Studies examining hospital mortality of patients admitted to intensive care units (ICUs) have revealed increased mortality after (or “off”) hours and on weekends.1-10 In most studies, however, this effect disappeared after controlling for illness severity.1,3-8,10 A systematic review and meta-analysis of the association between time of admission to the ICU and mortality found that patients admitted to the ICU during weekends had an 8% higher risk of death compared with patients admitted during weekdays, but found no such effect for after-hours admission.11
The Australian and New Zealand Intensive Care Society (ANZICS) Centre for Outcome and Resource Evaluation (CORE) manages the ANZICS Adult Patient Database (APD),12 which collects data on ICU admissions in Australian, New Zealand and, more recently, Hong Kong hospitals, and now holds over a million records. The minimum dataset and data definitions used are available on the ANZICS CORE website (http://anzics.com.au/core).
In 2008, 128 ICUs in Australia and New Zealand (about 65 000 ICU admissions), including 34 of the 35 tertiary hospitals, contributed toward the APD. This was estimated to capture over 80% of all Australian ICU admissions that year.13 Thus, the APD is an ideal tool for examining the relationship between time of admission to ICU and hospital mortality.
Previous studies have focused on whether the absence of on-site specialist intensivists after hours significantly increases the mortality of ICU patients admitted after hours.1-10 However, there was considerable heterogeneity in the patient population, definitions of after hours and results of these studies.1-10 The resources, rosters and work practices within ICUs specifically and hospitals in general vary considerably across Australia.13
Ethics approval for the study was granted by the Liverpool Hospital Human Research Ethics Committee.
There is no standard definition of “after hours” for intensive care practice in Australia, and previous publications have not used a consistent definition. A study of the ANZICS APD on the effect on patient outcome of discharge timing from Australian and New Zealand ICUs defined after hours as 18:00 to 05:59,14 so we used the same definition in our study. In hours, after hours, weekdays and weekends are defined in Box 1.
Outcomes at different admission times were examined in four ways:
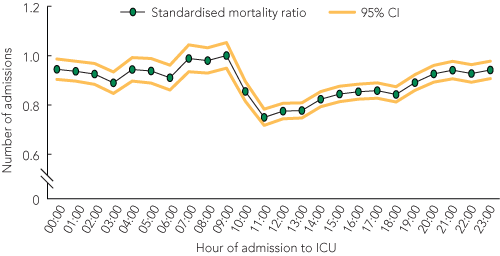
The study included 245 057 ICU patient episodes in 41 ICUs; of these, 47.8% of patients were admitted after hours (Box 2) and 20.1% of patients were admitted on weekends (Box 3). Patients admitted after hours and on weekends were younger than those admitted in hours but had higher APACHE III-j scores and predicted risk of death. Box 4 shows the diurnal variation in number of admissions and observed and APACHE III-j predicted risk of death, and Box 5 shows the diurnal variation in SMR.
ICU mortality, hospital mortality and SMRs were significantly increased among patients admitted after hours and on weekends compared with patients admitted in hours and on weekdays, respectively (Box 2 and Box 3). ICU and hospital lengths of stay were significantly increased among patients admitted on weekends (Box 3), but no such effect was seen after hours (Box 2).
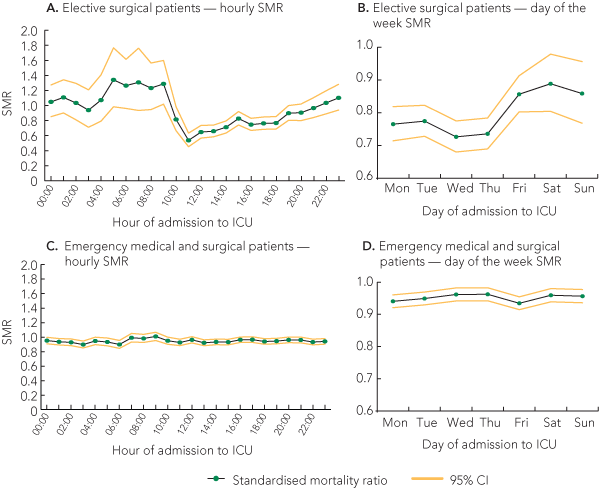
Multivariate logistic regression demonstrated that APACHE III-j risk of death, after-hours admission, weekend admission, a medical diagnosis on admission (as opposed to postoperative admission) and emergency (as opposed to elective surgical) admission were all independently associated with increased mortality (Box 6 and Box 7). Although most variables were highly significant (P < 0.001), elective surgical patients had a Wald χ2 statistic that was over 17 times larger than that of postoperative patients as a whole (847 v 48). Time-of-day and day-of-week SMRs varied considerably between elective surgical patients and emergency medical and surgical patients (Box 8).
Box 9 and Box 10 show the 15 most prevalent elective surgical diagnostic groups, and their observed mortalities and SMRs. Observed mortality was higher among patients who were admitted to the ICU after hours following cardiothoracic surgery, abdominal aortic aneurysm surgery and other gastrointestinal surgery. SMRs were higher among patients who were admitted to the ICU after hours following valvular heart surgery and abdominal aortic aneurysm repair. Many other diagnostic groups showed trends towards increased observed mortality and SMRs among after-hours and weekend admissions, but individually did not reach statistical significance. As seen in Box 9 and Box 10, the SMRs of some elective surgical diagnostic groups, such as “other respiratory surgery” and “laminectomy or spinal cord surgery” were higher in hours compared with after hours and weekdays compared with weekends.
A retrospective cohort study in the Paris metropolitan region showed that off-hours admission to the ICU is common, and may be associated with a slightly lower death rate.5 The researchers attributed this to a delay in assessment of individual patients admitted in hours, higher workloads and more invasive diagnostic and therapeutic interventions in hours. Day shifts are defined by law in France and the definition of off hours used in that study5 was different from our definition of after hours.
A systematic review found that weekend admission was associated with an 8% (95% CI, 4%–13%) higher risk of death than weekday admission. The meta-analysis was dominated by one study that included admission only during mid week (Tuesdays, Wednesdays and Thursdays) as the control group. It found significant heterogeneity among the studies. Moreover, it excluded studies that compared SMRs of the control and study groups.11 Our study population is bigger than that included in the meta-analysis. The definitions of SMRs in the meta-analysis were not uniform. We compared SMRs and did not correlate mortality to ICU physician staffing.
The difference in mortality for patients admitted to the ICU after hours and on weekends in our study was predominantly due to an effect seen in planned admissions to the ICU after elective surgery. This has not been reported before, although Dutch6 and Saudi Arabian1 researchers found similar trends in their studies. However, the Dutch study6 defined “elective surgery” differently from the ANZICS — they included all patients admitted to the ICU within 7 days of elective surgery, whereas the ANZICS defines elective surgical admissions as those admitted directly from the operating theatre or recovery room.
The use of SMRs to compare the mortality in cohorts of ICU patients is valid.15 APACHE III-j has been validated as a risk adjustor for calculation of the SMR among an Australasian ICU population.16
Our study has several limitations. The differences seen may be related to data entry, data synthesis or data integrity. However, as such data errors and inaccuracies are likely to be random, they are unlikely to significantly affect the findings in a study of this size. In addition, regular education and accreditation of data managers, and data verification are conducted by the ANZICS CORE, and the APD is recognised as a high-quality database.12 Elective surgical status is generally well recorded. The ANZICS APD audit of 1102 randomly selected admissions to 44 hospitals demonstrated elective surgical status was coded correctly in 94% of cases.17
We defined after hours as 18:00 to 05:59; other studies1,2,5-7 defined after hours as weeknights and all weekend. The most appropriate definition is unknown. We did not include Friday evenings and Monday mornings as weekends in our audit. This may have influenced our results, although we speculate that broadening the definition would further strengthen our findings.
2 Characteristics and outcomes of 245 057 patients admitted to Australian ICUs in hours and after hours, January 2000 – December 2008
3 Characteristics and outcomes of 245 057 patients admitted to Australian ICUs on weekdays and weekends, January 2000 – December 2008
4 Admissions to ICUs per hour of the day, with hospital mortality and APACHE III-j predicted risk of death
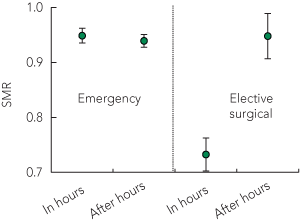
6 APACHE III-j SMRs for elective surgical and emergency patients admitted to intensive care units in hours and after hours
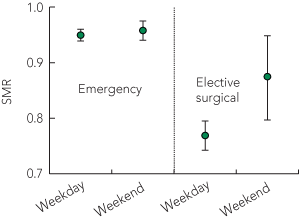
7 APACHE III-j SMRs for elective surgical and emergency patients admitted to intensive care units on weekdays and weekends
8 APACHE III-j SMRs for elective surgical and emergency patients admitted to ICUs by time of day and day of the week
9 Observed mortality and APACHE III-j standardised mortality ratios (SMRs) in hours and after hours for the 15 most prevalent elective surgical diagnoses
|
APACHE III-j = Acute Physiology and Chronic Health Evaluation III, 10th iteration. | |||||||||||||||
Received 18 August 2010, accepted 22 December 2010
- Deepak Bhonagiri1,2
- David V Pilcher3,4
- Michael J Bailey5
- 1 Liverpool Hospital, Sydney, NSW.
- 2 University of New South Wales, Sydney, NSW.
- 3 Alfred Hospital, Melbourne, VIC.
- 4 Australian and New Zealand Intensive Care Society Centre for Outcome and Resource Evaluation, Melbourne, VIC.
- 5 Australian and New Zealand Intensive Care Research Centre, Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
We thank ANZICS CORE staff, especially Carol George and Shaila Chavan; Associate Professor Gillian Bishop and Janice Gregory; and Dr Michael Parr.
None identified.
- 1. Arabi Y, Alshimemeri A, Taher S. Weekend and weeknight admissions have the same outcome of weekday admissions to an intensive care unit with onsite intensivist coverage. Crit Care Med 2006; 34: 605-611.
- 2. Barnett MJ, Kaboli PJ, Sirio CA, Rosenthal GE. Day of the week of intensive care admission and patient outcomes: a multisite regional evaluation. Med Care 2002; 40: 530-539.
- 3. Hixson ED, Davis S, Morris S, Harrison AM. Do weekends or evenings matter in a pediatric intensive care unit? Pediatr Crit Care Med 2005; 6: 523-530.
- 4. Laupland KB, Shahpori R, Kirkpatrick AW, Stelfox HT. Hospital mortality among adults admitted to and discharged from intensive care on weekends and evenings. J Crit Care 2008; 23: 317-324.
- 5. Luyt CE, Combes A, Aegerter P, et al. Mortality among patients admitted to intensive care units during weekday day shifts compared with “off” hours. Crit Care Med 2007; 35: 3-11.
- 6. Meynaar IA, van der Spoel JI, Rommes JH, et al. Off hour admission to an intensivist-led ICU is not associated with increased mortality. Crit Care 2009; 13: R84.
- 7. Morales IJ, Peters SG, Afessa B. Hospital mortality rate and length of stay in patients admitted at night to the intensive care unit. Crit Care Med 2003; 31: 858-863.
- 8. Sheu CC, Tsai JR, Hung JY, et al. Admission time and outcomes of patients in a medical intensive care unit. Kaohsiung J Med Sci 2007; 23: 395-404.
- 9. Uusaro A, Kari A, Ruokonen E. The effects of ICU admission and discharge times on mortality in Finland. Intensive Care Med 2003; 29: 2144-2148.
- 10. Wunsch H, Mapstone J, Brady T, et al. Hospital mortality associated with day and time of admission to intensive care units. Intensive Care Med 2004; 30: 895-901.
- 11. Cavallazzi R, Marik PE, Hirani A, et al. Association between time of admission to the intensive care unit and mortality: a systematic review and meta-analysis. Chest 2010; 138: 68-75.
- 12. Stow PJ, Hart GK, Higlett T, et al. Development and implementation of a high-quality clinical database: the Australian and New Zealand Intensive Care Society Adult Patient Database. J Crit Care 2006; 21: 133-141.
- 13. Drennan K, Hicks P, Hart GK. Intensive care resources & activity: Australia and New Zealand 2007/2008. Melbourne: Australian and New Zealand Intensive Care Society, 2010.
- 14. Pilcher DV, Duke GJ, George C, et al. After-hours discharge from intensive care increases the risk of readmission and death. Anaesth Intensive Care 2007; 35: 477-485.
- 15. Cook DA, Duke G, Hart GK, et al. Review of the application of risk-adjusted charts to analyse mortality outcomes in critical care. Crit Care Resusc 2008; 10: 239-251.
- 16. Cook DA, Joyce CJ, Barnett RJ, et al. Prospective independent validation of APACHE III models in an Australian tertiary adult intensive care unit. Anaesth Intensive Care 2002; 30: 308-315.
- 17. Australian and New Zealand Intensive Care Society Centre for Outcome and Resource Evaluation. APD data audit report. Cycle 1: 2007–2009. http://www.anzics.com.au/core/apd-data-audit-project (accessed Nov 2010).





Abstract
Objective: To study variation in mortality associated with time and day of admission to the intensive care unit (ICU).
Design: Retrospective cohort analysis using the Australian and New Zealand Intensive Care Society Adult Patient Database.
Setting and participants: 245 057 admissions to 41 Australian ICUs from January 2000 to December 2008.
Main outcome measures: Observed mortality and standardised mortality ratio (SMR) based on Acute Physiology and Chronic Health Evaluation III, 10th iteration (APACHE III-j) scores. Subgroup analysis was performed on the basis of elective surgical or emergency admission to ICU.
Results: 48% of patients were admitted after hours (18:00–05:59) and 20% of patients were admitted on weekends (Saturday and Sunday). Patients admitted after hours had a 17% hospital mortality rate compared with 14% of patients admitted in hours (P < 0.001); and SMRs of 0.92 (95% CI, 0.91–0.93) and 0.83 (95% CI, 0.83–0.84), respectively. Weekend admissions had a 20% hospital mortality rate compared with 14% on weekdays (P < 0.001), with SMRs of 0.95 (95% CI, 0.94–0.97) and 0.92 (95% CI, 0.92–0.93), respectively. Variation in outcome with time of admission to ICU was accounted for predominantly by elective surgical patients.
Conclusions: Patients admitted to ICUs in Australia after hours and on weekends have a higher observed and risk-adjusted mortality than patients admitted at other times. Further research is required to determine the causes and relationship to resource availability and staffing.