Cardiac interventional procedures — including cardiac surgery, percutaneous transluminal coronary angioplasty (PTCA) and implantation of cardioverter-defibrillator devices — have been major therapeutic advances in cardiovascular medicine and have led to declining coronary heart disease case fatality rates over the past few decades.1 These therapeutic advances are affecting health services around the world;2,3 the Health, United States, 2009 report included a special section on advances in medical technology.3 The report stated that the use of medical technology has tripled in the past decade and of the top five costliest procedures, three are cardiovascular and include PTCA (a 65% increase in use with a 108% inflation-adjusted cost increase between 1999 and 2006), implantation of medical devices including cardiac pacemakers and defibrillators (up 147%), and coronary artery bypass grafting (CABG) procedures (down 24%).3
There has also been a steady increase in the volume of these procedures conducted around Australia. In 2004, the Australian Institute of Health and Welfare estimated that cardiac surgical procedures were undertaken in over 50 public and private centres in Australia.1 CABG was the most common cardiac surgical procedure, followed by replacement of the mitral and aortic valve.1
The number of PTCA procedures performed in Australian hospitals has grown steadily, and with the introduction of new technologies (particularly drug-eluting stents) the cost per procedure has also escalated. In 2006–07, the Australian Institute of Health and Welfare reported over 35 000 PTCA procedures with or without insertion of bare-metal or drug-eluting stents.4 This rapidly evolving technique has been shown to be effective at relieving symptomatic angina and improving prognosis in patients with acute coronary syndromes.
Among people aged over 75 years, there was a fourfold increase in procedures over the same period, indicating a preference by older patients and/or their doctors for percutaneous coronary intervention (PCI). Since 1997–1998, PCI has replaced CABG as the most common coronary revascularisation treatment for coronary heart disease in Australia.1 Over the past few years, there has been a dramatic increase in PCI procedures (based on hospital separations in which a PCI was performed) in Victorian public hospitals, from 3644 in the 2003–04 financial year to 4561 in 2004–05, representing a 25% increase in procedures (Daniel Borovnicar, Victorian Government Department of Human Services, personal communication, April 2006). There was a 43% increase in the total cost over the 2 years. This increase is likely driven by the establishment of new catheterisation laboratories with PCI capability, but is also due to the higher cost of drug-eluting stents, which were introduced during this period.
Furthermore, the increasing use of implantable devices has created a range of imperatives similar to those posed by therapeutic drugs. An estimated 4% of the US population has at least one implanted medical device. A series of unanticipated failures was identified after widespread clinical use, resulting in urgent and costly recalls.5 The surveillance systems for devices such as pacemakers and implantable cardioverter-defibrillators increasingly involve registries with regular patient follow-up.
In the US, the Society of Thoracic Surgeons6 and the American College of Cardiology7 have established registries with the aim of improving the quality of care and clinical outcomes for surgical and interventional procedures, respectively. Similar initiatives have been undertaken in the United Kingdom8 and Europe;9 these have led to important developments including models for risk adjustment, enabling comparisons of outcomes on a risk-adjusted basis. The necessity for registries for quality performance and safety monitoring was demonstrated following concerns about the quality of individual surgeon performance in cardiac surgery in the Bristol inquiry.10 The inquiry highlighted the need for performance benchmarking and quality assurance in high-risk procedures, such as cardiac surgery, and sparked a dramatic growth in this area.8 Similar calls for the establishment of cardiac procedural registries in Australia have been made.11,12
At around this time, the Australasian Society of Cardiac and Thoracic Surgeons (ASCTS) recognised the need for a similar system for performance monitoring to be developed and trialled in Australia; this gave rise to the ASCTS Victorian cardiac surgery database project being initiated in 1999.13 The purpose of the registry was to establish a systematic approach to cardiac surgery data collection and reporting. This enables benchmarking of performance standards across hospitals to assure quality performance and improve clinical outcomes for patients undergoing cardiac surgery procedures.
Despite initial funding for the activity in six Victorian public hospitals, it was recognised that national engagement was required for an agreed set of variables. The ASCTS established a National Dataset Committee, which reviewed existing available cardiac surgery datasets and definitions to establish a standard set of data elements for collection in Australia. It was agreed that the dataset would remain stable and be revisited every 2 years for additions and changes according to feedback. The initial dataset comprised approximately 200 variables, separated into Patient Demographics, Risk Factors, Pre-operative Cardiac Status, Previous Cardiac Interventions, Haemodynamic Data, Operation Status/Category, Procedural Details, Postoperative data and Mortality, Discharge and Readmission data.14
30-day mortality after isolated CABG;
return to operating theatre for deep sternal wound infection;
return to operating theatre for haemorrhage;
ventilation time;
length of stay in intensive care; and
total length of hospital stay.
The identification of performance outside an agreed standard was made on the basis of statistical process control charts. In recent years, additional techniques including cumulative sum (CUSUM) control charts and variable life-adjusted displays have been included in the detection of outliers and variation of outcomes between units. The committee recognised the requirement for appropriate risk adjustment and the EuroSCORE (European System for Cardiac Operative Risk Evaluation) method was chosen.9 A major objective of the project was for the validation of the EuroSCORE for risk adjustment in the Australian context and the development of an Australian risk model if required.
a public report, outlining surgical activity and performance indicators to be made available through the state government web-site for community access;
a hospital-specific report, identifying the individual hospital and its performance against other participating units; and
a comprehensive surgeons’ report, sent to all ASCTS members, providing data on surgical activity in Victoria.
Commencing in 2001, with six Victorian public hospital units and collecting data on 2791 procedures, the ASCTS database registry has grown to contain over 30 000 surgical procedures. In 2010, the performance of 21 public and private cardiac surgical units around Australia will be monitored, and participation is increasing. Box 1 illustrates the 30-day mortality and deep sternal wound infection performance indicator reporting for 18 participating hospitals for the 2008–09 financial year using control charts. Box 2 illustrates unit performance against the mean performance from the participating centres and identifies UK and US reported mean mortality rates for comparison. Similar methods for monitoring are used for each of the five performance indicators for cardiac surgery on a quarterly basis.
At this stage, an Australian risk adjustment model for 30-day mortality has been developed, and future research will focus on appropriate risk adjustment for other performance indicators, including return to theatre for sternal wound infection and haemorrhage.15
Over the past 10 years, Victorian public hospital outcomes for cardiac surgery have been closely monitored, and at no stage has any unit been identified as an outlier requiring external peer review. In recent years, we have explored a variety of alternative methods for reporting and monitoring performance of participating units, including variable adjusted life displays, CUSUM methods and funnel plots. Communicating and expressing variation in performance is a major challenge as simplistic approaches such as ranking (league tables) fail to identify a lack of variation between centres. In an analysis of 175 ranked cardiac surgeons in New York state, the confidence intervals around risk-adjusted mortality were so wide that only two could be considered in the lowest mortality quartile, and only six could be considered in the highest mortality quartile.16 The perception of a difference due to ranking in this instance is completely misleading.
In 2009, the Australian Commission for Safety and Quality in Health Care called for tenders to test and validate the operating principles and technical standards for clinical quality registries. ASCTS, in collaboration with the Melbourne Interventional Group, proposed the development of the web-based Australian Cardiac Procedures Registry (ACPR) to monitor cardiac procedural activity in surgery, PCI and device implantation.17 The concept of a modular framework capturing the “cardiac patient journey” across a variety of interventions has been supported by the Cardiac Society of Australia and New Zealand. In the first year, it has focused on establishing standardised datasets and performance indicators for each of the three areas of clinical activity (Box 3). This will enable further evaluation of the impact of care on individuals rather than the focus on procedures inherent in separate procedural registries.
1 Monitoring unit performance for cardiac surgery — 30-day mortality and deep sternal wound infection, 2008–09
A. Control chart — observed 30-day mortality 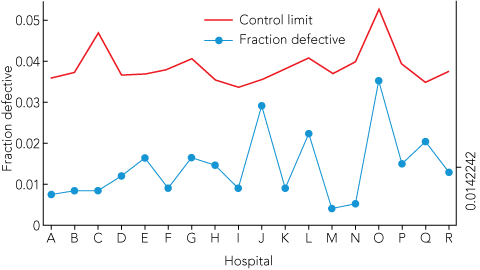 |
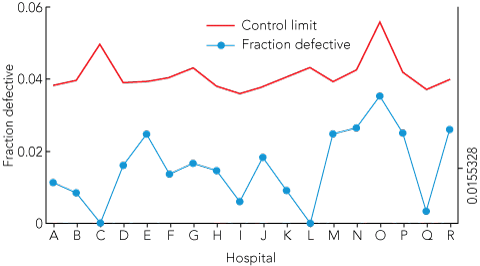 |
2 Mortality rate within 30 days following isolated coronary artery bypass grafting for the 18 hospital cardiac surgery units, 2008–09
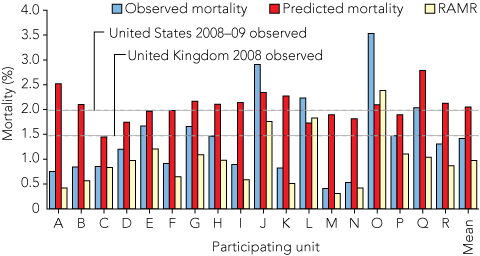 |
|
RAMR = risk-adjusted mortality rate using the AusSCORE model.15 |
3 Proposed key performance indicators for the Australian Cardiac Procedures Registry
Percutaneous coronary intervention
Mortality to 30 days
Periprocedural myocardial infarction
Target vessel failure to 30 days
Target vessel revascularisation
Stent thrombosis
Urgent inhospital coronary artery bypass grafting
Procedural success
Major bleeding inhospital
Stroke to 30 days
Door-to-balloon time
- Christopher M Reid1
- Angela L Brennan1
- Diem T Dinh1
- Baki Billah1
- Carl B Costolloe1
- Gilbert C Shardey2
- Andrew E Ajani3
- 1 Monash Centre of Cardiovascular Research & Education (CCRE) in Therapeutics, Department of Epidemiology and Preventive Medicine, School of Public Health and Preventive Medicine, Monash University, Melbourne, VIC.
- 2 Cabrini Medical Centre, Melbourne, VIC.
- 3 Royal Melbourne Hospital, Melbourne, VIC.
We acknowledge the following individuals for their contribution to the development and establishment of the ACPR:
ACPR Project Management Committee. Andrew Ajani, Barbara Anthony, Leonard Arnolda, Peter Bissaker, Alexander Black, Angela Brennan, Harriet Carruthers, Derek Chew, Carl Costolloe, Brett Dennett, Ron Dick, Diem Dinh, Stephen Duffy, Leeanne Grigg, Henry Krum, Jeff Lefkovits, Andrew MacIsaac, Leo Mahar, Steven McConchie, John McNeil, Harry Mond, Andrew Newcomb, Silvana Marasco, Al Mutazz Diqer, Chris Reid, Gil Shardey and Peter Subramaniam.
ACPR Data Definition Working Groups
Device. John Atherton, Angela Brennan, Karen Carey, Carmine De Pasquale, Diem Dinh, Henry Krum, Jo-Dee Lattimore, John McNeil, Harry Mond, Gerry O’Driscoll, Chris Reid, David Ross and Cameron Singleton.
PCI. Andrew E Ajani, Angela Brennan, David Brieger, Derek Chew, Diem Dinh, Stephen J Duffy, Christopher Hammett, Jeff Lefkovits, Andrew MacIsaac, Yuvi Malaiapan, Jamie Rankin, Chris Reid and Matt Worthly.
Cardiac Surgery. Peter Bissaker, Daniella Brasacchio, Diem Dinh, James Edwards, Clifford Hughes, David Marshman, Julie Mundy, Andrew Newcomb, Mark Newman, Gil Shardey, Peter Subramaniam and Hugh Wolfenden.
ACPR Steering Committee. Chris Reid, James Cameron, Karen Carey, Derek Chew, Niall Johnson, Larry Kelly, Leo Mahar, John McNeil, Harry Mond, John Rankin, Gil Shardey, James Tatoulis and Andrew Tonkin.
ACPR Web Development Team. Carl Costolloe, Ramya Jaganathan, Philip Scotney and Igor Yeykelis.
The ACPR was funded by the Australian Commission for Safety and Quality in Health Care (tender RFT 018/0809).
- 1. Australian Institute of Health and Welfare. Heart, stroke and vascular diseases, Australian facts 2004. Canberra: AIHW, Heart Foundation of Australia, 2004. (AIHW Cat. No. CVD 27.)
- 2. State of the heart in the USA. Lancet 2010; 375: 697.
- 3. National Center for Health Statistics. Health, United States, 2009: with special feature on medical technology. Hyattsville, Md: NCHS, 2010.
- 4. Australian Institute of Health and Welfare. Australian hospital statistics 2006–07. Canberra: AIHW, 2008. (AIHW Cat. No. HSE 55.)
- 5. Maisel WH. Medical device regulation: an introduction for the practicing physician. Ann Intern Med 2004; 140: 296-302.
- 6. Ferguson TBJ, Dziuban SW, Edwards FH, et al. The STS National Database: current changes and challenges for the new millennium. Ann Thorac Surg 2000; 69: 680-691.
- 7. Anderson HV, Shaw RE, Brindis RG, et al. A contemporary overview of percutaneous coronary interventions: the American College of Cardiology-National Cardiovascular Data Registry (ACC-NCDR). J Am Coll Cardiol 2002; 39: 1096-1103.
- 8. Keogh B, Kinsman R; Society of Cardiothoracic Surgeons of Great Britain and Ireland. 1998 National Adult Cardiac Surgical Database report. London: Society of Cardiothoracic Surgeons of Great Britain and Northern Ireland, 1999.
- 9. Roques F, Nashef SAM, Michel P, et al. Risk factors and outcome in European cardiac surgery: analysis of the EuroSCORE multinational database of 19030 patients. Eur J Cardiothorac Surg 1999; 15: 816-823.
- 10. Smith R. Regulation of doctors and the Bristol inquiry. BMJ 1998; 317: 1539-1540.
- 11. Tonkin A. Why Australia needs a cardiac procedures database. Heart Lung Circ 2001; 10 (1 Suppl): S22-S25.
- 12. Scott I. Why we need a national registry in interventional cardiology. Med J Aust 2008; 189: 223-227. <MJA full text>
- 13. Reid C, Solterbeck A, Buxton BF, et al. Developing performance indicators for cardiac surgery: a demonstration project in Victoria. Heart Lung Circ 2001; 10 (1 Suppl): S29-S33.
- 14. Australian Society of Cardiac and Thoracic Surgeons. ASCTS National Cardiac Surgery Database Program data definitions manual. Version 3. 2008. http://www.ccretherapeutics.org.au/research/ascts.html (accessed Aug 2010).
- 15. Reid C, Billah B, Dinh D, et al. An Australian risk prediction model for 30-day mortality after isolated coronary artery bypass: the AusSCORE. J Thorac Cardiovasc Surg 2009; 138: 904-910.
- 16. Jacobs JP, Cerfolio RJ, Sade RM. The ethics of transparency: publication of cardiothoracic surgical outcomes in the lay press. Ann Thorac Surg 2009; 87: 679-686.
- 17. Ajani AE, Szto G, Eccleston D, et al. The foundation and launch of the Melbourne Interventional Group: a collaborative interventional cardiology project. Heart Lung Circ 2006; 15: 44-47.





Abstract
Routine monitoring of performance in the provision of cardiac services aids quality assurance and enables comparisons of performance to national and international standards.
The Australasian Society of Cardiac and Thoracic Surgeons conducts a surgical registry that has grown from six hospitals participating in 2001 to 21 contributing in 2010.
Variation in performance is monitored on a quarterly basis through the use of control chart methodology, and a peer-review mechanism and governance process for reporting have been established.
Proposed future developments of the registry include its expansion to include interventional cardiology procedures, such as implantation of stents and cardiac devices, and a modular format, with the patient rather than the procedure being the key element of the system.
An Australian Cardiac Procedures Registry will provide information to stakeholders, including consumers, clinicians, health funders and policymakers, on performance standards and quality of care of medical services affecting an ever-increasing number of Australians.