1 Glossary
Price-elasticity: The extent to which consumption changes in response to price changes.
Cross-price elasticity: The change in consumption per unit change in the price of other products.
Income elasticity: The change in consumption per unit of change in income.
Consumer benefit: The difference between the value an individual places on a product and the price paid for the product.
Deadweight loss of taxation: The reduction in consumer benefit from taxation that increases the price and lowers consumption, less the taxation revenue collected.
In 2008, Australians aged 15 years and over consumed, on average, the equivalent of 9.95 L of pure ethanol per person.1 To reduce the lifetime risk from alcohol-related harm, National Health and Medical Research Council (NHMRC) guidelines recommend consuming no more than two standard drinks per day for both sexes, and, to reduce the risk on a single occasion of drinking, consuming no more than four standard drinks for both sexes.2 In 2007, 60.8% of the population drank at levels considered to pose low risk of harm in the short and long term, while 10.3% and 20.4% drank at levels considered risky in the short and long term, respectively.3 The social cost of alcohol consumption in the 2004–05 financial year was estimated at $15.3 billion, second to the cost of tobacco and almost double the cost of illicit drugs ($8.2 billion).4 Alcohol-related harm accounted for 3.2% of the total burden of disease and injury in Australia in 2003, equating to 3430 deaths and 85 435 disability-adjusted life-years (DALYs).5
A strategy to reduce alcohol-related harm is to reduce the average consumption of alcohol across the population.6 Evidence suggests that increasing the price of alcohol (usually via taxation) reduces consumption: a meta-analysis of 112 studies, comprising 1003 estimates of price-elasticity (see glossary, Box 1), found a significant negative relationship between alcohol price increases and consumption.7
In Australia, the United States and United Kingdom, excise taxes vary according to beverage type.8-10 In Australia, beer is taxed according to alcohol content above a 1.15% tax-free threshold, spirits are taxed at a higher rate, and wine is taxed as a percentage of the wholesale price. In contrast, a volumetric tax would apply the same rate of tax per litre of alcohol across all beverages.11 Increased taxes are generally passed on to consumers in the form of higher alcohol prices. This loss of consumer benefit (Box 1) may be partially offset by the redistribution of the additional taxation revenue as welfare and other government spending. However, the amount of tax collected and redistributed is likely to be substantially less than the loss in consumer benefit, a difference termed “deadweight loss” of taxation.
The tax rates calculated for the three scenarios were:
$28.61 per litre of pure alcohol to maintain the current deadweight loss; this was calculated by varying the tax rate continuously until the deadweight loss equalled that of the current tax system;
$24.81 per litre of pure alcohol to maintain the current level of taxation revenue; and
$57.97 per litre of pure alcohol to be consistent with the current tax rate applied to spirits.
We obtained published estimates of price elasticity for beer, wine and spirits.12 As no estimates were available for ready-to-drink (RTD) alcoholic beverages, their price elasticity was assumed to equal that of straight spirits. The only significant cross-price elasticity (the extent to which consumption of one beverage changes in response to price changes of another beverage) was a negative relationship between the price of beer and the consumption of spirits (raising beer prices reduces an individual’s budget to purchase spirits).11
Uncertainty in the net effect on alcohol consumption of implementing a volumetric tax was assumed to be normally distributed, with a standard error plus or minus 20% of the point estimate. The change in alcohol consumption was reduced by 3% per annum, which is the estimated growth in gross domestic product in Australia13 multiplied by an income elasticity of 1 (Box 1), to account for real growth in income.12
The cost to government of implementing a volumetric tax in Australia has been estimated at $18 million.14 To take account of the uncertainty of this estimate, we assumed that the cost varied between $14.4 million and $21.6 million. Reduction in future health expenditure (cost offsets) from the prevention of future disease and future complications was calculated in this model using data from the Australian Burden of Disease study5 and the Disease Costs and Impacts Studies.15 All costs were adjusted to the 2003 reference year using the consumer price index for health.16
A multistate life table model17 was used to measure the health benefits derived from implementing a volumetric tax in Australia. This model captured short-term and long-term consequences of reduced alcohol consumption using both disease and injury models. Diseases included ischaemic heart disease, ischaemic stroke, breast cancer, mouth and oropharyngeal cancer, oesophageal cancer, liver cancer, laryngeal cancer, hypertensive heart disease, cardiomyopathy, gallbladder and bile duct disease, pancreatitis, cirrhosis and alcohol use disorders. Injuries included road traffic accidents, falls, fires, burns and scalds, drowning, machinery accidents, suffocation and foreign bodies, suicide and self-inflicted injuries, and homicide and violence.
Epidemiological inputs to the disease models were taken from the Australian Burden of Disease study, including projected trends in incidence and case fatality.5 Trends were assumed to continue over the next 20 years, with disease rates remaining constant thereafter.
The average disability associated with each disease was taken from estimates of prevalence and severity-weighted years lived with disability for each disease.5 The relative risks for each disease and data sources are shown in Box 2. The change in relative risk of each disease was calculated from the change in alcohol consumption by assuming a linear increase (or decrease) in disease risk with increasing (or decreasing) alcohol consumption. This is a method of interpolating between the relative risks reported in the literature to capture the change in risk arising from a change in consumption.
The relationship between relative risk of mortality or disability from injury and alcohol consumption was assumed to be exponential. Exponential coefficients were estimated for each injury from direct estimates of the proportion of injuries attributed to alcohol5 and data on the prevalence of alcohol use in the Australian population.3 Total health gains are reported in disability-adjusted life-years (DALYs) averted — a single measure that accounts for both increases in years of life as well as gains in health.
A volumetric tax rate with no change in current deadweight loss results is predicted to result in a 2.77% reduction in annual consumption of pure alcohol and an estimated annual increase in taxation revenue of $492 million (Box 3). In this scenario, the price of spirits and RTD beverages decreased and the price of beer and wine increased. The increased consumption of spirits was more than offset by reduced consumption of beer and wine. A tax revenue-neutral scenario also increased the price of beer and wine and decreased the price of spirits and RTD beverages, but resulted in only a marginal decrease (0.05%) in overall alcohol consumption. A volumetric tax set equal to the current spirits tax rate provided a substantially greater reduction (23.85%) in consumption of alcohol and an increase in taxation revenue of $3094 million.
The cost of changing the taxation system for alcohol is estimated at $18 million, or an annualised equivalent of $0.58 million. There is evidence that all three scenarios of volumetric taxation would reduce health costs and increase health gains compared with current policy. The net health gain associated with a deadweight loss-neutral tax change is estimated at 21 000 DALYs averted, and the net cost as – $110 million per annum (Box 4). The tax revenue-neutral scenario provides a much smaller health gain of 380 DALYs and net cost of – $1.4 million. A volumetric tax rate equal to that of the current spirits excise provides the greatest health gain of 170 000 DALYs and net cost of – $870 million.
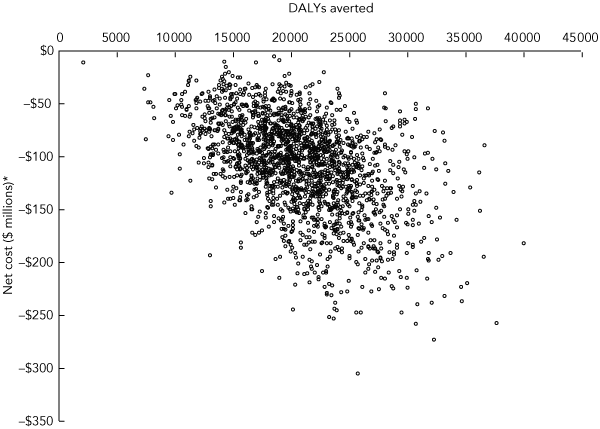
The cost-effectiveness plane for a deadweight loss-neutral volumetric tax is shown in Box 5. Each point represents one of the 2000 simulated results calculated to represent uncertainty around inputs to the model. The x axis measures the DALYs averted by the intervention, and the y axis measures the net cost of the intervention (a negative value on the y axis indicates a cost saving). The graph shows that all estimates have a y value less than 0 and an x value greater than 0, indicating that the intervention is cost-saving and associated with a health gain.
Second, we used estimates of price elasticity for beer, wine and spirits that date from 1994,11 and were unable to obtain an estimate for ready-to-drink (pre-mixed) beverages, so assumed it was equal to that of spirits. In addition, our model assumed that the type of alcoholic beverage consumed does not affect drinking-risk behaviour, but rather that the pure alcohol content is solely responsible. Our failure to account for the alcohol density of beverages and the rate at which people become intoxicated could have resulted in an overestimate of the potential health gains of an equalised volumetric tax.
Furthermore, both the negative and positive health effects of alcohol consumption were modelled, but the positive effects are debated.22 Thus, the health effects reported here might underestimate the full health impact of reduced alcohol consumption.
Evidence from the WHO-CHOICE study14 suggests that the most efficient public health response to the burden of alcohol misuse depends on the prevalence of alcohol use. Taxation represented the most cost-effective response in countries such as Australia with moderate or high levels of drinking. Our results indicate that the method of alcohol taxation is important in efficiently reducing the harm caused by alcohol use. An equalised volumetric alcohol tax is a cost-effective policy that would deliver significant health gains compared with existing taxation in Australia, which applies inconsistent rates per litre of pure alcohol.
However, in prioritising interventions, we need to combine technical approaches, such as economic evaluation, with approaches that facilitate due process.23 Other criteria often considered in evaluating health interventions include the capacity of the intervention to reduce inequity, acceptability to stakeholders, feasibility, sustainability, and potential for other consequences. Aspects of these criteria to consider before implementing volumetric taxation are shown in Box 6. These issues might have positive and negative effects on its acceptability. For example, a volumetric tax might be considered equitable in that the more individuals drink, the more they are taxed, but this approach might also be opposed by alcohol lobby groups, especially those in sectors whose sales are predicted to decline.
Systems are already in place to implement and monitor volumetric alcohol taxation and, once implemented, minimal resources would be needed to ensure its sustainability. The recent change in tax rates applied to pre-mixed alcoholic drinks highlights the Australian government’s motivation to adopt evidence-based policy.24,25 However, the vocal opposition from the alcohol industry demonstrates the political hurdles to such reform. In particular, a volumetric taxation system has the potential to create winners and losers within the alcohol industry — although spirits producers would potentially welcome the system, the beer and wine sectors are likely to oppose a relative tax increase on their products.
2 Relative risks of alcohol-related diseases at different intake levels (with abstinence as the reference value)18
3 Estimated changes in quantity of pure alcohol consumed and taxation revenue achieved by volumetric taxation
* Change in first year after new tax regime. † Per annum. ‡ Change in total pure alcohol is equal to [(total pure alcohol before tax change — total pure alcohol after tax change) ÷ total pure alcohol before tax change]. The total pure alcohol change is equal to the sum of change in pure alcohol for each alcoholic beverage category weighted by its proportion of total pure alcohol. |
|||||||||||||||
5 Cost-effectiveness plane of a deadweight loss-neutral scenario of volumetric taxation
 |
|
DALY = disability-adjusted life-year. * 2003 Australian dollars. |
6 Further criteria to consider before implementing volumetric alcohol taxation
The burden of intervention (amount paid) will be proportional to the amount of alcohol consumed.
Low-income drinkers will be more affected (tax-to-income ratio is greater).
The intervention is low-cost and will generate significant offsets.
Alcohol lobby groups (or companies) are likely to oppose the decision (as they may lose revenue), which may influence government policy.
The political scenario and perceived acceptance by voters will be other determinants for acceptability among politicians.
A section of the health-conscious population may accept volumetric taxation, whereas alcohol consumers may object to paying more for alcohol.
Received 30 June 2009, accepted 28 September 2009
- Joshua M Byrnes1
- Linda J Cobiac2
- Christopher M Doran1
- Theo Vos2
- Anthony P Shakeshaft1
- 1 National Drug and Alcohol Research Centre, University of New South Wales, Sydney, NSW.
- 2 Centre for Burden of Disease and Cost-Effectiveness, School of Population Health, University of Queensland, Brisbane, QLD.
Our research was funded by an Alcohol Education and Rehabilitation Foundation grant.
The funding body had no role in study design, data collection, analysis and interpretation or writing of this article.
- 1. Australian Bureau of Statistics. Apparent consumption of alcohol, Australia, 2007–08. Canberra: ABS, 2009. (ABS Cat. No. 4307.0.55.001.)
- 2. National Health and Medical Research Council. Australian guidelines to reduce health risks from drinking alcohol. Canberra: NHMRC, 2009.
- 3. Australian Institute of Health and Welfare. 2007 national drug strategy household survey: detailed findings. Canberra: AIHW, 2008. (AIHW Cat. No. PHE 107.)
- 4. Collins DJ, Lapsley HM. The costs of tobacco, alcohol and illicit drug abuse to Australian society in 2004/05. Canberra: Commonwealth of Australia, 2008.
- 5. Begg S, Vos T, Barker B, et al. The burden of disease and injury in Australia 2003. Canberra: Australian Institute of Health and Welfare, 2007. (AIHW Cat. No. PHE 82.)
- 6. Rose G, Daly S. The population mean predicts the number of deviant individuals. BMJ 1990; 301: 1031-1034.
- 7. Wagenaar AC, Salois MJ, Komro KA. Effects of beverage alcohol price and tax levels on drinking: a meta-analysis of 1003 estimates from 112 studies. Addiction 2009; 104: 179-190.
- 8. Australian Taxation Office. The alcohol industry — excise technical guidelines. Canberra: ATO, 2006. (Cat. No. NAT 14790-04.2006.)
- 9. European Commission. Excise duty tables: part I — alcoholic beverages. Brussels: European Commission, 2009. http://ec.europa.eu/taxation_customs/index_en.htm# (accessed Aug 2009).
- 10. Alcohol and Tobacco Tax and Trade Bureau. Taxes: tax and fee rate. Washington: US Department of the Treasury. http://www.ttb.gov/tax_audit/atftaxes.shtml#Beer (accessed Sep 2008).
- 11. Richardson J, Crowley S. Optimum alcohol taxation: balancing consumption and external costs. Health Econ 1994; 3: 73-87.
- 12. Clements KW, Selvanathan S. The economic determinants of alcohol consumption. Aust J Agric Econ 1991; 35: 209-231.
- 13. Productivity Commission. Economic implications of an ageing Australia. Research report. Canberra: The Commission, 1995.
- 14. Chisholm D, Rehm J, Van Ommeren M, Monteiro M. Reducing the global burden of hazardous alcohol use: a comparative cost-effectiveness analysis. J Stud Alcohol 2004; 65: 782-793.
- 15. Australian Institute of Health and Welfare. Health system expenditure on disease and injury in Australia, 2000–01. Canberra: AIHW, 2004. (AIHW Cat. No. HWE 26.)
- 16. Australian Bureau of Statistics. Consumer price index. Canberra: ABS, 2003. (ABS Cat. No. 6401.)
- 17. Barendregt JJ, Van Oortmarssen GJ, Van Hout BA, et al. Coping with multiple morbidity in a life table. Math Popul Stud 1998; 7: 29-49.
- 18. Cobiac LJ, Vos T, Doran C, Wallace A. Cost-effectiveness of interventions to prevent alcohol-related disease and injury in Australia. Addiction 2010; 104: 1646-1655.
- 19. Corrao G, Rubbiati L, Bagnardi V, et al. Alcohol and coronary heart disease: a meta-analysis. Addiction 2000; 95: 1505-1523.
- 20. Ridolfo B, Stevenson C. The quantification of drug-caused mortality and morbidity in Australia, 1998. Canberra: Australian Institute of Health and Welfare, 2001. (AIHW Cat. No. PHE 29. Drug Statistics Series No. 7.)
- 21. English DR, Holman CD, Milne E, et al. The quantification of drug cause morbidity and mortality in Australia. Canberra: Commonwealth Department of Human Services and Health, 1995.
- 22. Stockwell T, Chikritzhs T, Bostrom A, et al. Alcohol-caused mortality in Australia and Canada: scenario analyses using different assumptions about cardiac benefit. J Stud Alcohol Drugs 2007; 68: 345-352.
- 23. Carter R, Vos T, Moodie M, et al. Priority setting in health: origins, description and application of the Australian Assessing Cost-Effectiveness initiative. Expert Rev Pharmacoecon Outcomes Res 2008; 8: 593-617.
- 24. Doran C, Shakeshaft A. What price for public health: using taxes to curb drinking in Australia. Lancet 2008; 372: 701-703.
- 25. Shakeshaft A, Doran CM, Byrnes J. The role of research in the failure of the alcopops excise in Australia: what have we learned? Med J Aust 2009; 191: 223-225. <MJA full text>





Abstract
Objective: To estimate the potential health benefits and cost savings of an alcohol tax rate that applies equally to all alcoholic beverages based on their alcohol content (volumetric tax) and to compare the cost savings with the cost of implementation.
Design and setting: Mathematical modelling of three scenarios of volumetric alcohol taxation for the population of Australia: (i) no change in deadweight loss, (ii) no change in tax revenue, and (iii) all alcoholic beverages taxed at the same rate as spirits.
Main outcome measures: Estimated change in alcohol consumption, tax revenue and health benefit.
Results: The estimated cost of changing to a volumetric tax rate is $18 million. A volumetric tax that is deadweight loss-neutral would increase the cost of beer and wine and reduce the cost of spirits, resulting in an estimated annual increase in taxation revenue of $492 million and a 2.77% reduction in annual consumption of pure alcohol. The estimated net health gain would be 21 000 disability-adjusted life-years (DALYs), with potential cost offsets of $110 million per annum. A tax revenue-neutral scenario would result in an 0.05% decrease in consumption, and a tax on all alcohol at a spirits rate would reduce consumption by 23.85% and increase revenue by $3094 million. All volumetric tax scenarios would provide greater health benefits and cost savings to the health sector than the existing taxation system, based on current understandings of alcohol-related health effects.
Conclusions: An equalised volumetric tax that would reduce beer and wine consumption while increasing the consumption of spirits would need to be approached with caution. Further research is required to examine whether alcohol-related health effects vary by type of alcoholic beverage independent of the amount of alcohol consumed to provide a strong evidence platform for alcohol taxation policies.