Development of the HRX program was based on findings from the second round of coordinated care trials,1 run from 2003 to 2005 by GPpartners Ltd, the Division of General Practice covering northern Brisbane. This trial demonstrated that patients with chronic and complex conditions can benefit from a multidisciplinary, multisector, team-based approach to the planning and provision of their care. The trial resulted in an average reduction of 26% in inpatient costs for intervention patients.2 Another key outcome from the trial was the understanding that an electronic health record system was required to facilitate the flow of information between care team members, as existing paper-based systems did not work.
Increase in HRX usage by nurses in the Discharge Facilitation Unit and Community Assessment and Referral Services as their understanding of the benefits of shared health summaries increased;
Increase in registered patient numbers, from 474 in July 2007 to 1320 in June 2008;
Increased commitment by RBWH to promote recruitment of patients and GPs to the HRX through specific recruitment strategies — for example, uploading discharge documents, distributing HRX patient brochures, and identifying patients with complex conditions who would be likely to benefit;
Use of HRX to facilitate positive patient communication and help prevent unplanned readmission (demonstrated by case studies);
Significant and pressing interest expressed by other RBWH clinical units in accessing the shared patient information from primary care; and
Improvements in staff perception and acceptance of an SEHR, and benefits for patients and health care providers (demonstrated by user surveys).
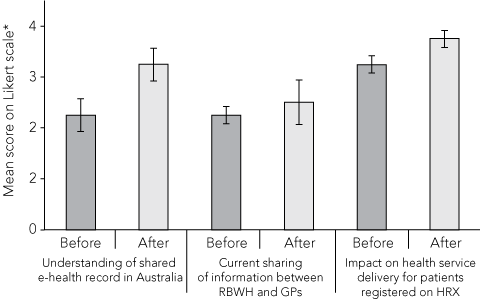
Results from a survey of RBWH staff involved in the HRX implementation before connection to the HRX and again 4 months after commencement of the trial are shown in Box 1. Staff were asked to grade their responses to the following questions based on a five-point Likert scale (from 1 “poor” to 5 “excellent”):
How would you describe your understanding of a shared electronic health record in Australia today?
How would you describe the current sharing of information and communication between your organisation and GPs?
What impact do you think the HRX will have on the delivery of health services for registered patients?
Case studies from the RBWH evaluation of two patients enrolled in the Team Care Coordination Program (Box 2, Box 3) illustrate the type of patient for whom the HRX is an ideal tool to facilitate improved care between GPs and other service providers.
Implementation of SEHR projects in Brisbane and the Northern Territory3 has shown that health communities and state/territory jurisdictions can implement such systems, and both need to be included in any health system’s transformation. These projects also demonstrate that components such as unique patient and provider identifiers, clinical coding standards and legislation and privacy standards need to be applied at a national level.
Professor Keith McNeil, Clinical Chief Executive Officer at the RBWH, noted:
For coordinated care to work, all parties must have access to a patient’s records at all times. We see the benefits of an SEHR when a patient is rushed to hospital at 3:00 am and hospital staff can access their up-to-date records.
Often countries have quoted time frames of 10 years or more to deliver SEHR systems.4 These estimates are quite realistic, given the significant change management required. Any SEHR program should anticipate and plan for several generations of software during the course of a widespread implementation.
1 Mean scores from surveys of hospital staff before and after implementation of the HRX system at RBWH
 | |||||||||||||||
2 Case study 1
Chronic renal failure
Chronic obstructive pulmonary disease
Ischaemic heart disease
Hyperlipidaemia
Non-insulin-dependent diabetes mellitus
Information recorded on the HRX and shared between members of the patient’s care team included:
Current medications
Allergies
Current conditions
Care team members (10 in total)
Case management coordination events
Initial health summary
Initial health assessment
General practitioner management plan
Allied health referrals
Allied health report
Hospital events
GP consultation events
Patient consent form
Outcomes regarding this case study:
The HRX enabled staff in the emergency department to access important and otherwise unknown patient information
The HRX enabled the patient’s community service coordinator to work with hospital clinicians and assist with strategies to prevent further hospital presentations, resulting in a reduction in unplanned visits to the emergency department
The patient reported increased satisfaction with his care and said he felt more confident since this episode of care and was more willing to follow up on other referrals
Ongoing updates are continually available via the HRX to the GP and the patient’s care team regarding his episodes of care.
3 Case study 2
Information recorded on the HRX and shared between members of the CARS team included:
Current medications
Allergies
Current conditions
Initial health summary
Initial health assessment
Service coordinator review
Outcomes regarding this case study:
Staff from CARS were able to contact the patient’s service coordinator to inform her that the patient was in hospital
The service coordinator was then able to contact the patient’s general practitioner to advise him of the patient’s admission
The GP could then liaise with the RBWH Discharge Facilitation Unit while the man was an inpatient
RBWH staff treating the patient found the HRX to be extremely helpful, as they were able to access important information
The HRX enabled coordination with other service providers for ongoing management and care.
- Brett V Silvester1
- Simon J Carr2
- GPpartners Ltd, Brisbane, QLD.
The second round of coordinated care trials was funded by the Australian Government Department of Health and Ageing and Queensland Health, with significant resources provided by non-government nursing agencies. The implementation of the HRX was supported by funding from the Australian Government Department of Health and Ageing, the Department of Veterans’ Affairs, and the Australian Government Department of Communication, Information Technology and the Arts. Extensia Solutions Pty Ltd also provided in-kind support. The Australian Commission on Safety and Quality in Health Care is helping to fund current HRX research.
Brett Silvester is the Deputy Chief Executive Officer and Simon Carr is the Manager of Information Systems at GPpartners. GPpartners receives significant funds from the Australian Government Department of Health and Ageing. Funding is also sourced through project and research funding pools, the Queensland Government, community organisations and private industry. GPs contribute with an annual membership fee.
- 1. The national evaluation of the second round of coordinated care trials: final report. Part 1: executive summary. Canberra: Commonwealth of Australia, 2007. http://www.health.gov.au/internet/main/publishing.nsf/Content/19F44B315755217ECA 2573DE007AF9DA/$File/FINAL%20CCT2%20Part%201%20Executive%20Summary.pdf (accessed Mar 2009).
- 2. The national evaluation of the second round of coordinated care trials: final report. Part 2: evaluation approach and summary findings of the second round of coordinated care trials. Tables 32 and 33. Canberra: Commonwealth of Australia, 2007: 103. http://www.health.gov.au/internet/main/publishing.nsf/Content/19F44B315755217ECA2573DE007AF9DA/$File/Part2%20pgs101-115.pdf (accessed Mar 2009).
- 3. Northern Territory Government. eHealthNT: about the shared electronic health record. http://www.ehealthnt.nt.gov.au/Shared_Electronic_Health_Record (accessed Mar 2009).
- 4. Center for Information Technology Leadership. The value of personal health records. Charlestown, Mass: CITL, 2008. http://www.citl.org/_pdf/CITL_PHR_Report.pdf (accessed Mar 2009).





Abstract
A shared electronic health record system has been successfully implemented in Australia by a Division of General Practice in northern Brisbane.
The system grew out of coordinated care trials that showed the critical need to share summary patient information, particularly for patients with complex conditions who require the services of a wide range of multisector, multidisciplinary health care professionals.
As at 30 April 2008, connected users of the system included 239 GPs from 66 general practices, two major public hospitals, three large private hospitals, 11 allied health and community-based provider organisations and 1108 registered patients.
Access data showed a patient’s shared record was accessed an average of 15 times over a 12-month period.
The success of the Brisbane implementation relied on seven key factors: connectivity, interoperability, change management, clinical leadership, targeted patient involvement, information at the point of care, and governance.
The Australian Commission on Safety and Quality in Health Care is currently evaluating the system for its potential to reduce errors relating to inadequate information transfer during clinical handover.