Depression is particularly prevalent among women.1,2 Women with depression may benefit from psychotherapeutic counselling (in addition to or instead of antidepressant medication);3 however, this form of treatment has been unaffordable for many.4
Mental health problems differentially affect women with greater socioeconomic stress, who may be least likely to access mental health services under a user-pays scheme.5 To improve access to mental health services, in November 2006, Medicare Australia introduced Medicare Benefits Schedule (MBS) items for mental health services under the Better Access Initiative. The Initiative allows patients with a mental health condition to receive up to 12 individual mental health services a year, including consultations with eligible psychologists, social workers and occupational therapists. Rebates for these services are available to patients who have been referred by a psychiatrist (Psychiatrist Assessment and Management Plan), paediatrician or general practitioner (General Practitioner Mental Health Care Plan).6
According to Medicare data, uptake of MBS mental health items has been rapid and substantial. From November 2006 to October 2007, the items accounted for 1 209 191 services.7 Growth was greater in metropolitan locations compared with rural and remote areas,6 and it was thought that initial beneficiaries were largely those already receiving counselling services.5 However, a survey of psychologists showed that 81% of clients seen under the mental health items were new to the practice, and 72% of new clients had not previously seen a psychologist.8 The survey also found that 36% of people seen under the Better Access Initiative were aged 25 years or younger, 57% were between 26 and 65 years, and 7% were over 65 years.8
There is otherwise little information about the characteristics of people who use mental health services. Consequently, it is not known whether providing subsidised services addresses inequities in service access.5 In this study, we aimed to:
quantify uptake of mental health items by women participating in the Australian Longitudinal Study on Women’s Health (ALSWH),9 particularly those who reported mental health problems on one or more surveys; and
describe and compare characteristics of women who have and have not used the mental health items; and
investigate the impact of the items on the costs of Medicare services.
The study involved analysis of longitudinal data from the ALSWH, a national population-based study of the health of Australian women born in one of three periods, 1921–1926 (“older cohort”), 1946–1951 (“mid-age cohort”), and 1973–1978 (“younger cohort”). Women were randomly selected from the Medicare database10 and all cohorts completed the baseline survey in 1996. The first follow-up survey was conducted for the mid-age cohort in 1998, older cohort in 1999, and younger cohort in 2000. Subsequent follow-up surveys were conducted on a rotational basis every 3 years. This study includes women who participated in follow-up surveys 4 (S4) in 2005 and 2006 for the older and younger cohorts and survey 5 (S5) in 2007 for the mid-age cohort, who consented to linkage of their ALSWH survey data with their Medicare records.
At each survey, women were asked whether a doctor had told them they had any of a list of chronic health conditions including depression and anxiety (and postnatal depression among younger women). Health status was measured by the 36-Item Short Form Health Survey (SF-36),11 which includes a Mental Health Index11,12 that correlates highly with other measures of depression and anxiety.13-15
Survey questions included number of visits to a GP, specialist doctor, optician, dentist, counsellor, or other allied health care provider, admission to hospital in the previous 12 months, and number and type of prescribed medications.16 Additionally, women were asked about health insurance, smoking, alcohol consumption, weight and height (used to calculate body mass index [BMI]),17 and physical activity.10 Sociodemographic data on age, marital status, education and country of birth were collected. Urban, inner regional, outer regional or remote area of residence was classified using the Accessibility/Remoteness Index of Australia.18
The study was approved by the Human Research Ethics Committee of the University of Newcastle.
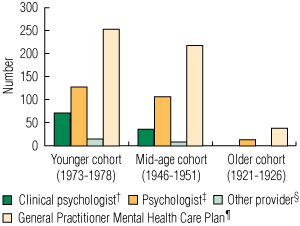
Data were available for 14 911 women who consented to linkage of their MBS and survey data — 3869 women in the younger cohort who completed the most recent survey (S4; 43% of the cohort), 6690 women in the mid-age cohort (S5; 64% of the cohort), and 4352 women in the older cohort (S4; 66% of the cohort). During the study period, 5% of women in the younger cohort, 2% of women in the mid-age cohort, and less than 1% of women in the older cohort had made claims for mental health items. Box 1 shows that the most common items were for a GP Mental Health Care Plan, clinical psychologists and other psychologist services.
Among women who reported depression, anxiety or other mental health condition on the most recent survey, 12% of those in the younger cohort, 10% of the mid-age cohort, and 1% of the older cohort had used mental health items (Box 2).
5% of younger women and 2% of mid-age women had mental health item claims (Group 1);
16% of younger women and 15% of mid-age women had a self-reported recent mental health condition, but no mental health item claims (Group 2);
12% of younger women and 17% of mid-age women had a self-reported past mental health condition, but no mental health item claims (Group 3); and
67% of younger women and 65% of mid-age women had no mental health item claims or self-reported mental health condition (Group 4).
Group comparisons in Box 3 indicate sociodemographic and health differences between these groups of women in the younger cohort. Similar results were seen in the mid-age cohort (data not shown). Women in Group 2 were more likely to visit a GP, specialist or hospital doctor and more likely to report taking medications for “nerves”, depression, or to help them sleep. There were no differences in area of residence, alcohol intake or country of birth. All variables in Box 3 are significant with P < 0.001 except BMI, where P = 0.002.
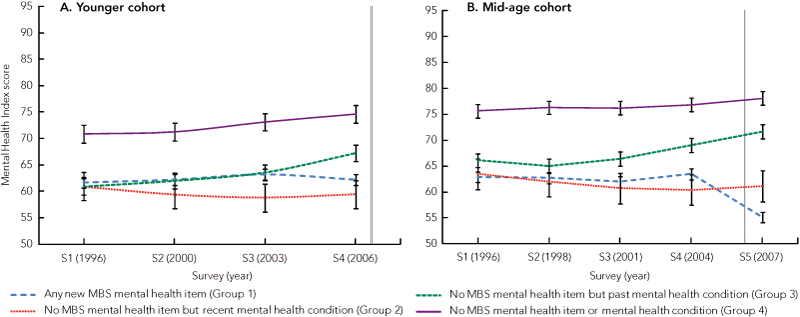
Box 4 shows SF-36 Mental Health Index scores for the younger and mid-age cohorts. Mental Health Index scores among women in both cohorts were lowest for women in Groups 1 and 2. Over time, there was an improvement in scores for women in Group 3 (S4 for younger cohort, S5 for mid-age cohort). For women in the mid-age cohort who had used mental health items (Group 1), the Mental Health Index score dropped significantly from survey 4 in 2004 to survey 5 in 2007, indicating a decline in mental health-related quality of life.
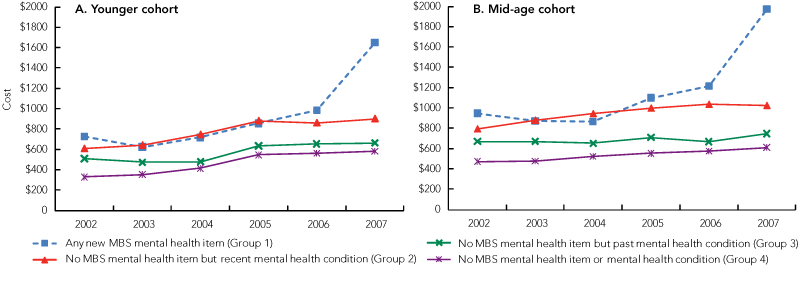
Box 5 and Box 6 show the increase in patient (out-of-pocket) and benefit (government) costs following introduction of the mental health items. Uptake of mental health items was associated with a steep increase in both cost types during 2007, with average yearly increases of $100–$150 for women, and $600–$800 for government.
Although earlier reports provided evidence of rapid uptake of mental health items, these findings indicate that the per-capita impact of the items is small. A large proportion of women reporting a history of mental health problems had no mental health item claims, suggesting that issues of access were not being addressed as intended.19
An analysis of the 1997 National Survey of Mental Health and Wellbeing showed that for every nine people with a mental health disorder, only one had consulted a mental health professional in the previous year.20 This study also showed that women were almost twice as likely to consult a mental health professional as men,20 so the impact of the mental health items among men may be lower than observed for women in our study.
Our data show that women who are more socioeconomically disadvantaged are less likely to access these services, despite mental health needs. The data also show a particularly low uptake of the items by the oldest group of women, consistent with other research suggesting undertreatment of mental health problems among older people.21 On the other hand, among women who did use the services, very few had previously reported seeing a counsellor, psychologist or social worker, indicating that new items reached women who were not previously accessing mental health care.
The mental health items are associated with increases in costs for women and for governments. It is therefore critical that the impact and equity of impact of these items are assessed further. This imperative exists not only because of costs to government, which have been described as considerable7,19 but also in view of the added economic stress on individual women and the potential for the scheme to increase health inequalities. If women who have difficulty managing on their available income and who have lower educational levels are less able to make use of mental health services despite their mental health needs, the scheme does not necessarily address gaps in service provision as intended.
Although our data provide information on characteristics of women using services covered by mental health items, our study has some limitations. One limitation is that not all women in the ALSWH consented to linkage with MBS data. Comparison between consenters and non-consenters at the time of completing survey 4 indicates small but statistically significant differences according to area of residence (consenters in the mid-age and older cohorts were more likely to live in urban or inner regional areas and less likely to live in outer regional or remote areas). In all three cohorts, women who gave consent to data linkage tended to be better educated and were more likely to be able to manage on their available income, which suggests a socioeconomic bias among consenters.22 However, if more disadvantaged women are less likely to use mental health items in spite of mental health needs, uptake of the items is likely to be even lower than shown here.
Other limitations include that some women may be accessing focused psychological services under the Better Outcomes in Mental Health Care program, which complements the Better Access Initiative and which is outside of the Medicare Benefits Schedule.23 By 2008, it was estimated that 153 000 Australians had used these services. Although some of this use would be picked up by the women’s self-reported visits to counsellors, there may be some underreporting of these services.
1 Number of women in each cohort who accessed Medicare Benefits Schedule mental health items, November 2006 – December 2007*
2 Use of Medicare Benefits Schedule mental health items by women with recent and past reports of a mental health condition*†
3 Characteristics of women from the younger cohort (1973–1978) according to use of Medicare Benefits Schedule mental health (MH) items and recent or past MH condition*
Visits to counsellor, psychologist or social worker (before introduction of MH items) |
|||||||||||||||
Provide care to any person with long-term illness, disability or frailty |
|||||||||||||||
4 SF-36 Mental Health Index scores for younger (1973–1978) and mid-age (1946–1951) cohorts according to mental health item claims and recent or past mental health condition*
Received 23 April 2010, accepted 2 November 2010
- Julie E Byles1
- Xenia Dolja-Gore2
- Deborah J Loxton3
- Lynne Parkinson4
- Jennifer A Stewart Williams5
- Research Centre for Gender, Health and Ageing, University of Newcastle, Newcastle, NSW.
The ALSWH was funded by the Australian Government Department of Health and Ageing. This study was supported by a grant from Australian Rotary Health.
None identified.
- 1. Lucht M, Schaub RT, Meyer C, et al. Gender differences in unipolar depression: a general population survey of adults between age 18 to 64 of German nationality. J Affect Disord 2003; 77: 203-211.
- 2. Hyde JS, Mezulis AH, Abramson LY. The ABCs of depression: integrating affective, biological and cognitive models to explain the emergence of the gender difference in depression. Psychol Rev 2008; 115: 291-313.
- 3. Abbass A, Hancock J, Henderson J, Kisely S. Short-term psychodynamic psychotherapies for common mental disorders. Cochrane Database Syst Rev 2006; (4): CD004687.
- 4. Chisholm D, Sanderson K, Ayuso-Mateos JL, et al. Reducing the global burden of depression: population-level analysis of intervention cost-effectiveness in 14 world regions. Br J Psychiatry 2004; 184: 393-403.
- 5. Hickey I, McGorry P. Increased access to evidence-based primary mental health care: will the implementation match the rhetoric? Med J Aust 2007; 187: 69-71. <MJA full text>
- 6. Crosbie D, Rosenberg S. Mental health and the new Medicare services: an analysis of the first six months. July 2007. http://www.mhca.org.au/documents/FINALMBSREPORT.pdf (accessed Dec 2010).
- 7. Whiteford H, Doessel D, Sheridan J. Uptake of Medicare Benefits Schedule items by psychologists and other mental health practitioners. Clinical Psychologist 2008; 12: 50-56.
- 8. Giese J, Lindner H, Forsyth C, Lovelock H. Survey of clients receiving Medicare-funded psychological services under the Better Access Initiative. InPsych: the Bulletin of the Australian Psychological Society Ltd 2008; 30 (4).
- 9. Australian Longitudinal Study on Women’s Health. http://www.alswh.org.au/surveys.html (accessed Dec 2010).
- 10. Brown WJ, Bryson L, Byles JE, et al. Women’s Health Australia: recruitment for a national longitudinal cohort study. Women Health 1998; 28: 23-40.
- 11. Ware JE, Kosinski M, Keller ST. SF-36 Physical and Mental Health Summary Scales: a user’s manual. Boston: Health Institute, 1994.
- 12. McCallum J, Shadbolt B, Wang D. Self-rated health and survival: a 7-year follow-up study of Australian elderly. Am J Public Health 1994; 84: 1100-1105.
- 13. Goldberg D, Bridges K, Duncan-Jones P, Grayson D. Detecting anxiety and depression in general medical settings. BMJ 1988; 297: 897-899.
- 14. Andresen EM, Malmgren JA, Carter WB, Patrick DL. Screening for depression in well older adults: evaluation of a short form of the CES-D (Center for Epidemiologic Studies Depression Scale). Am J Prev Med 1994; 10: 77-84.
- 15. Women’s Health Australia. The Australian Longitudinal Study on Women’s Health. Report 16. 10 June 2001. http://www.alswh.org.au/Reports/Technical/Report%2016%20ALSWH.pdf (accessed Dec 2010).
- 16. Young AF, Dobson AJ, Byles JE. Access and equity in the provision of general practitioner services for women in Australia. Aust N Z J Public Health 2000; 24: 474-480.
- 17. World Health Organization Consultation on Obesity. Obesity: preventing and managing the global epidemic: report of a WHO consultation. Geneva: WHO, 1999.
- 18. Australian Government Department of Health and Aged Care (GISCA). Measuring remoteness: Accessibility/Remoteness Index of Australia (ARIA). Canberra: DHAC, 2001.
- 19. Carey T, Rickwood D, Baker K. What does $UD27,650,523.80 worth of evidence look like? Clin Psychol 2009; 13: 10-16.
- 20. Andrews G, Issakidis C, Carter G. Shortfall in mental health service utilisation. Br J Psychiatry 2001; 179: 417-425.
- 21. Zhang Y, Chow V, Vitry AI, et al. Antidepressant use and depressive symptomatology among older people from the Australian Longitudinal Study of Ageing. Int Psychogeriatr 2010; 22: 437-444.
- 22. Byles J, Loxton D, Berecki J, et al. Use and costs of medications and other health care resources: findings from the Australian Longitudinal Study on Women’s Health. Report to the Department of Health and Ageing, June 2008.
- 23. Australian Government Department of Health and Ageing. Access to Allied Psychological Services (ATAPS). Canberra: DoHA, 2010. http://www.health.gov.au/internet/main/publishing.nsf/Content/mental-boimhc-ataps (accessed Dec 2010).





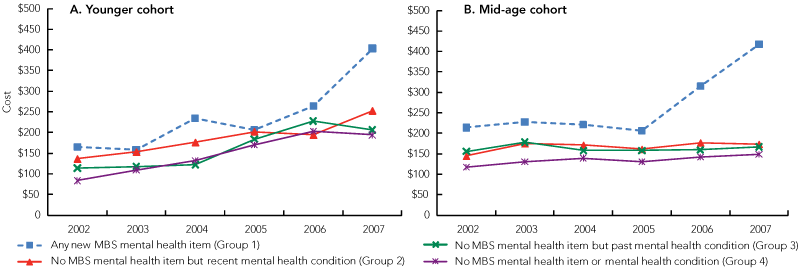
Abstract
Objective: To quantify women’s uptake of Medicare Benefits Schedule mental health items, compare characteristics of women by mental health service use, and investigate the impact on Medicare costs.
Design, setting and participants: Analysis of linked survey data and Medicare records (November 2006 – December 2007) of 14 911 consenting participants of the Australian Longitudinal Study on Women’s Health (ALSWH) across three birth cohorts (1921–1926 [“older cohort”], 1946–1951 [“mid-age cohort”], and 1973–1978 [“younger cohort”]).
Main outcome measures: Uptake of mental health items; 36-Item Short Form Health Survey (SF-36) Mental Health Index scores from ALSWH surveys; and patient (out-of-pocket) and benefit (government) costs from Medicare data.
Results: A large proportion of women who reported mental health problems made no mental health claims (on the most recent survey, 88%, 90% and 99% of the younger, mid-age and older cohorts, respectively). Socioeconomically disadvantaged women were less likely to use the services. SF-36 Mental Health Index scores among women in the younger and mid-age cohorts were lowest for women who had accessed mental health items or self-reported a recent mental health condition. Mental health items are associated with higher costs to women and government.
Conclusion: Although there has been rapid uptake of mental health items, uptake by women with mental health needs is low and there is potential socioeconomic inequity.