Adverse events in health care are common.1,2 Most current knowledge of adverse events is based on reviews of hospital medical records,1,2 incident reports by health staff3,4 or analysis of administrative databases.5 These approaches each have strengths, but also inherent biases and weaknesses,5,6 as many events will go unreported and unrecorded.7 Comparatively little is known about adverse events outside hospitals, although some evidence suggests they may be a significant contributor to harm in health care.8
Health care consumers are a relatively underused source of information about adverse events9 and about their views about such events. This underuse occurs despite evidence of consumers’ capability in noticing adverse events.9,10 Patient satisfaction surveys tend not to focus on adverse events so much as problems with interpersonal interactions or the delivery of care, and are most commonly conducted among inpatients.
An Australian population survey in 2000 reported an annual incidence of adverse events causing harm of 6.5% among adults in the community;11 these results are similar to those of a United States study.12 However, the Australian study’s low response rate of 43% raises concerns about response bias. It is unclear whether the rate of occurrence of adverse events has changed since the 2000 survey,11 in the wake of well publicised scandals13 and with the increased focus among clinicians, health care providers and policymakers on patient safety.13
We examined the incidence of self-reported adverse events causing harm in health care within a representative population sample of community-dwelling adults. We also used survey items from the previous Australian survey11 to examine attitudes about the performance of the health system in relation to safety.
In 2000, 4060 adults (1988 men and 2072 women; 69.4% of those who completed the initial interview) attended the clinic for biomedical examination. In 2004 and 2005, all participants were contacted again to be interviewed in Stage 2 of the NWAHS; 3522 (86.7%) completed these interviews, which provide the data for this study. The methods of the NWAHS,14 and the validity of these methods of selection in achieving an unbiased sample have been described previously.15
Our survey of health care experiences replicated the items used in a 2000 Australian study,11 which in turn was based on an earlier survey from the National Patient Safety Foundation at the American Medical Association.12
These next questions are about your experience of ANY medical adverse events or incidents arising from your health care that had the potential or did lead to unintended personal harm. These are things that may have gone wrong in hospital, at a doctor’s surgery, having x-rays or pathology tests, or in a related health setting like a pharmacy.
Some further examples were given:
. . . a wrong dose of medicine is given; uncontrolled pain after a procedure; results of pathology tests are lost or overlooked; an operation that was performed other than what was intended for the patient; a fall while in hospital or at home due to drug treatment; injury or adverse effects from treatment or medication other than known side effects; taking medication that made you sick.
Respondents also completed questionnaires on their use of health services (including their satisfaction with recent care), and on their health insurance status. A 6-item scale designed to assess an individual’s level of risk aversion asked respondents to consider how risky they considered various behaviours, such as not testing smoke detectors regularly, smoking tobacco products, and driving after consuming alcohol.11
Data were weighted to the estimated South Australian population in 199916 and 2001 Census data17 by region, age group, sex and probability of selection in the household, to account for differential non-response and provide population-representative estimates. Data were analysed with SPSS, version 13.0 (SPSS Inc, Chicago, Ill, USA). Univariate and multivariate logistic regression was used to model independent variables associated with adverse events.
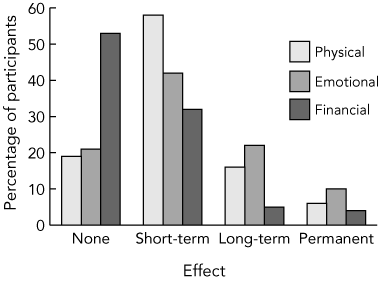
The impact of perceived harmful adverse events over time in physical, emotional and financial terms is shown in Box 1. Most of those experiencing a harmful adverse event (58%) described short-term physical effects, although 22% felt they had long-term or permanent effects. Regarding emotional consequences, 32% reported they had long-term or permanent effects from an adverse event. Short-term financial effects were felt by 32%, longer-term or permanent effects were reported by 9%.
In multiple logistic regression models people were significantly more likely to report experiencing harmful adverse events in the past year if they had been hospitalised in that year, had some level of dissatisfaction with their recent health care, reported a tendency to risk-taking behaviour compared with those more risk-averse, and if they had low income or completed higher education (Box 2). Age was not a significant variable.
Among all 3522 respondents, 18.6% thought safety for patients in the Australian health care system had improved over the past 5 years, 40.9% thought it had stayed the same and 28.4% felt it had become worse. Those who were dissatisfied with their last medical encounter were significantly more likely to believe the system had become worse compared with others (51% v 31%; P < 0.05). Young people (aged 20–34 years) were more likely to believe the system had not changed, middle-aged people (aged 35–54 years) to believe it had become worse, and older people to believe it had improved. The issues identified by respondents as coming to mind when thinking about the safety of patients in the Australian health care system are shown in Box 3. In general, older people were more likely than younger people to identify specific issues, such as exposure to infection. Younger age groups were more likely to list more general factors as issues, such as misdiagnosis.
When asked if they agreed if the current health care system had adequate measures in place to prevent adverse events, 43.2% reported they did not know. Two-thirds of respondents (66.9%) said they would report an adverse event if they experienced it, and only 5.4% said they would not report. Most (64.3%) felt somewhat or very confident that reporting an adverse event would remedy the situation, but 26.1% were not confident about that. When indicating the effect that groups potentially involved in their health care had on their safety as a patient, respondents were more likely to consider individual health professionals to have a positive effect than organisations or governments (Box 4). The only groups respondents thought significantly more likely to have a negative effect on their safety were health insurance companies (22.9% of respondents) and governments (28.2% of respondents).
Suggestions for how to improve the safety of health care for people in Australia focused largely on increasing resources (67.7% of responses). Suggestions included more funding (19.0%), increased staff numbers (34.9%), more beds or better access (5.5%), and more training of health care staff (8.3%). More information and better communication with people as patients was suggested by 8.6%, with only 1.0% suggesting people should be taking more responsibility for their own health and safety.
This study provides a recent picture of what a representative Australian population sample reports about the safety of their health care. The annual incidence of harmful adverse events as perceived by participants in our study was significantly lower than those in earlier Australian and US studies that used identical questions.11,12 Harmful adverse events have consequences that linger, with nearly a third of the respondents in our study who reported adverse events causing harm reporting long-term or permanent emotional effects, and over 20% describing long-term physical consequences.
The likelihood of experiencing harm from an adverse event over the past year was independently related to recent hospitalisation in that year, suggesting an increased risk associated with more complex disease and treatment. These findings further justify the focus of efforts to reduce adverse events in hospitals, and after discharge from hospital, as appropriate.18 Some individual characteristics (but not age) also influenced the association with reporting adverse events. Participants with either low income or higher education reported more adverse events. Higher education may increase the chances of individuals recognising problems with their care, or alternatively may be associated with increased expectations of care processes and outcomes.
The other independent factor associated with adverse events was a tendency to risk-taking behaviour. Such behaviour is associated with an increased chance of injury in different contexts.19 Willingness to take risks differs with context. However, the correlation across contexts is strong, suggesting that a single trait of risk-taking attitude exists.20,21 There is evidence to indicate that differences that exist across situational contexts are more likely to be differences in risk perception than in risk preferences.21 The significance of this for practitioners and the health care system lies in the potential for altering risk perception and risk-taking behaviour by improving communication. Communicating in a way that focuses on improving patients’ ability to perceive risk more accurately might reduce the incidence of adverse events. This may be as simple as clinicians and patients actively discussing and acting on such things as medication-related symptoms.22
Recall bias in the reporting of adverse events may also have been a limitation of our study. The level of satisfaction with recent health care was significantly related to the reporting of adverse events. We do not have data to infer the direction of causality — that is, does an adverse event reduce satisfaction with care, or are those less satisfied more likely to notice or perceive experiences as adverse events? However, previous studies have shown patient reports of problems are similar to those found from other data collection methods.23 A combination of underreporting by some patients and overreporting by others may account for this concordance.
Substantial variation can exist between event rates estimated from different sources of external data, such as medical records, staff incident reports or administrative databases.24 Patient reports thus become an alternative view on system quality, and allow us to identify potential target areas for intervention. Self-reports provide opportunities to explore patients’ perceptions of their care and the health system in collaborative reflective dialogue.
Our study was also subject to potential bias from survey non-response, although response rates in our sample were relatively high.25 In particular, there were no major differences between NWAHS participants and the general population in terms of health indicators or lifestyle behaviours.26 The strength of our study is the large representative population sample from which we obtained self-reported adverse events, covering both inpatient and ambulatory care.
A recent report indicated that Australians trusted their general practitioner more than other people involved in the health care system.27 The issue of the importance of trust placed in an individual has a corollary in the attitudes expressed about which groups affect patient safety. People were more likely to consider individual health care professionals as having a positive effect on safety than professional groups or those overseeing the health care system (eg, governments). Also, most respondents indicated that more resources were the key to improving the safety of health care. The converse of this can be seen in the views expressed about problem issues in health, which were focused around negligence and getting the right treatment. Again, this reflects a view that responsibility lies mostly with the individual health care professional rather than in systems improvement.
Despite many articles in the professional literature,28 there has been relatively little in the way of public health campaigns that put the view that systems change is the key to patient safety. Public discourse has often focused on the “bad apples” notion of safety, as evidenced by the publicity surrounding a small number of notorious cases.13,28 Some jurisdictions are advocating incident reporting and public reporting of health care outcomes in hospitals as a means of shifting the focus away from individual blame and onto the action being taken to improve hospitals’ performance.29 However, despite widespread acceptance in health care circles,5,13,28 a general public and political consensus has not been reached that supports a systems approach to patient safety. We feel it is time that professional bodies and public health care workers take up the task of informing and engaging with consumers to build a consensus to exert political pressure, so that systems improvement will eventually lead safety improvement.
1 Perceived physical, emotional and financial effects among the 148 participants who reported adverse events causing harm
2 Prevalence and multivariable logistic regression model of factors associated with self-reported adverse events over the past 12 months among 3522 participants in Stage 2 of the North West Adelaide Health Study
3 Percentage of the 3522 participants in Stage 2 of the North West Adelaide Health Study indicating issues that came to mind about safety for patients in the Australian health care system, by age group*
Received 28 September 2008, accepted 21 December 2008
- Robert J Adams1
- Graeme Tucker2
- Kay Price3
- Catherine L Hill1
- Sarah L Appleton1
- David H Wilson1
- Anne W Taylor2
- Richard E Ruffin1
- 1 Health Observatory, Discipline of Medicine, University of Adelaide, Adelaide, SA.
- 2 South Australian Department of Health, Adelaide, SA.
- 3 School of Nursing and Midwifery, University of South Australia, Adelaide, SA.
None identified.
- 1. Wilson RM, Runciman WB, Gibberd RW, et al. The Quality in Australian Health Care Study. Med J Aust 1995; 163: 458-471. <MJA full text>
- 2. Brennan TA, Leape LL, Laird NM, et al. Incidence of adverse events and negligence in hospitalized patients. Results of the Harvard Medical Practice Study I. N Engl J Med 1991; 324: 370-376.
- 3. Runciman WB, Sellen A, Webb RK, et al. The Australian Incident Monitoring Study. Errors, incidents and accidents in anaesthetic practice. Anaesth Intensive Care 1993; 21: 506-519.
- 4. Weingart SN, Callanan LD, Ship AN, Aronson MD. A physician-based voluntary reporting system for adverse events and medical errors. J Gen Intern Med 2001; 16: 809-814.
- 5. Scott IA, Ward M. Public reporting of hospital outcomes based on administrative data: risks and opportunities. Med J Aust 2006; 184: 571-575. <MJA full text>
- 6. Murff HJ, Patel VL, Hripcsak G, Bates DW. Detecting adverse events for patient safety research: a review of current methodologies. J Biomed Inform 2003; 36: 131-143.
- 7. Waring JJ. A qualitative study of the intra-hospital variations in incident reporting. Int J Qual Health Care 2004; 16: 347-352.
- 8. Woods DM, Thomas EJ, Holl JL, et al. Ambulatory care adverse events and preventable adverse events leading to a hospital admission. Qual Saf Health Care 2007; 16: 127-131.
- 9. Vincent CA, Coulter A. Patient safety: what about the patient? Qual Saf Health Care 2002; 11: 76-80.
- 10. Agoritas T, Bovier PA, Perneger TV. Patient reports of undesirable events during hospitalization. J Gen Intern Med 2005; 20: 922-928.
- 11. Clark RB. Australian Patient Safety Survey. Health Issues 2001; 69: 20-24.
- 12. National Patient Safety Foundation at the AMA [American Medical Association]. Public opinion of patient safety issues. Research findings. Boston: National Patient Safety Foundation, September 1997. http://www.npsf.org/pdf/r/1997survey.pdf (accessed Mar 2009).
- 13. Van Der Weyden MB. The Bundaberg Hospital scandal: the need for reform in Queensland and beyond [editorial]. Med J Aust 2005; 183: 284-285. <MJA full text>
- 14. Grant JF, Chittleborough CR, Taylor AW, et al. The North West Adelaide Health Study: detailed methods and baseline segmentation of a cohort for selected chronic diseases. Epidemiol Perspect Innov 2006; 3: 4.
- 15. Taylor A, Wilson DH, Wakefield M. Differences in health estimates using telephones and door-to-door survey methods — a hypothetical exercise. Aust N Z J Public Health 1998; 22: 223-226.
- 16. Australian Bureau of Statistics. Estimated resident population by age and sex in statistical local areas, Australia: data on floppy disk, Jun 1999. Canberra: ABS, 2000 (release date). (ABS Cat. No. 3227.0.)
- 17. Australian Bureau of Statistics. Census of population and housing: selected social and housing characteristics for statistical local areas, South Australia, 2001. Canberra: ABS, 2002. (ABS Cat. No. 2015.4.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/ProductsbyCatalogue/12A222C3B7BD5AC9CA256C310082CB94?OpenDocument (accessed Mar 2009).
- 18. Schoen C, Osborn R, Huynh PT, et al. Taking the pulse of health care systems: experiences of patients with health problems in six countries. Health Aff (Millwood) 2005; Jul-Dec Suppl Web Exclusives: W5-509-W5-525.
- 19. Turner C, McClure R, Pirozzo S. Injury and risk-taking behaviour — a systematic review. Accid Anal Prev 2004; 36: 93-101.
- 20. Weber EU, Blais AR, Betz NE. A domain-specific risk-attitude scale: measuring risk perceptions and risk behaviours. J Behav Dec Making 2002; 15: 263-290.
- 21. Dohman T, Falk A, Huffman D, et al. Individual risk attitudes: new evidence from a large, representative, experimentally-validated survey. Bonn: Institute for the Study of Labor (IZA), September 2005. (IZA Discussion Paper No. 1730.) http://ftp.iza.org/dp1730.pdf (accessed Mar 2009).
- 22. Weingart SN, Gandhi TK, Seger AC, et al. Patient-reported medication symptoms in primary care. Arch Intern Med 2005; 165: 234-240.
- 23. Weingart SN, Pagovich O, Sands DZ, et al. What can hospitalized patients tell us about adverse events? Learning from patient-reported incidents. J Gen Intern Med 2005; 20: 830-836.
- 24. Runciman WB, Roughhead EE, Semple SJ, Adams RJ. Adverse drug events and medication errors in Australia. Int J Qual Health Care 2003; 15 Suppl 1: i49-i59.
- 25. Dunstan DW, Zimmet PZ, Welborn TA, et al; Australian Diabetes, Obesity and Lifestyle Study (AusDiab). The Australian Diabetes, Obesity and Lifestyle Study (AusDiab) methods and response rates. Diabetes Res Clin Pract 2002; 57: 119-129.
- 26. Taylor AW, Dal Grande E, Gill T, et al. Do people with risky behaviours participate in biomedical cohort studies? BMC Public Health 2006; 6: 11.
- 27. Hardie EA, Critchley CR. Public perceptions of Australia’s doctors, hospitals and health care systems. Med J Aust 2008; 189: 210-214. <MJA full text>
- 28. Wilson RMcL, Van Der Weyden MB. The safety of Australian healthcare: 10 years after QAHCS [editorial]. Med J Aust 2005; 182: 260-261. <MJA full text>
- 29. Duckett SJ, Collins J, Kamp M, Walker K. An improvement focus in public reporting: the Queensland approach. Med J Aust 2008; 189: 616-617. <MJA full text>





Abstract
Objectives: To identify the incidence of self-reported harmful adverse events in the health care of community-dwelling adults, and to examine attitudes about safety in the health system.
Design: Cross-sectional, population-based survey.
Participants and setting: Analysis of data from 3522 adults participating in Stage 2 of the North West Adelaide Health Study, who were surveyed in 2004 and 2005.
Main outcome measures: Self-reported adverse events causing harm in the past year; attitudes to safety in health care, including adequacy of current measures for preventing adverse events, and the effect of groups like patients themselves, doctors and governments on patient safety.
Results: The annual incidence of self-reported harmful adverse events was 4.2%. The main types were medication error (45.5%) and misdiagnosis or wrong treatment (25.6%). Multiple logistic regression showed that self-reported harmful adverse events were more likely in people who had been hospitalised in the past 12 months (odds ratio [OR], 2.5; 95% CI, 1.9–3.4), those who had low annual income (< $12 000), those who completed higher education to the level of Bachelor degree or higher (OR, 3.0; 95% CI, 1.0–9.4), and those who had some level of dissatisfaction with their recent health care; and less likely in those more risk-averse rather than those with a tendency to risk-taking behaviour (OR, 0.6; 95% CI, 0.4–0.9). People were more likely to believe that individual health care professionals had a positive effect on safety than professional groups or government, and that more resources were the key to improving the safety of health care.
Conclusion: We found an incidence of self-reported harmful adverse events that was significantly lower than that found by a 2002 Australian survey (4.2% v 6.5%; P = 0.009). Better communication to help patients acquire more realistic risk perception may help reduce harm. Better communication could also increase public advocacy for systems improvement in safety to counter persisting community beliefs that individual action alone can redress the situation.