The number of bicyclists in Victoria is increasing,1-3 and cycling is the fourth most popular physical activity for Australians over the age of 16 years.2 Bicycle sales have outnumbered car sales for the past 9 years4 but, as there is no bicycle registration in Australia, the number of people who own and ride bicycles is largely unknown. Further, the data on cycling participation rates are available for selected years only.5
Despite the increasing number of bicyclists in Victoria, the number of reported bicycle casualty accidents does not seem to have changed substantially between 2002 and 2007.6 Controversy about the requirement for all cyclists to wear helmets continues,7 but the 1990 legislation making helmets compulsory for bicyclists in Victoria was associated with a decrease in non-fatal head injuries and fatalities.8-10 Several authors have called for more comprehensive strategies to prevent serious bicycle injuries, including separation of bicyclists from motor vehicle lanes and greater regulation of bicyclists’ behaviour and interaction with other road users.11-14
The state of Victoria has a population of over 5 million people, accounting for 24% of all Australians. Most of the population is concentrated in one large metropolitan area with 3.8 million people.15
Data on all patients who presented to the EDs of Victorian public hospitals after a bicycle-related injury were obtained from the VEMD. It has been estimated that more than 80% of ED presentations in the state are captured by the VEMD, and it has been found to be a reliable and valid database.16 Patients were included if a cause of injury was riding a bicycle or if a description of the injury event indicated a bicycle was involved. Only those not admitted to hospitals were included. Summary tables for the VEMD were provided by Monash University Accident Research Centre (ie, we did not use the raw data).
Data on all patients who were admitted to a Victorian public or private hospital after a bicycle-related injury were obtained from the VAED. The VAED contains data about all hospital admissions in Victoria.17 Patients were selected if the external cause-of-injury code was in the range V10–V19, referring to a bicyclist. As with the VEMD, summary tables for the VAED were provided by Monash University Accident Research Centre and we did not use raw data.
The VSTR is a statewide population-based trauma registry which includes prospectively collected data on all hospitalised major trauma patients in Victoria. The inclusion criteria for the VSTR have been described previously and include any of the following: death due to injury, an Injury Severity Score > 15, urgent surgery, and an intensive care unit stay longer than 24 hours requiring mechanical ventilation.18 The VSTR provides high-quality data as a result of its quality assurance policy including, among other things, date and time validation checks built into the web-based database.19 Demographic data, injury event details, clinical observations, management and outcomes were extracted for analysis.
Population estimates for Victoria were obtained from the Australian Bureau of Statistics.15 Descriptive statistics were used to summarise the profiles of ED presentations, hospital admissions, major trauma cases and deaths. We reported categorical data as percentages and 95% confidence intervals (CIs). For the coroners data, exact binomial CIs were calculated because of the small sample size. Continuous data were reported as median and interquartile range. Population-based incidence rates (95% CIs) were calculated for each 12-month period, based on the total population at the end of June 2002, 2003, 2004, 2005 and 2006. A Poisson regression model was used to test for a dose–response effect of increasing incidence over the 5 years by assuming a linear increase in the logarithm of the rate with increasing years.
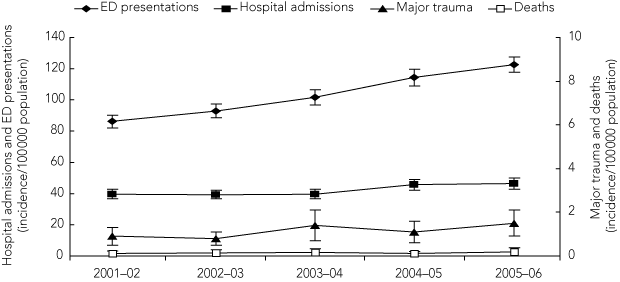
The incidence of bicycle-related injury increased over the 5-year period (Box 1): bicycle-related ED presentations rose from 86 to 122 per 100 000 population (incidence rate ratio [IRR] = 1.42; 95% CI, 1.37–1.48; P < 0.001); and bicycle-related hospital admissions rose from 40 to 46 per 100 000 population (IRR = 1.16; 95% CI, 1.09–1.23; P < 0.001). Data from the VSTR are consistent with this trend: bicycle-related major trauma cases increased from 1.0 per 100 000 population in 2001 to 1.5 per 100 000 population in 2006 (IRR = 1.76; 95% CI, 1.22–2.55; P = 0.002). A 37% rise in bicycle-related deaths was observed, although this increase in incidence was not significant (IRR = 1.58; 95% CI, 0.57–4.34; P = 0.375).
Irrespective of the data source, most patients injured in bicycle-related incidents were male and most were aged under 35 years (Box 2). Bicycle fatalities were more evenly distributed across the age groups, but 55% of fatally injured cyclists were aged over 35 years.
Most severe injuries occurred on streets or highways, but almost half of the less severe cases occurred elsewhere (Box 2). Bicycle-related major trauma most commonly occurred on a Sunday, and usually between 1:00 pm and 4:00 pm. Most fatal injuries occurred between 5:00 am and 8:00 am and 5:00 pm and 8:00 pm, which are peak traffic periods.
Our population-based study found that ED presentations and hospital admissions for bicycle injuries increased significantly from 2001 to 2006. There was also a marked increase in cyclists sustaining major trauma. Our findings of an average of about 5200 ED presentations a year for bicycle injuries (just over half from road collisions), contrasts with Victoria’s probably under-reported road-crash data, showing about 1200 bicycle casualty accidents per year.6 On the other hand, our use of hospital-based data, excluding injuries treated by general practitioners, may have underestimated the burden of bicycle injuries.
Consistent with previous reports,11,20,21 injured bicycle riders were predominantly young men, but the relative burden of major trauma cases and fatalities seemed to increase with age. In the major trauma and fatality groups, head injuries were the most common injury, consistent with previous studies.12,19,20,22
Wearing an approved safety helmet substantially reduces the risk of serious head injury in cyclists who fall or are involved in collisions with motor vehicles.10,12,23 A prospective study of 1710 bicycle casualties in Victoria, 1987–1989, before the introduction of compulsory helmet wearing, found that the 21% wearing an approved helmet had overall at least a 39% reduced risk of head injury and significantly less frequent severe head injuries.10 Recent anecdotal evidence suggests less compliance with helmet laws. However, of the 30 cyclists with a fatal injury for whom coronial data were available, 23 (77%) wore a helmet, a proportion consistent with a 1994 Victorian survey of helmet wearing.8 Updated statistics on helmet-law compliance are needed. Injuries to the extremities, although not life-threatening, were common among ED and hospital presentations and often involved long-term morbidity,24 so strategies to target these injuries are also needed.
Most serious injuries occur on streets or highways.25 Separation of bicyclists from cars results in fewer injuries.11,13,14 Our study presents data on when (VSTR) and where (all datasets) most collisions occurred, and could be used as a guide to where designated bicycle paths should be provided, and then their utility and impact on cyclists’ safety could be monitored. However, geographical, economic (and political) considerations often hinder provision of cycle paths. An alternative solution — restricting access for bicycle riders to major roads with high-speed vehicles, especially in peak periods — may not be well received by cyclists.
Research is needed on alcohol use by cyclists.11,21 Davidson found that over 60% of cyclists injured at night had consumed alcohol.11 As bicycle-related crashes may not always be reported to police,26,27 blood-alcohol tests may not be performed and the role of alcohol use in accidents ignored.
There is a need for greater community awareness of cyclists. Motorists need to be educated about safely sharing the road, and cyclists informed about potentially risky behaviours. The numerous bike organisations across Victoria could convey messages to their members, but bicyclists most at risk may not be members of these organisations. Indeed, most bicyclists are involved in non-organised cycling activities.5
As 55% of the fatally injured cyclists were aged over 35 years, education and prevention strategies should target this age group. In overseas studies,28 and Australian studies before helmet wearing was made compulsory,8,29,30 prevention strategies emphasised the importance of helmet-wearing. In Australia, further data are needed to identify factors other than helmet-wearing that contribute to preventing cycling injuries. These might include cycling skills and training in cycle riding, bicycle design, clothing, bicycle-path engineering, education of motorists, and other factors. Establishment of a reliable registry of bicycle participants would assist in understanding and improving cyclists’ road safety.
Bicycle accidents causing minor injuries are likely to be under-reported,12,26 and minor injuries would be dealt with by GPs. As no GP registry for such injuries exists, these data were not included. Thus, another important limitation is that not all minor injuries were included.
Received 25 August 2008, accepted 10 December 2008
- Mirjana Sikic1
- Antonina A Mikocka-Walus2
- Belinda J Gabbe2
- Francis T McDermott3
- Peter A Cameron1,2
- 1 Emergency Department, Alfred Hospital, Melbourne, VIC.
- 2 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
- 3 Department of Surgery, Monash University, Melbourne, VIC.
The VSTR is a Department of Human Services and Victorian Trauma Foundation funded and approved initiative. Belinda Gabbe is supported by a Career Development Award (465103) from the National Health and Medical Research Council (NHMRC). We thank Andrew Hannaford and Sue McLellan for their assistance with extracting data from the VSTR and the NCIS.
None identified.
- 1. Amy Gillett Foundation 2006–07 Annual report. Melbourne: Amy Gillett Foundation, 2007. http://www.amygillett.org.au/documents/AGF_Annual_Report_06_07.pdf (accessed Aug 2008).
- 2. Bauman A, Rissel C, Garrard J, et al. Cycling. Getting Australia moving. Barriers, facilitators and interventions to get more Australians physically active through cycling. Melbourne. Cycling Promotion Fund, 2008. http://www.cyclingpromotion.com.au/images/stories/downloads/CPFHlthRpr08V3prf1.pdf (accessed Aug 2008).
- 3. Bicycle Victoria. Census 2006. More people cycling more often! http://www.bv.com.au/change-the-world/40905/ (accessed Aug 2008).
- 4. Cycling Promotion Fund. Bicycle sales 2008. Melbourne: CPF, 2008. http://www.cyclingpromotion.com.au/images/stories/factsheets/CPFBikeSales08.pdf (accessed Jan 2009).
- 5. Australian Bureau of Statistics. Sports and physical recreation: a statistical overview, Australia, 2008 (Edition 2). Canberra: ABS, 2008. (Catalogue No. 4156.0.) http://www.abs.gov.au/ausstats/abs@.nsf/Products/C06A24F23644AD12CA2574D6001738AA?opendocument (accessed Apr 2008).
- 6. Vic Roads. Bicycle casualty accidents in Victoria by age in 2002–2007. Melbourne: Vic Roads, 2008. http://crashstat1.roads.vic.gov.au/crashstats/crash.htm (accessed Jan 2009).
- 7. Curnow WJ. The Cochrane Collaboration and bicycle helmets. Accid Anal Prev 2005; 37: 569-573.
- 8. Cameron MH, Vulcan AP, Finch CF, Newstead SV. Mandatory bicycle helmet use following a decade of helmet promotion in Victoria, Australia — an evaluation. Accid Anal Prev 1994; 26: 325-237.
- 9. McDermott F, Lane J. Protection afforded by cycle helmets. BMJ 1994; 309: 877.
- 10. McDermott FT, Lane JC, Brazenor GA, Debney EA. The effectiveness of bicyclist helmets: a study of 1710 casualties. J Trauma 1993; 34: 834-845.
- 11. Davidson JA. Epidemiology and outcome of bicycle injuries presenting to an emergency department in the United Kingdom. Eur J Emerg Med 2005; 12: 24-29.
- 12. Maimaris C, Summers CL, Browning C, Palmer CR. Injury patterns in cyclists attending an accident and emergency department: a comparison of helmet wearers and non-wearers. BMJ 1994; 308: 1537-1540.
- 13. Moodie R. It’s war on our roads and cars should not be the winners. The Age (Melbourne) 2008; 7 Mar.
- 14. Rivara FP, Thompson DC, Thompson RS. Epidemiology of bicycle injuries and risk factors for serious injury. Inj Prev 1997; 3: 110-114.
- 15. Australian Bureau of Statistics. Population by age and sex, Australian states and territories. Canberra: ABS, 2008. (Catalogue No. 3201.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/MF/3201.0 (accessed Jan 2009).
- 16. Stokes M, Ozanne-Smith J, Harrison J, Steenkamp M. Validation of an injury surveillance epidemiological data system used within emergency departments. Inj Control Saf Promot 2000; 7: 219-232.
- 17. Victorian Admitted Episodes Data Set. Melbourne: Department of Human Services, Acute Health Division, 1999.
- 18. Cameron PA, Finch CF, Gabbe BJ, et al. Developing Australia’s first statewide trauma registry: what are the lessons? ANZ J Surg 2004; 74: 424-428.
- 19. Victorian State Trauma Registry 2006-07: summary Report. Melbourne: Victorian State Trauma Outcome Registry and Monitoring Group, 2008.
- 20. McDermott FT, Klug GL. Injury profile of pedal and motor cyclist casualties in Victoria. Aust N Z J Surg 1985; 55: 477-483.
- 21. Rowe BH, Rowe AM, Bota GW. Bicyclist and environmental factors associated with fatal bicycle-related trauma in Ontario. CMAJ 1995; 152: 45-53.
- 22. Strohm PC, Sudkamp NP, Zwingmann J, et al. [Polytrauma in cyclists. Incidence, etiology, and injury patterns] [German]. Unfallchirurg 2005; 108: 1022-1028.
- 23. Lardelli Claret P, Luna del Castillo Jde D, Jiménez Moleón JJ, et al. [An assessment of the effect of helmet use among cyclists and the risk of head injury and death in Spain, 1990 to 1999] [Spanish]. Med Clin (Barc) 2003; 120: 85-88.
- 24. Urquhart DM, Williamson OD, Gabbe BJ, et al. Outcomes of patients with orthopaedic trauma admitted to level 1 trauma centres. ANZ J Surg 2006; 76: 600-606.
- 25. Drummond AE, Jee FM. The risks of bicyclist accident involvement. Melbourne: Monash University Accident Research Centre (MUARC), 1988. http://www.monash.edu.au/muarc/reports/muarc002.pdf (accessed Jan 2009).
- 26. Bicycle Victoria. Trauma: crash statistics and safety. Melbourne: Bicycle Victoria, 2008. http://www.bv.com.au/bikes-and-riding/10218/ (accessed Jan 2009).
- 27. Dennerlein JT, Meeker JD. Occupational injuries among Boston bicycle messengers. Am J Ind Med 2002; 42: 519-525.
- 28. Rivara FP, Thompson DC, Patterson MQ, Thompson RS. Prevention of bicycle-related injuries: helmets, education, and legislation. Annu Rev Public Health 1998; 19: 293-318.
- 29. Vulcan AP, Cameron MH, Watson WL. Mandatory bicycle helmet use: experience in Victoria, Australia. World J Surg 1992; 16: 389-397.
- 30. Wood T, Milne P. Head injuries to pedal cyclists and the promotion of helmet use in Victoria, Australia. Accid Anal Prev 1988; 20: 177-185.





Abstract
Objective: To investigate the incidence of bicycling injuries and bicycle injury characteristics in the Victorian population.
Design: Review of prospectively collected data.
Setting: Bicycling injury data were extracted from four datasets for the period July 2001 to June 2006: (i) emergency department (ED) presentations from the Victorian Emergency Minimum Dataset; (ii) hospital admissions from the Victorian Admitted Episodes Data Set; (iii) major trauma cases from the Victorian State Trauma Registry (VSTR); and (iv) deaths from the National Coroners Information System.
Main outcome measures: The profile and incidence of bicycling injuries across the datasets and years.
Results: In the 5 years, 25 920 bicycle-related ED presentations were recorded, 10 552 bicyclists were admitted to hospital, 298 bicycling injuries were classified as major trauma (VSTR), and there were 47 bicycling fatalities. From 2001 to 2006, the incidence of bicycle-related ED presentations (incidence rate ratio [IRR] = 1.42; 95% CI, 1.37–1.48), hospital admissions (IRR = 1.16; 95% CI, 1.09–1.23) and major trauma (IRR = 1.76; 95% CI, 1.22–2.55) increased significantly. Most of those injured were males, aged < 35 years, with road-related injuries. Patients classified as having major trauma had a significantly higher incidence of trunk and head/face/neck injuries compared with those presenting to an ED or admitted to hospital.
Conclusion: The incidence of serious bicycling injury has risen over recent years, highlighting the need for targeted prevention programs. Accurate data on cycling participation, use of injury prevention strategies, and injury profiles would assist in reducing bicycle-related injury.