We report the first two Australian cases of flood-related takotsubo cardiomyopathy, in patients who were trapped by life-threatening flash floods in and near Toowoomba, Queensland. It is well recognised that events that incite significant physical and emotional stress in individuals can trigger this syndrome, which often mimics acute myocardial infarction.
On 10 January 2011, at about 13:30, the Queensland city of Toowoomba experienced flash flooding caused by intense rainfall over the catchment areas of three creeks that traverse the city.1 When the central business district was hit by “a wave of water”, a 66-year-old female resident became trapped in her flooded and spinning car. She was removed from her car by witnesses. That evening she developed chest pain with associated shortness of breath and palpitations. The pain came and went throughout the night before she attended the local hospital.
Patient 2 was a 68-year-old female resident of the Lockyer Valley, located about 10 kilometres to the east of Toowoomba. At about 14:00 on 10 January 2011, the region experienced extremely rapid flooding of sufficient strength to carry cars.1
The patient was transferred to our tertiary hospital for ongoing assessment and management.
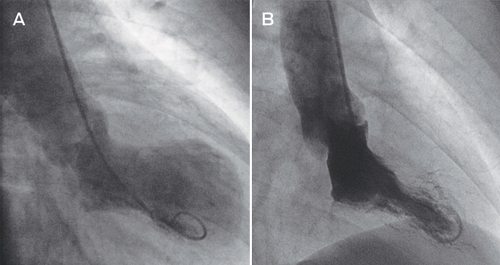
Selective coronary angiography revealed no significant coronary artery stenosis. Left ventriculography demonstrated left ventricular systolic dysfunction with severe hypokinesis and apical ballooning (Box, A). Transthoracic echocardiography confirmed the left ventriculography findings. There was no evidence of myocardial infarction on cardiac magnetic resonance imaging. We made a diagnosis of takotsubo cardiomyopathy.
The syndrome was first reported in the Japanese cardiology literature in 1991.2 It is named for the resemblance of left ventricle morphology on ventriculography during the acute phase to that of a Japanese octopus trap and is synonymous with the terms apical ballooning syndrome or ampulla cardiomyopathy. Since the initial description, at least two other accepted ballooning patterns (mid ventricular and basal) have been described.3
Takotsubo cardiomyopathy is colloquially known as “broken heart syndrome” or “stress cardiomyopathy”, acknowledging its frequent association with extreme emotional or physical stressors. The exact mechanism of the acute cardiomyopathy is unclear, but is likely to be secondary to abnormal responses to acute catecholamine surges. Examples of physical stressors include acute respiratory illnesses, administration of exogenous catecholamines (adrenaline, noradrenaline, or dobutamine in patients undergoing stress echocardiography), and acute subarachnoid haemorrhage. Takotsubo cardiomyopathy may occur in patients under general anaesthesia, suggesting an autonomic nervous system mechanism.4 The syndrome most often affects postmenopausal women;3,4 up to 90% have an identifiable stressful trigger event.4 Complete recovery from the syndrome is observed in nearly all cases (96%) within 7 to 37 days.5 Recurrence rates are reported to be between 5% and 10%.6 Mortality rates are low and published cases of death are rare.
Reported rates of acute coronary syndromes show increases after natural disasters. Onset of myocardial infarction is associated with acute physiological stress, from everyday triggers including the circadian rhythm (peak prevalence in the morning hours) to physical activity and severe meteorological events.7 Stressor events increase sympathetic activation of the autonomic nervous system, increasing blood pressure, heart rate, myocardial contractility and, consequently, myocardial oxygen demand. They are also associated with increased platelet aggregability, other prothrombotic changes, and altered intravascular sheer stress, which may disrupt atherosclerotic plaques, resulting in coronary artery occlusion and ischaemia.
Until very recently, the link between takotsubo cardiomyopathy and natural disasters had received little attention,8 although increased prevalence of acute coronary syndrome presentations coinciding with extreme natural events has been previously documented.9 Given that takotsubo cardiomyopathy has been under-recognised until recently and that it mimics myocardial infarction and coronary artery spasm, we suspect that takotsubo cardiomyopathy may explain some of the historically recognised instances of increased acute coronary syndromes during and shortly after natural disasters.
- 1. Holmes CE. Queensland Floods Commission of Inquiry. Final report. Brisbane: Queensland Government, 2012.
- 2. Dote K, Sato H, Tateishi H, et al. [Myocardial stunning due to simultaneous multivessel coronary spasms: a review of 5 cases] [Japanese]. J Cardiol 1991; 21: 203-214.
- 3. Eitel I, von Knobelsdorff-Brenkenhoff F, Bernhardt P, et al. Clinical characteristics and cardiovascular magnetic resonance findings in stress (takotsubo) cardiomyopathy. JAMA 2011; 306: 277-286.
- 4. Sharkey SW, Windenburg DC, Lesser JR, et al. Natural history and expansive clinical profile of stress (tako-tsubo) cardiomyopathy. J Am Coll Cardiol 2010; 55: 333-341.
- 5. Pernicova I, Garg S, Bourantas CV, et al. Takotsubo cardiomyopathy: a review of the literature. Angiology 2010; 61: 166-173.
- 6. Bybee KA, Kara T, Prasad A, et al. Systematic review: transient left ventricular apical ballooning: a syndrome that mimics ST-segment elevation myocardial infarction. Ann Intern Med 2004; 141: 858-865.
- 7. Culic V, Eterovic D, Miric D. Meta-analysis of possible external triggers of acute myocardial infarction. Int J Cardiol 2005; 99: 1-8.
- 8. Trebouet E, Prieur S, Dimet J, et al. Cardiovascular emergencies related to the Xynthia storm. Am J Emerg Med 2012; 30: 377-379.
- 9. Watanabe H, Kodama M, Okura Y, et al. Impact of earthquakes on Takotsubo cardiomyopathy. JAMA 2005; 294: 305-307.





No relevant disclosures.