Over the past 20 years, there has been a sustained rise in demand for emergency ambulance services across the developed world.1-4 Growth in emergency transportations is an important determinant of emergency department attendances.5 In particular, transport of older patients has a significant impact on acute hospital capacity because of high admission rates and long lengths of stay.6,7 Resultant pressure compromises access, quality of care and patient safety, with emergency department congestion and overcrowding reported regularly.8-11 The strains on ambulance services, however, are less well documented.
To date, researchers and service providers have focused on describing the increasing rate of ambulance use and the effect on response times over short periods.1-4,12-14 Some have examined the influence of demographic and health system dynamics on the use of emergency resources. Two recent reviews have suggested that changes in demographics, population health, health system practices, public expectations and accessibility of ambulance services contribute to rising demand, with population growth and ageing proposed as key drivers.15,16
Older people will make up an increasingly larger proportion of the population in the future.17 About 13% of the population in the United Kingdom, United States and Australia are currently aged over 65 years. It is projected that this will increase to 25% over the next 25 years, with the proportion aged over 85 years rising from 1.6% to around 5%.18-20
Emergency transportation data were provided in a de-identified format by Ambulance Victoria. Data elements comprised demographic characteristics (including age and sex) and clinical condition of the patient as identified at the time of the request for assistance using the Advanced Medical Priority Dispatch System (Priority Dispatch Corporation, Salt Lake City, Utah, USA). Population data published by the Australian Bureau of Statistics21-23 were used to calculate emergency transportation rates by age and sex. Projected population estimates from the Australian Bureau of Statistics (based on conservative assumptions of fertility, life expectancy and migration) were used to forecast demand for emergency transportation in 2014–15.
We calculated the average rate of transportation by age and sex over the 14-year study period and the expected number of transportations per year, aggregating age and sex. Observed and expected numbers of transportations were used to generate a standardised transportation ratio for each year. This was used to estimate the increase in transportations over time, allowing for changes in the demographic structure of the population.
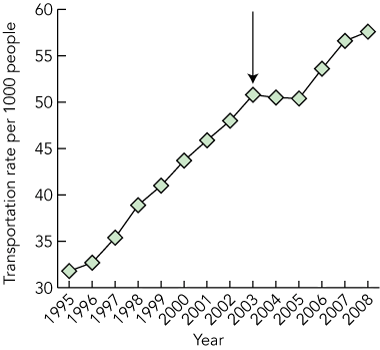
During the 14 years studied, there were 2 227 144 emergency ambulance transportations in metropolitan Melbourne. The crude rate of emergency transportation for males and females of all ages increased from 32 per 1000 people in 1994–95 to 58 per 1000 people in 2007–08 (Box 1). The rate decreased in late 2003 following the introduction of an ambulance referral service designed to curb demand — after adjusting for the effects and interactions of age, sex and the referral service, the rate was decreased by 10%. However, the rate increased again by 2006 to levels above those in 2003. For suitable patients, the referral service enables provision of self-care telephone advice, referral to a non-emergency transport service or referral to a community-based service as an alternative to emergency ambulance dispatch at the time of the initial telephone call. Ambulance Victoria data for 2011 indicate that about 8% of callers are currently directed to one of these options.
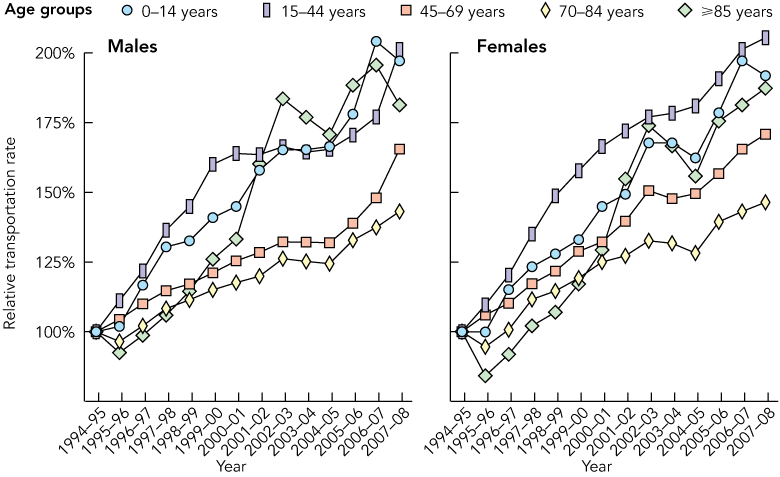
Transportation rate increases were only partly accounted for by changes in population size and age and sex distribution. The rate of transportation for all ages increased by 75% over the 14 years studied (95% CI, 62%–89%). This represented an average annual growth rate of 4.8% (95% CI, 4.3%–5.3%) beyond that explained by demographic changes. There were similar relative proportional increases in all age groups and the highest absolute rates were in the oldest patients (Box 2). Transportation rates relative to those in 1994–95 increased for males and females in all age groups in a linear and uniform manner (Box 3), suggesting an exponential increase in the transportation rates over time.
When log-linear modelling, which is usually applied to rates of occurrence of events, was tested against linear modelling of the data to 2007–08, the difference in performance was imperceptible. We therefore used both models to forecast demand in 2014–15 (Box 2). The total number of emergency transportations in metropolitan Melbourne could increase by 46%–69% by 2014–15.
The projected numbers and rates of transportations by age group to 2014–15 (Box 4 and Box 5) demonstrate that demand by people aged ≥ 85 years will continue to accelerate in the future. Among those aged ≥ 85 years, the rate could rise from the observed 474 per 1000 people in 2007–08 to more than 800 per 1000 people in 2014–15, with the absolute numbers of transportations rising more than twofold.
Our study shows that there has been a dramatic rise in emergency transportations in Melbourne over the 14-year period to June 2008. The association that we identified between transportation rates and increasing age concurs with previous findings.2,15,25-27 However, to our knowledge, this is the first study to identify an increasing and accelerated rate of demand by patients aged ≥ 85 years compared with other age groups, which cannot be explained by demographic changes alone, and it is the first to model future demand while taking population ageing into account.
Demand for emergency health care services among older patients is driven by many factors. Older patients often present to emergency departments with more complex clinical conditions than younger patients.6,7 The most commonly reported reasons for transportation of older patients in our study were similar to those identified previously 2,25,28 and no specific condition was responsible for the increasing ambulance use; falls, chest pain, breathing problems and light-headedness have been recognised as ailments associated with seeking health care.29 Reduced capacity to care for older relatives and an increasing proportion of the older population living alone,30 alongside reduced access to primary health care,31,32 can leave older patients with few alternatives for accessing health care, particularly outside normal working hours. Recent improvements in health awareness and increasing community expectation may also be factors.33 In addition, limited price signals (low or no cost) could drive ambulance use by older people.16 In Melbourne, funding arrangements via the government for a low-cost ($70) annual subscription ensure that the majority (86%) of patients transported have no out-of-pocket expense, and pensioners are entitled to free transport.
Ambulance services in the UK and Australia have taken steps to combat rising demand.34,35 Our study showed that introduction of a referral service reduced the rate of transportations but did not slow the steady increase over time. Although the referral service is diverting an increasing number of emergency requests to alternative resources, growth rates in transportation have returned to the historical norm. This shows that service providers and funding agencies across the continuum of emergency health care need to prioritise working together to develop a coordinated whole-of-system approach, including innovative models of out-of-hospital patient-centred care. Other demand management strategies that have been introduced include the UK’s NHS Direct and Victoria’s NURSE-ON-CALL and after-hours general practitioner clinics, but these have had little impact on reducing demand on emergency resources.36,37 The effects of other strategies that have been implemented — including outreach programs such as hospital-in-the-home and hospital-in-the-nursing-home, mobile specialist teams, and urgent-care walk-in clinics — are yet to be rigorously evaluated.38,39
As numbers and rates of presentations of older patients with complex illnesses and medication regimens increase, the training of emergency health care workers must ensure that they are equipped to meet the special care needs of older patients. This includes acknowledgement of limitations to care, especially with respect to aggressive treatment being inappropriate in very elderly and palliative-care patients.39 Service providers in the UK and Australia have recently introduced non-transportation protocols that extend paramedics’ duties to “treat and leave” patients at their place of residence. In addition, UK service providers have begun conveying patients to alternative, more appropriate health services, instead of emergency departments.40,41 Evaluation of the safety and efficacy of these alternative services is ongoing.42
A strength of our study is its population-based and longitudinal nature, which enabled analysis of 2.27 million emergency transportations over 14 years. The only other longitudinal study that we are aware of examined call rate data from the sole provider of ambulance services in London for three 1-week periods between 1989 and 1999.3 A limitation of our study is that it was not possible to identify the number of repeated transportations of same individuals, as the data were de-identified. Also, the predictions are based on past trends in transportation and demographics and, as such, rely on the same trends prevailing over the forecast period.
1 Emergency transportation rates for males and females of all ages, Melbourne (1994–95 to 2007–08 financial years)*
 |
|
|
2 Total numbers of emergency transportations and transportation rates by age group, Melbourne (1994–95, 2007–08 and 2014–15 financial years)
|
|
|
||||||||||||||
3 Emergency transportation rates by sex and age group, relative to rates for the financial year 1994–95, Melbourne (1994–95 to 2007–08 financial years)
Provenance: Not commissioned; externally peer reviewed.
Received 8 December 2010, accepted 11 April 2011
- Judy A Lowthian1
- Damien J Jolley1
- Andrea J Curtis1
- Alexander Currell1,2
- Peter A Cameron1
- Johannes U Stoelwinder1
- John J McNeil1
- 1 School of Public Health and Preventive Medicine, Monash University, Melbourne, VIC.
- 2 Ambulance Victoria, Melbourne, VIC.
Judy Lowthian is the recipient of a National Health and Medical Research Council postgraduate research scholarship to undertake her doctorate on emergency demand.
None identified.
- 1. Clark MJ, Purdie J, FitzGerald GJ, et al. Predictors of demand for emergency prehospital care: an Australian study. Prehosp Disaster Med 1999; 14: 167-173.
- 2. Svenson JE. Patterns of use of emergency medical transport: a population-based study. Am J Emerg Med 2000; 18: 130-134.
- 3. Peacock PJ, Peacock JL, Victor CR, Chazot C. Changes in the emergency workload of the London Ambulance Service between 1989 and 1999. Emerg Med J 2005; 22: 56-59.
- 4. Burt CW, McCaig LF, Valverde RH. Analysis of ambulance transports and diversions among US emergency departments. Ann Emerg Med 2006; 47: 317-326.
- 5. Steering Committee for the Review of Government Service Provision. Report on government services 2009. Canberra: Productivity Commission, 2009.
- 6. Aminzadeh F, Dalziel WB. Older adults in the emergency department: a systematic review of patterns of use, adverse outcomes, and effectiveness of interventions. Ann Emerg Med 2002; 39: 238-247.
- 7. George G, Jell C, Todd BS. Effect of population ageing on emergency department speed and efficiency: a historical perspective from a district general hospital in the UK. Emerg Med J 2006; 23: 379-383.
- 8. Kennedy JF, Trethewy C, Anderson K. Content analysis of Australian newspaper portrayals of emergency medicine. Emerg Med Australas 2006; 18: 118-124.
- 9. Ardagh M, Richardson S. Emergency department overcrowding — can we fix it? N Z Med J 2004; 117: U774.
- 10. Derlet RW, Richards JR, Kravitz RL. Frequent overcrowding in US emergency departments. Acad Emerg Med 2001; 8: 151-155.
- 11. Rowe B, Bond K, Ospina MB, et al. Frequency, determinants, and impact of overcrowding in emergency departments in Canada: a national survey of emergency department directors. Ottawa: Canadian Agency for Drugs and Technologies in Health, 2006.
- 12. The NHS Information Centre, Workforce and Facilities. Ambulance Services, England 2008–09. London: NHS, 2009.
- 13. Council of Ambulance Authorities. 2007–08 annual report. Adelaide: CAA, 2008.
- 14. St John. Annual report 2009. Wellington: St John, 2009.
- 15. Australian Institute for Primary Care. Factors in Ambulance demand: options for funding and forecasting. Melbourne: La Trobe University, 2007.
- 16. Lowthian JA, Cameron PA, Stoelwinder JU, et al. Increasing utilisation of emergency ambulances. Aust Health Rev 2011; 35: 63-69.
- 17. Christensen K, Doblhammer G, Rau R, Vaupel JW. Ageing populations: the challenges ahead. Lancet 2009; 374: 1196-1208.
- 18. Australian Bureau of Statistics. Future population growth and ageing. Australian Social Trends 4102.0 2009; March. http://www.ausstats.abs.gov.au/ausstats/subscriber.nsf/LookupAttach/4102.0Publication25.03.092/$File/41020_Populationprojections.pdf (accessed Aug 2010).
- 19. Office for National Statistics. Ageing: fastest increase in the ‘oldest old’. Newport, UK: ONS, 2009.
- 20. Administration on Aging. Projected future growth of the older population. Washington, DC: US Department of Health and Human Services, 2009.
- 21. Australian Bureau of Statistics. Regional population growth, Australia. 1994–05 to 2007–08. Canberra: ABS, 2011. (ABS Cat. No. 3218.0.)
- 22. Australian Bureau of Statistics. Census data. Canberra: ABS, 2010.
- 23. Australian Bureau of Statistics. Population projections, Australia, 2006 to 2101. Canberra: ABS, 2008. (ABS Cat. No. 3222.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/3222.0Main+Features12006%20to%202101?OpenDocument (accessed Aug 2010).
- 24. Australian Bureau of Statistics. Population by age and sex, regions of Australia, 2008. Canberra: ABS, 2009. (ABS Cat. No. 3235.0.)
- 25. Gerson LW, Shvarch L. Emergency medical service utilization by the elderly. Ann Emerg Med 1982; 11: 610-612.
- 26. McConnel CE, Wilson RW. The demand for prehospital emergency services in an aging society. Soc Sci Med 1998; 46: 1027-1031.
- 27. Rucker DW, Edwards RA, Burstin HR, et al. Patient-specific predictors of ambulance use. Ann Emerg Med 1997; 29: 484-491.
- 28. Dickinson ET, Verdile VP, Kostyun CT, Salluzzo RF. Geriatric use of emergency medical services. Ann Emerg Med 1996; 27: 199-203.
- 29. Minaker KL, Rowe J. Health and disease among the oldest old: a clinical perspective. Milbank Mem Fund Q Health Soc 1985; 63: 324-349.
- 30. Evans MDR, Kelley J. Trends in women’s labour force participation in Australia: 1984–2002. Melbourne: Melbourne University, 2004.
- 31. Joyce C, Piterman L. Trends in GP home visits. Aust Fam Physician 2008; 37: 1039-1042.
- 32. Catholic Health Australia. Survey of access to general practice services in residential aged care. Canberra: CHA, 2010.
- 33. Abernethie L, Nagree Y. Increased emergency department attendance: a qualitative investigation of health seeking behaviours. Just Policy 2004; 33: 6-16.
- 34. UK Department of Health. Taking healthcare to the patient: transforming NHS ambulance services. London: DH, 2005.
- 35. Council of Ambulance Authorities. 2008–09 annual report. Adelaide: CAA, 2009.
- 36. Munro J, Nicholl J, O’Cathain A, Knowles E. Impact of NHS direct on demand for immediate care: observational study. BMJ 2000; 321: 150-153.
- 37. Richardson DB, Mountain D. Myths versus facts in emergency department overcrowding and hospital access block. Med J Aust 2009; 190: 369-374. <MJA full text>
- 38. Cooke M, Fisher J, Dale J, et al. Reducing attendances and waits in emergency departments: a systematic review of present innovations. London: National Co-ordinating Centre for NHS Service Delivery and Organisation R&D, 2004.
- 39. Cameron PA, Joseph AP, McCarthy SM. Access block can be managed. Med J Aust 2009; 190: 364-368. <MJA full text>
- 40. Snooks H, Williams S, Crouch R, et al. NHS emergency response to 999 calls: alternatives for cases that are neither life threatening nor serious. BMJ 2002; 325: 330-333.
- 41. Snooks HA, Dale J, Hartley-Sharpe C, Halter M. On-scene alternatives for emergency ambulance crews attending patients who do not need to travel to the accident and emergency department: a review of the literature. Emerg Med J 2004; 21: 212-215.
- 42. University of Sheffield Medical Care Research Unit. Building the evidence base in pre-hospital urgent and emergency care: a review of research evidence and priorities for future research. London: UK Department of Health, 2010.





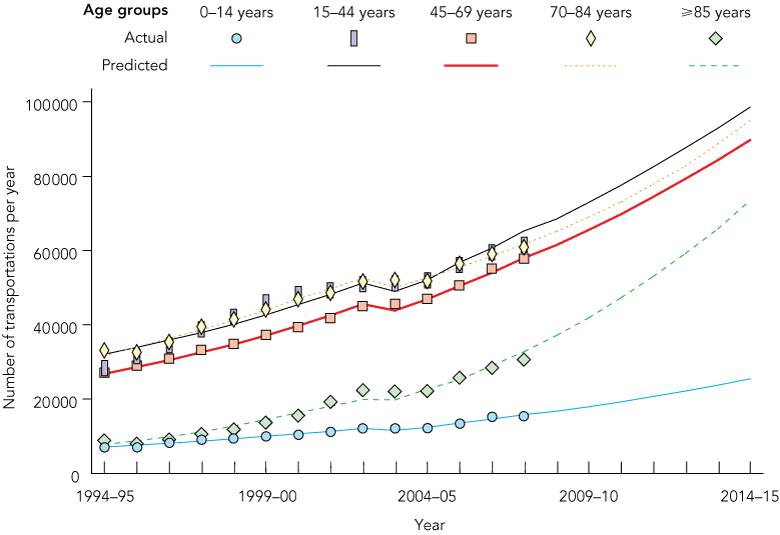
Abstract
Objective: To measure the growth in emergency ambulance use across metropolitan Melbourne since 1995, to measure the impact of population growth and ageing on these services, and to forecast demand for these services in 2015.
Design and setting: A population-based retrospective analysis of Ambulance Victoria’s metropolitan emergency ambulance transportation data for the period from financial year 1994–95 to 2007–08, and modelling of demand in the financial year 2014–15.
Main outcome measures: Numbers and rates of emergency ambulance transportations.
Results: The crude annual rate of emergency transportations across all age groups increased from 32 per 1000 people in 1994–95 to 58 per 1000 people in 2007–08. The rate of transportation for all ages increased by 75% (95% CI, 62%–89%) over the 14-year study period, representing an average annual growth rate of 4.8% (95% CI, 4.3%–5.3%) beyond that explained by demographic changes. Patients aged ≥ 85 years were eight times (incident rate ratio, 7.9 [95% CI, 7.6–8.3]) as likely to be transported than those aged 45–69 years over this period. Forecast models suggest that the number of transportations will increase by 46%–69% between 2007–08 and 2014–15, disproportionately driven by increasing usage by patients aged ≥ 85 years.
Conclusions: These findings confirm a dramatic rise in emergency transportations over the study period, beyond that expected from demographic changes. Rates increased across all age groups, but more so in older patients. In the future, such acceleration is likely to have major effects on ambulance services and acute hospital capacity. This calls for further investigation of underlying causes and alternative models of care.