Several fatal seizure-related motor vehicle accidents have highlighted the roles and responsibilities of patients with medical conditions that may influence driving safety, their treating doctors, and driver licensing authorities (DLAs).1-7 Here, we focus on epilepsy, but the same issues are relevant to many medical conditions that affect fitness to drive.
DLAs have the legal responsibility to determine eligibility to drive, and the treating doctor’s role is to provide relevant medical information. Although DLAs claim that they decide on a patient’s medical fitness to drive, it is a responsibility that is, in practice, shifted to the treating doctor.8 Drivers with some medical conditions are asked by the DLA to consult their doctor, who is issued with a set of guidelines that he or she applies when certifying a patient as fit or unfit to drive. This system is fraught with problems.
The shift of responsibility to the treating doctor creates a conflict of interest. The doctor is acting as an agent of the DLA and may be the only person standing between the patient and their drivers licence. The doctor needs to establish and maintain a trusting relationship with the patient to encourage the patient to follow their advice on treatment, accept possible side effects of treatment and provide accurate information on their progress. The patient often expects that the doctor will be their advocate against a bureaucracy that removes one of their basic rights and sometimes their livelihood. Decisions regarding driving will influence, and will be influenced by, doctor–patient relationships. Some doctors feel under pressure from their patients to make “favourable” decisions (E R S, A B B and J W D, unpublished observations). Some patients develop the perception that their treating doctor has deprived them of their livelihood or imposed hardship when their drivers licence is suspended. They can react by blaming the doctor, not following medical advice or making threats.8
DLAs suggest that this can be solved by referring the patient for a driving assessment or to a specialist.8 However, a driving assessment is not helpful in conditions such as epilepsy, where the impairment is intermittent, and referral to a specialist passes the responsibility from one doctor to another. DLAs offer no advice on how a specialist should proceed when fitness is uncertain. Medical report forms provided by DLAs do not include the option to refer the decision to the DLA.8 Some DLAs suggest to patients that the doctor is responsible for certifying their fitness. For example, some patients who have been reported as unfit to a DLA by a neurologist have been advised by the DLA that their licence is suspended but that it will be reinstated on receipt of a satisfactory report from a neurologist (E R S, unpublished observation). Some of these patients have then seen another neurologist and supplied a different history to regain their licence. Information held by the reporting neurologist and by the DLA is not made available to the new neurologist, who may have no reason to doubt the accuracy of the information provided by the patient.
Neurologists have become acutely aware of a further complication of certification by the treating doctor: their vulnerability to civil and criminal proceedings when injury or death arises from a seizure at the wheel experienced by a patient whom they have certified as fit to drive. In May 2002, a man with a history of epilepsy had a seizure while driving a bus on a country road, colliding with a tree. He and three of his passengers died. The coroner suspended the inquest, concluding that “the admissible evidence is capable of satisfying a jury beyond reasonable doubt that a known person has committed an indictable offence... There is a reasonable prospect that a jury properly instructed would convict that person” and referred the case to the New South Wales Director of Public Prosecutions.7 A NSW coronial inquest into the deaths of Gregory Arthur Petrie, Caroline Page, Barbara Alice Crouch and Kelvin John Fearn was started by coroner Tony Murray but suspended in 2006. The “known person” was the driver’s neurologist. The Director of Public Prosecutions declined to charge the doctor.
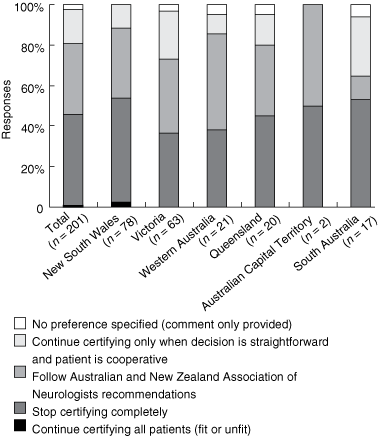
A poll of members of the Australian and New Zealand Association of Neurologists (ANZAN) in December 2006 revealed a high level of dissatisfaction among neurologists with the current system of certification (Box).9 As a result, ANZAN recommended that its members continue to certify driving fitness for patients with epilepsy only where fitness or otherwise is beyond doubt, and to refer other cases to the DLA, providing sufficient clinical information for an appropriately qualified person to determine fitness.9 This led to dialogue between the Epilepsy Society of Australia (ESA) and the National Transport Commission (NTC) and then with the Austroads Registration and Licensing Taskforce, which represents all driver licensing jurisdictions in Australia. In September 2007, the Taskforce accepted a recommendation from the NTC that “all medical reminder forms/letters will be revised to stipulate that responsibility for determining a person’s fitness to drive rests with the driver licensing agency”. (David Stuart-Watt, Program Manager, Registration and Licensing Program, Austroads, personal communication, October 2007). To our knowledge, this has not been implemented. At the same meeting, the Taskforce accepted, in principle, a proposal by the ESA and the ANZAN that certification be performed by the DLA, using relevant information provided by the treating doctor, rather than relying on the treating doctor’s opinion.
A review mechanism to deal with uncertain or exceptional cases is important in any certification system. Ideally, this should be an expert panel of neurologists, indemnified by the DLA. Such a panel exists only in Victoria, where it is convened by the Victorian Institute of Forensic Medicine, while NSW and South Australia use occupational health physicians and Queensland has no review mechanism at all.10
Drivers with medical conditions that impair their fitness to drive are legally obliged to notify the DLA. However, most drivers are unaware of this obligation.10 Treating doctors are not obliged to report all patients who are potentially unfit, except in SA and the Northern Territory. In SA, mandatory reporting is performed inconsistently (A B B, unpublished data). Mandatory reporting of all potentially unfit patients encourages concealment of symptoms, thereby impeding optimal treatment and ultimately reducing road safety.11,12 Nevertheless, the Queensland Government has recently considered the introduction of mandatory reporting following a coronial recommendation1 (Australian Medical Association of Queensland, personal communication, March 2007) and the Victorian Coroner is currently considering it (Catharine Sedgwick, Solicitor, Office of Public Prosecutions Victoria, personal communication, November 2008).
Doctors need to tell patients if their medical condition or its treatment may affect driving capacity, but there is a clear distinction between a doctor giving this advice and mandatory reporting. If a patient refuses to accept medical advice and continues to drive when it is unsafe to do so, then the doctor may need to breach patient confidentiality and disclose information to the DLA if it is in the interest of public safety.13,14 Most doctors will do this only as a last resort, as it will probably do serious harm to their relationship with the patient.
The ESA and ANZAN welcome the Australian Medical Association’s recently developed position statement on the role of the medical practitioner in determining fitness to drive motor vehicles,15 which is consistent with the views we present here.
- Ernest R Somerville1,2
- Andrew B Black3,2
- John W Dunne4,2
- 1 Comprehensive Epilepsy Service, Prince of Wales Hospital, Sydney, NSW.
- 2 Driving Committees, Epilepsy Society of Australia and Australian and New Zealand Association of Neurologists, Sydney, NSW.
- 3 Neurology Department, Queen Elizabeth Hospital, Adelaide, SA.
- 4 Western Australian Comprehensive Epilepsy Service, Neurology Department, Royal Perth Hospital, Perth, WA.
None identified.
- 1. Clements C, Deputy State Coroner. Inquest into the death of Jet Paul Rowland [2002]. File No. COR 605/04(2). Brisbane: Queensland Courts Office of the State Coroner, 2005. http://www.courts.qld.gov.au/Rowland1205.pdf (accessed Sep 2009).
- 2. Navy official guilty of killing family in crash. Sydney Morning Herald 2004; 25 Nov. http://www.smh.com.au/news/National/Navy-official-guilty-of-killing-family-in-crash/2004/11/25/1101219667225.html?from=storylhs (accessed Sep 2009).
- 3. Lethal lies: seven years for wiping out family. Sydney Morning Herald 2005; 18 Mar. http://www.smh.com.au/news/National/Lethal-lies-seven-years-for-wiping-out-family/2005/03/18/1111085997432.html (accessed Sep 2009).
- 4. R v Gillett. No. 03/11/1112, District Court of New South Wales, 2004.
- 5. Edmistone L, Watt A. Jail stint for deadly drive. Courier Mail (Brisbane) 2006; 7 Nov. http://www.news.com.au/couriermail/story/0,23739,2072052 3-3102,00.html (accessed Sep 2009).
- 6. Vicker EF, Deputy State Coroner. Finding upon inquest into the death of Norman John Hasluck (036/04). Ref No. 09/07. Perth: Perth Coroner’s Court, 2007. http://www.safetyandquality.health.wa.gov.au/docs/mortality_review/inquest_finding/Hasluck_finding.pdf (accessed Sep 2009).
- 7. DPP to get crash files. Border Mail (Albury) 2007; 30 Jan. http://www.bordermail.com.au/news/local/news/general/dpp-to-get-crash-files/374550.aspx (accessed Sep 2009).
- 8. Assessing fitness to drive for commercial and private vehicle drivers: medical standards for licensing and clinical management guidelines. Sydney: Austroads, 2003 (revised 2006). http://www.austroads.com.au/cms/AFTD%20web%20Aug%202006.pdf (accessed Sep 2009).
- 9. Somerville ER. Fitness to drive. Aust N Z Assoc Neurol Newsl 2007; 297: 6.
- 10. Assessing fitness to drive: interim review report. Melbourne: National Transport Commission, 2006. http://www.ntc.gov.au/filemedia/Reports/AFTDInterimReviewReportJul06.pdf (accessed Sep 2009).
- 11. American Academy of Neurology. Mandatory reporting of seizures can have a negative impact [press release]. 2 Apr 2003. http://www.aan.com/press/index.cfm?fuseaction=release.view&release=133 (accessed Sep 2009).
- 12. Salinsky MC, Wegener K, Sinnema F. Epilepsy, driving laws, and patient disclosure to physicians. Epilepsia 1992; 33: 469-472.
- 13. Tobin BM, Leeder SR, Somerville ER. Community versus individual benefit. Med J Aust 2002; 176: 279-280. <MJA full text>
- 14. Beran RG, Gerber P, Devereux JA. Usefulness of Austroads’ fitness-to-drive guidelines: lessons from the Gillett case. Med J Aust 2009; 190: 503-505. <MJA full text>
- 15. Australian Medical Association. The role of the medical practitioner in determining fitness to drive motor vehicles — 2008. Canberra: AMA, 2008. http://www.ama.com.au/node/3021 (accessed Sep 2009).





Abstract
Assessment of medical fitness to drive can be a sensitive and difficult task, particularly when it involves a condition such as epilepsy, where impairment is intermittent.
The patient, their doctor and the driver licensing authority (DLA) each have responsibilities, both to the patient and to the wider community of road users.
DLAs in Australia have shifted most of the responsibility for determining fitness to drive to the treating doctor. This creates a conflict of interest and may lead to unsafe decisions, damage to the doctor–patient relationship, interference with medical management and legal vulnerability for the doctor.
Australian neurologists have argued for a system in which the treating doctor provides objective information about the patient’s condition, rather than an opinion on fitness to drive, and the DLA uses that information to determine fitness. This must be supported by an expert review process.
Although drivers are legally obliged to notify the DLA when they become unfit, most people are unaware of this law. However, passing this responsibility to doctors in the form of mandatory reporting is counterproductive to road safety.