The GP Super Clinics Program is a federally funded program that uses an independent, competitive invitation-to-apply process to select preferred candidates based on which proposal best meets the local health needs and the objectives outlined in the GP Super Clinics Program Invitation to Apply.1 Some of these include: “well integrated multidisciplinary patient centred care”, “support for preventive care”, “high quality best practice care” and “efficient and effective use of Information Technology”.1
Local population health statistics (Box 1, Box 2) were used to determine appropriate geographical locations, local health issues and local use of the Medicare Benefits Schedule.2-4 Together, these rapid qualitative and quantitative approaches identified the following problems:
a high burden of prevalent chronic disease; and
a workforce deficit, and underuse of available Medicare items for screening, assessment and planning.
Qualitative data obtained during stakeholder interviews are summarised below.
To guide our involvement in the GP Super Clinics Program, we have developed a set of key objectives (Box 3).
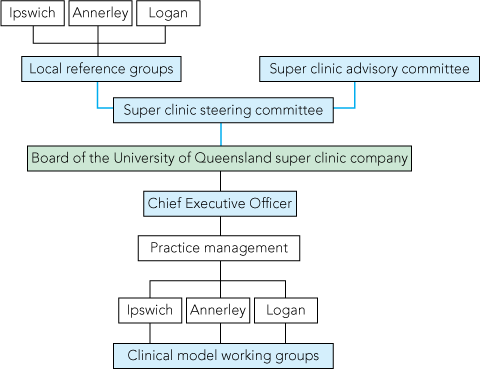
The diagram in Box 4 outlines the governance structure for the UQ GP super clinics. In short, there are local reference groups, a broad university-funded steering committee, and a university-funded super clinic advisory group that informs clinical, educational and research initiatives. UQ has also funded a 0.6 full-time-equivalent position of Director of GP Super Clinics to facilitate the development of the program. The clinics will operate on a mixed-billing business model, with GPs remunerated on a percentage of billing, not by salaries.
Our clinical-service and business models focus on enhancing the capacity of local general practices. Data show that most patients are highly satisfied with their “usual GP”.5 However, GPs often need to rely on other specialist medical and non-medical staff to facilitate optimal care for their patients. Likewise, many GPs develop specialised skills in an area of interest — so-called GPs with special interests or GPs with advanced skills. Within multidoctor practices, GPs occasionally refer patients to their colleagues who have additional skills in a particular area (eg, mental health, skin cancer medicine, women’s health). In ideal scenarios, these GPs would be supported by specialist colleagues who provide advice and patient consultations as required. This practice occurs, often, on an informal basis.
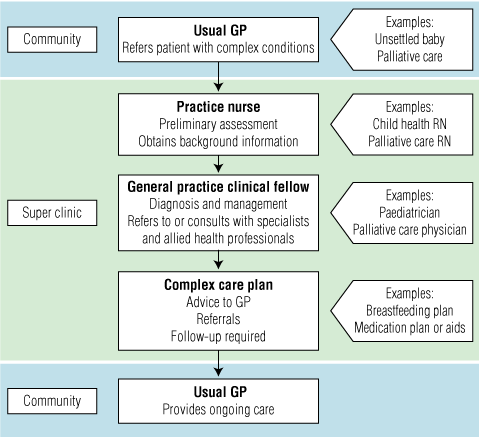
Our model, based in part on this experience, uses practice nurses, GPs with advanced skills, specialists and allied health professionals to manage patients with complex problems and to formalise this practice on a regional basis. Local GPs are encouraged to work sessions in their areas of special interest, and to develop locally appropriate clinical pathways based on available evidence and resources. These GPs will either hold, or be assisted to obtain, advanced qualifications in this area of special interest. This approach enhances the capacity of the local region, improves timely and appropriate access to specialised advice in an appropriate community-based location, addresses significant and emerging workforce pressures, and recognises the valuable role of “generalist” and “specialist” GPs in managing complex patient types. The model is illustrated in Box 5.
Having hospital-based clinical pharmacists as part of a collaborative team has been shown to improve patient safety and appropriate prescribing.6 However, community-based pharmacist support for GPs has been lacking,7 with schemes such as the home medicines review program having been underused, perhaps as a result of a lack of access or awareness. Yet, our stakeholder feedback suggested that many GPs would value appropriate and timely advice from pharmacists, especially when managing patients with complex conditions. At UQ, we developed a model for an extended-capability pharmacy and sought commercial providers to commit to providing this service in our Ipswich, Logan and Annerley sites. The Annerley GP super clinic site, based in the Pharmacy Australia Centre of Excellence, is adjacent to the University’s School of Pharmacy. These pharmacies will be involved in collaborative advanced medication management programs for patients with chronic diseases.
1 Indicators of health status in two University of Queensland GP super clinic localities compared with Queensland and with Australia as a whole2-4
No. per 1000 inhabitants or % (as shown) |
|||||||||||||||
2 Access to and use of health care services in two University of Queensland GP super clinic localities compared with Australia as a whole
3 University of Queensland GP super clinic objectives
Develop and assess the effectiveness of patient-centred, multidisciplinary clinical models for community management of patients who have chronic disease and/or risk factors for chronic disease. These models must:
Be financially sustainable;
Deliver quality, evidence-based chronic disease management services;
Empower patients to self-manage their chronic diseases.
Develop, trial and evaluate new health professional roles for primary health care, recognising the value of all health professionals and their particular skill sets.
Develop e-health solutions which enhance the capability of primary health care to:
Integrate patient care across the continuum of health services;
Enhance local health professionals’ capabilities to manage chronic disease;
Enhance patients’ capabilities to manage their own health care;
Evaluate the impact of chronic disease management strategies in terms of clinical outcomes, cost-benefit analysis and quality of life.
Develop vital and previously neglected community-based education opportunities for health professional students, which incorporate private health services (general practitioners and private hospitals) and provide vertical and horizontal integration of training opportunities.
Develop and implement community-based, primary health care research strategies focusing on the prevention and management of chronic diseases and associated lifestyle risk factors.
Share this knowledge through appropriate forums, and actively participate in the development of new models of primary health care.
- Jared M Dart1
- Claire L Jackson2
- Helen J Chenery3
- Paul N Shaw4
- David Wilkinson5
- Faculty of Health Sciences, University of Queensland, Ipswich, QLD.
Jared Dart is the sole Director of iHealth Solutions Pty Ltd, which was contracted to develop the super clinic proposal for the Redcliffe Hospital Foundation (Redcliffe super clinic, August 2008) and the UQ (Ipswich and Brisbane Southside super clinics, January to June 2009).
- 1. Australian Government Department of Health and Ageing. GP super clinics national program guide. Canberra: The Department, 2008. http://www.health.gov.au/internet/main/publishing.nsf/Content/pacd-gpsuperclincs-programguide (accessed Jun 2010).
- 2. Medicare Australia. Statistics. Divisions of general practice statistics reports [database on the internet]. Canberra: Medicare Australia, 2009. https://www.medicareaustralia.gov.au/statistics/div_gen_prac.shtml (accessed Jun 2010).
- 3. Population Health Information Development Unit. Population health profile for Divisions of General Practice: supplement. Report No. 74a. Adelaide: Public Health Information Development Unit, 2007; Mar.
- 4. Population Health Information Development Unit. Population health profile for Divisions of General Practice. Report No. 74. Adelaide: Public Health Information Development Unit, 2005; Nov.
- 5. Allan J, Schattner P, Stocks N, Ramsay E. Does patient satisfaction of general practice change over a decade? BMC Family Practice 2009; 10: 13.
- 6. Nissen L. Current status of pharmacist influences on prescribing of medicines. Am J Health Syst Pharm 2009; 66 Suppl 3: S29-S34.
- 7. Ackerman E, Williams ID, Freeman C. Pharmacists in general practice — a proposed role in the multidisciplinary team. Aust Fam Physician 2010; 39: 163-164.





Abstract
The GP Super Clinics Program is a highly topical and controversial initiative with varying levels of support within the policy, consumer and health care communities.
Here, we describe the GP super clinic initiative of the University of Queensland (UQ), and how it aims to enhance primary-care capacity in the regions where clinics are based.
The UQ GP super clinic model has considered the concerns of general practitioners, patients and other stakeholders, and addresses the needs of these groups while providing an excellent opportunity for the university to be involved in innovative service delivery, community-based education, primary-care service design and evaluation.