In the face of projections of the future escalating costs of health care, Australian governments recognise the need for structural reform of our health system. The final report of the National Health and Hospitals Reform Commission (NHHRC) articulated three reform goals, namely to: tackle major access and equity issues; redesign the health system to meet emerging challenges; and create an agile and self-improving health system for future generations.1
The NHHRC report sets out a vision for using evidence: (i) to inform short-term actions for system redesign to tackle access, equity and emerging challenges; and (ii) to guide continuous improvement and innovation in the longer term.1 It echoes recent statements by the Productivity Commission2 and by the new director of the United States National Institutes for Health who has prioritised “putting science to work for health care reform”.3 The purpose of our study was to explore the extent to which Australia is currently generating the kind of research that is needed to underpin health system reform, with a specific focus on hospital care.
Hospitals are a major target of the current reform agenda because they are the largest single recurrent item of health expenditure ($34 billion of the total $94 billion spent on health care annually)4 and are projected to be a main contributor to growth in this expenditure.5 Moreover studies of variation in hospital care and spending across health systems, such as Medicare in the US,6 have highlighted that policies focused on improving the efficiency of hospital service delivery could result in savings without reducing quality of care.7
The Australian hospital system has unique features that distinguish it from international systems, including the funding and administrative split between the federal and state governments and the mix of private and public funding of hospitals. Comparisons across different countries have shown that the wider health system structure is a determinant of the success of organisational strategies within hospitals, such as approaches to bed use.8
Bibliographic analyses have been used to describe the number and type of health research publications over time on topics such as health informatics;9 Indigenous health;10 tobacco and alcohol use and inadequate physical activity;11 and the quality and safety of hospital care.12 These studies provide an indication not only of how much evidence is available to inform policy deliberations, but also of research capacity in the particular field. We report the findings of a bibliographic analysis that investigated how much Australian research is available to guide the reform of Australian hospitals. We reviewed research focused on structures and processes in hospitals that are amenable to change by policy agencies or by hospitals. Our study addressed the questions shown in Box 1.
We searched MEDLINE to locate all research publications for the period 1 January 1996 to 31 December 2007 that focused on the organisation and delivery of Australian hospital services; the search strategy we used, outlined in Box 2, was developed with the help of a librarian and was based on published search strategies.13 We combined medical subject headings (MeSH) with text words to avoid missing publications that might not have been indexed during the time of our search. All search queries were combined by the Boolean operators “AND” or “OR” to increase sensitivity, reduce false positive findings and prevent repetitive citations. Research was limited to English language publications.
All of the available publications we identified using the search strategy were included in the coding process (Box 3). One researcher (T W) coded the publications and another (M H) reviewed the coding using the definitions and exclusions outlined below. There was 100% agreement after discrepancies were resolved through discussion.
Publications were included if their content focused on (i) Australian hospitals (inpatient and outpatient care), and (ii) systems, organisational structures and processes, health technologies affecting access to health care, the quality and cost of health care, and health outcomes.14 For example, publications focused on models of care, health care costs, integrated care models, clinical guideline implementation, accreditation and workforce satisfaction were included. Publications focused on clinical therapeutic interventions, including trials of these, were not included. To investigate whether we might have missed relevant articles that were published in clinical speciality areas, we ran a search for Australia (MeSH) and hospitals (MeSH) and kidney disease (MeSH and all text words related to kidney disease), and similarly for stroke, from 1996 to 2007. This did not yield any additional relevant articles.
Publications were classified as reporting empirical studies if they described original research and presented new data (either qualitative or quantitative). These were further characterised10,11 as follows.
Type of research: articles were coded as:
descriptive research: publications that explored the frequency, patterns or predictors of hospitalisation or related variables;
measurement research: publications that developed or examined the qualities of measurement instruments or validation of data sources related to hospital care; or
intervention research: studies that tested the efficacy, effectiveness or implementation of an intervention to a hospital system, structure or process (these publications were classified further by the type of intervention and clinical focus of the intervention — see Box 4).
Funding source: was coded on the basis of what was acknowledged. If no specific source was acknowledged and all authors were based at a university, publications were coded as “university funded”.
Hospital type: this was coded as public or private, based on where the research was conducted.
Descriptive analyses were performed using SPSS, version 15 (SPSS Inc, Chicago, Ill, USA).
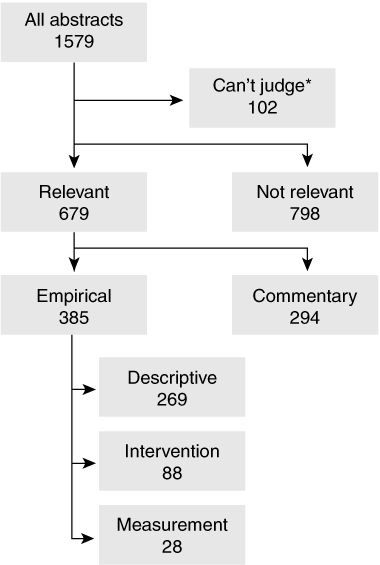
The results of the bibliometric analysis are presented in Box 3, Box 4 and Box 5. Our search strategy identified 679 articles published from 1996 to 2007 that focused on the organisation and delivery of Australian hospital services (Box 3). Of these, 57% (385) reported empirical research and 43% (294) were commentaries. Among the publications describing empirical research, 70% presented descriptive studies, 23% intervention studies and 7% measurement studies.
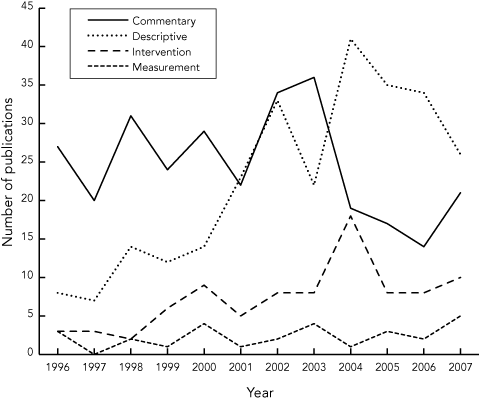
The number of publications increased from 41 in 1996 to 62 in 2007 (Box 5).
The interventions tested (Box 4) were: new services, systems, or restructures (20%); new or modified processes to improve patient treatment (20%); initiatives to improve safety and quality (15%); and workforce redesign (13%). A quarter of these interventions targeted the whole hospital (28%). The rest were focused on specific clinical services or wards within hospitals such as cardiac care (16%), paediatric care (13%) and maternity care (9%).
Box 4 shows that the main funding sources for the research were universities (34%), governments (33%), and research councils (13%). Most of the research was conducted in public hospitals (78%).
We found only a small amount of local research that was relevant to the reform of the Australian hospital system. From 1996 through 2007, 385 empirical publications —an average of 32 publications per year —examined the organisation and delivery of Australian hospital services. This finding is consistent with that of a previous study, spanning the 10-year period 1992 to 2001, in which selected journals were searched for Australian health services research (not just hospital-focused research), and which found 482 publications, including methodological and commentary articles.15
This limited amount of research that is focused on hospitals is roughly equivalent to that published about Indigenous health outcomes, an area that has been prioritised by the National Health and Medical Research Council (NHMRC) for targeted funding.10 Authors of another bibliometric study used PubMed to tabulate the number of biomedical publications by authors linked to an Australian institution.16 They identified 2250 Australian clinical trial publications over the 3-year period 2002 to 2004. This number is in dramatic contrast to the 385 empirical publications focused on the organisation and delivery of hospital services that we found over 12 years, even taking into account the different bibliographic methods used in the two studies.
Most of the empirical publications that we found were descriptive studies. Describing problems is, of course, the first step to solving them. However, practical decisions about the implementation of new policies and programs must be supported by evidence from intervention studies.17 We found only a very limited number of intervention studies; this is consistent with the findings of bibliographic analyses of research outputs in other health policy priority areas.10,11 The NHHRC final report1 recognised the urgent need to embed intervention research into the implementation of policies and programs as a strategy to create an agile and self-improving health system. This was also emphasised in a report of the review of public health research funding in Australia conducted for the NHMRC,17 which highlighted the need for research across the descriptive–intervention spectrum, with an emphasis on intervention studies to meet current and future policy needs. The challenge is to create mechanisms to enable large-scale intervention research to be conducted in the complex settings of hospitals contemporaneously with the implementation of new models of service delivery and organisation.
Although the numbers of articles examining the organisation and delivery of Australian hospital services was small, there is some evidence that the research effort is growing, albeit slowly. We found a 50% increase in publications per annum from 1996 to 2007; in contrast, the annual number of medical and health research publications by Australian authors increased by 100% from 1996 to 2004.16 Evidence from other countries shows that partnerships between researchers and policymakers,18,19 targeted investment,18,20 and increased use of routinely collected data for research6,20 could potentially accelerate this growth.
Examples of successful research partnerships include the Department of Veterans Affairs Veterans Health Administration (VHA) in the US and the Manitoba Centre for Health Policy in Canada. In 1998, the VHA established a partnership between researchers, clinicians and managers to examine clinical care. Known as the Quality Enhancement Research Initiative (QUERI), this approach has led to redesign of systems of care for priority areas, including chronic heart failure, stroke, mental health and diabetes,18 that have resulted in improvements in health system performance.18,19 The Manitoba Centre for Health Policy has worked in partnership with the Manitoba Ministry of Health for more than 25 years to provide analyses of health system performance and health needs that have led to reform in areas including hospital restructure and emergency department waiting times.20
Australia does not have a specific funding agency or specific research funding programs responsible for commissioning research to support the operational needs of the health system.21,22 Internationally, there has been significant targeted investment in health services research, for example, through the Service Delivery and Organisation Programme in the United Kingdom, the Canadian Health Services Research Foundation and the Institute of Health Services and Policy Research in Canada, and the Department of Health and Human Services Agency for Healthcare Research and Quality in the US.
Although information about the funding source was missing from many articles, we found that only around 10% of Australian research into hospital systems is funded by the NHMRC and the Australian Research Council. Our finding is in accord with the NHMRC’s relatively low expenditure on health services research. In 2008, this amounted to $24 million, only 3.88% of total NHMRC funding for research ($627 million).23 In contrast, the Canadian Institutes of Health Research spends $CA70.3 million annually on health services research, which is 6.33% of its total funding for research ($1.12 billion).24
Optimal funding schemes for the kind of research that will make a significant contribution to informing hospital reform will support partnership approaches, build capacity and provide for prompt review to meet policy timeframes.22 There is some early evidence that the NHMRC is considering new approaches.25 For example, the new NHMRC Partnership Projects, which ran their first funding round in 2008, will inject additional funds into projects that are conducted in partnership with policy and service delivery agencies (such as NSW Health and the Australian Commission on Safety and Quality in Healthcare). In order to provide timely evidence on emerging issues in the hospital system, and to support research that is conducted contemporaneously with the introduction of reforms,17 speedy review processes and frequent funding rounds are needed. The NHMRC also made a commitment in its 2007–2009 strategic plan to implement a policy and practice plan that included the establishment of Partnership Centres,26 which could potentially strengthen hospital-focused research through building capacity and long-term relationships with partnership agencies.
Health systems research has flourished in the VHA in the US and in Manitoba in Canada, in part because routinely collected health data were available for analysis.19 In Australia, routinely collected data (including information from Medicare, hospital inpatient statistics and mortality data) are among the most comprehensive available anywhere in the world. New national data-linkage facilities funded through the National Collaborative Research Infrastructure Strategy will further build the resource of routinely collected data in Australia by facilitating integration of information across jurisdictions and over time. Potentially, electronic health records may also become a related resource over time. But to make the most of it, we will need to tackle the major current barriers to using administrative health data for research, which include a shortage of skilled analysts and biostatisticians, and administrative obstacles to data access and use.
The difficulty in conducting systematic searches for health systems research has been acknowledged by others;13,15 our search strategy may have failed to capture some relevant articles because they used keywords and titles that fell outside its scope. It is also possible that a small number of additional articles may have been found through searches in other databases (eg, the Excerpta Medica Database, EMBASE). Quantifying the grey literature reports (eg, commissioned economic analyses and evaluations) was beyond the scope of this study. Although they may contain high-quality and relevant information, these reports may not be peer reviewed and are not accessible through centralised databases such as MEDLINE.
Although research is only one input to the development and implementation of sensible reforms of our hospitals, it has the potential to significantly improve quality, safety and the efficiency of use of hospital resources. The results of individual studies rarely produce significant shifts in policy. Rather, it is the distilled learning that come from bodies of research that provokes action.27 If we are to establish an evidence base for reform in Australia, increased capacity in health systems research will be required. We have some of the early building blocks in place, including new national research funding schemes, and burgeoning resources of routinely collected data, but more investment, and a strategic approach to developing partnerships and tackling current barriers to research, are needed if we wish to successfully put “science to work for health care reform”.
Our call for more applied research focused on health services and systems is not new. In 1972, Archie Cochrane outlined why more evidence was needed to inform the redesign of the UK National Health Service to increase its effectiveness and efficiency. He stated that, with more evidence, “there is a whole rational health service to gain”.28 This remains the case in Australia in 2010.
1 Research questions — how much Australian research is available to inform the reform of Australian hospitals?
How many peer-reviewed articles with a focus on the organisation and delivery of Australian hospital services have been published from 1996 to 2007?
Has the output increased over time?
What proportion of these articles present original empirical research?
Of the original empirical studies, how many have tested the effectiveness of a service-delivery intervention in the hospital setting?
Were the interventions tested aligned to strategic priorities for Australian hospitals?
Who is funding this research?
2 The MEDLINE search strategy used in this study
PubMed queries were performed using the MEDLINE interphase.
Query 4 — limit to publications in the English language only.
Query 5 — limit to year of publication: (a) Limits: publication date from 1996 to 2007.
3 Coding process to classify the publications, and overview of sample
 |
|
* Abstracts that were unclear or for which full publication was not available. |
- Mary Haines1
- Sally Redman1
- Louisa R Jorm2,1
- Teresa M Wozniak1
- Sanja Lujic2
- 1 Sax Institute, Sydney, NSW.
- 2 School of Medicine, University of Western Sydney, Sydney, NSW.
None identified.
- 1. National Health and Hospitals Reform Commission. A healthier future for all Australians — final report June 2009. http://www.health.gov.au/internet/nhhrc/publishing.nsf/Content/nhhrc-report (accessed Apr 2010).
- 2. Banks G. Challenges of evidence-based policy-making. Canberra: Australian Government Productivity Commission and Australian Public Service Commission, 2009. http://www.apsc.gov.au/publications09/evidencebasedpolicy.pdf (accessed Apr 2010).
- 3. Steinbrook R. Opportunities and challenges for the NIH — an interview with Francis Collins. N Engl J Med 2009; 361: 1321-1323.
- 4. Australian Institute of Health and Welfare. Health expenditure Australia 2006–07. Health and welfare expenditure series No. 35. Canberra: AIHW, 2008. (AIHW Cat. No. HWE 42.) http://www.aihw.gov.au/publications/hwe/hea06-07/hea06-07.pdf (accessed Apr 2010).
- 5. The Treasury, Australian Government. Intergenerational report 2007. Canberra: The Treasury, 2007. http://www.treasury.gov.au/documents/1239/PDF/IGR_2007_final_report.pdf (accessed Apr 2010).
- 6. Fisher ES, Wennberg DE, Stukel TA, et al. The implications of regional variations in Medicare spending. Part 1: the content, quality, and accessibility of care. Ann Intern Med 2003; 138: 273-287.
- 7. Fisher ES, Bynum JP, Skinner JS. Slowing the growth of health care costs — lessons from regional variation. N Engl J Med 2009; 360: 849-852.
- 8. Ham C, York N, Sutch S, et al. Hospital bed utilisation in the NHS, Kaiser Permanente, and the US Medicare programme: analysis of routine data. BMJ 2003; 327: 1257-1261.
- 9. Mendis K. Health informatics research in Australia: retrospective analysis using PubMed. Inform Prim Care 2007; 15: 17-23.
- 10. Sanson-Fisher RW, Campbell EM, Perkins JJ, et al. Indigenous health research: a critical review of outputs over time. Med J Aust 2006; 184: 502-505. <MJA full text>
- 11. Sanson-Fisher RW, Campbell EM, Hunt AT, et al. We are what we do: research outputs of public health. Am J Prev Med 2008; 35: 380-385.
- 12. Stelfox HT, Palmisani S, Scurlock C, et al. The “To Err is Human” report and the patient safety literature. Qual Saf Health Care 2006; 15: 174-178.
- 13. Wilczynski N, Haynes B, Lavis J, et al. Optimal search strategies for detecting health services research studies in MEDLINE. CMAJ 2004; 171: 1179-1185.
- 14. AcademyHealth. Advancing research, policy and practice [Internet]. What is HSR. http://www.academyhealth.org/About/content.cfm?ItemNumber=831&navItemNumber=514 (accessed Apr 2010).
- 15. Haas M. Health services research in Australia: an investigation of its current status. J Health Serv Res Policy 2004; 9 Suppl 2: S3-S9.
- 16. Mendis K, Mclean R. Increased expenditure on Australian health and medical research and changes in numbers of publications determined using PubMed. Med J Aust 2006; 185: 155-158. <MJA full text>
- 17. Public Health Research Advisory Committee. Report of the review of public health research funding in Australia. December 2008. Canberra: National Health and Medical Research Council, 2009. http://www.nhmrc.gov.au/_files_nhmrc/file/research/phr/Nutbeam.pdf (accessed Apr 2010).
- 18. Stetler CB, Mittman BS, Francis J. Overview of the VA quality enhancement research initiative (QUERI) and QUERI theme articles: QUERI Series. Implementation Sci [Internet] 2008; 3(8). http://www.implementationscience.com/content/3/1/8 (accessed Apr 2010).
- 19. Lomas J. Health services research. BMJ 2003; 327: 1301-1302.
- 20. University of Manitoba Faculty of Medicine. Manitoba Centre for Health Policy. http://umanitoba.ca/faculties/medicine/units/mchp/ (accessed Apr 2010).
- 21. Hall JP, Viney RC. National health reform needs strategic investment in health services research. Med J Aust 2008; 188: 33-35. <MJA full text>
- 22. Lomas J. Reaching for the clouds: options for support of health services research in the National Health and Medical Research Council of Australia. Paper prepared for the HSR Working Party of the National Health and Medical Research Council's Research Committee. Canberra: NHMRC, 2003.
- 23. National Health and Medical Research Council. Outcomes of funding rounds. http://www.nhmrc.gov.au/grants/rounds/index.htm (accessed Apr 2010).
- 24. Canadian Institutes of Health Research. Research about — health systems. http://www.cihr.gc.ca/e/40517.html (accessed Apr 2010).
- 25. Anderson WP, Papadakis EM. Research to improve health practice and policy. Med J Aust 2009; 191: 646-647. <MJA full text>
- 26. National Health and Medical Research Council. Strategic plan 2007–2009. Canberra: NHMRC, 2007. http://www.nhmrc.gov.au/_files_nhmrc/file/publications/synopses/strat_plan0709.pdf (accessed Apr 2010).
- 27. Black N. Health services research: the gradual encroachment of ideas. J Health Serv Res Policy 2009; 14: 120-123.
- 28. Cochrane A. Effectiveness and efficiency: random reflections on health services. London: Nuffield Provincial Hospitals Trust, 1972.





Abstract
Objective: To assess how much Australian research is available to inform reform of hospital services.
Design: Bibliographic analysis using a MEDLINE search to locate all research publications focused on the organisation and delivery of Australian hospital services for the period 1996 through 2007.
Main outcome measures: Number of peer-reviewed articles published by year and categorised by: study design (descriptive, methodological, intervention); type of intervention; clinical focus; and funding source.
Results: 679 articles on the organisation and delivery of Australian hospital services were published in peer-reviewed journals from 1 January 1996 to 31 December 2007. Of these, 57% were empirical research reports and 43% were commentaries. There were, on average, 32 empirical research articles per annum. Of the empirical research articles, 70% were descriptive, 23% tested an intervention, and 7% were methodological. Research output increased over time with increases in commentary and descriptive research being the main contributors to this trend. The main funding bodies for this research were universities and government departments.
Conclusion: A small but growing amount of local research is available to support reform of Australian hospital services. To boost the amount of relevant research evidence, we need to: build formal partnerships between researchers, policymakers, clinicians and health service managers; make targeted investment in health systems and services research; and increase the use of routinely collected data for research.