Since 1996, Australian men and women have been entitled to subsidised osteoporosis treatments through the Pharmaceutical Benefits Scheme (PBS) if they have had a minimal trauma fracture or have radiological evidence of one or more vertebral deformities. In 2007, this subsidy was extended to include patients aged 70 years or older with bone mineral density (BMD) T-scores ≤ – 3 at either the femoral neck or lumbar spine, even in the absence of a minimal trauma fracture or vertebral deformity. Previous studies, mainly involving women, suggest that many people with osteoporosis remain untreated, even after a minimal trauma fracture.1 Men are even less likely to receive treatment for osteoporosis, although osteoporotic fractures in elderly men are associated with increased morbidity, greater functional decline, higher mortality and increased health costs compared with osteoporotic fractures in women.2,3
Areal BMD (g/cm2) of the lumbar spine (L1–L4) and right hip was measured by dual x-ray absorptiometry (DXA) using a Discovery W scanner (Hologic Inc, Bedford, Mass, USA). Coefficients of variation for scans duplicated on 30 men were 2.1% for the femoral neck and 1.6% for the lumbar spine. Anteroposterior measurements were taken of the lumbar spine for vertebrae L1–L4. T-scores of individual vertebrae as well as the total area were calculated using the United States male reference range for the lumbar spine and US National Health and Nutrition Examination Survey reference range for the hip. All participants for whom the combined area of L1–L4 or at least two lumbar vertebrae had T-scores ≤ – 34 were deemed to meet the PBS BMD criteria for subsidised osteoporosis treatment. PBS criteria differ from World Health Organization definitions of osteoporosis (T-score < – 2.5), osteopenia (T-score between – 2.5 and – 1) and normal BMD (T-score > – 1).
Vertebral deformities were ascertained from lateral spinal scans of the area between thoracic 4–5 and lumbar 4–5 vertebrae, using the instant vertebral fracture assessment (VFA) function of the DXA scanner. Two scientists who were experienced in diagnosing vertebral deformities assessed the scans visually and semi-quantitatively. A vertebral deformity was defined as a 20% or greater reduction in height of the anterior or mid portion of a vertebral body relative to the posterior height of that body, or a minimum 20% reduction in any of these heights compared with the vertebral body above or below the affected vertebral body.5
A fracture history was obtained at the baseline interview for each patient. Only fractures that had occurred in the 10 years before baseline were used in our analyses. Ten years was chosen as the cut-off time because the association between prevalent fractures and subsequent fractures wanes with time.6 Three observers (K B, V N and R G C) independently rated fractures using the description of the mechanism of injury. Fractures were classified as minimal trauma fractures if the mechanism of injury was described as a fall from standing height or less; a fall on steps or curbs (but not down steps); or a minimal trauma incident other than a fall (eg, turning over in bed or coughing). There was a high level of agreement between observers, with all kappa (κ) values being > 0.84.
Medication use was ascertained by interview, and participants were asked to bring all prescription and non-prescription medication to the clinic for verification. Use of bisphosphonates and calcium and vitamin D supplements was coded as positive if participants brought them to the clinic or reported they had ever taken them.
Awareness of osteoporosis was determined from answers to the question, “Has a doctor or health care provider ever told you that you have osteoporosis (sometimes called ‘brittle bones’)?” Falls in the previous 12 months were established at the baseline interview.
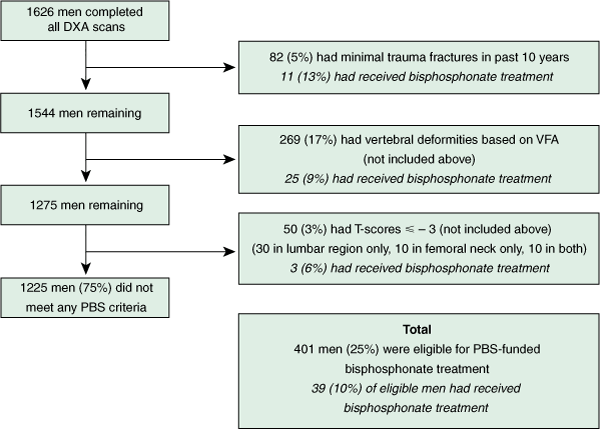
The prevalences of minimal trauma fractures, vertebral deformities and T-scores ≤ – 3 are shown in Box 1. Four hundred and one men (25%) were eligible for PBS-subsidised treatment, mainly due to the presence of vertebral deformities. Five per cent of men qualified on the basis of minimal trauma fracture, independent of BMD, and 3% qualified on the basis of low BMD in the absence of a minimal trauma fracture (Box 2). The proportion of men meeting the PBS criteria increased with age, from 21% in the 70–74-years age group to 46% in the ≥ 90-years age group (P for trend < 0.001) (Box 1). There was no significant difference in prevalence of past fractures (P = 0.4), vertebral deformities (P = 0.1) or T-scores ≤ – 3 (P = 0.2) between men recruited by invitation letter (n = 1436) and men who volunteered to be in the study before receiving a letter (n = 190).
One hundred and fifty-three men (9%) reported having at least one fracture in the previous 10 years; 82 of these fractures (76 non-vertebral and 6 vertebral) were classified as minimal trauma fractures, of which 61 (74%) occurred in the 5 years before baseline.
As some men met multiple criteria, a diagnostic flowchart was created to determine the numbers of men who met the PBS criteria and the proportional contribution of each criterion (Box 2). The flowchart shows how the men in the CHAMP study would have been identified as meeting the PBS criteria for osteoporosis treatment if they had been “screened” by first taking a history of minimal trauma fracture, then, if they did not meet this criterion, looking for evidence of a vertebral deformity and, finally, in the remaining men, measuring BMD. Two men met all three PBS criteria for osteoporosis treatment, 41 met two criteria and 358 met one criterion. Of the 401 men who met the PBS criteria for treatment, 351 (88%) did so on the basis of one or more vertebral deformities or a history of minimal trauma fracture. Fifty men (13%) met the criteria on the basis of DXA alone, with 40 of these men having T-scores ≤ – 3 in the lumbar spine.
Of the 401 men eligible for subsidised treatment under the PBS, 10% had taken, or were taking, a bisphosphonate, 14% a calcium supplement, and 7% a vitamin D supplement. Less than 1% had taken both vitamin D and calcium in conjunction with a bisphosphonate (Box 3).
Men were most likely to have taken bisphosphonates following a minimal trauma fracture (13%) and least likely if they had T-scores of ≤ – 3 with no fracture history (6%) (Box 2). Of the men who had had two or more falls and met PBS criteria, 16% had received bisphosphonate treatment, 9% had taken calcium, 7% had taken vitamin D, and none had taken the combination of bisphosphonate, calcium and vitamin D. An analysis of men who met the PBS criteria and had low BMD (T-scores < – 1) revealed similar low levels of treatment (data not shown).
Only 10% of men who met the PBS criteria reported knowing they had “osteoporosis”.
A further 45 men had taken bisphosphonates but did not meet the PBS criteria for subsidised osteoporosis treatment. Eight of these men self-reported Paget’s disease and six additional men were receiving glucocorticoid therapy. It was unclear why the remaining men were taking bisphosphonates.
Almost a quarter of the men in the CHAMP study met the PBS criteria for subsidised osteoporosis-specific treatment with bisphosphonates, but few of these men had received treatment or were aware they had osteoporosis. This lack of awareness may have resulted in substantial underestimation of osteoporosis prevalence in men in a recent report by the Australian Institute of Health and Welfare that relied on self-report of osteoporosis.7
Most men met the PBS criteria on the basis of PBS-defined vertebral deformities. Estimates of the prevalence of vertebral deformities reported in previous studies have varied widely, owing to different definitions of vertebral deformity. Out of a group of 555 men aged ≥ 60 years in the Geelong Osteoporosis Study, 10% of men aged 70–79 years and 15% of those aged 80 years or over had prevalent vertebral deformities, defined as at least 25% vertebral height reduction.8 The Dubbo Osteoporosis Epidemiology Study reported a vertebral deformity prevalence of 31% among 114 men of mean age 68.2 years.9 Other large epidemiological studies outside Australia have reported vertebral deformity prevalence rates of 13%–39% in men aged over 70 years.8,10
Identifying men with vertebral deformities is very important, as the presence of asymptomatic vertebral deformities is a strong predictor of future fracture risk,8 associated with a 19-fold increased risk of future vertebral fractures and 2.3-fold increased risk of hip fractures.11 In light of the high prevalence of vertebral deformities, our study raises the question of whether VFA scans may have a role to play in assessing osteoporosis risk. However, vertebral deformities identified by VFA scan alone do not meet the current PBS criterion for osteoporosis treatment, because the cost-effectiveness of basing treatment on the results of VFA has not been evaluated.
Very few men who met the PBS criteria for osteoporosis treatment were being treated with a bisphosphonate, calcium or vitamin D. This is consistent with other studies showing low rates of treatment for osteoporosis, even in people who are seen in hospital after minimal trauma fractures.1,12,13 Low treatment levels persist, despite evidence that treatment with bisphosphonates reduces vertebral and non-vertebral fractures in men.14 It should be noted that all bisphosphonate trials include calcium and vitamin D supplements as part of the treatment, yet few men in the CHAMP study had taken these supplements in conjunction with a bisphosphonate.
Identifying men who will benefit from osteoporosis treatment and increasing the proportion of eligible men receiving appropriate treatment is a public health issue. Both non-pharmacological treatments (falls prevention, physical activity, calcium and vitamin D supplementation) and pharmacological treatments need to be implemented to reduce fracture rates. Currently it is projected that, because of the ageing population, hip fractures may double by 2026 and increase fourfold by 2051.15 After a hip fracture, men are less likely than women to return to their homes or mobilise independently.16 Additionally, they have markedly higher mortality rates than women after all major fractures.17
The CHAMP study is one of the largest studies of osteoporosis in elderly men ever conducted in Australia. The participation rate of about 50% is similar to other studies of the very elderly requiring detailed physical assessments. Men in the CHAMP study are representative of men in the study area in terms of age and ethnicity18 and have similar health characteristics to older men in the nationally representative MATeS study.19 Nevertheless, it is likely that frailer men in poor health would have been less likely to have participated in our study, resulting in an underestimation of the prevalence of fractures and of low BMD.
The PBS requires vertebral deformities to be determined by radiographs, rather than VFA, as used in this study. VFA scans agree well with lateral spinal radiographs (96.3% agreement; κ = 0.79), and the sensitivity and specificity of VFA are both greater than 90%.20 However, VFA is better at detecting fractures with more than 25% height reduction, and may miss milder deformities or deformities in the upper thoracic spine, resulting in under-reporting of vertebral deformities.21
A weakness of our study was that minimal trauma fractures were self-reported rather than validated with radiological evidence, as is required to obtain PBS funding. In a European study of men aged over 70 years, self-reported fractures had a false positive rate of 11% and an under-reporting rate of 14%.22
1 Number (%) of participants who met PBS 2007 criteria for subsidised osteoporosis treatment, by age group*
Received 28 January 2010, accepted 29 June 2010
- Kerrin Bleicher1
- Vasi Naganathan2
- Robert G Cumming3
- Markus J Seibel4
- Philip N Sambrook5
- Fiona M Blyth2
- David G Le Couteur2
- David J Handelsman4
- Louise M Waite2
- Helen M Creasey2
- 1 Faculty of Medicine, University of Sydney, Sydney, NSW.
- 2 Centre for Education and Research on Ageing, University of Sydney, Concord Hospital, Sydney, NSW.
- 3 School of Public Health, University of Sydney, Sydney, NSW.
- 4 ANZAC Research Institute, University of Sydney, Concord Hospital, Sydney, NSW.
- 5 Institute of Bone and Joint Research, University of Sydney, Royal North Shore Hospital, Sydney, NSW.
The CHAMP study is funded by the National Health and Medical Research Council and the Ageing and Alzheimer’s Research Foundation (AARF). Kerrin Bleicher’s doctoral research is supported by an AARF scholarship. We would like to thank scientists Lynley Robinson and Beverly White for assessing the scans for vertebral deformities.
Markus Seibel is a member of advisory boards for Merck Sharp and Dohme, Novartis, Amgen and Sanofi-Aventis, and has received funding from these companies for institutional research. Philip Sambrook is a member of advisory boards for Merck Sharp and Dohme, Novartis, Amgen, Sanofi-Aventis and Servier, and has received speaker fees from these companies.
- 1. Kelly AM, Clooney M, Kerr D, et al. When continuity of care breaks down: a systems failure in identification of osteoporosis risk in older patients treated for minimal trauma fractures. Med J Aust 2008; 188: 389-391. <MJA full text>
- 2. Gennari L, Bilezikian JP. Osteoporosis in men. Endocrinol Metab Clin North Am 2007; 36: 399-419.
- 3. Bass E, French DD, Bradham DD, et al. Risk-adjusted mortality rates of elderly veterans with hip fractures. Ann Epidemiol 2007; 17: 514-519.
- 4. Hansen KE, Vallarta-Ast N, Krueger D, et al. Use of the lowest vertebral body T-score to diagnose lumbar osteoporosis in men: is “cherry picking” appropriate? J Clin Densitom 2004; 7: 376-381.
- 5. Donohoo E, editor. MIMS Bi-monthly. 4th ed. Sydney: CMP Medica Australia, 2006: 196-197.
- 6. Schousboe JT, Fink HA, Lui LY, et al. Association between prior non-spine non-hip fractures or prevalent radiographic vertebral deformities known to be at least 10 years old and incident hip fracture. J Bone Miner Res 2006; 21: 1557-1564.
- 7. Australian Institute of Health and Welfare. Arthritis and musculoskeletal conditions in Australia 2005: with a focus on osteoarthritis, rheumatoid arthritis and osteoporosis. Canberra: AIHW, 2005. (AIHW Cat. No. PHE 67.) http://www.aihw.gov.au/publications/phe/amca05/amca05.pdf (accessed May 2010).
- 8. Pasco J, Henry M, Korn S, et al. Morphometric vertebral fractures of the lower thoracic and lumbar spine, physical function and quality of life in men. Osteoporos Int 2009; 20: 787-792.
- 9. Pongchaiyakul C, Nguyen ND, Jones G, et al. Asymptomatic vertebral deformity as a major risk factor for subsequent fractures and mortality: a long-term prospective study. J Bone Miner Res 2005; 20: 1349-1355.
- 10. O’Neill TW, Felsenberg D, Varlow J, et al. The prevalence of vertebral deformity in European men and women: the European Vertebral Osteoporosis Study. J Bone Miner Res 1996; 11: 1010-1018.
- 11. Klotzbuecher CM, Ross PD, Landsman PB, et al. Patients with prior fractures have an increased risk of future fractures: a summary of the literature and statistical synthesis. J Bone Miner Res 2000; 15: 721-739.
- 12. Port L, Center J, Briffa NK, et al. Osteoporotic fracture: missed opportunity for intervention. Osteoporos Int 2003; 14: 780-784.
- 13. Teede HJ, Jayasuriya IA, Gilfillan CP. Fracture prevention strategies in patients presenting to Australian hospitals with minimal-trauma fractures: a major treatment gap. Intern Med J 2007; 37: 674-679.
- 14. Boonen S, Orwoll ES, Wenderoth D, et al. Once-weekly risedronate in men with osteoporosis: results of a 2-year, placebo-controlled, double-blind, multicenter study. J Bone Miner Res 2009; 24: 719-725.
- 15. Sanders KM, Nicholson GC, Ugoni AM, et al. Health burden of hip and other fractures in Australia beyond 2000. Projections based on the Geelong Osteoporosis Study. Med J Aust 1999; 170: 467-470. <MJA full text>
- 16. Holt G, Smith R, Duncan K, et al. Gender differences in epidemiology and outcome after hip fracture: evidence from the Scottish Hip Fracture Audit. J Bone Joint Surg Br 2008; 90: 480-483.
- 17. Bliuc D, Nguyen ND, Milch VE, et al. Mortality risk associated with low-trauma osteoporotic fracture and subsequent fracture in men and women. JAMA 2009; 301: 513-521.
- 18. Cumming RG, Handelsman D, Seibel MJ, et al. Cohort profile: the Concord Health and Ageing in Men Project (CHAMP). Int J Epidemiol 2009; 38: 374-378.
- 19. Holden C, McLachlan R, Pitts M. Men in Australia Telephone Survey (MATeS): a national survey of the reproductive health and concerns of middle-aged and older Australian men. Lancet 2005; 366: 218-224.
- 20. Ferrar L, Jiang G, Eastell R, et al. Visual identification of vertebral fractures in osteoporosis using morphometric x-ray absorptiometry. J Bone Miner Res 2003; 18: 933-938.
- 21. Fuerst T, Wu C, Genant HK, et al. Evaluation of vertebral fracture assessment by dual x-ray absorptiometry in a multicenter setting. Osteoporos Int 2009; 20: 1199-1205.
- 22. Ismail AA, O’Neill TW, Cockerill W, et al. Validity of self-report of fractures: results from a prospective study in men and women across Europe. European Prospective Osteoporosis Study Group. Osteoporos Int 2000; 11: 248-254.





Abstract
Objective: To determine the proportion of older Australian men who meet the Pharmaceutical Benefits Scheme (PBS) criteria for osteoporosis treatment and are receiving effective treatment.
Design and setting: A population-based, cross-sectional analysis of the baseline phase of the Concord Health and Ageing in Men Project (CHAMP), a large epidemiological study focusing on the health of older men. Data were collected through questionnaires and clinical assessments. Bone mineral density (BMD) of the hip and spine was measured by dual x-ray absorptiometry (DXA). Vertebral deformities were identified from DXA lateral vertebral fracture assessment images. The study was conducted at Concord Hospital, Sydney, between January 2005 and May 2007.
Participants: 1705 community-dwelling men aged 70 years or over from a defined geographical region around Concord Hospital.
Main outcome measures: Prevalence of vertebral deformities; previous minimal trauma fractures; BMD T-scores ≤ – 3; falls in the previous 12 months; use of bisphosphonates and calcium and vitamin D supplements.
Results: Of the 1705 men seen at baseline, 1626 completed all DXA scans and 401 (25%) met one or more of the PBS criteria for osteoporosis treatment. Ninety per cent of the men who met the PBS criteria were unaware they had osteoporosis. Of the men eligible for PBS-subsidised treatment, 39 (10%) reported use of a bisphosphonate, 56 (14%) had taken calcium supplements, and 28 (7%) had taken vitamin D supplements. Only three men had taken calcium, vitamin D and bisphosphonates in combination.
Conclusions: Despite a high prevalence of osteoporosis in elderly Australian men, awareness, diagnosis and treatment of the condition remain very low.