This is a republished version of an article previously published in MJA Open
Vitamin B12 (cobalamin) is an essential vitamin, required for DNA synthesis (and ultimately cell division) and for maintaining nerve myelin integrity.1 It is found almost exclusively in animal-based products including red meats, poultry, seafood, milk, cheese and eggs. As vitamin B12 is produced by bacteria in the large intestines of animals, plant-based foods are generally not a source of vitamin B12. It is therefore a nutrient of concern for vegetarians and particularly for vegans who choose an entirely plant-based diet. A cross-sectional analysis study involving 689 men found that more than half of vegans and 7% of vegetarians were deficient in vitamin B12.2
Vitamin B12 deficiency is a serious health problem that can result in megaloblastic anaemia, inhibition of cell division, and neurological disorders.3 Folate deficiency can also cause megaloblastic anaemia and, although a high folate intake may correct anaemia from a vitamin B12 deficiency, subtle neurological symptoms driven by the vitamin B12 deficiency may arise. Loss of intrinsic factor, gastric acid or other protein-digesting enzymes contributes to 95% of known cases of vitamin B12 deficiency.4 Other factors that may contribute to vitamin B12 deficiency are listed in Box 1.13 However, in vegetarian and vegan populations, dietary insufficiency is the major cause.4 Furthermore, high levels of folate can mask vitamin B12 deficiency — a concern for vegetarians and vegans whose folate intake is generally high while vitamin B12 intake is low. The addition of vitamin B12 to any foods fortified with folate has been advocated to prevent masking of haematological and neurological manifestations of vitamin B12 deficiency.14 Subtle neurological damage (even in the absence of anaemia) may be more likely in vegans because of their increased folate levels preventing early detection of vitamin B12 deficiency.4
Vitamin B12 deficiency can also lead to demyelinisation of peripheral nerves, the spinal cord, cranial nerves and the brain, resulting in nerve damage and neuropsychiatric abnormalities. Neurological symptoms of vitamin B12 deficiency include numbness and tingling of the hands and feet, decreased sensation, difficulties walking, loss of bowel and bladder control, memory loss, dementia, depression, general weakness and psychosis.3,4 Unless detected and treated early, these symptoms can be irreversible.
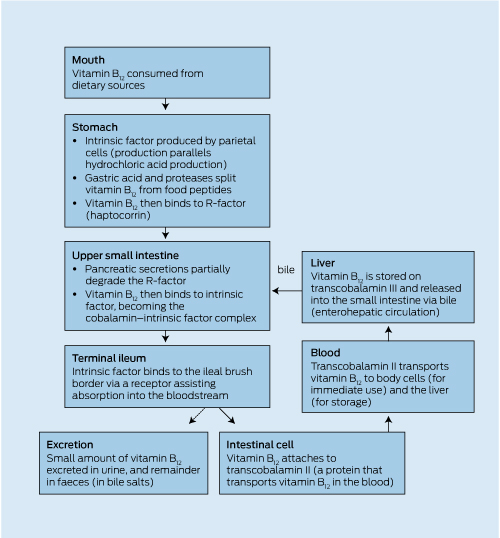
The digestion of vitamin B12 begins in the stomach, where gastric secretions and proteases split vitamin B12 from peptides. Vitamin B12 is then free to bind to R-factor found in saliva. Pancreatic secretions partially degrade the R-factor, and vitamin B12 is then bound to intrinsic factor. Intrinsic factor binds to the ileal brush border and facilitates the absorption of vitamin B12.15 Box 2 illustrates the process of vitamin B12 digestion and absorption. Vitamin B12 absorption may decrease if intrinsic factor production decreases. There are many well documented factors causing protein-bound vitamin B12 malabsorption, including gastric resection, atrophic gastritis, and the use of medications that suppress acid secretion (see Box 1).
Up to 89% of vitamin B12 consumed in the diet is absorbed, although as little as 9% is absorbed from some foods (including eggs).17,18 This relatively high rate of absorption, combined with low daily requirements and the body’s extremely efficient enterohepatic circulation of vitamin B12, contributes to the long period, often years, for a deficiency to become evident. Studies have been inconsistent in linking the duration of following an unsupplemented vegan diet with low serum levels of vitamin B12.2,19 Intestinal absorption is estimated to be saturated at about 1.5–2.0 µg per meal, and bioavailability significantly decreases as intake increases.18
Ageing causes a decreased level of proteases, as well as a reduced level of acid in the stomach. As a result, vitamin B12 is less effectively removed from the food proteins to which it is attached, and food-bound vitamin B12 absorption is diminished.4 The Framingham Offspring Study found that the vitamin B12 from supplements and fortified foods may be more efficiently absorbed than that from meat, fish and poultry.20
While low vitamin B12 status in vegetarians and vegans is predominantly due to inadequate intake, some cases of pernicious anaemia are attributable to inadequate production of intrinsic factor. Under the law of mass action, about 1% of vitamin B12 from large oral doses can be absorbed across the intestinal wall, even in the absence of adequate intrinsic factor.21
Taking a simple diet history can be a useful indicator of vitamin B12 intake and adequacy. However, laboratory analyses provide a much more accurate assessment. Measurement of serum vitamin B12 levels is a common and low-cost method of assessing vitamin B12 status. The earlier method of measuring vitamin B12 using biological assays was unreliable, as both the active and inactive analogues of vitamin B12 were detected, so levels were often overestimated.17 Modern radio isotope and immunoassay methods reliably measure biologically available analogues of vitamin B12. The early measured ranges of acceptable levels of serum vitamin B12 were determined using individuals who were apparently healthy but had potentially marginal levels of vitamin B12. This has resulted in reference intervals probably being set too low to provide a reliable clinical decision. To improve the ability to predict marginal vitamin B12 status, a higher reference interval (> 360 pmol/L) has been proposed.4,22 Objective measures of neurological damage have been found in patients with vitamin B12 levels below 258 pmol/L.23 However, the usual reference interval for vitamin B12 deficiency is < 220 pmol/L. Achieving national and international agreement on the definition of serum vitamin B12 deficiency would provide some clarity for comparison of studies and reduce variability in defining those at risk of deficiency. Internationally, the cut-off for vitamin B12 varies markedly between < 130 pmol/L and < 258 pmol/L.
Serum vitamin B12 levels alone do not provide a measure of a person’s reserves of the vitamin. It is recommended that a metabolic marker of vitamin B12 reserves, such as serum homocysteine, also be determined. Elevated homocysteine levels can be a useful indicator for vitamin B12 deficiency, because serum homocysteine levels increase as vitamin B12 stores fall. While serum homocysteine levels greater than 9 µmol/L suggest the beginning of depleted vitamin B12 reserves,24 standard laboratory reference intervals suggest levels greater than 15 µmol/L as a marker for depleted vitamin B12 reserves. Although homocysteine levels may also increase with folate or vitamin B6 deficiency, these deficiencies are likely to be rare in vegetarians and vegans.
Other markers for vitamin B12 deficiency include serum holotranscobalamin II (TC2) and urinary or serum methylmalonic acid (MMA). TC2 is the protein that transports vitamin B12 in blood, and its levels fall in vitamin B12 deficiency. Testing for this carrier protein can identify low vitamin B12 status before total serum vitamin B12 levels drop.25 Vitamin B12 is the only coenzyme required in the conversion of methylmalonyl-CoA to succinyl-CoA, so methylmalonyl-CoA levels increase with vitamin B12 deficiency. As it is toxic, methylmalonyl-CoA is converted to MMA, which accumulates in the blood and is excreted in the urine, enabling either urinary or serum MMA to be a useful measure of vitamin B12 reserves. Because TC2 is one of the earliest markers of vitamin B12 deficiency, it may be one of the better means of assessing vitamin B12 status.22
Box 3 shows the vitamin B12 nutrient reference values for Australia and New Zealand.26 As no recommended dietary intakes (RDIs) are available for infants under 12 months of age, an adequate intake is recommended instead. Vegans at all stages of the life cycle need to ensure an adequate and reliable source of vitamin B12 from fortified foods, or they will require supplementation equivalent to the RDI.
While reported cases of frank vitamin B12 deficiency in vegetarians or vegans are rare, several studies have found lower vitamin B12 levels in vegans and vegetarians compared with the general population.27,28 The European Prospective Investigation into Cancer and Nutrition (EPIC)-Oxford cohort study found that 121 of 232 vegans (52%), 16 of 231 vegetarians (7%) and one of 226 omnivores (0.4%) were classed as vitamin B12-deficient.2 There was no significant association between age or duration of subjects’ adherence to a vegetarian or vegan diet and the serum levels of vitamin B12.2 Intuitively, it is assumed that prevalence of deficiency increases with a longer duration of vegetarian diet. Although it can take years for deficiency to occur, it is likely that all vegans and anyone who does not regularly consume animal-based foods, and whose diets are unsupplemented or unfortified, will eventually develop vitamin B12 deficiency. Vegetarians and vegans should have their vitamin B12 status regularly assessed to enable early intervention if levels fall too low.
The risk of a breastfed infant becoming deficient in vitamin B12 depends on three factors: the vitamin B12 status of the mother during pregnancy; the vitamin B12 stores of the infant at birth; and the vitamin B12 status of the breastfeeding mother. The fetus obtains its initial store of vitamin B12 via the placenta, with newly absorbed vitamin B12 (rather than maternal stores) being readily transported across the placenta.29 Under normal conditions, full-term infants will have enough stored vitamin B12 at birth to last for about 3 months when the maternal diet does not contain vitamin B12.30 An infant born to a vegetarian or vegan mother is at high risk of deficiency if the mother’s vitamin B12 intake is inadequate and her stores are low. Vegetarian women who have repeated pregnancies place infants at greater risk, because their vitamin B12 stores are likely to have been depleted by earlier pregnancies.31 Vegetarian or vegan women must have a balanced diet, including adequate intake of vitamin B12, to provide for their babies during both pregnancy and lactation. Recent studies suggest that maternal stores of vitamin B12 are also reflected in breastmilk. When maternal serum vitamin B12 levels are low, vitamin B12 levels in breastmilk will also be low, and the infant will not receive an adequate vitamin B12 intake.32
There have been reports of deficiency in the breastfed infants of vegan (or “strict vegetarian”) mothers who did not supplement their diets with vitamin B12, because of the smaller stores of vitamin B12 gained by the infant during pregnancy and the low vitamin B12 content of breastmilk (reflective of the mothers’ serum levels).33,34 Infants have presented with a range of symptoms, often initially signalled by developmental delay.35 Lack of vitamin B12 in the maternal diet during pregnancy has been shown to cause severe retardation of myelination in the nervous system of the infant.36 Visible signs of vitamin B12 deficiency in infants may include involuntary motor movements, dystrophy, weakness, muscular atrophy, loss of tendon reflexes, psychomotor regression, cerebral atrophy, hypotonia and haematological abnormalities.37,38 While supplementation with vitamin B12 results in rapid improvements in laboratory measures of vitamin B12 status, there is continuing research about the long-term effects of deficiency in infants.37
It was once thought that some plant foods, such as spirulina, and fermented soy products, including tempeh and miso, were dietary sources of vitamin B12, but this has been proven incorrect.39 Recent research has found traces of vitamin B12 in white button mushrooms40 and Korean purple laver (nori),41 but the quantity in a typical serving means that they are not a significant dietary source of this vitamin. An average serving of mushrooms contains about 5% of the RDI, making the quantity required to supply adequate amounts of vitamin B12 to vegetarians impractical. Further, use of Korean laver is unlikely to be widespread in the Australian diet. With the unique exception of these two plant foods,40,41 any vitamin B12 detected in other plant foods is likely to be the inactive analogue, which is of no use to the body and can actually interfere with the absorption of the active form.42
Box 4 shows a sample vegetarian meal plan for a 19–50-year-old woman, which includes food sources typical in a Western-style diet and meets the RDI of vitamin B12 and requirements for other key nutrients (except vitamin D and long-chain omega-3 fatty acids). Excluding or limiting dairy foods or fortified soy milk from the vegetarian diet would necessitate the need for vitamin B12 supplements.
In contrast to the United States, where foods are extensively fortified with vitamin B12, Food Standards Australia New Zealand permits only a limited number of foods to be fortified with vitamin B12. This includes selected soy milks, yeast spread, and vegetarian meat analogues such as soy-based burgers and sausages. Examples of the vitamin B12 content of foods suitable for vegetarians are shown in Box 5.
In a vegan diet, using a supplement or consuming fortified foods is the only way to obtain vitamin B12. As the body can only absorb a limited amount of vitamin B12 at any one time, it is better to take small doses more often, instead of large doses less often. One study found that small doses of vitamin B12 in the range of 0.1–0.5 µg resulted in absorption ranging between 52% and 97%; doses of 1 µg and 5 µg resulted in mean absorption of 56% and 28%, respectively, while higher doses had even lower absorption, with 10 µg and 50 µg doses resulting in 16% and 3%, respectively, being absorbed.17 While sublingual supplements are often promoted as being more efficiently absorbed, there is no evidence to show that this form of supplement is superior to regular oral vitamin B12.44 Vitamin B12 supplements are not made from animal-based products and are suitable for inclusion in a vegan diet.
1 Causes of vitamin B12 deficiency, with contributing factors
Inadequate absorption or impaired utilisation
Loss of intrinsic factor, loss of gastric acid and/or other protein-digesting enzymes (contributes to 95% of known cases)4
Use of medications that suppress acid secretion, including somatostatin, cholecystokinin, atrial natriuretic peptide, and nitric oxide5
Pancreatic disease
Gastric resection, sleeve or banding surgery6
Ileal disease or ileal resection (secondary to Crohn’s disease)7
Use of metformin (oral hypoglycaemic agent)6
Use of angiotensin-converting enzyme inhibitor9
Use of levodopa and catechol-O-methyltransferase inhibitors10
Autoimmunity to intrinsic factor
Gastric infection with Helicobacter pylori11
Ileocystoplasty12
Atrophic gastritis
3 Recommended dietary intake (RDI)* and estimated average requirement (EAR)† of vitamin B12 per day26
4 A sample vegetarian meal plan designed to meet requirements for vitamin B12 and other key nutrients for a 19–50-year-old woman, showing vitamin B12 content of the foods*
Provenance: Commissioned by supplement editors; externally peer reviewed.
- Carol L Zeuschner1
- Bevan D Hokin1
- Kate A Marsh2
- Angela V Saunders3
- Michelle A Reid3
- Melinda R Ramsay4
- 1 Sydney Adventist Hospital, Sydney, NSW.
- 2 Northside Nutrition and Dietetics, Sydney, NSW.
- 3 Corporate Nutrition, Sanitarium Health and Wellbeing, Berkeley Vale, NSW.
- 4 Sanitarium Health and Wellbeing Services, Sanitarium Health and Wellbeing, Sydney, NSW.
We acknowledge the assistance of dietitians Sue Radd and Rebecca Prior in the early development stages of this article.
Kate Marsh previously consulted for Nuts for Life (Horticulture Australia), who are providing a contribution towards the cost of publishing this supplement. Angela Saunders, Michelle Reid and Melinda Ramsay are employed by Sanitarium Health and Wellbeing, sponsor of this supplement.
- 1. Cameron DG, Townsend SR, English A. Pernicious anaemia II: maintenance treatment with crystalline vitamin B12. Can Med Assoc J 1954; 70: 398-400.
- 2. Gilsing AM, Crowe FL, Lloyd-Wright Z, et al. Serum concentrations of vitamin B12 and folate in British male omnivores, vegetarians and vegans: results from a cross-sectional analysis of the EPIC-Oxford cohort study. Eur J Clin Nutr 2010; 64: 933-939.
- 3. Allen RH, Stabler SP, Savage DG, Lindenbaum J. Metabolic abnormalities in cobalamin (vitamin B12) and folate deficiency. FASEB J 1993; 7: 1344-1353.
- 4. Mangels R, Messina V, Messina M. The dietitians’ guide to vegetarian diets: issues and applications. 3rd ed. Sudbury, MA: Jones & Bartlett Learning, 2010.
- 5. Schubert ML. Gastric secretion. Curr Opin Gastroenterol 2007; 23: 595-601.
- 6. Aarts EO, Janssen IM, Berends FJ. The gastric sleeve: losing weight as fast as micronutrients? Obes Surg 2011; 21: 207-211.
- 7. Yakut M, Ustün Y, Kabaçam G, Soykan I. Serum vitamin B12 and folate status in patients with inflammatory bowel diseases. Eur J Intern Med 2010; 21: 320-323.
- 8. De Jager J, Kooy A, Lehert P, et al. Long term treatment with metformin in patients with type 2 diabetes and risk of vitamin B-12 deficiency: randomised placebo controlled trial. BMJ 2010; 340: c2181.
- 9. Tal S, Shavit Y, Stern F, Malnick S. Association between vitamin B12 levels and mortality in hospitalized older adults. J Am Geriatr Soc 2010; 58: 523-526.
- 10. Triantafyllou NI, Kararizou E, Angelopoulos E, et al. The influence of levodopa and the COMT inhibitor on serum vitamin B12 and folate levels in Parkinson’s disease patients. Eur Neurol 2007; 58: 96-99.
- 11. Kaptan K, Beyan C, Ural AU, et al. Helicobacter pylori--is it a novel causative agent in vitamin B12 deficiency? Arch Intern Med 2000; 160: 1349-1353.
- 12. Vanderbrink BA, Cain MP, King S, et al. Is oral vitamin B(12) therapy effective for vitamin B(12) deficiency in patients with prior ileocystoplasty? J Urol 2010; 184 (4 Suppl): 1781-1785.
- 13. Herbert V. Vitamin B12. In: Brown ML, editor. Present knowledge in nutrition. 5th ed. Washington, DC: Nutrition Foundation, 1984: 347-364.
- 14. Herbert V, Bigaouette J. Call for endorsement of a petition to the Food and Drug Administration to always add vitamin B-12 to any folate fortification or supplement. Am J Clin Nutr 1997; 65: 572-573.
- 15. Festen HP. Intrinsic factor secretion and cobalamin absorption. Physiology and pathophysiology in the gastrointestinal tract. Scand J Gastroenterol Suppl 1991; 188: 1-7.
- 16. Messina G, Norris J. Digestion, absorption, and transport. http://www.veganhealth.org/b12/dig (accessed Jun 2011).
- 17. Herbert V. Recommended dietary intakes (RDI) of vitamin B-12 in humans. Am J Clin Nutr 1987; 45: 671-678.
- 18. Watanabe F. Vitamin B12 sources and bioavailability. Exp Biol Med (Maywood) 2007; 232: 1266-1274.
- 19. Tungtrongchitr R, Pongpaew P, Prayurahong B, et al. Vitamin B12, folic acid and haematological status of 132 Thai vegetarians. Int J Vitam Nutr Res 1993; 63: 201-207.
- 20. Tucker KL, Rich S, Rosenberg I, et al. Plasma vitamin B-12 concentrations relate to intake source in the Framingham Offspring study. Am J Clin Nutr 2000; 71: 514-522.
- 21. Altay C, Cetin M. Oral treatment in selective vitamin B12 malabsorption. J Pediatr Hematol Oncol 1997; 19: 245-246.
- 22. Herrmann W, Obeid R, Schorr H, Geisel J. Functional vitamin B12 deficiency and determination of holotranscobalamin in populations at risk. Clin Chem Lab Med 2003; 41: 1478-1488.
- 23. Lindenbaum J, Healton EB, Savage DG, et al. Neuropsychiatric disorders caused by cobalamin deficiency in the absence of anemia or macrocytosis. N Engl J Med 1988; 318: 1720-1728.
- 24. Ubbink JB. What is a desirable homocysteine level? In: Carmel R, Jacobsen DW, editors. Homocysteine in health and disease. Cambridge, UK: Cambridge University Press, 2001: 485-490.
- 25. Herzlich B, Herbert V. Depletion of serum holotranscobalamin II. An early sign of negative vitamin B12 balance. Lab Invest 1988; 58: 332-337.
- 26. National Health and Medical Research Council, New Zealand Ministry of Health. Nutrient reference values for Australia and New Zealand including recommended dietary intakes. Canberra: NHMRC, 2006. http://www.nhmrc.gov.au/guidelines/publications/n35-n36-n37 (accessed May 2012).
- 27. Hokin BD, Butler T. Cyanocobalamin (vitamin B-12) status in Seventh-day Adventist ministers in Australia. Am J Clin Nutr 1999; 70 (3 Suppl): 576S-578S.
- 28. Miller DR, Specker BL, Ho ML, Norman EJ. Vitamin B-12 status in a macrobiotic community. Am J Clin Nutr 1991; 53: 524-529.
- 29. Allen LH. Vitamin B12 metabolism and status during pregnancy, lactation and infancy. Adv Exp Med Biol 1994; 352: 173-186.
- 30. Allen LH. Impact of vitamin B-12 deficiency during lactation on maternal and infant health. Adv Exp Med Biol 2002; 503: 57-67.
- 31. Allen LH, Rosado JL, Casterline JE, et al. Vitamin B-12 deficiency and malabsorption are highly prevalent in rural Mexican communities. Am J Clin Nutr 1995; 62: 1013-1019.
- 32. Specker BL, Black A, Allen L, Morrow F. Vitamin B-12: low milk concentrations are related to low serum concentrations in vegetarian women and to methylmalonic aciduria in their infants. Am J Clin Nutr 1990; 52: 1073-1076.
- 33. Renault F, Verstichel P, Ploussard JP, Costil J. Neuropathy in two cobalamin-deficient breast-fed infants of vegetarian mothers. Muscle Nerve 1999; 22: 252-254.
- 34. Weiss R, Fogelman Y, Bennett M. Severe vitamin B12 deficiency in an infant associated with a maternal deficiency and a strict vegetarian diet. J Pediatr Hematol Oncol 2004; 26: 270-271.
- 35. Grattan-Smith PJ, Wilcken B, Procopis PG, Wise GA. The neurological syndrome of infantile cobalamin deficiency: developmental regression and involuntary movements. Mov Disord 1997; 12: 39-46.
- 36. Lövblad K, Ramelli G, Remonda L, et al. Retardation of myelination due to dietary vitamin B12 deficiency: cranial MRI findings. Pediatr Radiol 1997; 27: 155-158.
- 37. Casella EB, Valente M, de Navarro JM, Kok F. Vitamin B12 deficiency in infancy as a cause of developmental regression. Brain Dev 2005; 27: 592-594.
- 38. Kühne T, Bubl R, Baumgartner R. Maternal vegan diet causing a serious infantile neurological disorder due to vitamin B12 deficiency. Eur J Pediatr 1991; 150: 205-208.
- 39. Van den Berg H, Dagnelie PC, van Staveren WA. Vitamin B12 and seaweed [letter]. Lancet 1988; 1(8579): 242-243.
- 40. Koyyalamudi SR, Jeong SC, Cho KY, Pang G. Vitamin B12 is the active corrinoid produced in cultivated white button mushrooms (Agaricus bisporus). J Agric Food Chem 2009; 57: 6327-6333.
- 41. Miyamoto E, Yabuta Y, Kwak CS, et al. Characterization of vitamin B12 compounds from Korean purple laver (Porphyra sp.) products. J Agric Food Chem 2009; 57: 2793-2796.
- 42. Dagnelie PC, van Staveren WA, van den Berg H. Vitamin B-12 from algae appears not to be bioavailable. Am J Clin Nutr 1991; 53: 695-697.
- 43. Food Standards Australia New Zealand. NUTTAB 2010 online searchable database. http://www.foodstandards.gov.au/consumerinformation/nuttab2010/nuttab2010onlinesearchable database/onlineversion.cfm (accessed Nov 2011).
- 44. Yazaki Y, Chow G, Mattie M. A single-center, double-blinded, randomized controlled study to evaluate the relative efficacy of sublingual and oral vitamin B-complex administration in reducing total serum homocysteine levels. J Altern Complement Med 2006; 12: 881-885.





Abstract
Vitamin B12 is found almost exclusively in animal-based foods and is therefore a nutrient of potential concern for those following a vegetarian or vegan diet. Vegans, and anyone who significantly limits intake of animal-based foods, require vitamin B12-fortified foods or supplements.
Vitamin B12 deficiency has several stages and may be present even if a person does not have anaemia. Anyone following a vegan or vegetarian diet should have their vitamin B12 status regularly assessed to identify a potential problem.
A useful process for assessing vitamin B12 status in clinical practice is the combination of taking a diet history, testing serum vitamin B12 level and testing homocysteine, holotranscobalamin II or methylmalonic acid serum levels.
Pregnant and lactating vegan or vegetarian women should ensure an adequate intake of vitamin B12 to provide for their developing baby.
In people who can absorb vitamin B12, small amounts (in line with the recommended dietary intake) and frequent (daily) doses appear to be more effective than infrequent large doses, including intramuscular injections.
Fortification of a wider range of foods products with vitamin B12, particularly foods commonly consumed by vegetarians, is likely to be beneficial, and the feasibility of this should be explored by relevant food authorities.