It has long been observed that individual responses to a drug, with regard to both efficacy and adverse effects, vary from person to person. A range of reasons for these variations has been proposed, including individual variation in pharmacokinetics and pharmacodynamics, concomitant medication use, concurrent disease, and environmental factors. In recent years, increasing attention has been given to genetics as a cause of interpersonal variation.1,2
Variations on the genes for the metabolising enzyme cytochrome P450 2C9 (CYP2C9) and vitamin K epoxide reductase (VKORC1) have been shown to be responsible for increasing the activity and hence the risk of elevated international normalised ratio and haemorrhage with warfarin.3 The factor V Leiden mutation results in higher coagulation protein stability, and its presence has a multiplicative effect on the risk of venous thromboembolism with combined oral contraceptives.4 Potentially fatal toxicity with azathioprine and 6-mercaptopurine because of thiopurine S-methyltransferase deficiency occurs in the presence of co-dominant polymorphisms leading to amino acid substitutions.5 In addition, genetic variations on the CYP450 genes controlling hepatic metabolism of drugs have been well investigated in recent decades.1
The completion of the Human Genome Project in 2003 and the development of cost-effective means for scanning large regions of DNA have paved the way for large-scale pharmacogenetic investigations involving many genetic loci. Very recently, a genome-wide study identified a variant in a gene (SLCO1B1) coding for a polypeptide involved in hepatic statin uptake that was associated with simvastatin-induced myopathy.6 Although the odds ratio for myopathy per risk allele on the SLCO1B1 gene was 4.3 (95% CI, 2.5–7.2), the cumulative risk of myopathy for heterozygotes over 5 years of taking 80 mg of simvastatin daily was less than 3%, and it was only one of many cofactors (eg, other medication, age > 65 years, and renal impairment) contributing to the risk.
The therapeutic benefit of this research could be said to be disappointing. However, investigation of genetic causes of idiosyncratic drug reactions has the potential to be more worthwhile than the investigation of effects like myopathy with statins in terms of the predictive value of the polymorphisms. Idiosyncratic reactions are often immune-mediated, commonly serious, currently unpredictable, and frequently result in reluctance to prescribe an otherwise useful drug. There has been at least one instance when an idiosyncratic hypersensitivity reaction resulted in a drug being sidelined for a newer alternative (clopidogrel replacing ticlopidine), even though most people using the original drug benefited without clinically significant ill effects.7
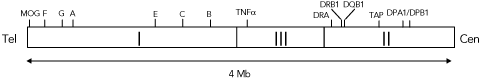
The most likely area of DNA for genetic variations that predispose to drug hypersensitivity reactions is the human leukocyte antigen (HLA) region (Box 1). This region is the genetic locus for many diseases and contains many genes associated with immune function.8,9
In December 2007, the United States Food and Drug Administration announced that, because of the associated risk of Stevens–Johnson syndrome and toxic epidermal necrolysis, people of Asian descent should be genetically tested for the HLA-B*1502 allele before starting therapy with carbamazepine.10 This was the first time a regulatory authority had recognised a genetic predisposition for a hypersensitivity reaction.
The initial identification of this association was in a case–control study conducted in a Han Chinese population.11 Genetic mapping involved a comparison of HLA genotypes for 44 patients with Stevens–Johnson syndrome or toxic epidermal necrolysis with those of 101 controls who had taken carbamazepine for at least 3 months without development of any skin reaction, and 93 healthy individuals. HLA-B*1502 was present in all the case patients, in 3% of control patients taking carbamazepine and in 9% of the healthy controls (see Box 2). Although Stevens–Johnson syndrome with carbamazepine also occurs among Caucasians, HLA-B*1502 has not been found in this group.14
Two other strong associations with genetic markers for drug hypersensitivity reactions have been identified in the HLA region: HLA-B*5701 predisposes to hypersensitivity with abacavir,12,15 and HLA-B*5801 predisposes to severe cutaneous reactions with allopurinol (Box 2).13
The association of HLA-B*5701 with abacavir hypersensitivity was initially identified in a cohort study conducted by a group from Perth in 2002, which found 18 cases of hypersensitivity in a cohort of 185.15 This association then became the subject of the first randomised controlled trial of a genetic polymorphism for a hypersensitivity reaction, the results of which were published in February 2008.12 In this study, almost 2000 abacavir-naïve HIV patients were randomly assigned to either prospective or retrospective screening for HLA-B*5701. Those in the prospective group who tested positive were not given abacavir. In the retrospective group, individuals developing signs and symptoms of hypersensitivity after starting treatment with the drug had percutaneous patch testing with abacavir. All of the patients who developed immunologically confirmed hypersensitivity possessed the genetic marker, meaning that none of these events occurred in the group who were prospectively screened. Of those retrospectively testing positive for the predisposing polymorphism, 48% had developed abacavir hypersensitivity.12
Following the initial identification of the polymorphism and before publication of the randomised controlled trial results, genotyping for HLA-B*5701 prior to initiation of abacavir had become the standard of care in the United Kingdom.16 As a result, prescription of abacavir increased because its use without hypersensitivity could be assured, indicating the benefit that can be achieved from investigation of genetic predispositions. In Australia, genotyping for HLA-B*5701 prior to abacavir use is now funded by Medicare.17
An intriguing result of the investigation of predisposing genetic polymorphisms in all three instances described here is the small proportion of individuals who possessed the genetic marker but took the drug without adverse effect (Box 2). This raises the possibility of other contributing genetic factors or of phenotypic and environmental cofactors. The study of skin reactions with allopurinol found that chronic renal dysfunction more than doubled the likelihood of a reaction.13 Depending on the cofactors present, it may be possible to prevent hypersensitivity, despite drug exposure, in those with the genetic marker.
Most hypersensitivity reactions have skin manifestations, but this is not always so. Clozapine-associated myocarditis typically is not associated with skin rash, but cardiac histology demonstrates its immune origin.18 Similarly, other reactions such as myalgia with eosinophilia, hepatitis and blood dyscrasias may be hypersensitivity reactions, raising the possibility that predisposing polymorphisms might be identifiable for a diverse range of adverse reactions. Other specific associations that may have strongly predisposing single nucleotide polymorphisms are cholestatic jaundice with flucloxacillin,19 agranulocytosis with terbinafine,20 thrombotic thrombocytopenic purpura with ticlopidine and clopidogrel,21 and interstitial nephritis with omeprazole,22 as well as the more obvious associations of angioedema with angiotensin-converting enzyme inhibitors, and anaphylaxis with penicillins and cephalosporins.
There are two significant obstacles to the conduct of this research in Australia. The first obstacle is obtaining a funding source for an investigation of drugs that are long out of patent. The Partnerships scheme recently launched by the National Health and Medical Research Council (NHMRC)23 might extend to such projects, provided the Therapeutic Goods Administration is allocated funding for research. The second obstacle is the multiple ethics and research governance applications required to obtain a sufficiently large cohort of cases.
- Kathlyn J Ronaldson1
- John J McNeil2
- Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
None identified.
- 1. Brockmöller J, Tzvetkov MV. Pharmacogenetics: data, concepts and tools to improve drug discovery and drug treatment. Eur J Clin Pharmacol 2008; 64: 133-157.
- 2. US Food and Drug Administration Center for Drug Evaluation and Research. Genomics at FDA. Publications by FDA staff. http://www.fda.gov/cder/genomics/publications.htm (accessed Sep 2008).
- 3. Schwarz UI, Ritchie MD, Bradford Y, et al. Genetic determinants of response to warfarin during initial anticoagulation. N Engl J Med 2008; 358: 999-1008.
- 4. Vandenbroucke JP, Koster T, Briët E, et al. Increased risk of venous thrombosis in oral-contraceptive users who are carriers of factor V Leiden mutation. Lancet 1994; 344: 1453-1457.
- 5. Otterness D, Szumlanski C, Lennard L, et al. Human thiopurine methyltransferase pharmacogenetics: gene sequence polymorphisms. Clin Pharmacol Ther 1997; 62: 60-73.
- 6. Link E, Parish S, Armitage J, et al; SEARCH Collaborative Group. SLCO1B1 variants and statin-induced myopathy — a genomewide study. N Engl J Med 2008; 359: 789-799.
- 7. Berger PB. Results of the Ticlid or Plavix Post-Stents (TOPPS) trial: do they justify the switch from ticlopidine to clopidogrel after coronary stent placement? Curr Control Trials Cardiovasc Med 2000; 1: 83-87.
- 8. The MHC Sequencing Consortium. Complete sequence and gene map of a human major histocompatibility complex. Nature 1999; 401: 921-923.
- 9. Chung WH, Hung SI, Chen YT. Human leukocyte antigens and drug hypersensitivity. Curr Opin Allergy Clin Immunol 2007; 7: 317-323.
- 10. US Food and Drug Administration Center for Drug Evaluation and Research. Information for healthcare professionals. Carbamazepine (marketed as Carbatrol, Equetro, Tegretol, and generics). FDA Alert 2007; 12 Dec. http://www.fda.gov/cder/drug/InfoSheets/HCP/carbamazepineHCP.htm (accessed Sep 2008).
- 11. Chung WH, Hung SI, Hong HS, et al. Medical genetics: a marker for Stevens–Johnson syndrome. Nature 2004; 428: 486.
- 12. Mallal S, Phillips E, Carosi G, et al. HLA-B*5701 screening for hypersensitivity to abacavir. N Engl J Med 2008; 358: 568-579.
- 13. Hung SI, Chung WH, Liou LB, et al. HLA-B*5801 allele as a genetic marker for severe cutaneous adverse reactions caused by allopurinol. Proc Natl Acad Sci U S A 2005; 102: 4134-4139.
- 14. Alfirevic A, Chadwick DW, Park BK, Pirmohamed M. Lack of association between serious carbamazepine hypersensitivity reactions and HLA-B in Caucasians. Br J Clin Pharmacol 2005; 59: 641.
- 15. Mallal S, Nolan D, Witt C, et al. Association between presence of HLA-B*5701, HLA-DR7, and HLA-DQ3 and hypersensitivity to HIV-1 reverse-transcriptase inhibitor abacavir. Lancet 2002; 359: 727-732.
- 16. Ingelman-Sundberg M. Pharmacogenomic biomarkers for prediction of severe adverse drug reactions. N Engl J Med 2008; 358: 637-639.
- 17. Australian Government Department of Health and Ageing. Medicare Benefits Schedule Online. Items 71203 and 73323. http://www9.health.gov.au//mbs/search.cfm?q=abacavir&sopt=S (accessed Apr 2009).
- 18. Kilian JG, Kerr K, Lawrence C, Celermajer DS. Myocarditis and cardiomyopathy associated with clozapine. Lancet 1999; 354: 1841-1845.
- 19. Fairley CK, McNeil JJ, Desmond P, et al. Risk factors for development of flucloxacillin associated jaundice. BMJ 1993; 306: 233-235.
- 20. Pillans PI, Boyd IW. Toenails and agranulocytosis. Intern Med J 2007; 37: 572-575.
- 21. Bennett CL, Connors JM, Carwile JM, et al. Thrombotic thrombocytopenic purpura associated with clopidogrel. N Engl J Med 2000; 342: 1773-1777.
- 22. Myers RP, McLaughlin K, Hollomby DJ. Acute interstitial nephritis due to omeprazole. Am J Gastroenterol 2001; 96: 3428-3431.
- 23. National Health and Medical Research Council. NHMRC Partnerships for better health: creating effective collaboration between policy and research. http://www.nhmrc.gov.au/grants/partnerships/ (accessed Apr 2009).





Abstract
Individuals vary in their response to a medication with regard to efficacy and adverse effects.
The human leukocyte antigen (HLA) region of DNA offers the key to predicting drug hypersensitivity reactions.
Single nucleotide polymorphisms for hypersensitivity reactions with carbamazepine, abacavir and allopurinol have been identified.
A randomised controlled trial demonstrated the effectiveness of prospective screening for the predisposing genetic marker in preventing all cases of the hypersensitivity reaction with abacavir.
Further pharmacogenetic investigation of hypersensitivity reactions could be conducted in Australia by establishing a network of sentinel hospitals.