It remains debatable that the Rudd government’s health care reform solutions were revolutionary. The collective proposals fell short of addressing the fundamental causes of health system failure. Despite the efforts of the government in producing weighty reports with hundreds of pages and dozens of recommendations,2-5 the solutions (according to some) were chiefly mechanistic and structural, although the National Health and Hospitals Reform Commission (NHHRC) report has much useful information and many viable recommendations. At last month’s Council of Australian Governments (COAG) meeting, the heads of agreement between the Commonwealth, states and territories authoritatively pronounced on a range of high-level principles, particularly on shared funding, standards of care and performance, and committing to local governance, but it is not clear how reform will be accomplished or what its eventual shape will be.
Basic questions remain unanswered, such as, “What is collectively meant by health?” Most in the medical community are busy treating breakdowns in individual patients’ conditions, and are thus dissonant about, and distant from, such a question. At what point will we be happy with the health system? What will a well functioning, clearly focused health care service look like?6-9
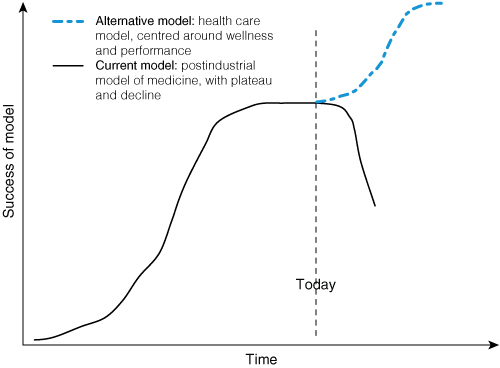
We illustrate the point in Box 1. The old paradigm of health care was predicated on industrial thinking and disease management, the mainstays of which are drugs, procedures and biochemical and radiological testing. This needs to shift to a wellness-oriented system focused on performance and outcomes, requiring a radical overhaul.
Consider the values of stakeholders in the system now, which we have observed emerging for some time. They can be seen expressed increasingly through participants’ behaviours, practices, attitudes and beliefs. Consider how it might be if they were reframed. In Box 2, the normative values are those toward which the respective stakeholder groups ought to be striving.
In short, while some groups and individuals display normative values some of the time, these instances are much rarer than is preferable. Stakeholder groups are “tribal”,10 favouring their in-group membership over others, and pursue anachronistic or idiosyncratic values. Yet, if human societies eschew the greater good, they run the risk of confronting the “tragedy of the commons” — a well known phenomenon in which the pursuit of sectional interests jeopardises collective wellbeing, as was seen in the recent international banking crisis, and is occurring with deforestation and climate change. We need to reorient the system, aiming to satisfy the needs of the whole community, and taking a less inward, narcissistic focus.
Can we get to this stage? Are we being excessively optimistic? In a modern psychology classic,11 Howard Gardner examined how to get people to think differently, and he specified how leaders could induce groups to change their mindsets. He argued that there were seven levers for change, which he called the “seven Rs”:
reason involves employing logic and weighing factors so that people are persuaded about the potential change
research is adduced by collecting, analysing and interpreting data to bolster the argument
resonance means that something has to “feel right” to be supported
redescriptions are used to assist in convincing people, that is, the core message is recoded in several forms, because different people respond to different messages
resources and rewards are important to support the planned change
real world views of people should be acted on, to try to create a mind shift
resistances (factors which solidify into resistance to change, or disagreement with the proposed change) should be identified, and attempts made to nullify them.
Government plans usually try to grind the gears of reason (the population is in favour of the general logic of health care reform) and resonance (the public suspects intuitively that reform is overdue). The public have noted that the states and territories have been provided with resources and rewards by the federal government in the past round of reform proposals. However, how they will flow to the stakeholder groups to act as incentives for them is not clear, particularly with the reshaped national political landscape since the August 2010 election. The NHHRC’s precursor report provided some research (but not randomised controlled data, of course) in support of a revamped health system. More work is likely to be needed by the new government, if they want to pursue reform, to recode their message into redescriptions for various stakeholder groups (after all, how many of us, apart from academics or policy wonks, will, in reality, read lengthy policy reports?). Redescriptions should be designed to overcome various resistances which coagulate whenever reform is proposed. As far as real-world values are concerned, we have made explicit what we believe they are now, or are becoming, and should be encouraged to become, in Box 2.
What we have seen is a range of measures to put the federal government’s current reform proposals into effect (Box 3). While commentators will no doubt feel the package is supportable within the current paradigm, it is unlikely to be a game changer in the way we are advocating.
If there was an inkling that the new government was willing to articulate an argument grounded in values, a plan for implementation as useful as Gardner’s, and reform based much more on improving health rather than alterations to the structure,13,14 people might be more encouraged. Fresh thinking like this is needed in the new parliament. Otherwise, we may risk seeing no real lasting reform, continue to lament lost opportunities, fail to provide the underpinnings to Van Der Weyden’s “innovative and revolutionary reform”, and encounter, with perpetual deja vu, many more inquiries and reports into our health system. That will be in no one’s interests.
2 Present and emerging versus normative values for health care
3 Examples of policy and legislative reform measures12
- Jeffrey Braithwaite1
- Clare A Skinner2
- Mei Ling Döéry3
- 1 Australian Institute of Health Innovation, University of New South Wales, Sydney, NSW.
- 2 Royal North Shore Hospital, Sydney, NSW.
- 3 Victorian Health Promotion Foundation, Melbourne, VIC.
Jeffrey Braithwaite’s work is supported by National Health and Medical Research Council Program grant 568612.
None identified.
- 1. Van Der Weyden MB. Health reform cycles. Med J Aust 2010; 192: 625. <MJA full text>
- 2. Australian Government. A national health and hospitals network for Australia’s future. Canberra: Commonwealth of Australia, 2010. http://www.yourhealth.gov.au/internet/yourhealth/publishing.nsf/Content/nhhn-report-toc/$FILE/NHHN%20-%20Full%20report.pdf (accessed Jan 2011).
- 3. Australian Government. A national health and hospitals network: further investments in Australia’s health. Canberra: Commonwealth of Australia, 2010. http://www.health.gov.au/internet/main/publishing.nsf/Content/nhhn-report-2/$File/NHHN%20Report%20two.pdf (accessed Jan 2011).
- 4. Australian Government. A national health and hospitals network for Australia’s future: delivering better health and better hospitals. Canberra: Commonwealth of Australia, 2010. http://www.health.gov.au/internet/yourhealth/publishing.nsf/Content/report-redbook/$File/HRT_report3.pdf (accessed Jan 2011).
- 5. National Health and Hospitals Reform Commission. A healthier future for all Australians: final report — June 2009. Canberra: Australian Government, 2009. http://www.health.gov.au/internet/nhhrc/publishing.nsf/Content/nhhrc-report (accessed Jan 2011).
- 6. Braithwaite J, Goulston K. Turning the health system 90 degrees down under. Lancet 2004; 364: 397-399.
- 7. Braithwaite J, Runciman WB, Merry AF. Towards safer, better healthcare: harnessing the natural properties of complex sociotechnical systems. Qual Saf Health Care 2009; 18: 37-41.
- 8. Braithwaite J, Westbrook M, Iedema R, et al. A tale of two hospitals: assessing cultural landscapes and compositions. Soc Sci Med 2005; 60: 1149-1162.
- 9. Braithwaite J, Westbrook MT, Travaglia JF, et al. Are health systems changing in support of patient safety? A multi-methods evaluation of education, attitudes and practice. Int J Health Care Qual Assur 2007; 20: 585-601.
- 10. Braithwaite J, Iedema RA, Jorm C. Trust, communication, theory of mind and the social brain hypothesis: deep explanations for what goes wrong in health care. J Health Organ Manag 2007; 21: 353-367.
- 11. Gardner H. Changing minds: the art and science of changing our own and other people’s minds. Boston: Harvard Business School Press, 2004.
- 12. Australian Government Department of Health and Ageing. Health Reform. Canberra: Commonwealth of Australia, 2010. http://www.yourhealth.gov.au/internet/yourhealth/publishing.nsf/content/home (accessed Jan 2011).
- 13. Braithwaite J. How to restructure-proof your health service. BMJ 2007; 335: 99.
- 14. Braithwaite J. Invest in people, not restructuring [letter]. BMJ 2005; 331: 1272.





Abstract
We do not have a health system with collaboratively oriented values.
Reforms that former prime minister Kevin Rudd initiated, which are now Prime Minister Julia Gillard’s to prosecute, do not support such a health system.
Reformers have consistently ignored present and potential values.
A plan for reform of the health system must take into account differing stakeholders’ objectives and values and incorporate new values.
This requires an agreement by stakeholders to embrace the common good.
It will also need strong leadership and a willingness to embrace fundamental change.