Anatomy of the human body has been taught to medical students by dissection of embalmed, donated cadavers for centuries.1 Until recent decades, this has been a rite of passage for medical students, delivering fundamental regional, relational and topographical anatomical knowledge,2 together with tactile gnosis (ie, what various human tissues feel like)3 and dissection heuristics (ie, tissue-handling techniques).4 It has also helped junior medical students deal with issues surrounding death.5
However, over the past several decades, despite the protestations of many, the teaching of anatomy by dissection has gradually decreased.6-9 As more and more essential educational material has been packed into medical school curricula, time-consuming anatomical dissection has fallen by the wayside. This has led to a wide variation in the amount of anatomy taught at Australian and New Zealand medical schools.2,10
The surgical community and other clinicians associated with the University of Sydney soon became very concerned, as the lack of anatomical knowledge of students reaching the clinical years made the teaching of clinical medicine and surgery generally very difficult.8 Student surveys in 1998, 1999 and 2006 revealed widespread dissatisfaction with anatomy teaching (University of Sydney, Faculty of Medicine: preparation for hospital practice questionnaire results, 1998 and 1999; and University of Sydney Medical Program Year 3 curriculum survey, 2006).
A review of the University of Sydney Medical Program was undertaken in 2007.11 Following representations from numerous individuals and groups, including students, the review report recommended the “strengthening” of anatomy teaching. This led to a trebling of the total hours of anatomy teaching in Medicine 1 and 2 (the first 2 years of the graduate medical program) from 50.5 to 152.5 hours (since expanded to 170.5 hours) (Deborah Bryce, Senior Lecturer, Discipline of Anatomy and Histology, University of Sydney, personal communication).
The course was first conducted in 2009, when it was very favourably evaluated by the Office of Medical Education of the University of Sydney.12 This article analyses the results of the 2010 course.
Acceptance of students into the elective “Anatomy by whole body dissection” course was on a first-come-first-served basis, with a maximum of 32 places offered. The dissection course was based on the classical Cunningham’s manual of practical anatomy, volumes 1 to 3.13 Dissection schedules were drawn up in colour-coded spreadsheet form to cover each of the 34 days of dissection. Each day’s schedule listed the area to be dissected, the required prereading of the texts, and the dissection tasks to be carried out that day, clearly outlined. The actual dissection instructions were transcribed onto laminated colour-coded cards. All diagrams in the manuals were projected and displayed on four large central console screens. Surgical-quality instruments were provided so that dissection could be carried out at a rapid pace in this intense full-time course.
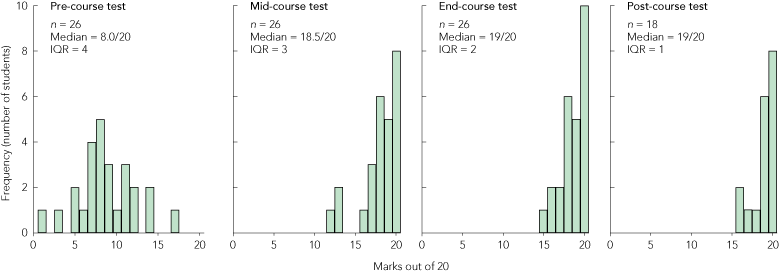
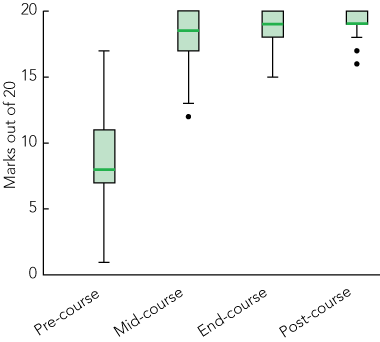
In 2010, 29 students participated in the course. Three students of the 29 enrolled in this course did not attend the pre-course assessment and were excluded from our analysis. All 26 students who participated in the pre-course assessment also took part in the mid-course and end-course assessments. Eighteen of these students took part in the post-course assessment 1 month after the end of the dissection course. The histograms in Box 1 show the distribution of marks (out of a maximum of 20) scored in each assessment. The median pre-course assessment score was 8/20 (IQR, 4) and the subsequent median test scores were 18.5/20 (IQR, 3), 19/20 (IQR, 2) and 19/20 (IQR, 1) in the mid-course, end-course and post-course assessments, respectively. These test scores are also represented in Box 2, which shows the median test scores plus the IQR for each of the four assessment time points as well as minimum and maximum values and outliers.
teaching methods, resources and supervision;
dissection manuals, projected images and laminated instructions;
teaching by surgical trainees and supervisors;
frequent practical assessments; and
teaching anatomy by dissection within a clinical context.
methodical dissection leading to the acquisition of anatomical knowledge with an appreciation of relations between structures (22);
the development of a three-dimensional mind map of the various anatomical regions (8);
anatomical information being put in a clinical context by demonstrators and supervisors (15); and
the presence of supervisors teaching clinical anatomy in their area of expertise to small groups (14).
Students found the least favourable features of the course to be:
Opinion on the importance of gross topographical human anatomy in medical education ranges from those who believe it is the basis of all medical knowledge14 to those who feel that such anatomical knowledge is superfluous. There is abundant evidence that medical students appreciate that a good basic knowledge of human anatomy is essential to safe and sound medical practice, even if this is not fully appreciated by some of the writers of their respective curricula.15
The universal approval of this anatomy dissection course by the participants, together with their recommendation that it should be available to all students, indicates a perception that anatomical instruction is currently deficient and that dissection should be reintroduced to some degree into the regular medical curriculum. This consideration is supported by a number of commentators.15-18 It must be acknowledged that these students were highly motivated and their enthusiasm may not be shared by all of their peers. The strong approval of the course would indicate that it is a time-effective way to impart clinical anatomical knowledge in the shortened 4-year modern medical curriculum — a conclusion supported by others.19,20
The concept of the three-dimensional relational mind map of the regions of the human body is not new (Norman Eizenberg, Professor, Department of Anatomy and Developmental Biology, Monash University. Melbourne, personal communication). However, many students remarked that this concept, best imparted by anatomical dissection, produced a clarity of understanding of regional relational anatomy not appreciated before.19,21
The poor performance of this cohort of students in the pre-course assessment was a matter of concern, especially as all members of the group were just 12 months away from provisional registration as medical practitioners. Only nine of the 26 students managed to correctly answer at least half of the 20 questions asked (ie, reached a 50% pass mark). Almost 25% of the total answers were considered to be answers of concern, indicating a perfunctory knowledge of gross human anatomy. This occurred despite the fact that this was a group of students expressing an interest in anatomy, with a majority considering a surgical career. It must be noted that this cohort of students had not been fully exposed to the “strengthened” anatomy course recommended by the 2007 review of the University of Sydney Medical Program.11
There are a number of reports in the medical literature of patient misadventure due to inadequate anatomical knowledge, many involving damage to adjacent structures.22-25 The medicolegal aspect of such errors makes the question of how much anatomical knowledge is necessary for safe medical practice of great importance. With the recorded wide variation in the amount and standard of anatomical instruction currently practised in Australian and New Zealand medical schools,2,10 there is an apparent need for the introduction of a standard basic national curriculum in gross human anatomy.26 Such a curriculum has been formulated for North America.14 The new curriculum should include dissection anatomy as a significant component and have a barrier assessment (ie, an assessment that halts progress in the course until satisfactorily completed). This would ensure that medical graduates have a reasonable knowledge of gross human anatomy and are equipped to properly understand the amazingly complex biological structure with which most of them will be intimately concerned throughout the rest of their professional careers.
After our experience with this dissection course, we agree with a recent United Kingdom report that:
[A]natomy should remain a principal component of medical education, with dissection as its core teaching method. Further collaboration between surgeons and anatomists should strengthen a naturally close and mutually beneficial relationship.17
1 Dissection course: test histograms for pre-course, mid-course, end-course and post-course assessments
 |
- George Ramsey-Stewart1
- Annette W Burgess2,3
- David A Hill3
- 1 Discipline of Anatomy and Histology, University of Sydney, Sydney, NSW.
- 2 Central Clinical School, Royal Prince Alfred Hospital, Sydney, NSW.
- 3 Sydney Medical School, University of Sydney, Sydney, NSW.
Dr Georgina Luscombe, Adjunct Lecturer, University of Sydney, kindly carried out the statistical evaluations. We wish to thank Associate Professor Kevin Keay, Head of the Discipline of Anatomy and Histology, University of Sydney, for his support. We are indebted to surgical colleagues and other procedural specialists who, together with surgical trainees, gave generously of their time to make the course possible. Lastly, the course would not have been possible without the support of Marcus Robinson, Senior Technical Officer, Anatomy Technical and Teaching Support Unit, University of Sydney, and his dedicated technical staff.
None identified.
- 1. Magee R. Art macabre: resurrectionists and anatomists. ANZ J Surg 2001; 71; 377-380 .
- 2. Parker LM. What’s wrong with the dead body? Use of the human cadaver in medical education. Med J Aust 2002; 176: 74-76. <MJA full text>
- 3. Thompson RVS. Art macabre: is anatomy necessary [letter]? ANZ J Surg 2001; 71: 779.
- 4. Patkin M. Surgical heuristics. ANZ J Surg 2008; 78: 1065-1069.
- 5. Parker LM. Anatomical dissection: why are we cutting it out? Dissection in undergraduate teaching. ANZ J Surg 2002; 72: 910-912.
- 6. Taylor TKF. Art macabre: is anatomy necessary [letter]? ANZ J Surg 2001 ; 71: 780-781.
- 7. Bogduk N. Art macabre: is anatomy necessary [letter]? ANZ J Surg 2001; 71: 782.
- 8. Bokey L, Chapuis P. Art macabre: is anatomy necessary [letter]? ANZ J Surg 2001; 71: 781.
- 9. Fahrer M. Art macabre: is anatomy necessary [letter]? ANZ J Surg 2001; 71: 783-784.
- 10. Craig S, Tait N, Boers D, McAndrew D. Review of anatomy education in Australian and New Zealand medical schools. ANZ J Surg 2010; 80: 212-216.
- 11. Goulston K, Oates K. Review of the University of Sydney Medical Program. October 2007. Sydney: University of Sydney, 2007. www.medfac.usyd.edu.au/forstaff/usydmp-review (accessed Oct 2010).
- 12. Jeffery HE, Klein L, Garlan K. Anatomy dissection elective: report and evaluation. Sydney: Office of Medical Education, University of Sydney, 2009.
- 13. Romanes GJ, editor. Cunningham’s manual of practical anatomy. 15th ed. Oxford: Oxford University Press, 1986.
- 14. Educational Affairs Committee of the American Association of Clinical Anatomists. A clinical anatomy curriculum for the medical student of the 21st century: gross anatomy. Clin Anat 1996; 9: 71-99.
- 15. Xu B. Traditional anatomy teaching and problem-based learning: is there a middle way? ANZ J Surg 2008; 78: 6.
- 16. Isull PJ, Kejriwal R, Blyth P. Surgical inclination and anatomy teaching at the University of Auckland. ANZ J Surg 2006; 76: 1056-1059.
- 17. Gogalniceanu P, Palman J, Madani H, et al. Traditional undergraduate anatomy education — a contemporary taboo. ANZ J Surg 2010; 80: 6-7.
- 18. Gogalniceanu P, O’Connor EF, Raftery A. Undergraduate anatomy teaching in the UK. Bull R Coll Surg Engl 2009; 91: 102-106.
- 19. Peck D, Skandalakis JE. The anatomy of teaching and the teaching of anatomy. Am Surg 2004; 70: 366-368.
- 20. Seyfer AE, Welling D, Fox JP. The value of surgeons teaching anatomy to first-year medical students. Bull Am Coll Surg 2007; 92: 8-14.
- 21. Fahrer M. Art macabre: is anatomy necessary [editorial]? ANZ J Surg 2001; 71: 333-334.
- 22. Ellis H. Medico-legal consequences in surgery due to inadequate training in anatomy [editorial]. Int J Clin Skills 2007; 1: 8-9.
- 23. Goodwin H. Litigation and surgical practice in the UK. Br J Surg 2000; 87: 977-979.
- 24. Ellis H. Medico-legal litigation and its links with surgical anatomy. Surgery 2002; 20: 1-2.
- 25. Sugand K, Abrahams P, Khurana A.The anatomy of anatomy: a review for its modernization. Anat Sci Educ 2010; 3: 83-93.
- 26. Chapuis P, Fahrer M, Eizenberg N, et al. Should there be a national core curriculum for anatomy [editorial]? ANZ J Surg 2010; 80: 475-477.





Abstract
Objective: To evaluate the 2010 “Anatomy by whole body dissection” course, a 7-week elective course offered to senior medical students at the University of Sydney at the end of their third year.
Design, setting and participants: In the 2010 course, 29 students divided into eight groups carried out whole-body dissections on eight cadavers over a 34-day period. Surgical trainees acted as demonstrators, and surgeons and anatomists as supervisors. The students were assessed by practical tests involving the identification of 20 tagged structures in four wet specimens before, during, at the end of, and 1 month after the course. In addition, students were asked to complete an anonymous feedback questionnaire about the course.
Main outcome measure: Acquisition of topographical anatomical knowledge, and student feedback on the usefulness of the course.
Results: A significant increase in topographical clinical anatomical knowledge was demonstrated among the participants and was maintained in the short term. The median pre-course assessment score was 8/20 (interquartile range [IQR], 4) and the median post-course assessment score was 19/20 (IQR, 1). This difference was statistically significant (P < 0.001). All students rated the course as “very good”, and unanimously recommended that the course be available to all students as part of the medical curriculum.
Conclusion: Students’ knowledge of anatomy improved significantly between the pre-course and post-course assessments, and all students rated the course very favourably. This supports our view that dissection anatomy should be an integral component of medical education.