In 2003, mental health disorders comprised 13.3% of the total burden of disease.1 Chronic conditions provide challenges in communicating and coordinating care across multiple health providers and care settings.2 In mental health, stigma, confidentiality and issues relating to competency for decision making further increase the complexity of discharge planning.3 Although there are robust governance practices for clinical procedures in the private hospital setting,4 there are often limited structures to leverage improvements in coordination and communication across care providers, particularly in smaller private facilities. In both acute and community settings, poor communication is increasingly being identified as a factor in adverse health events5,6 and diminished safety and quality of care.7
In spite of an emerging interest in issues associated with clinical handover,8-10 there is limited information on clinical handover from private mental health services to community practitioners.11 A review of discharge practices at both study sites revealed a disparate approach to discharge documentation and communication, with most patients given only a nursing discharge summary and a medication list. Monthly audits of discharge letters from visiting medical officers (VMOs) revealed that the rate of mailing to the referring practitioner within 14 days of patient discharge was as low as 50%. A lack of consistency and coordination was evident, and local general practitioners expressed their concern about inadequate provision of timely and appropriate information. In response to the need for improved care coordination, the Revolving doors: effective communication in the handover of mental health patients to community health practitioners (CHOCYS) project has been funded as part of a clinical handover initiative by the Australian Commission on Safety and Quality in Health Care (ACSQHC). Using a quality improvement method,12 the CHOCYS project sought to develop and test a standardised clinical handover strategy for improving information transfer between hospital and community-based providers.
A collaborative approach was used to address issues relating to discharge planning. This involves executive support and clinical leadership to drive practice improvement within a time-limited process.13 It uses the plan-do-study-act (PDSA) cycle: plan: plan the change to be tested; do: carry out the test and implement the strategy; study: analyse the results, evaluate data from the trial and summarise the lessons learnt; act: adjust the strategy and plan the next cycle, or embed the new strategy and monitor.12,13
Implementation of the project was managed by a project team composed of hospital and community health care providers and patient representatives (on the steering committee). The PDSA model provided a structured and iterative process for developing a standardised discharge process and outcome assessment strategy.12,13
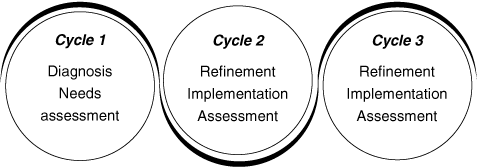
The intervention was conducted in three cycles (see below). Schemata for the study, identifying key steps in the three cycles and the ongoing engagement with the practice setting, are shown in Box 1. Under the specific cycles, details are provided to show how the process of consultation, implementation, reflection and measurement evolved to achieve the project objectives. A number of comparative clinical indicators (CCIs) were developed for the project from the information derived from Cycle 1.14
This phase involved a comprehensive needs assessment and diagnosis of the issues to be addressed. It is important to note that the directors of clinical services (S K W and A K C) applied on behalf of the study sites to be funded by ACSQHC in a competitive process. Therefore, there were clinical champions and an organisational climate supportive of quality improvement. The Steering Committee (made up of the two directors of clinical services, the medical director, a psychiatrist, a pharmacist, a GP, a Division of General Practice representative, a patient representative, a discharge coordinator [from both sites] and the project coordinator) provided the knowledge, skills and networks for reviewing current discharge clinical handover practice. An internal reference group consisting of senior clinical administrative executives, nursing and allied health representatives, pharmacists, CMOs and psychiatrists was set up. Community-based practitioners, including GPs, psychologists and psychiatrists, were surveyed for their needs relating to the discharge process (surveys were mailed, faxed, or handed out at continuing professional development seminars held at each site). Brief demographics of these participants are shown in Box 2.
Medical diagnosis, physical findings and investigations that were new findings for the episode of care;
Pharmacotherapy initiated; and
Psychosocial transactions that formed part of patient care for the treatment episode.
The CCIs developed in consultation with the reference group are shown in Box 3.
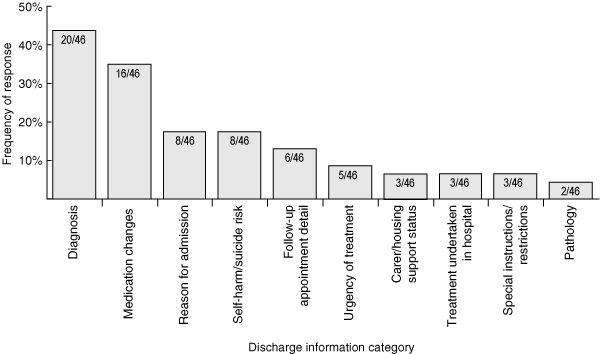
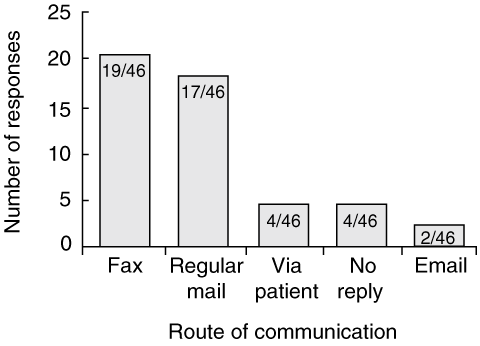
Overall findings of the study (based on a 42% response rate from community practitioners15) are summarised in Box 4. Practitioners’ preferences for content and method of communication after discharge are shown in Box 5 and Box 6. Most respondents preferred the discharge summary to be sent via fax. Practitioners identified communication of diagnosis, medications and risk of self-harm as priorities.
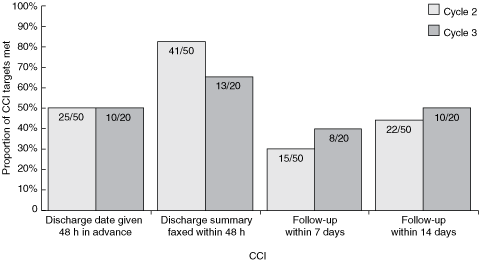
Results of the process CCIs for Cycle 2 and 3 are shown in Box 7. Each indicator was analysed to determine barriers and facilitators to implementation. The Steering Committee resolved that the project documentation had been sufficiently refined to become the standard procedure. However, some issues are yet to be resolved regarding sustainability of the gains achieved. For example, contact with community pharmacies was considered to be an important element in encouraging medication concordance and safety. Over 50% of patients agreed to have their community pharmacist contacted if necessary, and criteria were developed to identify patients at risk of medication error, overdose, or polypharmacy/drug interaction, but this process requires further refinement to meet its potential.
Characteristics of patients recruited for the intervention are shown in Box 8. On follow-up, seven patients (35%) still did not remember the interaction surrounding the discharge process. The 13 patients (65%) who could recall this interaction expressed a high degree of satisfaction with the overall process.
This CHOCYS project collaboratively developed and implemented a strategy to streamline communication at discharge. The team is currently entering Cycle 4, focusing on sustainability of the process and quality of the information provided. Promoting and sustaining effective communication strategies is likely to improve patient safety, quality of care, medication outcomes and community practitioner and patient satisfaction. Our study revealed that clinical handover needs to be more than a discursive reflection and stringing together of ad-hoc processes. It requires a defined purpose, structure, delegation of responsibility, and appraisal of outcomes.9 Organisational commitment, executive support, and active representation and participation of key stakeholder groups contributed to the success of the project. It will be important to keep monitoring the outcomes of the process in the longer term to ensure sustained and continued practice improvement. Instituting the practice changes in organisational policy will facilitate this process.
Our study achieved a number of important goals: it delineated the process outcomes and challenged many of the barriers perceived to be associated with inter- and intra-provider communication in mental health; it demonstrated the feasibility of collaboration and engagement within a private health care model; it empirically and systematically devised a set of CCIs appropriate to the mental health setting; and it showed the capacity to implement best practice within a quality improvement framework. The importance of executive support, clinical leadership and key stakeholder engagement for driving projects of this kind cannot be overemphasised.16
Our study had several limitations. Non-random sampling was used to solicit responses from health care providers and patients. Response rates to the surveys were fairly low, although comparable to those for other surveys of this type.15 Context-specific factors, such as the presence of salaried CMOs and an on-site pharmacy, would need to be considered in applying these findings to other settings. It is also important to note that this was a quality improvement project, focusing on the day-to-day elements of clinical practice, which differentiates this type of data collection from traditional experimental designs.17 These caveats should be considered when interpreting our study findings.
The scant literature relating to handover in the private mental health care setting11 means there is a limited basis for comparison of our results with those of other studies. However, a recent report by Kripalani and colleagues identifies communication failure and inadequate information transfer at discharge as contributing to adverse health care.18 Their study recommends the use of standardised processes. Additional research is required to demonstrate the impact of the CHOCYS project on longer-term outcomes, such as adverse health events and concordance with recommended treatment strategies.
Our project allowed the development and testing of a negotiated, evidence-based communication strategy designed to promote patient safety and quality of care. This re-engineering of systems and processes happened without investment in expensive information systems, although the business processes and systems were developed to allow easy migration to e-health systems at a later stage.19 Integral to the process has been determining practitioners’ and patients’ satisfaction with the clinical handover communication strategy with respect to timeliness, content and format. The number of patient participants who found it difficult to recollect the discharge process is of concern, and identifying people at higher risk of rehospitalisation, relapse, self-harm or non-concordance7 is an important factor to be considered in further iterations of this project.
2 Community practitioner demographics, Cycle 1 (n = 46)
* Figures represent number of practitioners, except where otherwise specified. |
|||||||||||||||
4 Community practitioners’ survey results for Cycle 1 (before intervention) and Cycles 2 and 3 (after intervention)*
Discharge summary should be available at first follow-up appointment |
|||||||||||||||
VMO = visiting medical officer. * Figures represent number of responses. |
|||||||||||||||
5 Priorities of community practitioners (n = 46) with respect to discharge information categories*
 | |||||||||||||||
|
* Providers were asked to number the categories from 1 to 10, with 1 being their highest priority. | |||||||||||||||
- Susan K Wood1
- Allison K Campbell1
- Judith D Marden1
- Lavinia Schmidtman1
- George H Blundell1
- Noella J Sheerin1
- Patricia M Davidson2
- 1 St John of God Health Care, Sydney, NSW.
- 2 Centre for Cardiovascular and Chronic Care, Curtin University of Technology (Sydney), Sydney, NSW.
None identified.
- 1. Begg S, Vos T, Barker B, et al. The burden of disease and injury in Australia 2003. Canberra: Australian Institute of Health and Welfare, 2007.
- 2. Rothman A, Wagner E. Chronic illness management: what is the role of primary care? Ann Intern Med 2003; 138: 256-261.
- 3. Corrigan JM. How stigma interferes with mental health care. Am Psychol 2004; 59: 614-625.
- 4. Australian Private Hospitals Association. Summary and recommendations of submission from the Australian Private Hospitals Association to the National Health and Hospitals Reform Commission. 2008. http://www.apha.org.au/publications.html (accessed Feb 2009).
- 5. Cook RI, Render M, Woods DD. Gaps in the continuity of care and progress on patient safety. BMJ 2000; 320: 791-794.
- 6. Kohn LT, Corrigan JM, Donaldson MS. To err is human: building a safer health care system. Washington, DC: National Academy Press, 2000.
- 7. Owen C, Rutherford V, Jones M, et al. Psychiatric rehospitalization following hospital discharge. Community Ment Health J 1997; 33: 13-24.
- 8. Patterson E, Roth E, Woods D, et al. Handoff strategies in settings with high consequences for failure: lessons for health care operations. Int J Qual Health Care 2004; 16: 125-132.
- 9. Strategies to improve hand-off communication: implementing a process to resolve questions. Jt Comm Perspect Patient Saf 2005; 5 (7): 11.
- 10. Sharing information at transfers: proven technique to aid handoff communication. Jt Comm Perspect Patient Saf 2005; 5 (12): 9-10.
- 11. Wong M, Yee K, Turner P. Clinical handover literature review. Hobart: eHealth Services Research Group, University of Tasmania, 2008.
- 12. Deming WE. Out of the crisis. Cambridge, Mass: Massachusetts Institute of Technology, 1986.
- 13. Øvretveit J, Bate P, Cleary P, et al. Quality collaboratives: lessons from research. Qual Saf Health Care 2002; 11: 345-351.
- 14. Huw D, in consultation with the Scottish Research Network on Health Care Management. Measuring and reporting the quality of health care: issues and evidence from international research literature. Edinburgh: NHS Quality Improvement Scotland, 2006.
- 15. Buchan T, Boldy D. Improving mental health services in a local area: an exploratory study. Aust Health Rev 2004; 28: 292-300.
- 16. Newton P, Halcomb E, Davidson P, et al. Barriers and facilitators to the implementation of the collaborative methodology: reflections from a single site. Qual Saf Health Care 2007; 16: 409-414.
- 17. Speroff T, James BC, Nelson EC, et al. Guidelines for appraisal and publication of PDSA quality improvement. Qual Manag Health Care 2004; 13: 33-39.
- 18. Kripalani S, LeFevre F, Phillips C, et al. Deficits in communication and information transfer between hospital-based and primary care physicians: implications for patient safety and continuity of care. JAMA 2007; 297: 831-841.
- 19. Dracup K, Morris P. Passing the torch: the challenge of handoffs. Am J Crit Care 2008; 17: 95-97.





Abstract
Objectives: To develop and test a standardised clinical handover discharge strategy for improving information transfer between private mental health hospitals and community practitioners.
Design, setting and participants: A quality improvement intervention using collaborative, iterative methods to develop a standardised discharge and outcome assessment strategy. 150 patient participants were consecutively recruited from two private mental health care hospitals in New South Wales between April and September 2008. Opinions of community practitioners and patients on the discharge process and discharge documentation were solicited by written questionnaires and telephone interviews.
Main outcome measures: Community practitioner satisfaction; patient satisfaction; documentation of discharge date at least 48 hours before discharge; faxing of discharge summaries to community practitioners within 48 hours of discharge; proportion of patients receiving a follow-up telephone call within 7 days or 14 days of discharge.
Results: Both community practitioners and patients believed the intervention was positive. Between Cycle 2 and Cycle 3, documentation of the discharge date at least 48 hours before discharge remained unchanged at 50%; the proportion of discharge summaries faxed within 48 hours of discharge went from 0 to 82% in Cycle 2 and fell to 65% in Cycle 3. Telephone follow-up of patients within 7 days and within 14 days improved by 10% and 6%, respectively, between Cycle 2 and Cycle 3.
Conclusions: A standardised discharge communication strategy improved the timeliness, content, and format of information provided to community practitioners. The intervention was well accepted by patients and providers.