Induced abortion has been increasingly practised by doctors in Australia since the late 1960s.1-3 Until the early 1990s, when medical abortion using mifepristone became available, induced abortion was performed using surgical techniques. However, mifepristone came under tight restrictions with the passage of the “Harradine amendment” to the Therapeutic Goods Act 1989 (Cwlth) in 1996.4,5 The overturning of the Harradine amendment in 2006 enabled mifepristone to be imported into and used in Australia6 but, to date, no drug company has applied to the Therapeutic Goods Administration to market the drug in Australia. About 80 medical practitioners are currently licensed to import and use mifepristone for the purpose of abortion in their own practices under the Authorised Prescriber legislation of the Therapeutic Goods Act.7
Although induced abortion forms part of the normal practice of most specialist obstetricians and gynaecologists in the United Kingdom, and many in the United States and Europe, this is thought to be less the case among Australian specialists.8-10 No formal survey of the abortion practice of Australian specialist obstetricians and gynaecologists has previously been undertaken, and there are few overseas studies in the literature.8-12 Given the importance of specialist input into women’s reproductive health, we conducted a survey of the opinions on and practice of abortion among Australian specialist obstetricians and gynaecologists.
The term “induced abortion” was used to cover termination of pregnancy using either surgical or medical methods as defined in the guidelines for induced abortion of the Royal College of Obstetricians and Gynaecologists in the UK.8 “Early” abortion was defined as up to and including 13 weeks of pregnancy; abortion up to this gestation is generally performed by surgical methods in current Australian practice. “Late” abortion was defined as abortion after 13 weeks’ gestation; in Australia, the majority of abortions at gestations greater than 13 weeks are performed by medical methods.
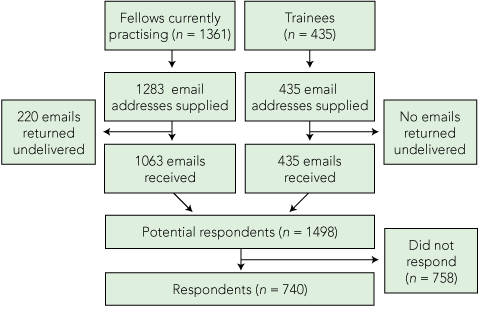
Practising Australian Fellows of the RANZCOG who had supplied the College with an email address (1283/1361; 94.3%) and all 435 Australian trainees (who are required to supply an email address for registration) were sent an email outlining the purpose of the survey and inviting them to participate by clicking on a link which enabled them (on one occasion only) to anonymously complete the questionnaire (Box 1). A reminder email was sent 3 weeks later, inviting those who had not yet completed the survey to do so.
A total of 220 emails were returned from Fellows as undeliverable, leaving 1498 potential respondents (Box 1). From these, 740 responses were received (response rate of 49.4% for those successfully emailed). There were 583 Fellows and 142 trainees, and 15 did not identify as either. Age groups and sex of respondents are shown in Box 2.
Questions 5 to 9, regarding practice of induced abortion, were answered only by the 632 respondents who stated that they did not hold views that would make them totally opposed to abortion, and some chose not to answer one or more questions. Five-hundred and seventeen respondents (81.8% of those not opposed) believed that the provision of induced abortion should be part of general obstetric and gynaecological practice (Box 3). Of these 517 respondents, 505 (97.7%) stated that the practice of abortion should be part of the curriculum for RANZCOG trainees. Five hundred and sixty (88.6%) of those not holding views making them totally opposed to abortion believed abortion should be available in the public health system throughout Australia. However, some of these respondents commented that the currently oversubscribed public operating lists should not be used for surgical abortions, and that these should be provided in dedicated clinics within the public system, as in the UK.
Details of abortion practice are shown in Box 3. Abortion formed part of the usual practice of 463 (73.3%) of those not opposed to abortion. Notably, 204 respondents reported that they perform abortion only for severe fetal abnormality or serious maternal medical conditions — this corresponds to 44.1% of those who stated that they do perform abortions, and to 32.3% of those not opposed to abortion. The proportions of respondents who reported performing abortions for public and private patients were consistent with the numbers who reported practising in these sectors. Seventeen respondents stated that they were willing to perform abortions but did not do so because of limited hospital access. The questionnaire design did not allow us to determine the total number of respondents who do not currently perform abortion purely because of their practice circumstances. Fifteen others said that they practised in small communities and, although they did not hold views making them totally opposed to abortion, they did not want to become “the abortion doctor” in such a centre, partly because of the increased workload and partly because of possible social stigma for themselves or their families. Several respondents strongly made the point that they would not accept fees for performing abortion, including one who wrote, “I donate the fee to charity so that I feel I am doing a needed procedure”.
This electronic survey elicited responses from only 49.4% of those successfully emailed, so that the views of more than half of the Fellows and trainees of the RANZCOG remain unknown. However, the demographics of the respondents were consistent with the age, sex and practice patterns of the College Fellowship as reported in the most recent RANZCOG workforce survey.13 This study is only the second electronic survey emailed to RANZCOG Fellows and trainees using the College database. The first elicited a response rate of only 16%,14 so increasing familiarity with the process might lead to higher response rates to future surveys. Initially, a number of email recipients expressed concerns about the legitimacy of a survey dealing with abortion and contacted us directly. We attempted to allay these concerns by sending the second (reminder) email with electronic signatures to all email addresses, and by giving verbal assurances to those who contacted us.
There are few overseas studies comparable to ours. A 1989 UK survey of 396 consultant gynaecologists showed that 73% “agreed with a woman’s right to choose” — only slightly lower than among the general population. Abortions up to 12 weeks’ gestation were performed by 75% of respondents, but 20% of these did not do so after 12 weeks’ gestation, and only 10% would do so after 20 weeks (this survey antedated the wide availability of medical abortion in the UK).9
1 Flow diagram of participation of Australian Fellows and specialist trainees of the RANZCOG in the survey
 |
|
RANZCOG = Royal Australian and New Zealand College of Obstetricians and Gynaecologists. |
3 Responses to survey questions 5–7 from respondents who stated they did not hold religious or conscientious views that would make them totally opposed to abortion (n = 632)
Received 4 October 2009, accepted 18 February 2010
- Caroline M de Costa1
- Darren B Russell2
- Michael Carrette3
- 1 Department of Obstetrics and Gynaecology, James Cook University School of Medicine, Cairns Campus, Cairns, QLD.
- 2 Cairns Base Hospital, Cairns, QLD.
- 3 Cairns Private Hospital, Cairns, QLD.
We are grateful to all our colleagues who took the time to complete the survey. We also thank Ms Hilary Waugh and the staff of the Teaching and Development Unit, James Cook University, for their invaluable assistance in conducting the survey.
None identified.
- 1. Victorian Law Reform Commission. Law of abortion: final report. Melbourne: Victorian Government Printer, 2008: 144-147.
- 2. de Crespigny LJ, Savulescu J. Abortion: time to clarify Australia’s confusing laws. Med J Aust 2004; 181: 201-203. <MJA full text>
- 3. Taskforce on Women and the Criminal Code. Women and the criminal code [report]. Brisbane: Queensland Government, 2002. http://www.women.qld.gov.au/resources/criminal-code/ (accessed Aug 2009).
- 4. Healy DL, Fraser H. The anti-progesterones are coming — induced menses, abortion, and labour? BMJ 1985; 290: 580-581.
- 5. Hansard, Australian Senate. Debates. Therapeutic Goods Amendment Bill 1996 (No. 2). 8 May 1996. http://www.aph.gov.au/hansard/senate/dailys/ds080596.pdf (accessed Oct 2009).
- 6. Zinn C. Health minister is stripped of his right to veto use of abortion pill. BMJ 2006; 332: 441.
- 7. Therapeutic Goods Administration. Access to unapproved therapeutic goods — authorised prescribers. Canberra: TGA, 2004. http://www.tga.gov.au/docs/html/authpres.htm#ap (accessed Sep 2009).
- 8. Royal College of Obstetricians and Gynaecologists Guideline Development Group. The care of women requesting induced abortion. Evidence-based clinical guideline no. 7. London: RCOG, 2004.
- 9. Savage W, Francome C. Gynaecologists’ attitudes to abortion. Lancet 1989; 2: 1323-1324.
- 10. Sparrow MJ. A woman’s choice. Aust N Z J Obstet Gynaecol 2004; 44: 88-92.
- 11. Francome C, Savage WD. Gynaecologists’ abortion practice. Br J Obstet Gynaecol 1992; 99: 153-157.
- 12. American Congress of Obstetricians and Gynecologists. ACOG patient education: special precedures. Induced abortion. http://www.acog.org/publications/patient_education/bp043.cfm (accessed Aug 2009).
- 13. Bell R. The 2003 RANZCOG workforce survey. O&G Magazine 2003; 5: 174-178.
- 14. Ellwood D. What do our readers think of ANZJOG? Aust N Z J Obstet Gynaecol 2009; 49: 343.





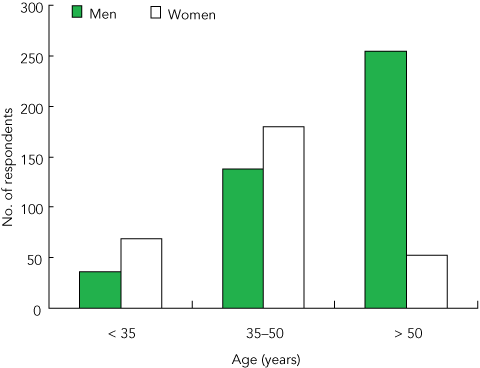
Abstract
Objective: To determine the opinions and current practice of obstetricians and gynaecologists and trainees in the specialty with regard to induced abortion.
Design, setting and participants: A voluntary, anonymous survey of Australian Fellows and specialist trainees of the Royal Australian and New Zealand College of Obstetricians and Gynaecologists was conducted between 23 June and 31 July 2009 using an email invitation to proceed to an online questionnaire.
Main outcome measures: Attitudes to abortion; self-reported usual practice of induced abortion.
Results: Of 1498 Fellows and trainees invited to complete the questionnaire, 740 (49%) did so. Of these respondents, 632 (85%) stated that they did not hold religious or conscientious views that would make them totally opposed to abortion; 463 of these (73%) reported performing abortion as part of their personal practice, with 204 (44%) doing so only for severe fetal abnormality or serious maternal medical conditions. 108 respondents reported holding views that made them totally opposed to abortion — 60 (56%) opposed it in any situation at all and 48 (44%) opposed it with limited exceptions. Of those opposed, 34 (32%) added comment that they perform abortion for severe fetal abnormality or serious maternal medical conditions, and a further 17 (16%) commented that they refer women requesting abortion in these circumstances to colleagues. Of the respondents not opposed to abortion, 89% supported the availability of induced abortion within the public health system, and half felt that national availability of mifepristone would modify their practice of induced abortion.
Conclusions: There was broad support among responding specialist obstetricians and gynaecologists and trainees for the availability of induced abortion in Australia. This study highlights the difficulties of accurately reporting a wide range of views on a contentious issue.