There is increasing recognition of the impact of common disorders such as depression and misuse of alcohol and other drugs (AOD) on illness-related burden and health care costs.1 Comorbidity is the rule rather than the exception, with up to 89% of people with AOD use disorders also experiencing depression.2
Abbreviations
AOD |
Alcohol and other drugs |
ANOVA |
Analysis of variance |
BDI-II |
Beck Depression Inventory II |
CAC |
Clinician-assisted computer |
CBT |
Cognitive behaviour therapy |
MI |
Motivational interviewing |
OTI |
Opiate Treatment Index |
PCT |
Person-centred therapy |
Available evidence-based treatment manuals focus on treatment for single problems rather than comorbid conditions.3 Moreover, despite the availability of effective treatments for depression and AOD-related disorders, there is a substantial gap between treatment need and accessibility.4 As the treatments are often high-intensity and require specialist training, they are only accessible to a minority of people in need.5 The presence of comorbid disorders compounds difficulties in treatment access and provision.6
Computer-based treatments may improve access to and acceptability of treatments for these common mental health problems.7-9 Computers allow widespread dissemination of highly specialised evidence-based treatments in a cost-effective and timely manner8 across primary care, mental health services and AOD clinical settings.
We have previously reported on the first randomised controlled trial of computer-based psychological treatment for people with depression and comorbid AOD use.10 Compared with a single-session control condition, therapist- and computer-delivered treatments produced superior outcomes at 12-month follow-up. Interestingly, computer-based treatment delivered significantly better overall substance use outcomes than the other treatments.10
The study reported here represents a large-scale replication of our original trial, involving participants from rural and urban New South Wales and employing a control condition that matched for therapist contact across the 10-session intervention. It was hypothesised that participants would report reductions in depression, alcohol and cannabis misuse at 3-month follow-up, and that improvement would be greater in the treatment groups than the control group.
Our study was conducted between January 2005 and August 2007.
The primary outcome variables in our study were depression, use of alcohol and use of cannabis.
Depression. Participants were regarded as being depressed if they had a Beck Depression Inventory II (BDI-II) score11 of ≥ 17.
Harmful use of alcohol. Harmful use of alcohol was defined as use in excess of recommended national guidelines in Australia at the time of the study,12 which equated to an average consumption of more than four standard drinks per day for men, or two per day for women during the previous month. One standard drink was defined as containing 10 g ethanol (equivalent to 12.5 mL pure alcohol). These guidelines have since been revised to two 10 g ethanol drinks per day for both men and women.12
Harmful use of cannabis. Harmful use of cannabis was defined as an Opiate Treatment Index (OTI) quotient (Q) score13 for cannabis of over 0.14, equating to average use in excess of once weekly during the month prior to baseline.
Primacy. For each participant, we attempted to establish “primacy”, or the temporal relationship between the person’s substance use (alcohol or cannabis) and his or her depression. If substance use problems preceded depressive symptoms for the person’s current episode, we diagnosed the person as having a primary substance use problem (a substance-induced depressive disorder). Conversely, if the person’s depressive symptoms preceded problems with alcohol or cannabis, a primary (or independent) depressive disorder was diagnosed. If we could not determine a primary condition, the person received an “unable to be determined” diagnosis. It was important to establish primacy, as there is some evidence that an independent depressive disorder will require different treatment planning from a substance-induced depressive disorder — the latter usually leading to treatment of the substance use problem first, with the assumption that doing so will resolve the depressive symptoms. In the context of the current trial, primacy was a potential confounding factor in examining treatment response.
Eligibility criteria for the study were a BDI-II score11 of ≥ 17 and concurrent use of alcohol or cannabis at harmful levels in the month before baseline. Participants were excluded if they (i) were using alcohol or cannabis below harmful thresholds; (ii) were under 16 years of age; (iii) had a psychotic disorder; (iv) were not fluent in English; or (v) reported a history of traumatic brain injury.
The most common referral pathway for recruitment to our study was self-referral (n = 125 [46%]) in response to advertisements promoting the study. Other referrals came from public AOD outpatient treatment facilities (n = 84 [31%]), general practices (n = 22 [8%]), non-government support agencies (n = 21 [8%]), government-funded employment services (n = 12 [4%]) and public mental health outpatient clinics (n = 10 [4%]).
Demographic information was collected using the Diagnostic Interview for Psychosis.14 The following specific assessments were also made at baseline and 3 months.
The BDI-II11 is a 21-item self-report questionnaire used to screen for the presence of depressive symptoms over the previous 2-week period.15 The maximum possible score is 63 points.
The OTI Q score13 is a self-report measure of the quantity and frequency of use of 11 substances. The score represents the average number of use occasions in the month before interview. A score of 1 equates to once daily use, a score of 0.14 to once weekly use.
The SCID-IV-RV16 provides diagnostic, clinician-rated measures of major depressive disorder, alcohol misuse/dependence and cannabis misuse/dependence, based on criteria set out in the Diagnostic and statistical manual of the mental disorders, 4th edition (DSM-IV).17 For the purposes of our study, the SCID diagnosis was dichotomised into two separate variables, indicative of misuse/no misuse and dependence/no dependence for alcohol and cannabis use.
After initial screening to determine eligibility, participants completed a baseline assessment at one of seven study clinics located in rural and urban NSW. Classification of sites as urban or rural18 was done on the basis of participant postcode, but generally urban participants were drawn from Newcastle and Gosford, and rural participants from Cessnock, Wyong, Orange, Cowra and Bathurst.
All participants received one face-to-face session with a therapist and were then randomly allocated to receive:
Nine weekly, 60-minute sessions of integrated cognitive behaviour therapy and motivational interviewing (CBT/MI) delivered by a therapist (n = 87); or
Nine weekly, 60-minute sessions of clinician-assisted computerised (CAC) therapy, consisting of integrated CBT/MI delivered by a computer with minimal therapist assistance) (n = 97); or
Nine weekly, 60-minute sessions of person-centred therapy (PCT), consisting of supportive counselling delivered by a therapist (n = 88) (the control group).
Participants and assessors were blind to allocation until after the first session.
Participants were asked whether they had a preference for any treatment arm (yes/no), and a variable was created based on whether or not this preference matched their treatment allocation (yes/no/no preference).
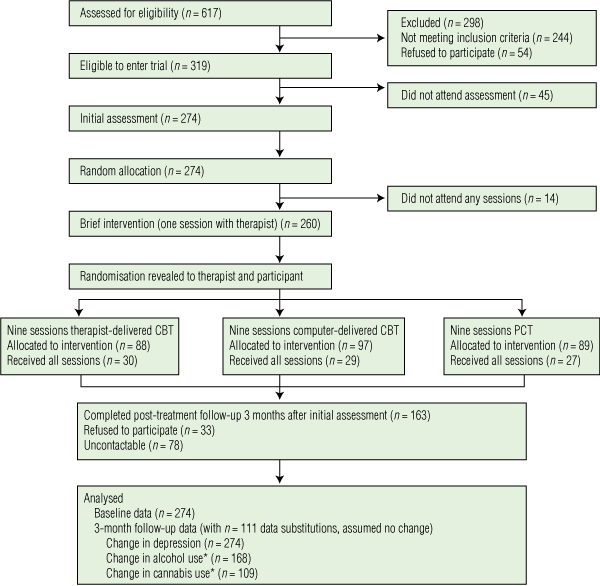
All participants were eligible to receive a follow-up assessment, regardless of treatment attendance, at 3 months after baseline. Participants received $20 reimbursement for each assessment (at baseline and 3 months), but not for treatment. Follow-up assessments were completed by trained research officers, independent of baseline measurements and treatments, who were blind to treatment allocation. The flow of participants through the study is shown in Box 1.
All treatments were structured and delivered according to a treatment manual designed specifically for the treatments associated with the study. All sessions were recorded on audiotape, and a random 25% sample from each session of each treatment condition was selected for fidelity analysis by an independent rater. Each session was conducted individually, with session 1 comprising assessment feedback, commencement of MI, psychoeducation (information about the signs, symptoms and impact of depression, alcohol and cannabis use), and initial goal setting.
Therapist-delivered integrated CBT/MI10 comprised nine 60-minute sessions of CBT, with MI employed thematically throughout treatment. The treatment sessions integrated depressive and AOD-related strategies, making explicit the links between conditions.
CAC therapy was identical in content to therapist-delivered integrated CBT/MI, but was delivered via a computer program with minimal therapist input. Therapist input10 was a brief, structured, 10-minute check-in session at the conclusion of each session.
PCT, consisting of therapist-delivered supportive counselling, was adapted from an unpublished manual by Sellman JD, Sullivan PF and Dore GM entitled “Brief treatment programme for alcohol dependence: person-centred therapy therapist’s manual” (Christchurch School of Medicine, New Zealand). It was delivered over nine 60-minute weekly sessions and was included to control for therapist (live) contact, but not for therapy content.
Treating therapists were intern, registered or clinical psychologists, who received weekly clinical supervision from us. This included review of selected audio-recorded sessions and allowed any issues about delivery of the interventions to be raised. All therapists delivered treatments in all three treatment arms.
Participants in our study were 274 people with a mean BDI-II score of 32 (range, 17–59) and current harmful use of alcohol (n = 168) and/or cannabis (n = 109).
The mean age was 40 years (range, 17–70 years), and 57% of participants were men. Participants had left school at a mean age of 16 years (range, 12–19 years), with 42 (15%) gaining tertiary qualifications and 121 (44%) gaining trade and technical qualifications. At baseline, 159 (58%) were unemployed and receiving a disability benefit (n = 56), unemployment benefit (n = 65) or other benefit (n = 38). No differences were detected between treatment groups in these characteristics.
Forty-one per cent of the sample was rural (3% remote, 6% outer regional, 33% inner regional).18 A significantly higher proportion of rural-based than urban-based participants were referred to the study from general practice clinics (23% v 2%; χ24 = 37.609; P < 0.001).
About a third of participants (107 [39%]) reported receiving treatment for AOD use and depression in the previous 12 months — most commonly medication (57% of those receiving treatment). Participants had visited a general practitioner an average of eight times in the previous 12 months, but 69 (25%) had made only one or two visits, and 29 (11%) no visits.
Almost half the participants (133 [49%]) expressed a preference for therapist-delivered treatment and 13 (5%) for CAC treatment, with the remaining 128 (47%) having no preference. Ninety-two participants (34%) who indicated a preference for treatment were allocated to their preferred treatment modality.
Of the 168 participants (61%) who met criteria for harmful use of alcohol at baseline, 88 (52%) were men. Participants in this group reported consuming an average of 11 standard drinks per day in the month before assessment (mean OTI Q score, 11.30 [SD, 7.55]; range, 2.00–68.00).
One hundred and nine participants (40%) met criteria for harmful cannabis use at baseline, of whom 71 (65%) were men. The reported average use was 12 times per day in the month before baseline (mean OTI Q score, 11.92 [SD, 16.82]; range, 0.14–100.00). Sixty-nine participants (25%) met criteria for harmful use of both alcohol and cannabis at baseline, 139 (51%) for alcohol use only and 66 (24%) for cannabis use only.
In considering the relationship between current depression and AOD use, and using SCID criteria, 32% of participants were rated by clinicians as having a primary depressive disorder and 6% as having substance-induced depression. For the remaining 62%, primacy of depression over AOD disorders could not be established because both conditions always occurred together, with very few (if any) periods of abstinence.
The degree of therapists’ adherence to treatment protocols is discussed in Box 2.
Participants attended a mean of 5.6 (SD, 3.9) sessions, with no significant differences between treatment groups in level of attendance (mean, 6.1 [therapist CBT/MI] v 5.3 [CAC] v 5.4 [PCT]; F2,223 = 1.046; P = 0.353).
Participants receiving CBT/MI (therapist- or computer-delivered) had significantly reduced levels of depression at 3-month follow-up (based on mean reduction in BDI-II score) compared with those receiving PCT (6.87-point v 3.84-point reduction; F1,273 = 5.164; P = 0.024), but there were no significant differences between computer- and therapist-delivered approaches in reducing depression. Change in depression was not associated with sex (F1,266 = 1.1073; P = 0.301), age (r = 0.001, P = 0.987) or rurality (F1,273 = 0.000; P = 0.997).
Participants without a particular preference for treatment at baseline reported significantly less change in depression than those who nominated a treatment preference, regardless of whether this matched their allocation (F1,273 = 4.142; P = 0.017).
Participants for whom primacy of depression over AOD use disorders could not be established reported significantly less change in depression than people who had either a substance-induced or independent depressive condition (F1,273 = 5.913; P = 0.003).
There was a positive correlation between change in depression and change in alcohol use (r = 0.344; P < 0.001), but no association between change in depression and change in cannabis use (r = 0.083, P = 0.179).
The proportions of participants meeting a range of threshold criteria for depression at 3 months are shown in Box 3. There was a non-significant trend towards fewer CAC therapy recipients reporting above-baseline-threshold depression at 3 months than therapist-delivered treatment recipients (χ21 = 3.587, P = 0.058).
Change in alcohol use was significantly related to treatment allocation, with CBT/MI therapy associated with four times the reduction in alcohol consumption compared with PCT (mean reduction in drinks/day, 4.88 [CBT/MI] v 1.03 [PCT]; F1,167 = 8.333; P = 0.004). Participants receiving CAC therapy reported a 2.5 times greater reduction in alcohol use than those who received therapist-delivered treatment (mean reduction in drinks/day, 6.11 [CAC group] v 2.40 [therapist group]; F1,167 = 7.875; P = 0.006).
Change in alcohol use was positively correlated with change in depression (r = 0.405; P < 0.001) and change in cannabis use (r = 0.238; P = 0.002). There was no significant association between change in alcohol use and sex (F1,167 = 0.837, P = 0.362), age (r = – 0.027; P = 0.732), rurality (F1,167 = 0.898; P = 0.345), primacy of alcohol use over depression (F1,167 = 0.332; P = 0.718), or treatment preference (F1,167 =1.346; P = 0.263).
A significantly higher proportion of CBT/MI than PCT recipients achieved at least a 50% reduction in alcohol use relative to baseline (χ21 = 9.947; P = 0.028) (Box 3). Participants receiving CAC therapy were also significantly more likely than those receiving therapist-delivered treatment to reduce their alcohol consumption by at least 50% relative to baseline (χ21 = 4.835; P = 0.002). There was a non-significant trend towards more CAC therapy recipients reporting abstinence from alcohol than therapist-delivered treatment recipients (χ21 = 3.635; P = 0.057).
Change in cannabis use was not significantly associated with participating in CBT/MI (F1,108 = 2.214, P = 0.140), despite there being a 3-point reduction in OTI Q score for CBT/MI groups and the PCT group reporting a small increase in use (0.15 points). Although the reported reduction in cannabis use among CAC therapy participants was twice that among participants receiving therapist-delivered treatment (a 2.7-point v 1.1-point fall in OTI Q score), the difference was not statistically significant (F1,108 = 0.893; P = 0.347).
Change in cannabis use was not significantly associated with sex (F1,108 = 1.656; P = 0.201), age (r = – 0.042; P = 0.663), rurality (F1,109 = 0.090; P = 0.765), primacy of cannabis use over depression (F1,108 = 0.272; P = 0.762), or treatment preference (F1,108 = 0.058; P = 0.943).
Change in cannabis use was significantly correlated with change in alcohol use (r = 0.396; P < 0.001), but not with change in depression (r = 0.182; P = 0.059).
There was no significant relationship between treatment allocation and rates of abstinence, rates of 50% reduction in cannabis use and the proportion of participants continuing to use cannabis above a harmful threshold at 3-month follow-up (Box 3).
The combination of sex, age, rurality, treatment preference (CBT/MI v PCT; CAC- v therapist-delivered therapy), primacy, treatment allocation, change in alcohol use and change in cannabis use significantly predicted change in depression (F8,249 = 5.419; P < 0.001) (Box 4). Independent predictors in this model were primacy of AOD/depressive disorders (with failure to determine primacy associated with less change), and change in alcohol use over the same time period, with a non-significant trend towards CBT/MI treatment predicting greater change than PCT (P = 0.064). The model accounted for about 17% of the variance in depression (Box 4).
A second linear regression used to predict change in alcohol use was significant (F8,167 = 6.100; P < 0.001), indicating that change in depression and change in cannabis use were each independent predictors of change in alcohol use between baseline and 3 months (Box 4). This model accounted for 26% of the variance in alcohol use.
A third linear regression used to predict change in cannabis use, with the same set of predictors as the previous regression models, was also significant (F8,108 = 3.012; P = 0.003). The only independent predictor of change in cannabis use was change in alcohol use. This model accounted for 22% of variance in cannabis use (Box 4).
Our study is the largest to report on the use of CAC therapy in a group reporting severe levels of depression at initial assessment and concurrent heavy use of alcohol or cannabis. It adds to the emerging literature supporting the use of integrated CBT/MI for people with depression and comorbid AOD misuse.19 Participants achieved simultaneous improvement in mental health and reduction in AOD symptoms, with change in depression, alcohol use and cannabis use independently predicting change in each other, after accounting for presenting symptoms, treatment allocation and demographic background. This is in line with expert advice that concurrent treatment does not jeopardise treatment outcomes for either the mental health or AOD use condition,20 and that integrating depression and AOD-focused CBT/MI into the same intervention enhances improvement in both conditions over a single-focused treatment.19
Thus, practitioners working with people who have a mental health problem and comorbid harmful drug use should feel confident in encouraging their clients to consider multiple simultaneous targets for treatment within a CBT/MI framework. Therapist-delivered and CAC CBT/MI treatments resulted in similar patterns of positive change across depressive and AOD domains, indicating the two different modes of providing integrated treatment for depression and comorbid AOD use perform similarly well. As PCT was associated with significantly less reduction in depression and alcohol consumption compared with CBT/MI, PCT is not recommended for the treatment of these comorbid conditions.
CAC therapy may be a particularly important treatment consideration for people with comorbid alcohol misuse and depression, given the evidence for an enhanced treatment response for both depressive and alcohol use outcomes associated with the computerised treatment modality.
The promising results for CAC therapy are particularly important, considering that, after the initial face-to-face session, it required, on average, only 16 minutes per session of clinician time — less than half that required for therapist-delivered CBT/MI treatment (57 min/session) or PCT (41 min/session). In our study, check-in sessions at the end of CAC sessions were conducted by a qualified psychologist, but the content was generic in nature. Arguably, many health professionals or primary care workers (eg, nurse practitioners working in primary care settings) with minimal specific training in mental health, substance misuse or comorbidity could provide this support, potentially also using phone-based delivery. This is in contrast to the highly specialised therapist-delivered CBT/MI, which may need appreciably more training and support before and during dissemination. This makes CAC potentially more cost- and time-effective than face-to-face treatment, with no evidence of reduced efficacy using this approach.
Rurality, age, sex and treatment preference for therapist-delivered approaches were not associated with treatment response in our study, indicating the potentially broad appeal of CAC therapy across various demographic groups in the community.
Our results are based on short-term responses to treatment for depression and comorbid AOD misuse. Longer term follow-up is required to substantiate our study findings.21
In substituting data for participants who did not complete the 3-month follow-up assessment, we assumed no change, when in fact their depression or alcohol or cannabis use may have deteriorated. This may have inflated the improvement observed in these primary outcomes. Compared with participants who completed the 3-month follow-up assessment, non-completers were not systematically different with respect to baseline depression, alcohol or cannabis use, or patterns of treatment allocation.
Notwithstanding these limitations, the results of our study show promise for the benefits of integrated CBT/MI treatment for depression and comorbid AOD misuse, particularly using the computerised modality of delivery, and this is worthy of further exploration.
1 Flow of participants through the study
 | |||||||||||||||
|
CBT = cognitive behaviour therapy. PCT = person-centred therapy. * Includes only participants who were using above the threshold for hazardous use of this substance at baseline. | |||||||||||||||
2 Therapists’ adherence to treatment protocols
Session 1
Session 1 was common to all treatments. The maximum allocated time for the session was 60 minutes. The average duration of session 1 was 64 minutes (range, 22–169 minutes), and clinicians were rated as adherent in 85% of cases. Clinicians were rated as non-adherent for reasons such as technical difficulties (eg, the audio recording being partly inaudible [80% of non-adherent cases]), or because the client was in crisis and the session agenda was suspended in favour of addressing the crisis issues (20% of non-adherent cases). Crisis sessions all exceeded the 60-minute session limit and were the longest in duration (range, 99–169 minutes).
Therapist-delivered integrated CBT/MI
The maximum allocated time for each therapist-delivered integrated CBT/MI session was 60 minutes. Across sessions 2–10, clinicians providing this treatment were rated as adherent in 56% of instances (range, 35%–78%). The average session duration was 57 minutes (range, 16–102 minutes). Reasons for non-adherence included technical difficulties, such as the audio recording being partly inaudible (68% of non-adherent cases); suspension of the session because of the client being in crisis (16% of non-adherent cases) (crisis relating to a major life event [25%], high suicidal ideation [50%], or severe alcohol or other drug relapse [25%]); and exceeding the 60-minute session time limit for non-crisis reasons (16% of non-adherent cases). Sessions 4, 7 and 8 had the lowest adherence ratings (35%, 40%, 36%, respectively), most often because of technical difficulties (62% of cases) or because the client was suicidal or undergoing a life crisis (15% of cases). These particular sessions tended to involve a shift from behavioural approaches to cognitive approaches, such as schema-focused therapy (sessions 7 and 8), and a shift from phase 1 motivational approaches towards phase 2 approaches, with a concomitant move from negotiating change to setting plans for change and action-oriented strategies (sessions 4 and 8).
Clinician-assisted computer (CAC) check-in sessions
In the CAC sessions, clinicians checked in with each participant for a maximum of 10 minutes at the conclusion of each computer session. The average check-in session lasted 16 minutes (range, 4–61 minutes). Clinicians were judged as adherent in 39% of cases. Reasons for non-adherence included technical difficulties, such as the audio recording being partly inaudible (23% of non-adherent cases); the client being in crisis (19% of non-adherent cases) (crisis relating to a major life event [67%] or severe relapse to depression [33%]); and exceeding the 10-minute session time limit for non-crisis reasons (58% of non-adherent cases). Crisis sessions were the longest in duration (range, 34–61 minutes), and these occurred most often after session 2, which was the first computerised session (83% of cases), or session 4, when plans for change and action were discussed (17% of cases). Sessions 2–4 required longer check-in sessions, on average, than the other sessions (20 minutes v 15 minutes).
Person-centred therapy (PCT)
The maximum allocated time for each PCT session was 60 minutes. Session content was identical across sessions 2–10 for this treatment, with adherence items relating to the implementation of PCT strategies and the absence of any CBT/MI strategies. Clinicians were rated as adherent in 73% of cases. The average session duration was 41 minutes (range, 10–74). Reasons for non-adherence included technical difficulties with the audio recording of sessions (92%), and exceeding the 60-minute time limit for non-crisis reasons (8%). Sessions that exceeded the time limit were spread across the treatment period.
CBT = cognitive behaviour therapy. MI = motivational interviewing.
3 Depression, alcohol use and cannabis use at 3-month follow-up, by treatment allocation*
|
CBT/MI† (n = 185) |
PCT (n = 89) |
P |
CAC therapy‡ (n = 97) |
Therapist-delivered treatment§ (n = 177) |
P |
|||||||||
Depression |
|
|
|
|
|
|
|||||||||
Absent (BDI-II score ≤ 10) |
30 (16%) |
9 (10%) |
0.176 |
18 (19%) |
21 (12%) |
0.129 |
|||||||||
At least 50% reduction |
35 (19%) |
13 (15%) |
0.379 |
22 (23%) |
26 (15%) |
0.096 |
|||||||||
Above threshold (BDI-II score ≥ 17) |
137 (74%) |
73 (82%) |
0.144 |
68 (70%) |
142 (80%) |
0.058 |
|||||||||
Alcohol use¶ |
|
|
|
|
|
|
|||||||||
Abstinent |
9 (8%) |
3 (6%) |
0.582 |
7 (13%) |
5 (5%) |
0.057 |
|||||||||
At least 50% reduction |
47 (41%) |
9 (17%) |
0.028 |
25 (45%) |
31 (28%) |
0.002 |
|||||||||
Using above harmful threshold |
38 (33%) |
17 (32%) |
0.811 |
13 (23%) |
42 (38%) |
0.063 |
|||||||||
Cannabis use¶ |
|
|
|
|
|
|
|||||||||
Abstinent |
8 (11%) |
7 (21%) |
0.164 |
4 (10%) |
11 (16%) |
0.309 |
|||||||||
At least 50% reduction |
22 (29%) |
11 (32%) |
0.751 |
14 (33%) |
19 (28%) |
0.582 |
|||||||||
Using above harmful threshold |
34 (45%) |
14 (41%) |
0.685 |
20 (48%) |
28 (42%) |
0.551 |
|||||||||
BDI-II = Beck Depression Inventory II. CAC = clinician-assisted computerised. CBT = cognitive behaviour therapy. MI = motivational interviewing. PCT = person-centred therapy. * Data are n (%) or P values. † Integrated CBT/MI (whether therapist- or computer-delivered). ‡ Integrated CBT/MI (computer-delivered). § Therapist-delivered treatment (integrated CBT/MI or PCT). ¶ Included only those participants who were using above the threshold for harmful use of this substance at baseline. |
|||||||||||||||
4 Linear regression analysis predicting change in depression, alcohol use and cannabis use between baseline and 3-month follow-up
|
β* |
t† |
P |
95% CI for β |
|||||||||||
Change in depression‡ |
|
|
|
|
|||||||||||
(Constant) |
|
1.749 |
0.082 |
– 1.062, 17.895 |
|||||||||||
Rurality |
– 0.024 |
– 0.380 |
0.704 |
– 3.195, 2.162 |
|||||||||||
Sex |
0.006 |
0.102 |
0.919 |
– 0.116, 0.128 |
|||||||||||
Age |
0.081 |
1.367 |
0.173 |
– 0.779, 4.308 |
|||||||||||
Primacy |
– 0.172 |
– 2.862 |
0.005 |
– 0.945, – 0.180 |
|||||||||||
Treatment preference |
0.097 |
11.565 |
0.119 |
– 0.349, 3.049 |
|||||||||||
CBT/MI§ v PCT |
– 0.129 |
– 1.857 |
0.064 |
– 6.125, 0.180 |
|||||||||||
CAC¶ v therapist-delivered treatment** |
0.070 |
– 0.966 |
0.335 |
– 1.621, 4.739 |
|||||||||||
Change in cannabis use |
0.002 |
0.040 |
0.968 |
– 0.208, 0.216 |
|||||||||||
Change in alcohol use |
0.319 |
5.210 |
0.000 |
0.289, 0.641 |
|||||||||||
Change in alcohol use‡ †† |
|
|
|
|
|||||||||||
(Constant) |
|
3.391 |
0.001 |
6.368, 24.131 |
|||||||||||
Rurality |
– 0.095 |
– 1.319 |
0.189 |
– 3.996, – 0.795 |
|||||||||||
Sex |
– 0.038 |
– 0.530 |
0.597 |
– 0.137, 0.079 |
|||||||||||
Age |
– 0.093 |
– 1.306 |
0.194 |
– 3.845, 0.784 |
|||||||||||
Primacy |
– 0.082 |
– 1.169 |
0.244 |
– 3.100, 0.795 |
|||||||||||
Treatment preference |
– 0.004 |
– 0.058 |
0.953 |
– 1.608, 1.515 |
|||||||||||
CBT/MI§ v PCT |
– 0.063 |
– 0.770 |
0.442 |
– 3.981, 1.747 |
|||||||||||
CAC¶ v therapist-delivered treatment** |
– 0.142 |
– 1.744 |
0.083 |
– 5.292, 0.329 |
|||||||||||
Change in depression |
0.352 |
4.930 |
0.000 |
0.158, 0.370 |
|||||||||||
Change in cannabis use |
0.196 |
2.776 |
0.006 |
0.094, 0.555 |
|||||||||||
Change in cannabis use‡ †† |
|
|
|
|
|||||||||||
(Constant) |
|
1.1804 |
0.074 |
– 11.125, 23.623 |
|||||||||||
Rurality |
0.011 |
0.113 |
0.910 |
– 3.172, 3.556 |
|||||||||||
Sex |
– 0.057 |
– 0.600 |
0.550 |
– 0.257, 0.137 |
|||||||||||
Age |
– 0.125 |
– 1.369 |
0.174 |
– 5.602, 1.028 |
|||||||||||
Primacy |
– 0.118 |
– 1.215 |
0.227 |
– 4.195, 1.008 |
|||||||||||
Treatment preference |
0.018 |
0.185 |
0.854 |
– 1.936, 2.334 |
|||||||||||
CBT/MI§ v PCT |
– 0.148 |
– 1.349 |
0.180 |
– 6.901, 1.314 |
|||||||||||
CAC¶ v therapist-delivered treatment** |
– 0.009 |
– 0.081 |
0.935 |
– 4.158, 3.831 |
|||||||||||
Change in depression |
0.107 |
1.135 |
0.259 |
– 0.070, 0.257 |
|||||||||||
Change in alcohol |
0.374 |
4.040 |
0.000 |
0.230, 0.675 |
|||||||||||
ANOVA = analysis of variance. CAC = clinician-assisted computerised. CBT = cognitive behaviour therapy. MI = motivational interviewing. PCT = person-centred therapy. * Standardised regression coefficient. †t statistic for β. ‡ ANOVA results: change in depression (F8,249 = 5.419, P < 0.001, ΔR2 = 0.169); change in alcohol use (F8,167 = 6.100, P < 0.001, ΔR2 = 0.258); change in cannabis use (F8,108 = 3.012, P = 0.003, ΔR2=0.215). § Integrated CBT/MI (therapist- or computer-delivered). ¶ Integrated CBT/MI (computer-delivered). ** Therapist-delivered treatment (integrated CBT/MI or PCT). †† Included only those participants who were using above the threshold for harmful use of this substance at baseline. |
|||||||||||||||
- Frances J Kay-Lambkin1,2
- Amanda L Baker2
- Brian Kelly2
- Terry J Lewin2
- 1 National Drug and Alcohol Research Centre, University of New South Wales, Sydney, NSW.
- 2 Centre for Brain and Mental Health Research, University of Newcastle, Newcastle, NSW.
Our research was supported in full by a grant from the Alcohol Education and Rehabilitation Foundation. The conduct and analysis of the study were independent of the funding body. Our study was carried out in accordance with the National Health and Medical Research Council’s National statement on ethical conduct in human research.
Brian Kelly is member of the board of the Centre for Rural and Remote Mental Health Queensland. He has received consultancy fees from the Sax Institute and the Australian Primary Health Care Research Institute.
- 1. World Health Organization. The global burden of disease: 2004 update. Geneva: WHO, 2008.
- 2. Helmus TC, Downey KK, Wang LM, et al. The relationship between self-reported cocaine withdrawal symptoms and history of depression. Addict Behav 2001; 26: 461-467.
- 3. Kay-Lambkin FJ, Baker A, Lewin T. The “co-morbidity roundabout”: a framework to guide assessment and intervention strategies and engineer change among people with co-morbid problems. Drug Alcohol Rev 2004; 23: 407-424.
- 4. Australian Bureau of Statistics. National Survey of Mental Health and Wellbeing: summary of results, 2007. Canberra: ABS, 2008. (ABS Cat. No. 4326.0.)
- 5. Brown CH, Ten-Have TR, Jo B, et al. Adaptive designs for randomized trials in public health. Annu Rev Public Health 2009; 30: 1-25.
- 6. Kavanagh DJ, Mueser K, Baker A. Management of co-morbidity. In: Teesson M, editor. Co-morbid mental disorders and substance use disorders: epidemiology, prevention and treatment. Canberra: Commonwealth of Australia, 2003: 78-107.
- 7. Kaltenthaler E, Parry G, Beverley C, Ferriter M. Computerised cognitive-behavioural therapy for depression: systematic review. Br J Psychiatry 2008; 193: 181-184.
- 8. Bewick BM, Trusler K, Barkham M, et al. The effectiveness of web-based interventions designed to decrease alcohol consumption — a systematic review. Prev Med 2008; 47: 17-26.
- 9. Cuijpers P, van Straten A, Andersson G. Internet-administered cognitive behavior therapy for health problems: a systematic review. J Behav Med 2008; 31: 169-177.
- 10. Kay-Lambkin FJ, Baker A, Lewin T, Carr VJ. Computer-based psychological treatment for comorbid depression and problematic alcohol and/or cannabis use: a randomized controlled trial of clinical efficacy. Addiction 2009; 104: 378-388.
- 11. Beck AT, Steer RA, Brown GK. Manual for the Beck Depression Inventory-II. San Antonio, Tex: Psychological Corporation, 1996.
- 12. National Health and Medical Research Council. Australian guidelines to reduce health risks from drinking alcohol. Canberra: NHMRC, 2009. http://www.nhmrc.gov.au/publications/synopses/ds10syn.htm (accessed Jun 2011).
- 13. Darke S, Heather N, Hall W, et al. Estimating drug consumption in opioid users: reliability and validity of a “recent use” episodes method. Br J Addict 1991; 86: 1311-1316.
- 14. Castle DJ, Jablensky A, McGrath JJ, et al. The diagnostic interview for psychoses (DIP): development, reliability and applications. Psychol Med 2006; 36: 69-80.
- 15. Dawe S, Loxton N, Hides L, et al. Review of diagnostic and screening instruments for alcohol and other drug use and other psychiatric disorders. 2nd ed. Canberra: Commonwealth of Australia, 2002.
- 16. First MB, Spitzer RL, Gibbon M, Williams JB. Structured Clinical Interview for DSM-IV-TR axis I disorders, research version, patient edition. New York: Biometrics Research, New York State Psychiatric Institute, 2001.
- 17. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Text revision. Washington, DC: APA, 2000.
- 18. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remoteness classifications. Canberra: AIHW, 2004. (AIHW Cat. No. PHE 53.)
- 19. Baker AL, Kavanagh DJ, Kay-Lambkin FJ, et al. Randomized controlled trial of cognitive-behavioural therapy for coexisting depression and alcohol problems: short-term outcome. Addiction 2010; 105: 87-99.
- 20. Kalman D, Kim S, DiGirolamo G, et al. Addressing tobacco use disorder in smokers in early remission from alcohol dependence: the case for integrating smoking cessation services in substance use disorder treatment programs. Clin Psychol Rev 2010; 30: 12-24.
- 21. Hasin DS, Tsai W-Y, Endicott J, et al. Five-year course of major depression: effects of comorbid alcoholism. J Affect Disord 1996; 41: 63-70.





Abstract
Objective: To compare computer-delivered and therapist-delivered treatments for people with depression and comorbid addictive disorders.
Design: Randomised controlled clinical trial.
Setting and participants: Our study was conducted between January 2005 and August 2007 at seven study clinics in rural and urban New South Wales. Participants were 274 people who had a Beck Depression Inventory II (BDI-II) score ≥ 17 and were using alcohol and/or cannabis at harmful levels in the month before baseline. They were self-referred or referred from other sources such as outpatient drug treatment clinics, general practices and non-government support agencies.
Interventions: Participants were randomly allocated to receive (1) integrated cognitive behaviour therapy and motivational interviewing (CBT/MI) delivered by a therapist; (2) integrated CBT/MI delivered by computer, with brief therapist assistance at the end of each session (clinician-assisted computerised [CAC] treatment), or (3) person-centred therapy (PCT), consisting of supportive counselling given by a therapist (the control group). All three treatments were delivered according to a manual developed specifically for the study.
Main outcome measures: Changes in depression, alcohol use and cannabis use at 3 months after baseline; significant predictors of change in the primary outcome variables.
Results: Compared with computer- or therapist-delivered CBT/MI, PCT was associated with significantly less reduction in depression and alcohol consumption at 3 months. CAC therapy was associated with improvement at least equivalent to that achieved by therapist-delivered treatment, with superior results as far as reducing alcohol consumption. Change in depression was significantly predicted by change in alcohol use (in the same direction) and an ability to determine primacy, irrespective of whether this was for drug use or depression. Change in alcohol use was significantly predicted by changes in cannabis use and depression, and change in cannabis use by change in alcohol use. In the regression model, treatment allocation did not independently predict change, but was associated with significant reduction in depression and alcohol use at 3 months.
Conclusions: Over a 3-month period, CBT/MI was associated with a better treatment response than supportive counselling. CAC therapy was associated with greater reduction in alcohol use than therapist-delivered treatment.
Trial registration number: ACTRN12610000274077.