Medical workforce demographics are changing. More women than men are graduating as doctors,1 and a third of the current generation of junior doctors in Australia are in their 30s. This means that more doctors are raising children in their training years,2 and a desire to balance work with domestic commitments is influencing their vocational choices.2 For an increasing number of junior doctors, undertaking full-time training and withdrawing from domestic and other responsibilities may not be feasible, particularly during advanced training. These demographic changes are likely to become more pronounced with the substantial increase in medical graduate numbers in Australia, from about 1200 in 2003 to nearly 3000 in 2012.3 Despite this, permanent flexible training positions across the medical subspecialties are lacking.
A letter to the BMJ in 1978, anticipating the increase in women doctors, said that unless part-time training is accepted as normal, we should “discourage schoolgirls from wanting to be doctors and medical schools from admitting them”.4 Thirty years on, the evolution of core curricula and the diversification of training settings, as well as the marked changes in medical workforce demographics, all stand in clear contrast to the constancy of the full-time nature of advanced physician training.
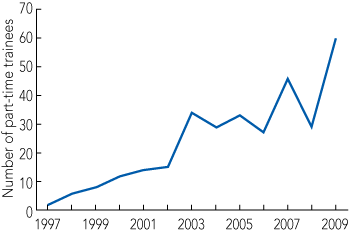
In the most recent list of training positions for the Royal Australasian College of Physicians (RACP),5 only three of 42 adult advanced training positions were expressly advertised as amenable to part-time, job-share or other types of flexibility. There has been no formal quantification of demand for flexible training among physician trainees, but the increasing number of advanced trainees undertaking part-time training (from two in 1997 to 60 in 2009)1 suggests that a demand exists (the relative percentage has remained at around 5% because of the increase in trainees from 443 to 1157 over this period) (Box 1). Currently, nearly three-quarters of part-time trainees are women (Ms E Newton, Education Deanery, RACP, personal communication), and despite comparable proportions of women, there are fewer part-time trainees in adult medicine than in the other specialties (Box 2).
Models that can be adapted for medical training purposes are a full-time flexible model, a part-time flexible model including supernumerary positions (ie, positions created on top of pre-existing positions) and a job-share model (Box 3). Of these, supernumerary positions are most amenable to satisfying both workforce and trainee demands, as they can be designed to increase workforce numbers at times of peak clinical demand, while accommodating trainee commitments. Job-share positions within paediatric training are well established and have a number of distinct advantages (eg, work is allocated on a rotational basis to suit trainees) and disadvantages (eg, coworkers need to adapt to working with two people responsible for the same tasks [Box 3]).
Research on trainee outcomes with these models, although limited, has shown clearly that job sharing results in high levels of satisfaction and enthusiasm, less tiredness and no evidence of compromised continuity of care.6 A study of part-time trainees found that they scored significantly better than their full-time colleagues on humanistic skills.7 However, there is a lack of information specifically on educational outcomes, and it is not known whether a minimum level of training is required to maintain skills, or whether gaining of competencies is affected by breaks in the otherwise immersive training experience. Rigorous educational research is required to close this information gap. Views of the supervising departments and hospital administrations have also not been sought, and prospective research is needed in this area.
Use of alternative training environments can enhance flexibility. There is current interest in developing specialist training positions in non-traditional environments (eg, private hospitals and community clinics), reflecting where most health care is delivered. Concurrent with this, the federally sponsored Specialist Training Program8 provides an opportunity to generate positions that meet both training imperatives and workforce need, but have flexibility as an integral component.
Quantification: A first step to overcoming barriers would be quantification of the demand for flexible training, as a perceived lack of flexible training may suppress demand.9 Furthermore, specialist colleges should increase awareness by making previously successful programs available.
Administrative issues: Trainees wishing to job share may be discouraged by inability to find a suitable partner. An actively promoted job-share register would enable trainees to network with others of similar seniority and geographical location. An administrative contact within specialist colleges could help trainees to devise an appropriate program, similar to a scheme in the United Kingdom where each region has a coordinator for flexible training. Trainees should contribute by registering demand and reporting flexible training difficulties. Medical administrations can assist by promoting their policy on flexible training and, where feasible, committing to offer positions (particularly in the light of new federal legislation supporting employees’ rights to request a flexible work environment).10
Funding: In a tight fiscal environment, funding poses a significant barrier, particularly to supernumerary positions. Funding of full-time flexible models and job-share models can occur through adaptation of pre-existing positions, whereas supernumerary posts require a new source of funding. A model from the UK provides one approach, where supernumerary positions are funded centrally under the Flexible Careers Scheme, developed as part of the Improving Working Lives for Doctors initiative.11 Centralised funding of these positions is justified, given that flexible training is a workforce issue, with research indicating that trainees with family commitments may choose not to work rather than to work full time.12 However, where supernumerary positions are funded from non-governmental sources (eg, “soft” money, research grants, benevolent funds), these should still be accredited as advanced training posts if they fulfil the criteria set by the specialist college and involve no conflict of interest.
Provenance: Not commissioned; externally peer reviewed.
- Suzanne E Mahady1
- Storr Liver Unit, Westmead Hospital, Sydney, NSW.
Thanks to Libby Newton and the RACP for providing additional data on part-time training. This work was supported in part by the Storr Liver Unit, University of Sydney, Sydney, NSW. However, it represents my own opinions and not those of my place of employment or the local area health service.
None identified.
- 1. Australian Government Department of Health and Ageing. Health workforce resources. Medical Training Review Panel: thirteenth report. http://www.health.gov.au/internet/main/publishing.nsf/Content/work-pubs-mtrp-13 (accessed May 2010).
- 2. Institute of Medical Education and Training. Exploration and development of potential models of flexible working for junior doctors in hospital positions, NSW, 2006. Sydney: IMET, 2006.
- 3. Australian Medical Association. Training and workplace flexibility. Final report. Canberra: AMA, 2001.
- 4. Potter J. Part-time training open to all [letter]? BMJ 1978; 2: 572-573.
- 5. The Royal Australasian College of Physicians. Trainee positions. http://www.racp.edu.au/page.cfm?path=/page/pv_train (accessed [members only] Jun 2010).
- 6. Whitelaw CM, Nash MC. Job-sharing in paediatric training in Australia: availability and trainee perceptions. Med J Aust 2001; 174: 407-409. <MJA full text>
- 7. Carling PC, Hayward K, Coakley EH, Wolf AM. Part-time residency training in internal medicine: analysis of a ten-year experience. Acad Med 1999; 74: 282-284.
- 8. Australian Government Department of Health and Ageing. Specialist Training Program (STP). http://www.health.gov.au/internet/main/publishing.nsf/Content/work-spec (accessed Jun 2010).
- 9. Evans J, Goldacre MJ, Lambert TW. Views of UK medical graduates about flexible and part-time working in medicine: a qualitative study. Med Educ 2000; 34: 355-362.
- 10. Australian Government. Fair Work Ombudsman. Flexible working arrangements. http://www.fairwork.gov.au/employment/conditions-of-employment/flexible-working-arrangements/pages/default.aspx (accessed Mar 2011).
- 11. United Kingdom. NHS Careers. Flexible Careers Scheme (FCS). http://www.nhscareers.nhs.uk/details/Default.aspx?Id=650 (accessed Mar 2011).
- 12. Tolhurst HM, Stewart SM. Balancing work, family and other lifestyle aspects: a qualitative study of Australian medical students’ attitudes. Med J Aust 2004; 181: 361-364. <MJA full text>





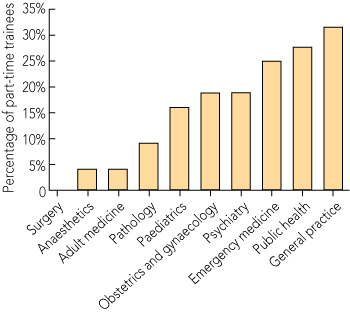
Abstract
Demographic changes among junior doctors are driving demand for increased flexibility in advanced physician training, but flexible training posts are lacking.
Suitable flexible training models include flexible full-time, job-share and part-time positions.
Major barriers to establishing flexible training positions include difficulty in finding job-share partners, lack of funding for creating supernumerary positions, and concern over equivalence of educational quality compared with full-time training.
Pilot flexible training positions should be introduced across the medical specialties and educational outcomes examined prospectively.