This is the first reported Australian case of synovial sarcoma of the pharynx. A 29-year-old man had a large hypopharyngeal mass excised and received radiotherapy and chemotherapy. No recurrence was seen 12 months later.
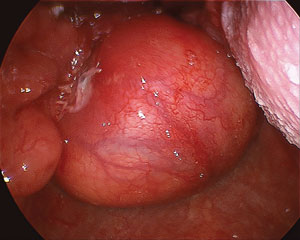
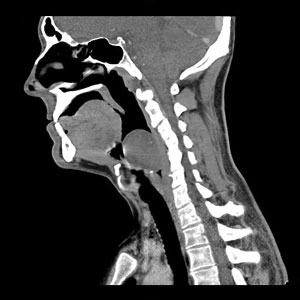
Flexible endoscopy examination revealed a well circumscribed, encapsulated tumour arising from the left lower lateral wall of the oropharynx and hypopharynx, and from the left arytenoid on its posterior aspect (Box 1). Computed tomography (CT) scanning revealed a 3 × 4.1 cm soft tissue mass arising from the left pharyngeal wall just inferior to the tonsillar fossa (Box 2).
Synovial sarcomas are high-grade soft tissue sarcomas that are thought to arise from pluripotential mesenchymal stem cells.1,2 They account for 10% of all soft tissue sarcomas, and less than 10% occur in the head and neck region.2,3 Since the first case of head and neck synovial sarcoma was described in 1954, there have been fewer than 200 cases reported in the world literature.4 Published cases of synovial sarcoma of the pharynx are rare,5-9 and to our knowledge, this is the first reported case in Australia.
There is a male predominance, with a male-to-female ratio of 3 : 2, and although synovial sarcomas can occur at any age, they are most commonly found in patients aged between 25 and 35 years.5,9,10 The neck is the most commonly reported site for primary synovial sarcoma within the head and neck, followed by the upper aerodigestive tract.4 The most typical presentation is a painless mass;2 however, pain, odynophagia, otalgia, bleeding and, in rare cases, pulmonary metastases have also been described.
Our patient presented with non-specific upper aerodigestive symptoms, which highlights the importance of a thorough clinical examination. Case reports of pharyngeal synovial sarcomas have found that most patients present within 3 months of the onset of symptoms.5-7 This is in contrast with our patient, who presented after years of loud snoring, progressive globus sensation and eventually stridor. This resulted in a very large tumour almost completely occluding the airway.
There are two types of synovial sarcoma, monophasic and biphasic.11 Two-thirds are biphasic, comprising a mixture of elongated basophilic spindle cells and glandular structures made of columnar epithelial cells. Monophasic forms are composed solely of spindle cells or, very rarely, epithelial cells. Monophasic forms are easier to misdiagnose as fibrosarcomas or malignant peripheral nerve sheath tumours, and immunohistochemistry that shows positive reactions for keratin and EMA and FISH can help differentiate these from other sarcomas.1,11
Work-up should include PET and CT scanning of the head, neck and chest to determine the extent of local disease and to search for metastases. The treatment of choice is complete surgical excision with clear margins and adjuvant radiotherapy.4,12-14 For soft tissue sarcomas in general, clear margins have been associated with reduced recurrence and improved survival.12,14 The issue of margin status is particularly important for pharyngeal disease, where attaining wide margins is technically more difficult, and postoperative function for speech and swallowing are important considerations.
Postoperative radiotherapy is increasingly recommended as it is associated with reduced local recurrence;4,13,14 however, a survival advantage is yet to be demonstrated. Treatment of the cervical lymph nodes in patients with nodal disease should comprise therapeutic lymph node dissection. There have been no studies on the roles of elective lymph node dissection and prophylactic regional radiotherapy in node-negative patients, and this is an area for future research.
The role of neoadjuvant or adjuvant chemotherapy for synovial sarcoma is inconclusive. In a meta-analysis of 14 randomised controlled trials,15 doxorubicin-based chemotherapy was associated with improved recurrence-free survival but not overall survival. A more recent study on ifosfamide-based chemotherapy for synovial sarcomas of the extremities showed an improvement in disease-specific survival.16 As always, the benefits of chemotherapy need to be weighed against the potential significant side effects.
Synovial sarcoma is an aggressive disease with a 5-year survival rate of less than 75%.17 There are conflicting conclusions regarding survival among patients with head and neck disease, with some authors reporting a better prognosis for synovial sarcomas of the head and neck compared with the extremities,18 and others reporting a worse prognosis.19 Favourable prognostic indicators include younger age (< 20 years), monophasic subtype, wide excision and, most significantly, smaller tumour size (< 5 cm).3,4
Disease recurrence is a significant problem, with up to 45% of patients with head and neck synovial sarcoma developing a local recurrence and 33% developing distant metastatic disease.4 Further, recurrences occur late, with a mean time to local recurrence of 3.6 years and a mean time to distant recurrence of 5.7 years reported for whole-body synovial sarcoma.17 This highlights the importance of long-term follow-up for these usually younger patients. All patients should initially undergo monthly review, with thorough clinical examination including nasoendoscopy of the pharynx. Where resources permit, patients should also be offered follow-up PET scanning, as this is a sensitive test for detecting recurrent disease.
- 1. Sturgis EM, Potter BO. Sarcomas of the head and neck region. Curr Opin Oncol 2003; 15: 239-252.
- 2. Carrillo R, Rodriguez-Peralto JL, Batsakis JG. Synovial sarcomas of the head and neck. Ann Otol Rhinol Laryngol 1992; 101: 367-370.
- 3. Amble FR, Olsen KD, Nascimento AG, Foote RL. Head and neck synovial cell sarcoma. Otolaryngol Head Neck Surg 1992; 107: 631-637.
- 4. Harb WJ, Luna MA, Patel SR, et al. Survival in patients with synovial sarcoma of the head and neck: association with tumor location, size, and extension. Head Neck 2007; 29: 731-740.
- 5. Saydam L, Kizilay A, Kalcioglu MT, et al. Synovial sarcoma of the pharynx: a case report. Ear Nose Throat J 2002; 81: 36-39.
- 6. Chew KK, Sethi DS, Stanley RE, et al. View from beneath: pathology in focus. Synovial sarcoma of hypopharynx. J Laryngol Otol 1992; 106: 285-287.
- 7. Shaariyah MM, Mazita A, Masaany M, et al. Synovial sarcoma: a rare presentation of parapharyngeal mass. Chin J Cancer 2010; 29: 631-633.
- 8. Palmer BV, Levene A, Shaw HJ. Synovial sarcoma of the pharynx and oesophagus. J Laryngol Otol 1983; 97: 1173-1176.
- 9. Betal D, Babu R, Mehmet V. Monophasic synovial sarcoma of the pharynx: a case report. Int Semin Surg Oncol 2009; 6: 9.
- 10. Onerci M, Sarioglu T, Gedikoglu G, et al. Synovial sarcoma in the neck. Int J Pediatr Otorhinolaryngol 1993; 27: 79-84.
- 11. Fletcher CDM, McKee. Soft tissue tumours. In: McGee JO, Isaacson PG, Wright NA, editors. Oxford textbook of pathology. Vol 2b. Oxford: Oxford University Press, 1992: 2131-2132.
- 12. Guadagnolo BA, Zagars GK, Ballo MT, et al. Long-term outcomes for synovial sarcoma treated with conservation surgery and radiotherapy. Int J Radiat Oncol Biol Phys 2007; 69: 1173-1180.
- 13. Mamelle G, Richard J, Luboinski B, et al. Synovial sarcoma of the head and neck: an account of four cases and review of the literature. Eur J Surg Oncol 1986; 12: 347-349.
- 14. Italiano A, Penel N, Robin YM, et al. Neo/adjuvant chemotherapy does not improve outcome in resected primary synovial sarcoma: a study of the French Sarcoma Group. Ann Oncol 2009; 20: 425-430.
- 15. Sarcoma Meta-analysis Collaboration. Adjuvant chemotherapy for localised resectable soft-tissue sarcoma of adults: meta-analysis of individual data. Lancet 1997; 350: 1647-1657.
- 16. Eilber FC, Brennan MF, Eilber FR, et al. Chemotherapy is associated with improved survival in adult patients with primary extremity synovial sarcoma. Ann Surg 2007; 246: 105-113.
- 17. Krieg AH, Hefti F, Speth BM, et al. Synovial sarcomas usually metastasize after >5 years: a multicenter retrospective analysis with minimum follow-up of 10 years for survivors. Ann Oncol 2011; 22: 458-467.
- 18. Pai S, Chinoy RF, Pradhan SA, et al. Head and neck synovial sarcomas. J Surg Oncol 1993; 54: 82-86.
- 19. Kartha SS, Bumpous JM. Synovial cell sarcoma: diagnosis, treatment, and outcomes. Laryngoscope 2002; 112: 1979-1982.





No relevant disclosures.