In 1980, the National Trachoma and Eye Health Program (NTEHP) gave the first national data on eye health and vision loss in Australian Aboriginal and Torres Strait Islander peoples.1 At that time, rates of blindness in Indigenous Australians were 10 times higher than in other Australians, which is a striking paradox, as Aboriginal people have the best recorded visual acuity.2,3
There have been several national programs to improve the delivery of eye care to Indigenous Australians,4-6 and there are ongoing efforts by committed individuals and groups. Occasional reports underscore the ongoing presence of trachoma and the dramatic increase in diabetic eye disease.7-13 However, since the 1980 report, there have been no further national surveys on the status of Indigenous eye health to assess the adequacy of current services and for future planning.
Data from the June 2006 national census were used to delineate 30 geographic areas that each included about 300 Indigenous people.14 The sampling method has been described in detail elsewhere.15 Data collection was undertaken in 2008.
The sample size was determined to detect a doubling in the rate of presenting vision impairment in Indigenous Australians compared with the rate in the Australian population as a whole (“mainstream” Australia). Rates of vision impairment in mainstream Australia have been reported as 4.2% for the better eye in adults16 and 5% in the worse eye for 12-year-old children.17
Standardised demographic data were collected by means of a written questionnaire (self-administered or completed with the help of field staff and an interpreter if necessary).18-20 A standardised eye examination was carried out on all participants. This included measurement of distance and near presenting visual acuity (VA),19,21 pinhole testing if VA was < 6/12, or autorefraction and testing with correction if indicated, and visual field assessment with a Humphrey frequency doubling technology (FDT) test (Zeiss, Jena, Germany). Appropriate arrangements were made for treatment or referral.
Trachoma was graded in each eye, using a × 2.5 magnifying loupe, according to the World Health Organization simplified grading system.22 Digital photographs of the everted left tarsus were graded independently.23
Fundal photographs of each eye were taken using a Canon CR-DGi retinal camera (Canon, Tokyo, Japan). Anteriorly focused, retroillumination photographs of the lens were taken in eyes with VA of < 6/12 to assess cataract.24 Pupil-dilating drops were used when needed. Retinal photographs were assessed in a masked fashion (ie, with the grader blinded to the clinical condition or previous clinical grading of the patient) for diabetic retinopathy,25 macular changes26 or optic disc cupping.27
A diagnosis of glaucoma was made if the cup-to-disc ratio (CDR) (ie, the ratio comparing the diameter of the “cup” portion of the optic disc with the total diameter of the optic disc) was greater than 0.8 or if two or more points on FDT testing were missed in an eye with a CDR of greater than 0.7.19,28 To determine the distribution of optic disc diameters and CDRs in Indigenous Australians, 816 consecutive optic disc photographs were measured (data not presented here): 0.7 was 2 SD from the mean and 0.9 was 3 SD from the mean.29
The target population included 2007 Indigenous children and 1655 adults. Of these, 1694 children (84.4%) and 1189 adults (71.8%) were examined (Box 1). Of 163 non-Indigenous adults in four communities, 136 (83.4%) were examined.
Additionally, in 26 communities, 402 Indigenous children who lived outside the sample area (and were thus ineligible for the study) were examined, as were 425 ineligible adults in 19 communities. Children living within or outside the sample area were generally similar demographically, although the ineligible children were more likely to speak English (Box 2). The ineligible adults differed in several ways from adults in the sample, reflecting self-selection for an eye examination.
Ninety-six per cent of responses to questionnaire items were complete.
For both children and adults, there were no statistically significant differences in presenting binocular distance vision between eligible and ineligible groups (χ2 test P values were between 0.3 and 0.9) (Box 3). Overall, 1.5% of eligible Indigenous children had low vision (VA < 6/12) and 0.2% were blind (VA < 6/60). Of the eligible Indigenous adults, 9.4% had low vision and 1.9% were blind.
Weighted rates of vision loss were age-standardised to the Australian population.14 The relative risks (RRs) of low vision and blindness in Indigenous adults compared with mainstream adults were 2.8 and 6.2, respectively (Box 4).16 By contrast, in Indigenous children compared with mainstream children the RRs of low vision and blindness were 0.2 and 0.6, respectively (Box 4).17,30,31
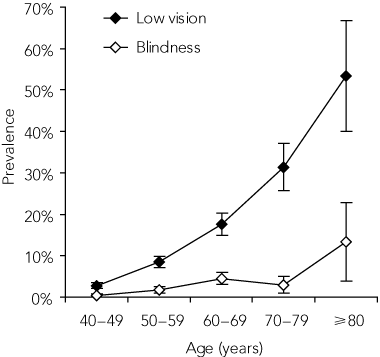
Both low vision and blindness in adults increased markedly with age (Box 5). Among Indigenous adults over the age of 80 years, 53% had low vision and 13% were blind.
The most common cause of bilateral blindness in Indigenous adults was cataract and the most common cause of low vision was uncorrected refractive error (Box 6). In Indigenous children, uncorrected refractive error was the cause of blindness in one of three children and of low vision in 14 of 25 children. Refractive error was the most common cause of monocular low vision in all groups (Box 7). Ocular trauma was the leading cause of monocular blindness in Indigenous adults.
A third of adults in each of the groups (eligible Indigenous, ineligible Indigenous and non-Indigenous) were unable to read normal-sized print (N8) with their near vision on presentation (Box 8). More non-Indigenous than Indigenous participants wore reading glasses during testing (χ2 = 19.0; P < 0.001). There was no significant difference in near vision or the use of reading glasses between the three groups. (χ2 test P values were between 0.2 and 0.3).
Of 1052 participants with presenting VA of ≥ 6/12, 39 (3.7%) missed one FDT point and 96 (9.1%) missed two or more points. In 134 with presenting VA of < 6/12, 8 (6.0%) missed one FDT point and 27 (20.1%) missed two or more points. The correlation between FDT testing and visual function is not well established, and the prevalence of visual field loss detected by FDT testing has not been determined.32
We were unable to include eligible non-Indigenous adults in all remote and very remote communities. In most very remote communities, the non-Indigenous population was small and transient and, in two remote communities, it was considered inappropriate to examine non-Indigenous subjects. With the very small sample of non-Indigenous adults, only limited comparisons could be made, and no significant differences were found between non-Indigenous adults in our sample and adults in mainstream Australia.16
The good vision of Indigenous children can be accounted for by the relative infrequency of myopia,2 although the prevalence of myopia may have increased recently.33 Nevertheless, uncorrected refractive error was responsible for vision loss in 15/28 Indigenous children (54%), and only 8% of Indigenous children wore glasses. Of the 15 Indigenous children with vision impairment due to refractive error, four (27%) were wearing glasses that were not appropriate and reduced their vision to < 6/12. By comparison, the Sydney Myopia Study found that refractive error caused at least 74% and possibly 96% of vision impairment in 6-year-olds30 and 75% in 12-year-olds,17,31 and that spectacles were worn by 4% of younger children and 19% of older children.17,31 A detailed comparison between these studies and ours of the prevalence and causes of blindness in children cannot be made because of the very small numbers involved.
Although our study showed that vision impairment was less common in Indigenous than non-Indigenous children, low vision and blindness were much more frequent in Indigenous adults than in mainstream Australian adults, and were the result of different causes. In mainstream Australia, age-related macular degeneration (AMD) causes 48% of blindness.16 AMD was not seen in our sample population, although one ineligible Indigenous adult was blind from AMD. Similarly, glaucoma, which causes 14% of blindness in mainstream Australia,16 was not seen in our sample population, although one ineligible Indigenous adult was blind from glaucoma. However, optic atrophy and trachoma were common in our study. Our results showed that unoperated cataract was a much more important cause of blindness in Indigenous adults (32%) than in mainstream Australian adults (12%),16 as was refractive error (14% in Indigenous adults compared with 4% in the mainstream).16
Similar differences between Indigenous adults and mainstream adults in the causes of low vision were seen. Cataract was a much more common cause of low vision in Indigenous adults (27%) than in mainstream adults (14%).16 The pattern was similar for diabetic retinopathy (12% v 2%).16 On the other hand, AMD was a less common cause of low vision in Indigenous adults than in mainstream adults (2% v 10%).
In 1980, the NTEHP reported 871 blind Aboriginal people out of 10 601 over the age of 40 years (8.2%),1 a rate about 10 times higher than the rate in non-Aboriginal people. The NTEHP rate is much higher than the 2.8% we found. Detailed comparisons of our study with the NTEHP study are difficult, as their sample was predominantly from more remote areas, their data were aggregated, and their non-Aboriginal sample was self-selected. Nevertheless, some comparison can still be made. In the NTEHP study,1 among Aboriginal people aged over 40 years, blindness was caused by corneal disease in 52% of subjects (84% of which was due to trachoma [ie, 44% of the total]); by cataract in 40%; by diabetes, AMD and other retinal causes in 4%; and by glaucoma in 0.7%. The corresponding data from our study were 9% for corneal disease (all due to trachoma), 32% for cataract, 14% for retinal causes (9% due to diabetes), and no bilateral blindness due to glaucoma.
The rate of self-reported diabetes in Indigenous adults was 0.03% in the NTEHP study1 compared with 37% in our study. Changes in both lifestyle and diet have been implicated in this increase.34 In the NTEHP study, diabetic retinopathy was not separated as a cause of blindness, and all retinal causes, including diabetic retinopathy, caused only 4% of blindness. We found two out of 22 cases of blindness (9%) to be due to diabetic retinopathy.
3 Binocular presenting distant visual acuity among participants in the National Indigenous Eye Health Survey*
Received 23 July 2009, accepted 10 November 2009
- Hugh R Taylor1,2
- Jing Xie2,3
- Sarah Fox2,3
- Ross A Dunn2,3
- Anna-Lena Arnold2,3
- Jill E Keeffe2,3
- 1 Melbourne School of Population Health, University of Melbourne, Melbourne, VIC.
- 2 Vision Cooperative Research Centre, Sydney, NSW.
- 3 Centre for Eye Research Australia, University of Melbourne, Melbourne, VIC.
We wish to recognise the contributions of the National Indigenous Eye Health Survey Advisory Committee (Michael Wooldridge, Ian Anderson, Sandra Bailey, Stephanie Bell, Joe Chakman, Amanda Davis, William Glasson, Mick Gooda, Elissa Greenham, Belinda Sullivan, Debbie Sweeney) and the Steering Committee (Robert Casson, Rowan Churchill, Mark Gillies, William Glasson, Timothy Henderson, Brian Layland, Mark Loane, Ian McAllister, Tharmalingam Mahendrarajah, Richard Mills, Nigel Morlet, Helen Morrissey, Henry Newland, Richard Rawson, Gerd Schlenther). We also thank Mitasha Marolia, Anthea Burnett, Tomer Shemesh, and the many Aboriginal health workers and eye health co-ordinators who assisted with our study (especially Barbara O’Connor, Desley Culpin and Phyllis Tighe), as well as the many volunteers who helped with field work (including Jan Lovie-Kitchen, Nora Ley and Carmel McInally).
Our research was supported by Vision CRC, the International Centre for Eyecare Education, The Eye Foundation and the Harold Mitchell Foundation.
- 1. Royal Australian College of Ophthalmologists. The National Trachoma and Eye Health Program of the Royal Australian College of Ophthalmologists. Sydney: Royal Australian College of Ophthalmologists, 1980.
- 2. Taylor HR. Racial variations in vision. Am J Epidemiol 1981; 113: 62-80.
- 3. Taylor HR. Prevalence and causes of blindness in Australian Aborigines. Med J Aust 1980; 1: 71-76.
- 4. Taylor V, Ewald D, Liddle H, Warchiver I. Review of the implementation of the National Aboriginal and Torres Strait Islander Eye Health Program. Canberra: Commonwealth of Australia, 2004.
- 5. Taylor HR. Eye health in Aboriginal and Torres Strait Islander Communities. Canberra: Commonwealth of Australia, 1997.
- 6. Mayers N. Report to the Royal Australian College of Ophthalmologists. Sydney: RACO, 1982.
- 7. Stocks NP, Hiller JE, Newland H, McGilchrist CA. Trends in the prevalence of trachoma, South Australia, 1976 to 1990. Aust N Z J Public Health 1996; 20: 375-381.
- 8. Mak DB, O’Neill LM, Herceg A, McFarlane H. Prevalence and control of trachoma in Australia, 1997–2004. Commun Dis Intell 2006; 30: 236-247.
- 9. Jaross N, Ryan P, Newland H. Prevalence of diabetic retinopathy in an Aboriginal Australian population: results from the Katherine Region Diabetic Retinopathy Study (KRDRS). Report no. 1. Clin Experiment Ophthalmol 2003; 31: 32-39.
- 10. Jaross N, Ryan P, Newland H. Incidence and progression of diabetic retinopathy in an Aboriginal Australian population: results from the Katherine Region Diabetic Retinopathy Study (KRDRS). Report no. 2. Clin Experiment Ophthalmol 2005; 33: 26-33.
- 11. Lansingh VC, Weih LM, Keeffe JE, Taylor HR. Assessment of trachoma prevalence in a mobile population in Central Australia. Ophthalmic Epidemiol 2001; 8: 97-108.
- 12. Wright HR, Taylor HR. Clinical examination and laboratory tests for estimation of trachoma prevalence in a remote setting: what are they really telling us? Lancet Infect Dis 2005; 5: 313-320.
- 13. McAllister IL. Screening for diabetic retinopathy in rural and remote areas of Australia. Aust N Z J Ophthalmol 1998; 26: 105-106.
- 14. Australian Bureau of Statistics. 2006 census. Experimental estimates of Aboriginal and Torres Strait Islander Australians, Jun 2006. (ABS Cat. No. 3238.0.55.001.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/3238.0.55.001Main+Features1Jun%202006? (accessed Feb 2010).
- 15. Fox SS, Arnold A-L, Keeffe JE, Taylor HR. Sampling and recruitment methodology for a national eye health survey of Indigenous Australians. Aust N Z J Public Health 2010. In press.
- 16. Taylor HR, Keeffe JE, Vu HT, et al. Vision loss in Australia. Med J Aust 2005; 182: 565-568. <MJA full text>
- 17. Robaei D, Huynh SC, Kifley A, Mitchell P. Correctable and non-correctable visual impairment in a population-based sample of 12-year-old Australian children. Am J Ophthalmol 2006; 142: 112-118.
- 18. Ferraro JG, Mazzoni LL, Keeffe JK, et al. Evaluation of an eye health program: the Vision Initiative. Ophthalmic Epidemiol 2006; 13: 127-135.
- 19. Mueller A, Vu HT, Ferraro JG, et al. Rapid and cost-effective method to assess vision disorders in a population. Clin Experiment Ophthalmol 2006; 34: 521-525.
- 20. Burnett AM. Development and validation of a rapid assessment methodology for avoidable blindness in Aboriginal and Torres Strait Islander populations [PhD thesis]. Sydney: University of New South Wales, 2009.
- 21. Keeffe JE, Lovie-Kitchin JE, Maclean H, Taylor HR. A simplified screening test for identifying people with low vision in developing countries. Bull World Health Organ 1996; 74: 525-532.
- 22. Thylefors B, Dawson CR, Jones BR, et al. A simple system for the assessment of trachoma and its complications. Bull World Health Organ 1987; 65: 477-483.
- 23. Taylor HR, Fox SS, Xie J, et al. The prevalence of trachoma in Australia: the National Indigenous Eye Health Survey. Med J Aust 2009; 192: 248-253. <MJA full text>
- 24. Ferraro JG, Pollard T, Müller A, et al. Detecting cataract causing visual impairment using a nonmydriatic fundus camera. Am J Ophthalmol 2005; 139: 725-726.
- 25. Wilkinson CP, Ferris FL, Klein RE; Global Diabetic Retinopathy Project Group. Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology 2003; 110: 1677-1682.
- 26. Bird AC, Bressler NM, Bressler SB, et al. An international classification and grading system for age-related maculopathy and age-related macular degeneration. Surv Ophthalmol 1995; 39: 367-374.
- 27. Constantinou M, Ferraro JG, Lamoureux EL, Taylor HR. Assessment of optic disc cupping with digital fundus photographs. Am J Ophthalmol 2005; 140: 529-531.
- 28. Robin TA, Müller A, Rait J, et al. Performance of community-based glaucoma screening using frequency doubling technology and Heidelberg retinal tomography. Ophthalmic Epidemiol 2005; 12: 167-178.
- 29. Foster PJ, Buhrmann R, Quigley HA, Johnson GJ. The definition and classification of glaucoma in prevalence surveys. Br J Ophthalmol 2002; 86: 238-242.
- 30. Robaei D, Rose K, Ojaimi E, et al. Visual acuity and the causes of visual loss in a population-based sample of 6-year-old Australian children. Ophthalmology 2005; 112: 1275-1282.
- 31. Robaei D, Kifley A, Rose KA, Mitchell P. Refractive error and patterns of spectacle use in 12-year-old Australian children. Ophthalmology 2006; 113: 1567-1573.
- 32. Broman AT, Quigley HA, West SK, et al. Estimating the rate of progressive visual field damage in those with open-angle glaucoma, from cross-sectional data. Invest Ophthalmol Vis Sci 2008; 49: 66-76.
- 33. Taylor HR, Robin TA, Lansingh VC, et al. A myopic shift in Australian Aboriginals: 1977–2000. Trans Am Ophthalmol Soc 2003; 101: 107-112.
- 34. Daniel M, Rowley KG, McDermott R, O’Dea K. Diabetes and impaired glucose tolerance in Aboriginal Australians: prevalence and risk. Diabetes Res Clin Pract 2002; 57: 23-33.





Abstract
Aim: To determine the prevalence and causes of vision loss in Indigenous Australians.
Design, setting and participants: A national, stratified, random cluster sample was drawn from 30 communities across Australia that each included about 300 Indigenous people of all ages. A sample of non-Indigenous adults aged ≥ 40 years was also tested at several remote sites for comparison. Participants were examined using a standardised protocol that included a questionnaire (self-administered or completed with the help of field staff), visual acuity (VA) testing on presentation and after correction, visual field testing, trachoma grading, and fundus and lens photography. The data were collected in 2008.
Main outcome measures: VA; prevalence of low vision and blindness; causes of vision loss; rates of vision loss in Indigenous compared with non-Indigenous adults.
Results: 1694 Indigenous children and 1189 Indigenous adults were examined, representing recruitment rates of 84% for children aged 5–15 years and 72% for adults aged ≥ 40 years. Rates of low vision (VA < 6/12 to ≥ 6/60) were 1.5% (95% CI, 0.9%–2.1%) in children and 9.4% (95% CI, 7.8%–11.1%) in adults. Rates of blindness (VA < 6/60) were 0.2% (95% CI, 0.04%–0.5%) in children and 1.9% (95% CI, 1.1%–2.6%) in adults. The principal cause of low vision in both adults and children was refractive error. The principal causes of blindness in adults were cataract, refractive error and optic atrophy. Relative risks (RRs) of vision loss and blindness in Indigenous adults compared with adults in the mainstream Australian population were 2.8 and 6.2, respectively. By contrast, RRs of vision loss and blindness in Indigenous children compared with mainstream children were 0.2 and 0.6, respectively.
Conclusion: Many causes of vision loss in our sample were readily avoidable. Better allocation of services and resources is required to give all Australians equal access to eye health services.