Malignant mesothelioma (MM) of the pleura or peritoneum is a universally fatal disease predominantly caused by exposure to asbestos. In Australia, the incidence of MM has increased steadily since the early 1960s, initially affecting workers mining and milling raw asbestos and manufacturing asbestos products (the first wave), and then workers who used asbestos products in industry (the second wave). Over the past 20 years, there has been increasing concern about a third wave — people diagnosed with MM after short-term and/or low-level exposure to asbestos in the home or workplace.1 Home maintenance and renovation involving asbestos-containing building products is one of the activities most frequently associated with this third wave. It is a source of ongoing concern, given the widespread distribution of asbestos-containing products in homes and other buildings in Australian cities and towns.
Two forms of asbestos — serpentine (chrysotile or white asbestos) and amphibole (crocidolite or blue asbestos, and amosite or brown asbestos) — have been mined in and imported into Australia. Chrysotile was the main form of asbestos mined in Australia until crocidolite was mined at Wittenoom in the north of Western Australia, beginning in 1943 and continuing until 1966. More than 60% of the crocidolite produced was used in the manufacturing of asbestos cement products. For many years, Australia also imported both raw asbestos and manufactured asbestos goods. By 1954, Australia was ranked fourth among Western countries (after the United States, the United Kingdom and France) for gross consumption of asbestos cement products. However, on a per capita basis, Australia was top of the list.2
After World War II, asbestos cement products were commonly used as a building material in Australia. Asbestos cement products used in building include fibro sheeting; water, drainage and flue pipes; roofing shingles and guttering. Until the 1960s, 25% of all new homes were clad in asbestos cement.2 The use of asbestos was slowly phased out in the 1970s and 1980s, but it is still found in structures built in the late 1980s. A total ban on the use of any type of asbestos was not introduced in Australia until 2003.
Direct occupational exposure to raw asbestos or asbestos products remains the predominant cause of MM, and the number of cases is not expected to peak until 2020.3 However, with the ban on mining and asbestos use, the number of occupational cases will decrease over the next 20–30 years.3 On the other hand, MM cases as a result of non-occupational exposure to asbestos are increasing, and there is little understanding of when, and at what level, this third wave will peak.
Occupational exposures were the main source of exposure to asbestos for men (82.8%) but not for women (16.6%) (Box 1). There were about 10% of cases (158/1631) with unknown exposure and about 5% (75/1631) with no known exposure.
A total of 195 cases (96 men) were associated with non-occupational exposures. Fifty-eight cases (28 men) were ex-residents of Wittenoom, 87 (55 men) were home renovators and in 50 cases (13 men) their “other non-occupational” exposure included visiting Wittenoom (15 [nine men]); living with an asbestos worker (22 [three men]) and various other residential exposures, such as dusting asbestos louvres or playing (as a child) in sheds used to store asbestos cement products (13 cases [one man]). For men, non-occupational exposure accounted for 6.8% of all cases; for women, it accounted for 44.4% (Box 1).
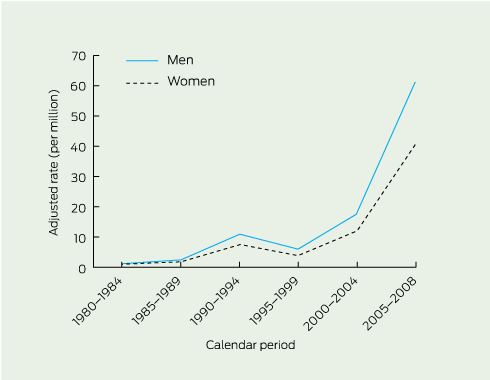
The first case of MM associated with exposure attributed to home maintenance and renovation was registered in 1981. Of the 87 cases recorded, 55 men and 32 women, 84 had pleural MM (53 men) and three peritoneal MM (two men). There has been a steady increase in both the number and incidence rates of home maintenance/renovation cases since the mid 1980s (Box 2). Incidence rates for the last two periods (2000–2004 and 2005–2008) were significantly higher than the base rate (1980–1984) (Box 3, Box 4). For both men and women, home renovators now constitute the largest proportion of all non-occupational cases. Between 2005 and 2008, 8.4% of MM cases in men and 35.7% of those in women were attributed to home renovation.
After controlling for sex and both year and age at diagnosis, the latency period for home renovators was found to be significantly shorter than that for all other groups (Box 5). At diagnosis, home renovators were older than the people in the other two non-occupational groups but slightly younger than those in the two occupational groups (Box 5).
To be included in the home renovator category, people had to have been exposed to asbestos either while performing simple renovations to their homes or, as family members, to have been exposed while these activities took place. The types of reported activities in this category included sanding asbestos cement walls in preparation for painting; lifting linoleum floors; replacing “tilux” (asbestos cement used in place of ceramic tiles) in bathrooms; and using asbestos cement sheeting for putting up fences and sheds, extending laundries, and enclosing verandas to create “sleep-outs”. Some of these activities, particularly those involving the use of power tools, can produce short-term, high concentrations of asbestos fibres,4 and major renovation works may increase background fibre concentrations in the medium term, contributing to increased cumulative exposure.4 In most instances in this series, exposure was limited to a single task, which may have lasted for only a few days.
Based on reported first exposures, the home renovator group had the shortest estimated latency period. Latency periods have mostly been observed to be shorter in groups with occupational rather than non-occupational exposure.5-7 There are two reasons which may explain why we found a shorter latency period for MM cases with home renovation exposure.
First, there has been a shorter follow-up period of this group. Exposure in the home renovator group started in the 1960s, while exposure for the occupational groups commenced in the mid 1940s and early 1950s. As time from exposure increases so, necessarily, does the average latency period.
Second, recalling when exposure first occurred is difficult, particularly for non-occupational exposures. This is likely to be reflected in the greater proportion of women, compared with men, who could not recall any asbestos exposure (“no known” exposure) (Box 1). This difficulty in recalling non-occupational exposures means that some patients may have been exposed to asbestos before the recorded renovation episode and therefore their latency period has been underestimated.
With the wide use of asbestos products in Australian homes after World War II,2 the exact number of homes containing asbestos cement or other asbestos products is not known accurately. In one survey, 62.9% of homes in the Australian Capital Territory were found to contain asbestos.8 It was more common in older homes, with over 70% of homes built before 1965 containing asbestos, but was found in fewer than 1% of homes built after 1984.8 A recent survey of Australian adults found that over 80% of respondents reported exposure to asbestos either at work or at home.9
Home renovation is a common activity in Australia.10,11 In a survey of home owners in Adelaide, major renovations were undertaken in about 34% of homes over a 5-year period (1986–1991).11 Renovations were more common in older homes, particularly those over 50 years old.11 In the 10-year period to 1999, 66% of homes across Australia, built between 1920 and 1949, had been renovated.10 In the Australian survey on potential asbestos exposure mentioned above, only about a third of respondents reported taking precautions to reduce exposure to asbestos fibres or dust in their homes.9 Although a Code of Practice for the safe removal of asbestos has been published,12 advice contained in the code is directed to owners of large buildings and asbestos removalists and not to small operators, individual tradesmen or home renovators.13
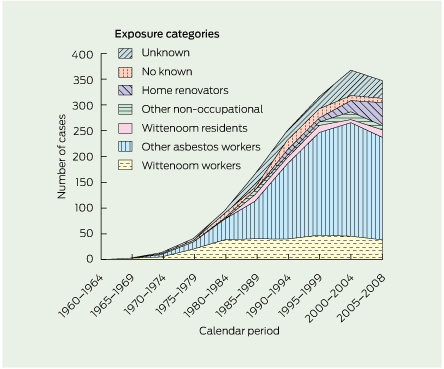
2 Malignant mesothelioma in Western Australia, by exposure category and calendar period, 1960–1964 to 2005–2008
3 Age-adjusted increase in relative incidence rates of malignant mesothelioma attributed to asbestos exposure during home renovation — Western Australia
4 Relative change, 1980–1984 to 2005–2008, in incidence rates of malignant mesothelioma attributed to asbestos exposure during home renovation (adjusted for age and sex) — Western Australia
Received 7 February 2011, accepted 11 July 2011
- Nola J Olsen1
- Peter J Franklin1
- Alison Reid1
- Nicholas H de Klerk1
- Timothy J Threlfall2
- Keith Shilkin1
- Bill Musk3
- 1 University of Western Australia, Perth, WA.
- 2 Western Australian Cancer Registry, Department of Health Western Australia, Perth, WA.
- 3 Sir Charles Gairdner Hospital, Perth, WA.
No relevant disclosures.
- 1. Landrigan PJ. The third wave of asbestos disease: exposure to asbestos in place. Public health control. Introduction. Ann N Y Acad Sci 1991; 643: xv-xvi.
- 2. National Occupational Health and Safety Commission. The incidence of mesothelioma in Australia 1999 to 2001, Australian Mesothelioma Register Report 2004. 16th report. Canberra: NOHSC, 2004. http://safeworkaustralia.gov.au/AboutSafeWorkAustralia/WhatWeDo/Publications/Documents/47/Australian_Mesothelioma_Register_Report_2004_Archived_PDF.pdf (accessed Jul 2011).
- 3. Leigh J, Davidson P, Hendrie L, Berry D. Malignant mesothelioma in Australia, 1945-2000. Am J Ind Med 2002; 41: 188-201.
- 4. Brown SK. Asbestos. In: Spengler JD, Samet JM, McCarthy JF, editors. Indoor air quality handbook. New York: McGraw-Hill Professional, 2001: 38.1-38.17.
- 5. Bianchi C, Giarelli L, Grandi G, et al. Latency periods in asbestos-related mesothelioma of the pleura. Eur J Cancer Prev 1997; 6: 162-166.
- 6. Marinaccio A, Binazzi A, Cauzillo G, et al. Analysis of latency time and its determinants in asbestos related malignant mesothelioma cases of the Italian register. Eur J Cancer 2007; 43: 2722-2728.
- 7. Reid A, Heyworth J, de Klerk NH, Musk B. Cancer incidence among women and girls environmentally and occupationally exposed to blue asbestos at Wittenoom, Western Australia. Int J Cancer 2008; 122: 2337-2344.
- 8. Howell M. ACT asbestos surveys - health risk assessment. Final report. ACT Asbestos Taskforce. Canberra: URS Pty Ltd, 2005. http://www.asbestos.act.gov.au/resources/pdfs/Asbestos_Health_Risk_08_05.pdf (accessed Jul 2011).
- 9. Howat P, Jalleh G, Lin C, et al. Residential exposure to asbestos: implications for public health. Proceedings of the 39th Annual Conference of the Public Health Association of Australia; 2009; Sep 28-30; Canberra. ISBN 978-1-8-75990-28-3.
- 10. Australian Bureau of Statistics. Australian social trends 2002. Canberra: ABS, 2002. (ABS Cat. No. 4102.0.)
- 11. Baum S, Hassan R. Home owners, home renovation and residential mobility. J Sociol 1999; 35: 23-41.
- 12. National Occupational Health and Safety Commission. Code of practice for the safe removal of asbestos. 2nd ed. Canberra: NOHSC, 2005. http://safeworkaustralia.gov.au/AboutSafeWorkAustralia/WhatWeDo/Publications/Documents/234/SafeRemoval%20ofAsbestos2ndEditionNOHSC2002_2005.pdf (accessed Jul 2011).
- 13. Bromwich D. The 2005 Australian Asbestos Codes of Practice: an occupational hygiene perspective. Occup Health Saf Aust NZ 2006; 22: 463-470.





Abstract
Objective: To determine trends in incidence of malignant mesothelioma (MM) caused by exposure to asbestos during home maintenance and renovation.
Design, setting and participants: Using the Western Australian Mesothelioma Register, we reviewed all cases of MM diagnosed in WA from 1960 to the end of 2008, and determined the primary source of exposure to asbestos. Categories of exposure were collapsed into seven groups: asbestos miners and millers from Wittenoom; all other asbestos workers; residents from Wittenoom; home maintenance/renovators; other people exposed but not through their occupation; and people with unknown asbestos exposure; or no known asbestos exposure. Latency periods and age at diagnosis for each group were calculated and compared.
Results: In WA, 1631 people (1408 men, 223 women) were diagnosed with MM between 1960 and 2008. Since 1981, there have been 87 cases (55 in men) of MM attributed to asbestos exposure during home maintenance and renovation, and an increasing trend in such cases, in both men and women. In the last 4 years of the study (2005–2008), home renovators accounted for 8.4% of all men and 35.7% of all women diagnosed with MM. After controlling for sex and both year and age at diagnosis, the latency period for people exposed to asbestos during home renovation was significantly shorter than that for all other exposure groups, but the shorter follow-up and difficulty recalling when exposure first occurred in this group may partly explain this.
Conclusions: MM after exposure to asbestos during home renovation is an increasing problem in WA, and these cases seem to have a shorter latency period than other types of exposure. MM cases related to renovation will probably continue to increase because of the many homes that have contained, and still contain, asbestos building products.