In recent years, there has been a fundamental shift in medical genetics. From an initial focus on chromosomal and rare Mendelian disorders, the application of genetics in medicine has expanded to become relevant to all areas of health care.1 With evidence mounting that family history is a risk factor for many common multifactorial disorders,2 there is increasing focus on the clinical utility of family history for identifying high-risk subgroups in the population.3
Family history has long been emphasised in undergraduate medical training as a fundamental part of history taking.4 Although the primary care setting is perhaps best suited to assessing family history details,5 hospitalisation also offers opportunities to identify heritable risk factors. For people who seldom use primary care services, an acute hospital admission may be their only contact with health care professionals in years. The hospitalisation of someone with an undiagnosed Mendelian disorder may also offer a rare diagnostic opportunity for the patient and any high-risk relatives. For example, an acute myocardial infarction in a 45-year-old man with previously unrecognised familial hypercholesterolaemia represents an opportunity for diagnosis and implementation of an effective long-term health care management plan. For first-degree relatives at highest risk, there is evidence that characterisation of an inherited disorder presenting as an acute illness is a powerful stimulus for effective communication about the condition within the family.6
Studies have examined the benefits of a detailed family history in the primary care setting,7 but there has been no focus on the potential opportunity to record a standardised family history for hospitalised inpatients. In the absence of published data on the frequency or adequacy of family history taking among adults admitted to hospital, we retrospectively reviewed the family histories documented by medical staff for patients admitted to the short-stay medical unit (SSMU) in Royal Perth Hospital (RPH), a major tertiary teaching hospital in Perth, Western Australia.
The details recorded from the case notes were: age and sex, presenting complaints, past medical history, and discharge diagnoses. All family history details recorded by emergency or SSMU staff were noted. Specific note was made of details recorded for more than one generation of family members. Family histories were categorised into three broad groups (Box 1).
There were 1807 recorded admissions to the SSMU during the 6-month study period. The 300 patients (165 women, 135 men) whose case notes were reviewed ranged in age from 18 to 98 years (median age, 64 years). There were 92 patients aged < 50 years, 109 aged 50–74 years, and 99 aged > 74 years. The patients’ presenting complaints at admission are listed in Box 2.
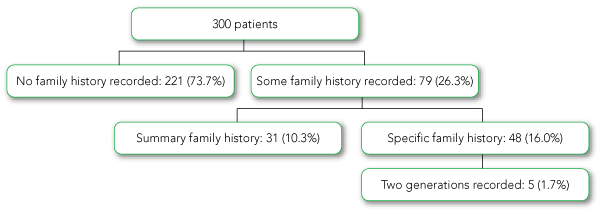
Among the 300 case notes reviewed, 221 (73.7%) contained no comments to indicate that family history had been considered, which left about one in four cases in which there was at least some documentation of family history during admission (Box 3). Of the 300 patients, 48 (16.0%) had some specific medical details documented about at least one family member. A family tree was not documented in any case notes, and family history details of two generations of family members were recorded for only five patients.
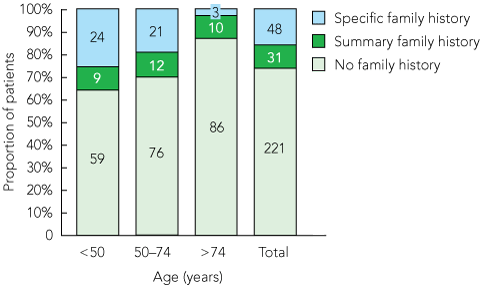
Patient age appeared to influence the frequency of a more detailed family history being recorded, with a trend towards increased documentation of family history among younger patients (Box 4).
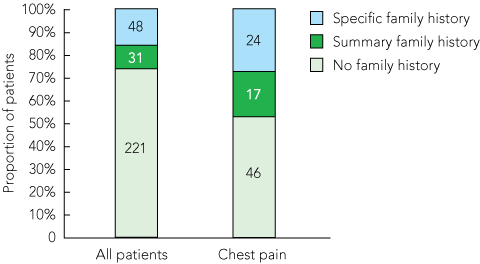
The highest level of family history documentation was found in the case notes of patients presenting with chest pain, 47% of which included some comment about family history (Box 5). Of these 87 patients (32 men, 55 women; median age, 59 years), 29 (33.3%) had a comment recorded about the presence or absence of ischaemic heart disease among relatives.
The reason for the better documentation of family history among patients admitted with chest pain is uncertain. Of potential relevance, however, is the published outcome of an earlier retrospective audit in the same hospital of the rate of diagnosis of familial hypercholesterolaemia among patients presenting with cardiac-type chest pain or for diagnostic coronary angiography.8 This survey, conducted 4 years earlier, identified comments about family history in only 14% of cases. It is also noteworthy that an RPH emergency department admission sheet specifically for patients with chest pain does not include a prompt to record family history.
We considered whether our observation of documented family history in only 26% of cases is an Australian phenomenon. A recent retrospective audit in the United Kingdom of the quality of surgical clinical notes identified family histories in 33% of cases,9 only marginally higher than our findings. As these are retrospective audits, we also considered whether family history is asked for but not documented in some instances. A direct observational study in the United States, which reviewed ambulatory patient visits to family physicians, found that family history was discussed in 51% of new patient visits but only 22% of visits with established patients.10 The study also found that family histories were discussed less often when patients were unwell. These findings are in keeping with the low rate of documented family history taking that we identified.
Ask about any history of a similar illness in the family. Inquire about the health and, if relevant, the causes of death and ages of death of the parents and siblings. However, if there is any suggestion of an hereditary disease a complete family tree should be constructed.4
The extent of neglect in documentation of family history that we have identified prompted us to consider why this component of the medical examination is so frequently overlooked. It is possible that high workloads may encourage medical staff to abandon this component of the clinical examination. Alternatively, it may reflect a prevailing culture among medical staff of focusing on acute issues and ignoring potential chronic or long-term health issues, particularly those of relatives, whom staff may not consider to fall within the professional duty of care expected of them. As there is a predominance of local graduates among the junior medical staff of RPH, it is possible that our finding may simply reflect local issues in the teaching of medical undergraduates. In this respect, it is notable that medical genetics is the youngest of the medical specialties, and core capabilities in genetics for Australian and New Zealand medical graduates were first defined in 2008.11
Family history is currently rarely considered by medical staff caring for acutely ill patients in hospital. Beyond its role as a tool for assessing genetic risk, many experienced clinicians recognise that family history offers an opportunity to gain further insight into the social circumstances of individual patients — a vital component of patient care. As family history offers an increasing range of opportunities for improved health outcomes,12 any failure to routinely assess it is a lost opportunity to improve the health of those at increased risk of familial disease.
1 Family history categories
Family history with some specific details recorded
Family history with summary information only
No documentation available to indicate whether family history had been considered
Received 16 August 2009, accepted 22 December 2009
- Andrew R Langlands1
- David A Prentice1
- David Ravine2
- 1 Royal Perth Hospital, Perth, WA.
- 2 Western Australian Institute for Medical Research, School of Pathology and Laboratory Medicine, University of Western Australia, Perth, WA.
We are grateful to Professor Jon Emery and Dr June Crowhurst for their insightful comments and criticisms. Thanks also to Nicola Hill in Medical Records and Rieno Ienco in the information technology department at Royal Perth Hospital.
None identified.
- 1. Guttmacher AE, Collins FS. Welcome to the genomic era [editorial]. N Engl J Med 2003; 349: 996-998.
- 2. Yoon PW, Scheuner MT, Peterson-Oehlke KL, et al. Can family history be used as a tool for public health and preventive medicine? Genet Med 2002; 4: 304-310.
- 3. O’Neill SM, Rubinstein WS, Wang C, et al; Family Healthware Impact Trial group. Familial risk for common diseases in primary care: the Family Healthware Impact Trial. Am J Prev Med 2009; 36: 506-514.
- 4. Talley NJ, O’Connor S. Clinical examination: a systematic guide to physical diagnosis. 3rd ed. Churchill Livingstone, 1996: 8-9.
- 5. Reid GT, Walter FM, Brisbane JM, Emery JD. Family history questionnaires designed for clinical use: a systematic review. Public Health Genomics 2009; 12: 73-83.
- 6. McCune CA, Ravine D, Worwood M, et al. Screening for hereditary haemochromatosis within families and beyond. Lancet 2003; 362: 1897-1898.
- 7. Qureshi N, Bethea J, Modell B, et al. Collecting genetic information in primary care: evaluating a new family history tool. Fam Pract 2005; 22: 663-669.
- 8. Bates TR, Burnett JR, van Bockxmeer FM, et al. Detection of familial hypercholesterolaemia: a major treatment gap in preventative cardiology. Heart Lung Circ 2008; 17: 411-413.
- 9. Osborn GD, Pike H, Smith M, et al. Quality of clinical case note entries: how good are we at achieving set standards? Ann R Coll Surg Engl 2005; 87: 458-460.
- 10. Acheson LS, Wiesner GL, Zyzanski SJ, et al. Family history-taking in community family practice: implications for genetic screening. Genet Med 2000; 2: 180-185.
- 11. Human Genetics Society of Australasia Education Committee. Core capabilities in genetics for medical graduates. http://www.hgsa.com .au/images/UserFiles/Attachments/Core capabilitiesingeneticsforMedgrads1.pdf (accessed May 2010).
- 12. Khoury MJ, Gwinn M, Yoon PW, et al. The continuum of translation research in genomic medicine: how can we accelerate the appropriate integration of human genome discoveries into health care and disease prevention? Genet Med 2007; 9: 665-674.





Abstract
Objective: To retrospectively review the frequency and adequacy of family histories recorded from patients admitted to a short-stay medical unit in a tertiary teaching hospital.
Design, setting and patients: A formal audit of the medical records of 300 randomly selected patients who were admitted to the Royal Perth Hospital short-stay medical unit between July and December 2007.
Main outcome measure: Proportion of patient records with family history documents.
Results: Of the 300 patient records, 48 (16.0%) contained a family history with specific details about the presence or absence of a medical condition in at least one relative. Overall, 221 records (73.7%) had no family history documented. There was a trend towards more frequent and detailed family histories being recorded from younger patients and those presenting with chest pain.
Conclusions: Family history was seldom documented in patients admitted to a short-stay medical unit in a tertiary teaching hospital. An increased focus on family history taking among acutely ill patients offers potential health gains for patients and their high-risk relatives, particularly as preventive or risk-reducing health care strategies are emerging for a growing number of heritable disorders.