.3%) of the young people attending headspace did so with high or very high levels of psychological distress (Box 2). This compares with only 9% in the general community aged 16–24 years, and 21% of young people diagnosed with mental disorder in the NSMHW.14 Males aged 12–14 years were most likely to present with the lowest levels of psychological distress, while females aged 15–20 years were most likely to present at the highest level of distress. By early adulthood, the distress levels of males and females converged. These patterns were reflected in the mean K10 scores. For males, these increased from 20.7 (standard deviation [SD], 8.2) for those aged 12–14 years to 26.9 (SD, 9.0) for those aged 21–25 years. The increase for females was less pronounced, from 25.7 (SD, 9.4) to 27.7 (SD, 9.1) for those aged 12–14 years and 21–25 years, respectively. Only the younger boys had a mean in the moderate range for the K10; means for all other age groups were in the high-distress range.
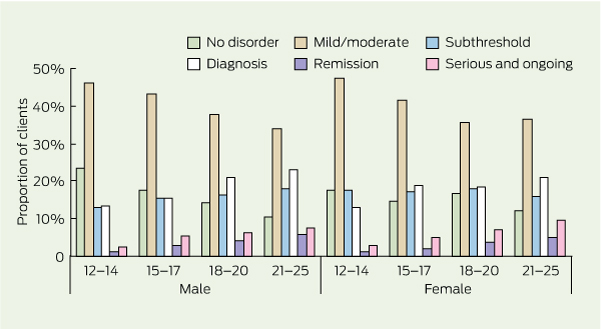
Stage of illness development reflected the expected age-related trajectory using a population health approach based on the spectrum of mental health interventions21 (Box 3). Overall, there were 14.6% of clients with no mental disorder, 39.6% with mild to moderate symptoms, 16.9% with subthreshold diagnosis, 18.8% with full-threshold diagnosis, 3.5% with periods of remission, and 6.4% with serious and ongoing mental disorder. With increasing age, there were fewer clients in the no mental disorder and mild to moderate groups, relative stability in the subthreshold group, and increased proportions in the full-threshold diagnosis, remission, and serious or ongoing disorder categories.
The results show that almost two-thirds of headspace clients are female, which partly reflects the sex difference in the distribution of mood and anxiety disorders for this age group within the Australian population.14 However, in the future, headspace will need to respond more effectively to mental ill health in young men, which typically manifests through substance misuse and behavioural problems, conditions that can mask underlying emotional disorders. The higher proportion of Aboriginal and Torres Strait Islander clients, compared with their proportional representation in the overall population, indicates the need for mental health support in this population group and that the youth-friendly focus of headspace centres may be attractive to young Aboriginal and Torres Strait Islander people. In contrast, there is a lower proportion of clients born outside Australia compared with their proportional representation in the overall population, which suggests that some of these demographic groups may still experience significant barriers to service use.
That a third of the young adult headspace clients were not engaged in education, employment or training indicates the vulnerability of youth with mental health issues to disengagement from vocational opportunities. This is a situation that must be addressed, particularly during the current period of growing unemployment.22
headspace is serving young people outside major metropolitan areas — an excellent outcome for Australia, which struggles to provide an effective mental health service response in regional and rural areas.23 There has been a deliberate strategy to locate headspace centres in regional areas, with the aim of eventually providing national coverage so that all young people have reasonable access to services.
The presenting issues for young people attending headspace centres are primarily problems with how they feel, mostly related to feeling depressed or anxious. The initiative was set up to better respond to the need for care for such high-prevalence mental ill health in young people. However, formal diagnosis of mental disorder by an appropriately qualified clinician is available for only a small proportion of clients. This partly reflects the multidisciplinary nature of the headspace workforce, many of whom are not trained in formal diagnosis and who use psychotherapeutic approaches that are not diagnosis driven. It also suggests the need for an expanded diagnostic approach that incorporates clinician assessment of at-risk and subthreshold conditions.24 Over half the young people presenting were in the early stages of the development of mental disorder, having mild to moderate or subthreshold symptoms, as specifically targeted by the initiative. Nevertheless, almost 20% had an established disorder and about 10% had a serious ongoing disorder, showing the wide range of clinical presentations that headspace centres need to accommodate.
Received 24 September 2013, accepted 28 November 2013
- Debra J Rickwood1,2
- Nic R Telford2
- Alexandra G Parker2
- Chris J Tanti2
- Patrick D McGorry3
- 1 Faculty of Health, University of Canberra, Canberra, ACT.
- 2 headspace National Youth Mental Health Foundation, Melbourne, VIC.
- 3 Orygen Youth Health Research Centre, University of Melbourne, Melbourne, VIC.
We are all employed by or directly involved with headspace National Youth Mental Health Foundation.
- 1. McGorry PD, Tanti C, Stokes R, et al. headspace: Australia’s National Youth Mental Health Foundation — where young minds come first. Med J Aust 2007; 187 (7 Suppl): S68-S70. <MJA full text>
- 2. Slade T, Johnston A, Teesson M, et al. The mental health of Australians 2. Report on the 2007 National Survey of Mental Health and Wellbeing. Canberra: Australian Department of Health and Ageing, 2009.
- 3. Gibb SJ, Fergusson DM, Horwood LJ. Burden of psychiatric disorder in young adulthood and life outcomes at age 30. Br J Psychiatry 2010; 197: 122-127.
- 4. Merikangas KR, He JP, Burstein M, et al. Lifetime prevalence of mental disorders in US adolescents: results from the National Comorbidity Survey Replication—Adolescent Supplement (NCS-A). J Am Acad Child Adolesc Psychiatry 2010; 49: 980-989.
- 5. Kessler RC, Amminger GP, Aguilar-Gaxiola S, et al. Age of onset of mental disorders: a review of recent literature. Curr Opin Psychiatry 2007; 20: 359-364.
- 6. McGorry PD. The specialist youth mental health model: strengthening the weakest link in the public mental health system. Med J Aust 2007; 187 (7 Suppl): S53-S56. <MJA full text>
- 7. Rickwood DJ, Van Dyke N, Telford N. Innovation in youth mental health services in Australia: common characteristics across the first headspace centres. Early Interv Psychiatry 2013; 4 Jul [Epub ahead of print]. doi: 10.1111/eip.12071.
- 8. Gulliver A, Griffiths KM, Christensen H. Perceived barriers and facilitators to mental health help-seeking in young people: a systematic review. BMC Psychiatry 2010; 10: 113.
- 9. Rickwood DJ, Deane FP, Wilson CJ. When and how do young people seek professional help for mental health problems? Med J Aust 2007; 187 (7 Suppl): S35-S39. <MJA full text>
- 10. Kessler RC, Andrews G, Colpe LJ, et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med 2002; 32: 959-976.
- 11. McGorry PD, Purcell R, Hickie IB, et al. Clinical staging: a heuristic model for psychiatry and youth mental health. Med J Aust 2007; 187 (7 Suppl): S40-S42. <MJA full text>
- 12. Australian Bureau of Statistics. Mental health and wellbeing: profile of adults, Australia, 1997. Canberra: ABS, 1998. (ABS Cat. No. 4326.0.)
- 13. Goldman HH, Skodol AE, Lave TR. Revising Axis V for DSM-IV: a review of measures of social functioning. Am J Psychiatry 1992; 149: 1148-1156.
- 14. Australian Institute of Health and Welfare. Young Australians: their health and wellbeing 2011. Canberra: AIHW, 2011. (AIHW Cat. No. PHE 140.)
- 15. Australian Bureau of Statistics. Estimates of Aboriginal and Torres Strait Islander Australians, June 2011. Canberra: ABS, 2013. (ABS Cat. No. 3238.0.55.001.)
- 16. Australian Bureau of Statistics. Migration, Australia, 2007–08. Canberra: ABS, 2009. (ABS Cat. No. 3412.0.)
- 17. Australian Bureau of Statistics. Reflecting a nation: stories from the 2011 census. Canberra: ABS, 2013. (ABS Cat. No. 2071.0.)
- 18. Australian Bureau of Statistics. Population estimates by remoteness area, 2011 to 2012. Canberra: ABS, 2013. (ABS Cat. No. 3218.0.)
- 19. Australian Bureau of Statistics. 2011 Census of population and housing: estimating homelessness, 2011. Table 8 homeless operational groups and other marginal housing, number of persons–by selected characteristics–2011. Canberra: ABS, 2012. (ABS Cat. No. 2049.0.)
- 20. COAG Reform Council. Education in Australia 2012: five years of performance. Sydney: COAG Reform Council, 2013.
- 21. Australian Department of Health and Ageing. Promotion, prevention and early intervention for mental health: a monograph. Canberra: Australian Government, 2000.
- 22. Scott J, Fowler D, McGorry P, et al. Adolescents and young adults who are not in employment, education, or training. BMJ 2013; 347: f5270.
- 23. Carbone S, Rickwood D, Tanti C. Workforce shortages and their impact on Australian youth mental health service reform. Advances in Mental Health 2011; 10: 92-97.
- 24. Kessler RC, Merikangas KR, Berglund P, et al. Mild disorders should not be eliminated from the DSM-V. Arch Gen Psychiatry 2003; 60: 1117-1122.





Abstract
Objectives: To provide the first national profile of the characteristics of young people (aged 12–25 years) accessing headspace centre services — the Australian Government’s innovation in youth mental health service delivery — and investigate whether headspace is providing early service access for adolescents and young adults with emerging mental health problems.
Design and participants: Census of all young people accessing a headspace centre across the national network of 55 centres comprising a total of 21 274 headspace clients between 1 January and 30 June 2013.
Main outcome measures: Reason for presentation, Kessler Psychological Distress Scale, stage of illness, diagnosis, functioning.
Results: Young people were most likely to present with mood and anxiety symptoms and disorders, self-reporting their reason for attendance as problems with how they felt. Client demographic characteristics tended to reflect population-level distributions, although clients from regional areas and of Aboriginal and Torres Strait Islander background were particularly well represented, whereas those who were born outside Australia were underrepresented.
Conclusion: headspace centres are providing a point of service access for young Australians with high levels of psychological distress and need for care in the early stages of the development of mental disorder.