On 11 June 2009, the World Health Organization raised the influenza pandemic alert to Phase 6 (defined as human-to-human spread of the virus in at least two countries in one WHO region and sustained community-level outbreaks in at least one country in another WHO region), in response to the emergence of an A(H1N1) influenza subtype.1
Community mitigation interventions in Australia for pandemic (H1N1) 2009 (“swine flu”) have included identifying cases, treating and isolating infected patients, and quarantine. A great deal of cooperation from the public is required to successfully implement these measures. Unlike our South-East Asian neighbours, Australia has been relatively unaffected by severe acute respiratory syndrome (SARS) or the H5N1 influenza strain, and this may affect how our community responds to pandemic (H1N1) 2009. It has been previously reported that perceptions or beliefs about an outbreak may be important in determining compliance with official advice.2,3 Willingness to adhere may also be influenced by the severity of illness that people observe in the community relative to their own need for income and the potential level of disruption to their lives. In addition, public response is likely to be affected by the perceived effectiveness of the government in dealing with the crisis.4
We sought to rapidly explore initial community feelings and risk perceptions of the pandemic (H1N1) 2009 outbreak in Australia, during a period of scientific uncertainty about the risks and severity of the outbreak. We collected data during Phase 5 of the influenza pandemic alert, from 2 May 2009, when the WHO reported a total of 615 cases from 15 countries,5 to 29 May 2009, by which time 15 510 cases had been reported from 53 countries;6 147 of these cases were reported from Australia, with no related deaths.
A total of 584 community members were approached in person, of whom 499 (85.4%) agreed to participate. A further 26 people who were approached were excluded because of insufficient English proficiency, and another eight were < 18 years of age. The survey was emailed to 197 people, of whom 121 (61.4%) returned a completed survey, giving a total of 620 respondents. Respondents overall were younger than Sydney residents, with 55% of survey respondents aged < 35 years (Box 1) compared with 33% of Sydney residents, as reported in the Australian Bureau of Statistics 2006 census.
Less than half the respondents (41.6%; 258/620) agreed that “health authorities are exaggerating the risk of a pandemic”, and half (51.5%; 319/620) believed that health authorities would be truthful about what was happening during an influenza pandemic. More than half the respondents (57.9%; 359/620) believed that the government would be prepared to quickly and effectively respond to an influenza pandemic. When asked how they thought pandemic influenza would affect their health if they were infected, 42.9% (266/620) stated that it would “very seriously” or “extremely” affect their health (Box 2).
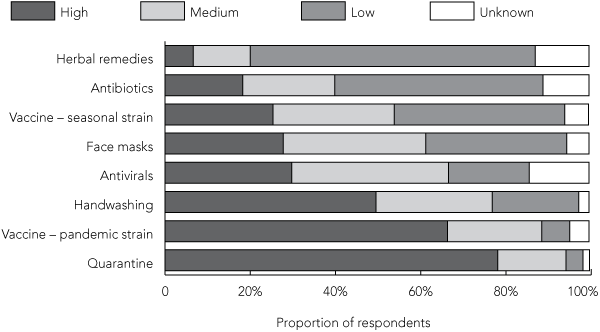
Most respondents (63.4%; 393/620) reported that being placed in home quarantine would constitute a “high” to “very high” inconvenience or problem. Not being able to attend work (52.4%; 325/620) and not having access to groceries and other supplies (40.2%; 249/620) were ranked as highly problematic aspects of quarantine. Respondents who were self-employed or in casual employment were significantly more likely to rate not being able to work as problematic (odds ratio [OR], 1.41 [95% CI, 1.00–1.98]; P = 0.03). Not having access to groceries and other supplies was more problematic for people < 35 years of age compared with older age groups (OR, 1.46 [95% CI, 1.02–2.09]; P = 0.03). Quarantine and vaccination with a pandemic vaccine were rated as more effective than hand hygiene for the prevention of pandemic influenza (Box 3). Women were significantly more likely than men to rate quarantine (OR, 0.64 [95% CI, 0.46–0.89]; P = 0.006) and vaccination with a pandemic vaccine (OR, 0.69 [95% CI, 0.49–0.98]; P = 0.03) as highly effective. This was not the case for handwashing.
Participants were asked to indicate whether or not they would take a prophylactic course of antiviral drugs, or give it away to their family members, in the event that they were exposed to a person with pandemic influenza. Most (69.7%; 432/620) said they would take the course as instructed, while 16.3% (101/620) would divert it to family members.
Despite a rapid increase in the number of pandemic (H1N1) 2009 cases worldwide and the heightened saturation of information about the disease and its spread, few of our respondents believed they were at high to very high risk of contracting pandemic influenza. Our results concur with those of a study that found low levels of anxiety towards swine flu in a cohort in the United Kingdom.7
Risk perceptions are defined by the perceived seriousness of a health threat and perceived personal vulnerability. During the SARS outbreak, willingness to comply with risk-reducing behaviour was linked with perceived immediacy and seriousness of the threat.8,9 Many of the reports in the early stages of the swine flu pandemic described the H1N1 virus as causing milder influenza than other viruses previously linked to pandemics, which may account for the low risk-perception levels in our study. Encouraging the public to undertake specific behaviour relating to hygiene may therefore prove difficult. Previous studies suggest that compliance with health-related recommendations will increase if people believe they have a high likelihood of being affected or they perceive the illness to have severe consequences.3,10
During the SARS outbreak, a Hong Kong study found that people were more likely to comply with health-related recommendations if they believed that the government was providing clear and sufficient information about the outbreak, and that the government could be trusted to control the spread of infection.10 We found a high proportion of respondents believed our government was prepared to respond quickly and effectively to a pandemic situation, which could have positive implications for compliance with official advice.
The high efficacy rating of quarantine in our study is possibly due to intense media coverage of the government using quarantine for suspected cases in Australia at the early stages of the outbreak in Victoria. The high acceptance level may also reflect the media’s presentation of quarantine as being relatively recreational, rather than causing any particular cost other than nuisance for the patient. Fewer than half of our respondents rated hand hygiene as an effective infection prevention measure, with more respondents rating isolation and advances in medical science (such as the development of a pandemic vaccine) above the cornerstone of infectious disease prevention. As the community no longer witnesses the effects of severe infectious diseases, such as polio, the social normative role of hand hygiene should now be reintroduced with large public campaigns.
Our study has several limitations. First, it was conducted in one city and was limited to English-speaking participants. Additional research into differing reactions to the outbreak among other ethnic groups is required. Second, our study sample has the potential to be biased towards community members who are particularly concerned about pandemic influenza. Our survey measured a specific population’s views at a specific point in time; their beliefs and attitudes reflect the information available at the time and will not be stable. It is unknown whether responses given to the hypothetical situations posed in the survey would accurately reflect the respondents’ real-world responses. However, behavioural intention-focused research indicates the potential for intentions to reasonably predict actual behaviour.11
Our respondents were largely cooperative and supportive of the government’s ability to handle the pandemic. Where they were being failed was in the lack of provision of structured routine updates on the pandemic and lessons on the importance of basic personal hygiene for the containment of respiratory infections.
1 Demographic characteristics of the participants (n = 620)
Characteristic |
No. (%) |
||||||||||||||
Sex |
|
||||||||||||||
Male |
266 (42.9%) |
||||||||||||||
Female |
346 (55.8%) |
||||||||||||||
Not specified |
8 (1.3%) |
||||||||||||||
Age group (years) |
|
||||||||||||||
18–24 |
129 (20.8%) |
||||||||||||||
25–34 |
209 (33.7%) |
||||||||||||||
35–44 |
97 (15.6%) |
||||||||||||||
45–54 |
87 (14.0%) |
||||||||||||||
55–64 |
69 (11.1%) |
||||||||||||||
≥ 65 |
23 (3.7%) |
||||||||||||||
Not specified |
6 (1.0%) |
||||||||||||||
Home/living arrangements |
|
||||||||||||||
Live with partner/spouse |
184 (29.7%) |
||||||||||||||
Live with partner/spouse and children |
134 (21.6%) |
||||||||||||||
Live in shared accommodation |
95 (15.3%) |
||||||||||||||
Live with parents |
88 (14.2%) |
||||||||||||||
Live alone |
84 (13.5%) |
||||||||||||||
Other |
24 (3.9%) |
||||||||||||||
Not specified |
11 (1.8%) |
||||||||||||||
Highest qualification |
|
||||||||||||||
University degree/equivalent |
397 (64.0%) |
||||||||||||||
TAFE certificate/diploma |
116 (18.7%) |
||||||||||||||
Higher school certificate |
71 (11.5%) |
||||||||||||||
School certificate |
20 (3.2%) |
||||||||||||||
None |
9 (1.5%) |
||||||||||||||
Not specified |
7 (1.1%) |
||||||||||||||
Ethnic background |
|
||||||||||||||
Caucasian |
467 (75.3%) |
||||||||||||||
Asian |
90 (14.5%) |
||||||||||||||
Other |
29 (4.7%) |
||||||||||||||
Middle Eastern |
26 (4.2%) |
||||||||||||||
Aboriginal or Torres Strait Islander |
1 (0.2%) |
||||||||||||||
Not specified |
7 (1.1%) |
||||||||||||||
Employed |
|
||||||||||||||
No |
113 (18.2%) |
||||||||||||||
Full time |
331 (53.4%) |
||||||||||||||
Part time |
57 (9.2%) |
||||||||||||||
Casual |
64 (10.3%) |
||||||||||||||
Self-employed |
51 (8.2%) |
||||||||||||||
Not specified |
4 (0.6%) |
||||||||||||||
TAFE = Technical and Further Education. |
|||||||||||||||
2 Participant awareness and perceived risk of swine flu and pandemic influenza (n = 620)
Question and response |
No. (%) |
||||||||||||||
Are you aware of the swine flu situation? |
|||||||||||||||
Yes |
596 (96.1%) |
||||||||||||||
No |
10 (1.6%) |
||||||||||||||
No response |
14 (2.3%) |
||||||||||||||
Do you feel that you currently have enough information about the swine flu situation? |
|||||||||||||||
Yes |
338 (54.5%) |
||||||||||||||
No |
273 (44.0%) |
||||||||||||||
No response |
9 (1.5%) |
||||||||||||||
How long do you think a pandemic will last? |
|||||||||||||||
< 1 month |
16 (2.6%) |
||||||||||||||
1–2 months |
110 (17.7%) |
||||||||||||||
3–6 months |
141 (22.7%) |
||||||||||||||
6 months – 1 year |
93 (15.0%) |
||||||||||||||
1–2 years |
27 (4.4%) |
||||||||||||||
> 2 years |
19 (3.1%) |
||||||||||||||
Unsure |
152 (24.5%) |
||||||||||||||
Other |
34 (5.5%) |
||||||||||||||
No response |
28 (4.5%) |
||||||||||||||
If you were infected by pandemic influenza, how seriously do you think it would affect your health? |
|||||||||||||||
Not at all |
7 (1.1%) |
||||||||||||||
Somewhat affect |
275 (44.4%) |
||||||||||||||
Very seriously affect |
206 (33.2%) |
||||||||||||||
Extremely affect |
60 (9.7%) |
||||||||||||||
Don’t know |
72 (11.6%) |
||||||||||||||
Please indicate your level of risk of catching influenza during a pandemic |
|||||||||||||||
Very high |
35 (5.6%) |
||||||||||||||
High |
98 (15.8%) |
||||||||||||||
Medium |
201 (32.4%) |
||||||||||||||
Low |
156 (25.2%) |
||||||||||||||
Very low |
79 (12.7%) |
||||||||||||||
Don’t know |
51 (8.2%) |
||||||||||||||
- Holly Seale1
- Mary-Louise McLaws1
- Anita E Heywood1
- Kirsten F Ward2
- Chris P Lowbridge3
- Debbie Van4
- Jan Gralton1
- C Raina MacIntyre1
- 1 School of Public Health and Community Medicine, Faculty of Medicine, University of New South Wales, Sydney, NSW.
- 2 General Practice NSW, Sydney, NSW.
- 3 Public Health Unit, Sydney South West Area Health Service, Sydney, NSW.
- 4 Faculty of Medicine, University of New South Wales, Sydney, NSW.
We would like to thank Associate Professor Heather Worth for her assistance and advice on this project.
Raina MacIntyre receives funding from influenza vaccine manufacturers GlaxoSmithKline and CSL Biotherapies for investigator-driven research. However, these payments were not used for this study.
- 1. International Society for Infectious Diseases. ProMED-mail Archive Number 20090425.1557. PRO/AH/EDR> Influenza A (H1N1) virus, human - N America (02). 25 Apr 2009. http://www.promedmail.org/pls/otn/f?p=2400: 1001:1432717334138957::::F2400_P1001_BACK_PAGE,F2400_P1001_ARCHIVE_NUMBER,F2400_P1001_USE_ARCHIVE:1001,200 90425.1557,Y (accessed May 2009).
- 2. Lau JTF, Yang X, Tsui H, Kim JH. Monitoring community responses to the SARS epidemic in Hong Kong: from day 10 to day 62. J Epidemiol Community Health 2003; 57: 864-870.
- 3. Tang CS-K, Wong C-Y. An outbreak of the severe acute respiratory syndrome: predictors of health behaviors and effect of community prevention measures in Hong Kong, China. Am J Public Health 2003; 93: 1887-1888.
- 4. Blendon RJ, Koonin LM, Benson JM, et al. Public response to community mitigation measures for pandemic influenza. Emerg Infect Dis 2008; 14: 778-786.
- 5. World Health Organization. Influenza A(H1N1) – update 9. 2 May 2009. http://www.who.int/csr/don/2009_05_02/en/index.html (accessed Jun 2009).
- 6. World Health Organization. Influenza A(H1N1) – update 41. 29 May 2009. http://www.who.int/csr/don/2009_05_29/en/index.html (accessed Jun 2009).
- 7. Rubin GJ, Amlot R, Page L, Wessely S. Public perceptions, anxiety, and behaviour change in relation to the swine flu outbreak: cross sectional telephone survey. BMJ 2009; 339: b2651.
- 8. Cava MA, Fay KE, Beanlands HJ, et al. Risk perception and compliance with quarantine during the SARS outbreak. J Nurs Scholarsh 2005; 37: 343-347.
- 9. Leung GM, Ho L-M, Chan SKK, et al. Longitudinal assessment of community psychobehavioral responses during and after the 2003 outbreak of severe acute respiratory syndrome in Hong Kong. Clin Infect Dis 2005; 40: 1713-1720.
- 10. Tang CS-K, Wong C-Y. Factors influencing the wearing of facemasks to prevent the severe acute respiratory syndrome among adult Chinese in Hong Kong. Prev Med 2004; 39: 1187-1193.
- 11. Wroe AL, Turner N, Salkovskis PM. Understanding and predicting parental decisions about early childhood immunizations. Health Psychol 2004; 23: 33-41.





Abstract
Objective:
Design, setting and participants: Cross-sectional survey of Sydney residents during WHO Phase 5 of pandemic (H1N1) 2009. Members of the public were approached in shopping and pedestrian malls in seven areas of Sydney between 2 May and 29 May 2009 to undertake the survey. The survey was also made available by email.
Main outcome measures: Perceived personal risk and seriousness of the disease, opinion on the government and health authorities’ response, feelings about quarantine and infection control methods, and potential compliance with antiviral prophylaxis.
Results: Of 620 respondents, 596 (96%) were aware of pandemic (H1N1) 2009, but 44% (273/620) felt they did not have enough information about the situation. More than a third (38%; 235/620) ranked their risk of catching influenza during a pandemic as low. When asked how they felt pandemic influenza would affect their health if they were infected, only a third (33%; 206/620) said “very seriously”. Just over half of the respondents (58%; 360/620) believed the pandemic would be over within a year. Respondents rated quarantine and vaccination with a pandemic vaccine as more effective than hand hygiene for the prevention of pandemic influenza.
Conclusions: Emphasising the efficacy of recommended actions (such as hand hygiene), risks from the disease and the possible duration of the outbreak may help to promote compliance with official advice.