Around 30% of all hip fractures in the community occur in residential aged care, representing a substantial cost to the health care system. Evidence from overseas on calcium and vitamin D supplementation and hip protectors suggests these strategies could reduce hip fractures in aged care facilities by up to 50%.1-3
The project nurse provided link people from each intervention facility with information and resources to assist with preventing falls and fractures. An initial training session was held in November 2005. A set of resources was developed to support the 2005 falls prevention guidelines (known as the “Big Green Box”).4 The implementation of these resources was further encouraged during 3-monthly network meetings, held from February 2006 to June 2007 (six meetings in total), convened by the project nurse and attended by the link people. Intervention facility staff were also invited to attend a workshop to learn how to plan and run exercise programs. Support for the intervention was obtained from Divisions of General Practice.
At the time of the census, there were 5391 permanent residents. Box 1 shows that randomisation produced reasonably similar characteristics for residents in the control and intervention groups.
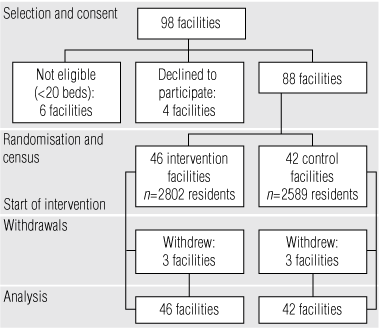
Monthly falls data collection forms were returned by 76%–97% of facilities for each month from July 2005 to June 2007. There was no systematic bias in returns according to type of facility or phase of the study (pre-intervention or intervention). Overall, six facilities withdrew from the project during the intervention. All withdrawing facilities provided sufficient data to allow retention in analyses (Box 2).
Falls events recorded by facilities are shown in Box 3. For the entire cohort (intervention and control groups), there were 13.5 fractured neck of femur events per 1000 falls. Of these events, two occurred within the first 3 months of admission (15%). The risk of death within 3 months of a fall that resulted in a neck of femur fracture was 33%. Similar rates for all events were reported during the pre-intervention and intervention periods, after accounting for high variability of fall rates within facilities per month. The two-stage longitudinal regression model showed no evidence of change in the rate of falls from 16.0 per 100 beds (95% CI, 14.2 to 17.9) for either the pre-intervention stage (0.14 falls per 100 beds per month; 95% CI, − 0.17 to 0.45; P = 0.37) or after intervention commencement (− 0.023 falls per 100 beds per month; 95% CI, − 0.14 to 0.09; P = 0.686), when averaged over both groups. There were also no significant differences between intervention and control groups at commencement, with the intervention group being 2.40 falls per 100 beds (95% CI, − 1.25 to 6.24; P = 0.198) higher than the control group (12.91 falls per 100 beds; 95% CI, 6.89 to 18.93), nor over the first slope representing the pre-intervention period (0.18 more falls per 100 beds per month; 95% CI, − 0.39 to 0.76; P = 0.532) or over the second slope representing the intervention period (0.13 fewer falls per 100 beds per month; 95% CI, − 0.36 to 0.10; P = 0.259).
A sensitivity analysis excluding facilities that withdrew indicated no change in results.
Other trials of falls injury prevention in aged care facilities have produced varied results. One trial showed a reduction in falls by repeat fallers;1 others failed to produce any reduction in falls or fractures;2,3 and one showed reduction in hospital admissions.1 The most significant results came from a French trial of vitamin D and calcium supplementation5 and a Danish trial of hip protector use,6 although the reductions in risk of hip fractures seen in these studies have not been replicated in subsequent studies. Two recent studies have used a wider range of strategies, with better results,7,8 although the short period of intervention in one trial makes the results less convincing.
Another possibility is that the intervention period was too short. A German study seems to support this possibility.8 Falls injury prevention programs may also not be effective if they involve a significant proportion of people with dementia. Subgroup analyses of an intervention trial in aged care facilities that showed an overall reduction in falls failed to show a reduction in residents with cognitive impairment.7
1 Characteristics of 5391 residents in participating facilities at the time of the census, January–February 2006
* Defined as anyone who can stand and walk with or without assistance. |
|||||||||||||||
Received 20 April 2009, accepted 24 September 2009
- John A Ward1
- Mandy Harden1
- Richard E Gibson2
- Julie E Byles2,3
- 1 Hunter New England Health, Newcastle, NSW.
- 2 Research Centre for Gender, Health and Ageing, University of Newcastle, Newcastle, NSW.
- 3 Hunter Medical Research Institute, Newcastle, NSW.
This project was funded by the NSW Health Department’s Health Promotion Demonstration Research Projects Grants Scheme.
Mandy Harden was employed as the project nurse for the research project.
- 1. Ray WA, Taylor JA, Meador KG, et al. A randomized trial of a consultation service to reduce falls in nursing homes. JAMA 1997; 278: 557-562.
- 2. Rubenstein LZ, Robbins AS, Josephson KR, et al. The value of assessing falls in an elderly population. A randomized clinical trial. Ann Intern Med 1990; 113: 308-316.
- 3. McMurdo ME, Millar AM, Daly F. A randomized controlled trial of fall prevention strategies in old people’s homes. Gerontology 2000; 46: 83-87.
- 4. Australian Council for Safety and Quality in Health Care. Preventing falls and harm from falls in older people: best practice guidelines for Australian hospitals and residential aged care facilities. Canberra: Commonwealth of Australia, 2005. http://www.health.gov.au/internet/safety/publishing.nsf/Content/FallsGuidelines-2005Down loads (accessed Jan 2010).
- 5. Chapuy MC, Arlot ME, Duboeuf F, et al. Vitamin D3 and calcium to prevent hip fractures in the elderly women. N Engl J Med 1992; 327: 1637-1642.
- 6. Lauritzen JB, Hindso K. Prevention of hip fractures with hip protectors. Osteoporosis Int 1977; 5: 125-130.
- 7. Jensen J, Lundin-Olsson L, Nyberg L, Gustafson Y. Fall and injury prevention in older people living in residential care facilities: a cluster randomized trial. Ann Intern Med 2002; 136: 733-741.
- 8. Becker C, Kron M, Lindemann U, et al. Effectiveness of a multifaceted intervention on falls in nursing home residents. J Am Geriatr Soc 2003; 51: 306-313.





Abstract
Objective: To test the effectiveness of using a full-time project nurse to assist residential aged care facilities in using evidence-based approaches to falls injury prevention.
Design, setting and participants: Cluster randomised controlled trial involving 5391 residents in 88 aged care facilities in the Hunter and Lower Mid North Coast areas of New South Wales. Residents were followed for 545 days or until death or discharge. Data were collected from July 2005 to June 2007.
Intervention: Employment of a project nurse to encourage best-practice falls injury prevention strategies during the 17-month intervention period.
Main outcome measures: Monthly data about falls, falls injury and falls injury prevention programs; audit of hospitalisation for fractured neck of femur.
Results: Despite significant increases in the provision of hip protectors and use of vitamin D supplementation in both intervention and control facilities, there was no difference in the number of falls or falls injuries between the intervention and control groups, nor a reduction in falls overall. There was also no difference between the 7-month pre-intervention period and the intervention period in the number of falls or falls injuries. Factors related to residents having an increased risk of falls with fractured neck of femur included being ambulant, having dementia, increasing age, and having a high falls risk assessment score.
Conclusion: It is difficult to change falls risk among high-risk populations, including people with dementia. The use of important strategies such as hip protectors and vitamin D and calcium supplementation increased during the study, probably with contamination of control facilities. Longer follow-up may be required to measure the impact on falls outcomes of the strategy of using a facilitating nurse.
Trial registration: Australian New Zealand Clinical Trials Registry ACTRN12605000540617.