Ovarian cancer, the sixth most common cause of cancer death among Australian women,1 has a poor prognosis, mainly because about 75% of cancers are diagnosed at an advanced stage when treatment is unlikely to be curative.2 The symptoms of ovarian cancer are often non-specific,3,4 and delays in diagnosis may, in part, explain why the disease has so often spread beyond the ovaries at diagnosis.5 Anecdotally, there is a perception that the journey from first presentation to diagnosis is often long and circuitous for women with ovarian cancer.
Few international and no Australian studies have attempted to formally document the diagnostic experience of women with ovarian cancer.5-7 While some have endeavoured to estimate diagnostic delays, estimates of time from first presentation to diagnosis are varied, with British and Swedish studies reporting that most women are diagnosed within 1 month,6,8,9 while others from the United States5 and Norway7 found that 40%–45% of women experienced delays of 3 or more months. As health system differences between countries probably explain some of this variation, it is important for Australian clinicians and policymakers to have access to information from the Australian setting.
The Australian Ovarian Cancer Study was an Australia-wide population-based study. Eligible participants were women aged 18–79 years with suspected invasive or borderline epithelial ovarian, fallopian tube or primary peritoneal cancer who were identified between January 2002 and June 2005 through gynaecological oncology units and state-based cancer registries.10 A total of 3550 women were identified; of these, 307 (8.6%) died before contact could be made, 194 (5.5%) could not be contacted, and the treating doctor refused contact with 133 (3.7%). A further 171 (4.8%) were excluded because they could not complete the questionnaires in English (70), could not give informed consent (35) or were too sick (66). The remaining 2745 women were invited to participate (most before surgery) and, of these, 2319 (84% of those approached) agreed to take part. After surgery, a further 634 women were excluded: 608 because their final diagnosis was not epithelial ovarian cancer, 25 because their cancer was diagnosed before the study period, and one because she was not an Australian resident.
Characteristics of the 1463 women are shown in Box 1. Overall, 145 women (10%) reported that their cancer was diagnosed incidentally, most often at a routine check-up (50%) or when consulting for another condition (41%). These women were excluded from further analyses.
The remaining 1318 women presented to a doctor with one or more symptoms (mean, 1.9). The most common symptoms were abdominal fullness (44%) and abdominal or pelvic pain (41%) (Box 2).
While some women reported making many visits to multiple doctors before being diagnosed with cancer, this was the exception (Box 3). Of the 1318 women, 116 (9%) were told they (probably) had ovarian cancer by the first doctor they consulted, while most women were given their diagnosis by either the second (578, 44%) or third (430, 33%) doctor they saw. Only 78 women (6%) reported seeing five or more different doctors before their cancer was diagnosed.
In terms of numbers of consultations, a third of the women received a diagnosis by their second consultation, almost two-thirds were diagnosed within three consultations, and three-quarters by the fourth consultation (Box 3). Only 55 women (4%) reported making more than eight visits to one or more doctors for the same symptoms before being diagnosed.
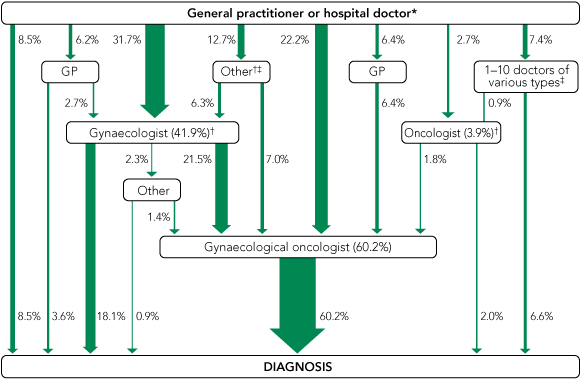
Box 4 summarises the diagnostic pathways of the women, and Box 5 shows the proportions who saw various types of doctors at some stage before diagnosis; one in five saw a specialist outside the fields of gynaecology and oncology. Ultimately, most women received their cancer diagnosis from a gynaecological oncologist (60%) or a gynaecologist (18%).
The interval between first presentation and cancer diagnosis ranged from 0 to 155 months, although 66% of cancers were diagnosed in ≤ 1 month and 80% within 3 months (Box 6). Only 153 cancers (11.6%) were not diagnosed within 6 months.
Box 7 shows that factors significantly associated with a delay of more than 6 months included living in remote areas of Australia (odds ratio [OR], 4.6; 95% CI, 1.7–12.2 v metropolitan areas); annual household income below $45 000 (OR, 1.6; 95% CI, 1.0–2.6); the number of doctors consulted (OR, 7.0; 95% CI, 3.1–15.7 for five or more v one); and presentation with multiple symptoms (OR, 1.6; 95% CI, 1.0–2.5), abdominal pain (OR, 1.7; 95% CI, 1.1–2.5) or bowel symptoms (OR, 1.8; 95% CI, 1.1–2.9). Longer symptom duration (≥ 1 month) was associated with more rapid diagnosis after presentation (OR, 0.4; 95% CI, 0.2–0.6 v < 1 month).
To our knowledge, this is the first study to describe in detail the diagnostic pathways experienced by women with ovarian cancer in Australia. Our results with respect to time to diagnosis are in close accord with another Australian study that found that 70% of women with ovarian cancer were diagnosed within 3 months of first experiencing symptoms.11
We found a strong association between residing in a remote area of Australia and being diagnosed more than 6 months after presentation, although the number of women involved was small. Women from remote areas may have poorer access to primary care services12 and make fewer visits to GPs and specialists than women living in urban areas.13 Access inequalities may also explain why women with lower incomes were more likely to have longer diagnostic delays than women with higher incomes, as evidence suggests that, in Australia, all else being equal, those with higher incomes are more likely to consult a specialist than those with a lower income.14
We also found that the number, type and duration of symptoms a woman presented with were associated with whether she was diagnosed more than 6 months after presentation. These findings largely concur with other studies that have investigated determinants of diagnostic delay in patients with ovarian cancer.5,7,15 Clinicians faced with a woman presenting with several non-gynaecological symptoms probably consider more common diagnoses associated with those symptoms in the first instance, thus potentially delaying diagnosis. However, we did not have information directly from medical practitioners and thus cannot provide insights into how doctors make clinical judgements when faced with the complex symptoms and signs associated with ovarian cancer.
3 Number of different doctors seen and total number of visits for the same symptoms before diagnosis (n = 1318)
Received 22 October 2009, accepted 28 April 2010
- Susan J Jordan1,2
- Jane E Francis3
- Anne E Nelson3
- Helen M Zorbas3
- Karen A Luxford3
- Penelope M Webb2
- 1 School of Population Health, University of Queensland, Brisbane, QLD.
- 2 Queensland Institute of Medical Research, Brisbane, QLD.
- 3 National Breast and Ovarian Cancer Centre, Sydney, NSW.
These analyses were funded by the National Breast and Ovarian Cancer Centre. The Australian Ovarian Cancer Study was supported by the US Army Medical Research and Materiel Command under DAMD17-01-1-0729, the Cancer Council Tasmania and the Cancer Foundation of Western Australia; the Australian Cancer Study was supported by the National Health and Medical Research Council (NHMRC) of Australia (199600). Susan Jordan is supported by a Postdoctoral Public Health Training Fellowship and Penelope Webb by a Research Fellowship from the NHMRC.
None identified.
- 1. Australian Institute of Health and Welfare. Cancer in Australia: an overview, 2008. Canberra: AIHW, 2008.
- 2. Marsden DE, Friedlander M, Hacker NF. Current management of epithelial ovarian carcinoma: a review. Semin Surg Oncol 2000; 19: 11-19.
- 3. Webb PM, Purdie DM, Grover S, et al. Symptoms and diagnosis of borderline, early and advanced epithelial ovarian cancer. Gynecol Oncol 2004; 92: 232-239.
- 4. Goff BA, Mandel LS, Melancon CH, Muntz HG. Frequency of symptoms of ovarian cancer in women presenting to primary care clinics. JAMA 2004; 291: 2705-2712.
- 5. Goff BA, Mandel L, Muntz HG, Melancon CH. Ovarian carcinoma diagnosis. Cancer 2000; 89: 2068-2075.
- 6. Thulesius HO, Lindgren AC, Olsson HL, Hakansson A. Diagnosis and prognosis of breast and ovarian cancer — a population-based study of 234 women. Acta Oncol 2004; 43: 175-181.
- 7. Paulsen T, Kaern J, Kjaerheim K, et al. Symptoms and referral of women with epithelial ovarian tumors. Int J Gynaecol Obstet 2005; 88: 31-37.
- 8. Kirwan JM, Tincello DG, Herod JJ, et al. Effect of delays in primary care referral on survival of women with epithelial ovarian cancer: retrospective audit. BMJ 2002; 324: 148-151.
- 9. Flam F, Einhorn N, Sjövall K. Symptomatology of ovarian cancer. Eur J Obstet Gynecol Reprod Biol 1988; 27: 53-57.
- 10. Merritt MA, Green AC, Nagle CM, Webb PM. Talcum powder, chronic pelvic inflammation and NSAIDs in relation to risk of epithelial ovarian cancer. Int J Cancer 2008; 122: 170-176.
- 11. Lataifeh I, Marsden DE, Robertson G, et al. Presenting symptoms of epithelial ovarian cancer. Aust N Z J Obstet Gynaecol 2005; 45: 211-214.
- 12. Young AF, Dobson AJ, Byles JE. Determinants of general practitioner use among women in Australia. Soc Sci Med 2001; 53: 1641-1651.
- 13. Brown WJ, Young AF, Byles JE. Tyranny of distance? The health of mid-age women living in five geographical areas of Australia. Aust J Rural Health 1999; 7: 148-154.
- 14. Van Doorslaer E, Clarke P, Savage E, Hall J. Horizontal inequities in Australia’s mixed public/private health care system. Health Policy 2008; 86: 97-108.
- 15. Ryerson AB, Eheman C, Burton J, et al. Symptoms, diagnoses, and time to key diagnostic procedures among older US women with ovarian cancer. Obstet Gynecol 2007; 109: 1053-1061.





Abstract
Objective: To describe the diagnostic pathways experienced by a large, representative group of Australian women with ovarian cancer, and to document the time between first presentation to a medical professional and clinical diagnosis.
Design, setting and participants: 1463 women with epithelial ovarian cancer from an Australia-wide population-based study (2002–2005) completed a telephone interview in which they described the events that led to the diagnosis of their cancer.
Main outcome measures: Number and type of doctors consulted, investigations performed, referral patterns and the time from first presentation to diagnosis.
Results: Of the 1463 women, 145 had their cancer diagnosed incidentally and were excluded from analysis. Most of the remaining 1318 women (1222, 93%) presented first to their general practitioner. As a result of their first medical consultation, 75 women (6%) were given a diagnosis, and 484 (37%) were referred to a gynaecologist, gynaecological oncologist or oncologist for further assessment. Overall, 85% of women visited three or fewer doctors before their cancer was diagnosed; 66% of cancers were diagnosed within 1 month of the initial presentation, and 80% were diagnosed within 3 months. For 12% of women, the diagnostic process took longer than 6 months; this was more likely for women residing in remote Australia, those with lower incomes, and those presenting with abdominal pain or bowel symptoms, or with more than one symptom.
Conclusions: Despite anecdotal suggestions to the contrary, most women with ovarian cancer in Australia are investigated and diagnosed promptly. The diagnostic process is more protracted for a minority of women, and the factors we found to be associated with diagnostic delay warrant further investigation.