Community-based medical education is growing in Australia to meet the increased demand for quality clinical education in expanded settings.1 This demand has been created by rising medical student numbers and the limitations on teaching within tertiary hospitals arising from factors such as shorter admissions and sicker patients.2 General practice provides a ready source of ambulatory patients with a wide range of medical and health needs. Building capacity for teaching in general practice is integral to providing a quality teaching experience.3,4
This is an exciting challenge for general practice,1,3 and patient participation is vital to its sustainability. Despite the increasing use of clinical skills centres, contact with real patients remains crucial for developing clinical acumen. As proposed by a consumer advocate, “you can play with dead bodies and dummies for as long as you like, but at some stage you’ve got to meet the real person”.5 Patients have traditionally played a passive role in medical education, but their contribution to clinical teaching is now being emphasised and developed. Their experience complements the expertise of medical educators, offering a different perspective on health, disease and health care. Collaboration with patients can enhance students’ awareness of the factors that influence patients’ health and quality of life.6
Studies show that medical student education does not compromise patient satisfaction with care, and have identified key reasons patients choose to be involved. Although some participate for their own benefit, most are altruistic, wishing to help the student and the doctor and to use their condition to facilitate learning. Patients also feel qualified to assist in developing medical students’ professional skills and attitudes.7-14 In fact, they appear a willing but potentially underutilised resource for training senior medical students; for example, a South Australian study found that general practice patients expected greater involvement in teaching sessions than actually occurred.14 However, that small study was conducted in traditional teaching practices in urban settings, where patients may be more accepting of senior medical student involvement.
The method and survey instrument were based on those used in a previous study of the views of urban Australian general practice patients on the involvement of medical students in their consultations.14
In our study, patients attending six rural (Rural, Remote and Metropolitan Areas [RRMA]15 category 4: small rural cities) and 11 regional (RRMA 2: other metropolitan centres) general practices involved in student teaching in NSW were invited to participate. The students involved were University of Wollongong graduate-entry medical students (25% of RRMA 2 background and 33%, RRMA 3–7 [rural and remote centres]). The study was conducted at the end of their first study year, in the final two student placements, in November 2008.
Forty-six patients (39%) did not indicate any reason they might refuse medical student involvement. Among the tick options, reasons cited for possible refusal were “personal” (49; 42%); “concerns for patient privacy” (23; 20%) and “students lacked experience” (20; 17%). Only eight patients (7%) indicated student personality as a reason for refusing student involvement. Box 1 lists the main themes found in the free-text responses for consent and refusal, and illustrative citations.
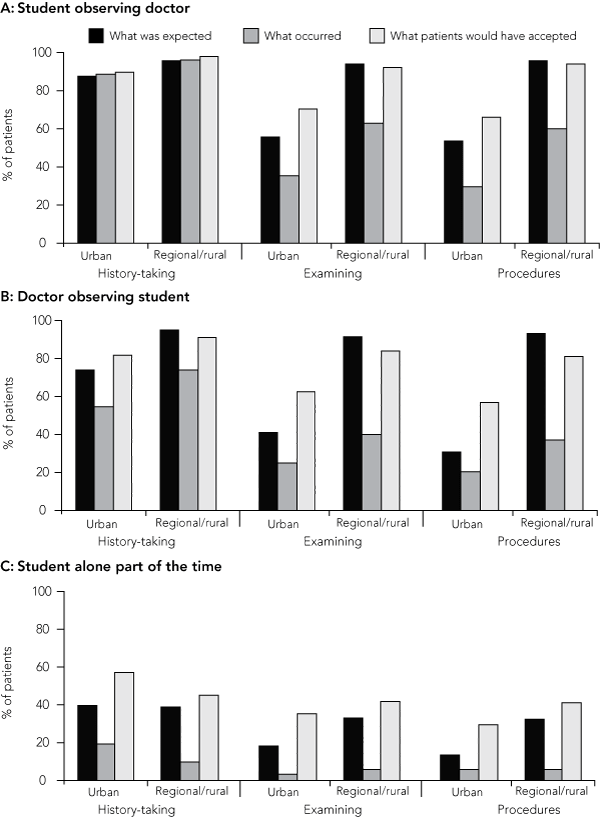
Most patients (94%–96%) expected that the student would observe the doctor taking a history, examining the patient or undertaking a procedure, and most (92%–95%) also expected that the student would undertake some aspect of the consultation with the doctor observing (Box 2). Only about a third of patients (32%–39%) expected that the student would be alone during part of the encounter and would conduct some aspect of the consultation. There was no difference in expectations between patients who had previous experience of student involvement in consultations and those who did not.
Students observed the doctor taking a history in 96% of consultations, and this would have been accepted by 98% of patients (Box 2). Less often, students observed the doctor examining the patient (63%) and undertaking a procedure (60%). However, most patients would have accepted the student observing the doctor in these aspects of the consultation (92% and 94%, respectively).
Box 2 also compares the results of this survey with those from the previous study in urban general practices,14 which used the same survey questions and involved third-year graduate-entry medical students.
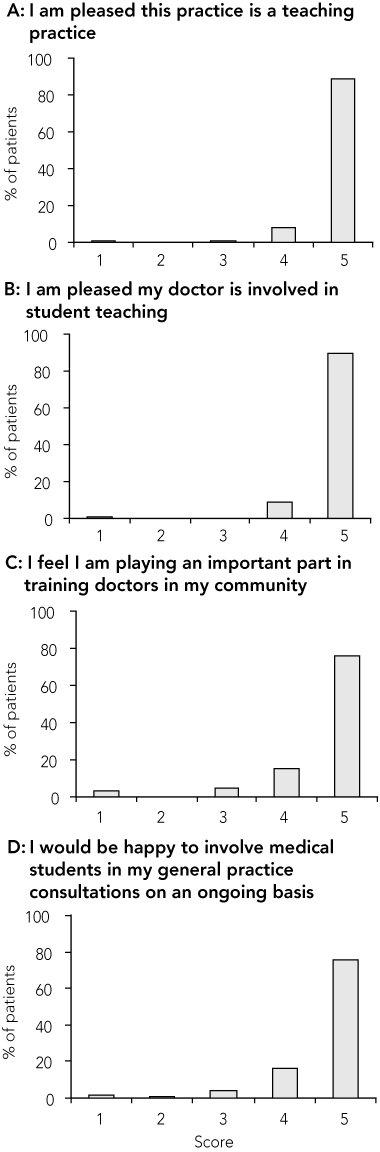
Patients strongly supported the involvement of their general practice in medical student teaching, with 89% strongly agreeing that they were pleased the practice was a teaching practice and 90% that their doctor was involved in teaching (Box 3).
This study replicates an important finding of the previous survey in an urban setting,14 that patients were willing to accept more student involvement than actually occurred. However, there were substantial differences in the student clinical activities that the two patient groups expected, experienced or accepted. Despite the fact that the regional/rural students had relatively less clinical experience than their urban counterparts at the time of study, the regional/rural patients expected, and would have accepted, higher levels of involvement than occurred. Also, in the regional/rural setting, students were more involved in patient consultation than the urban students.
Our results should be interpreted with caution in light of the small number of participants and the fact that patients came from only one regional and one rural area. Although GPs clearly play a central role in deciding what is appropriate, our study confirmed earlier findings of patients’ positive views on consulting with students in general practice and the reasons they may consent or refuse to be involved.14,16 It also repeated the findings of a previous study in urban Australian general practices that patient willingness to be involved in student learning is both underestimated and underused,14 and extended those findings to regional/rural settings and to patients with no previous experience of medical student involvement in their consultations. The regional/rural patients in our study saw themselves as “part of the real context of health care”, a theme also previously described in a study conducted in general practice in Sweden.16
1 Themes of patients’ free-text responses and illustrative citations
Question: What are your reasons for agreeing to student involvement in your consultation today?
Student learning: Because everybody’s got to learn.
Previous experience of patients: Prior positive experience with students.
Recruiting more doctors: We need more doctors so the students need hands-on experience.
Comfort with student involvement: No concerns.
Question: When might you refuse medical student involvement in your consultation?
Intimate issues: Very intimate issue only.
Personal factors: Knowing the student personally.
Student supervision: I wouldn’t object but would like the doctor to oversee the student.
- J Nicky Hudson1
- Kathryn M Weston2
- Elizabeth E Farmer3
- Rowena G Ivers4
- Russell W Pearson5
- Graduate School of Medicine, University of Wollongong, Wollongong, NSW.
This study was supported by a small grant from the University of Wollongong Health and Behavioural Sciences Faculty Research Committee. These funds were used to pay research assistants for data collection in the GP surgeries and travel to the surgeries, and for preparation of the ethics application. None of the funds were used for study design, analysis or interpretation, or writing or publication of this article.
- 1. Van Der Weyden MB. Expanding primary care-based medical education: a renaissance of general practice [editorial]? Med J Aust 2007; 187: 66-67. <MJA full text>
- 2. Australian Institute of Health and Welfare. Trend to shorter hospital stays continues [media release]. Canberra: AIHW, 1999. http://www.aihw.gov.au/mediacentre/1999/mr19990630.cfm (accessed Aug 2009).
- 3. Thistlethwaite JE, Kidd MR, Hudson JN. General practice: a leading provider of medical student education in the 21st century? Med J Aust 2007; 187: 124-128. <MJA full text>
- 4. Pearce R, Laurence CO, Black LE, Stocks N. The challenges of teaching in a general practice setting. Med J Aust 2007; 187: 129-132. <MJA full text>
- 5. McGhee K. Your patient. Aust Doct 2007; (Nov 23): 47.
- 6. Kelly D, Wykurz G. Patients as teachers: a new perspective in medical education. Educ Health 1998; 11: 369-377.
- 7. Morrison JM, Murray TS. Preliminary study into the opinions of patients about the presence of medical students in the general practice consultation. Health Bull (Edinb) 1995; 53: 343-347.
- 8. Cooke F, Galasko G, Ramrakha V, et al. Medical students in general practice: how do patients feel? Br J Gen Pract 1996; 46: 361-362.
- 9. Nair BR, Coughlan JL, Hensley MJ. Student and patient perspectives on bedside teaching. Med Educ 1997; 31: 341-346.
- 10. O’Flynn N, Spencer J, Jones R. Consent and confidentiality in teaching in general practice: survey of patients’ views on presence of medical students. BMJ 1997; 315: 1142.
- 11. Bentham J, Burke J, Clark J, et al. Students conducting consultations in general practice and the acceptability to patients. Med Educ 1999; 33: 686-687.
- 12. Wykurz G, Kelly D. Developing the role of patients as teachers: literature review. BMJ 2002; 325: 818-821.
- 13. Chipp E, Stoneley S, Cooper K. Clinical placements for medical students: factors affecting patients’ involvement in medical education. Med Teach 2004; 26: 114-119.
- 14. Salisbury K, Farmer EA, Vnuk A. Patients’ views on the training of medical students in Australian general practice settings. Aust Fam Physician 2004; 33: 281-283.
- 15. Australian Government Department of Health and Ageing. Rural, Remote and Metropolitan Areas (RRMA) Classification. http://www.health.gov.au/internet/main/publishing.nsf/content/work-st-bmp-wher-rrma (accessed Jan 2010).
- 16. Haffling A-C, Hakansson A. Patients consulting with students in general practice: survey of patients’ satisfaction and their role in teaching. Med Teach 2008; 30: 622-629.





Abstract
Objective: Community-based medical education is growing to meet the increased demand for quality clinical education in expanded settings, and its sustainability relies on patient participation. This study investigated patients’ views on being used as an educational resource for teaching medical students.
Design: Questionnaire-based survey.
Setting and participants: Patients attending six rural and 11 regional general practices in New South Wales over 18 teaching sessions in November 2008, who consented to student involvement in their consultation.
Main outcome measures: Patient perceptions, expectations and acceptance of medical student involvement in consultations, assessed by surveys before and after their consultations.
Results: 118 of 122 patients consented to medical student involvement; of these, 117 (99%) completed a survey before the consultation, and 100 (85%) after the consultation. Patients were overwhelmingly positive about their doctor and practice being involved in student teaching and felt they themselves played an important role. Pre-consultation, patients expressed reluctance to allow students to conduct some or all aspects of the consultation independently. However, after the consultation, they reported they would have accepted higher levels of involvement than actually occurred.
Conclusions: Patients in regional and rural settings were willing partners in developing skills of junior medical students, who had greater involvement in patient consultations than previously reported for urban students. Our study extends the findings from urban general practice that patients are underutilised partners in community-based medical training. The support of patients from regional and rural settings could facilitate the expansion of primary care-based medical education in these areas of workforce need.