Shift-to-shift medical and nursing handovers have been identified as high-risk areas in which improved clinical handover solutions are urgently required.1 Clinical handover requires a transfer of information, responsibility and accountability for patient care.2 Unless the receiver of the information during handover understands and acts upon the information given, continuity of patient care will not be achieved.
Major factors inhibiting handover improvements include the lack of basic understanding of handover processes and the absence of a common structure.1 Medical shift-to-shift handover remains poorly defined and poorly understood.3 Many hospitals do not have clear policies on how to conduct effective handover, and the transfer of responsibility and accountability is not well practised.4 At the same time, the nursing profession has a long tradition of practising shift-to-shift handover.5 Recently, the efficiency and effectiveness of nursing handovers have been scrutinised, and the need to improve and optimise the accurate transfer of information, responsibility and accountability has been identified.6 More importantly, the need to improve clinical handover has been recognised as important for reducing errors, improving patient safety and responding to the increasing use of information technology.7
Despite a proliferation of research literature on clinical handover over the past 5 years, there remains a lack of evidence on best practice.8 Studies recommending the development of standardised operating protocols (SOPs) and minimum datasets (MDSs) are an important step towards improving handover processes.9-13 A number of SOPs and MDSs have been developed and implemented, including the widely promoted SBAR (situation–background–assessment–recommendation) technique14 and the handover tool utilised in the TeamSTEPPS program.15 However, most of these SOPs and MDSs lack validation in clinical settings, and few studies provide details on the experiences and practices of their implementation.8,15 There is also little evidence that any of these SOPs and MDSs have been developed through direct engagement with health professionals. Furthermore, none of the SOPs and MDSs appear to adequately address the transfer of both responsibility and accountability during handover.
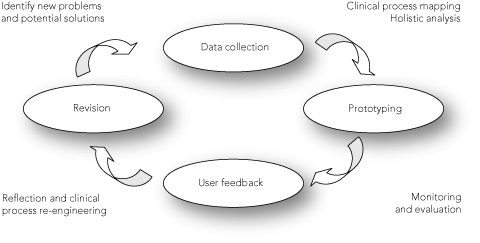
We adopted a sociotechnical approach to understanding and improving clinical handover.16 Our research team comprised four hospital staff members (three nurses, one registrar) with experience in clinical areas and two information systems researchers. Integrating expertise from clinical and information systems within the research team allowed us to use an iterative approach in combination with qualitative field techniques underpinned by user-centred design principles.16-18 This helped to optimise transferability and sustainability of the research outputs (Box 1).
Five steps were involved. Step 1 focused on understanding current handover practices, acquiring data on users’ experiences and attitudes, and generating insight into key factors affecting handover and the inter-relationships between them. We conducted 120 observation sessions (60 with nurses, 60 with doctors) and 112 interviews (51 with nurses, 61 with doctors) across the six clinical areas (nursing and clinical handovers for all three departments). Interviews were audio-recorded and researchers also took comprehensive notes covering not just the content but also other factors of potential relevance, including body language and frequency of interruptions (although interviews were conducted in a separate room, clinical staff answered pagers when necessary). Interview transcripts were analysed using a coding process drawing on the principles of grounded theory.19
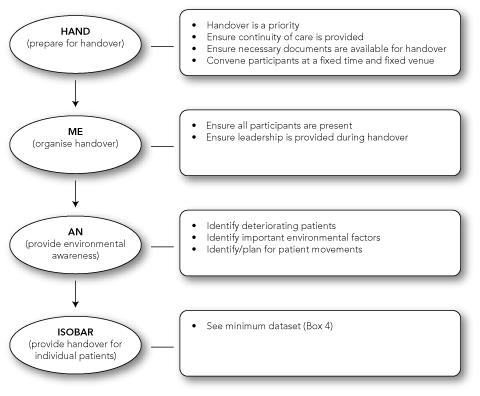
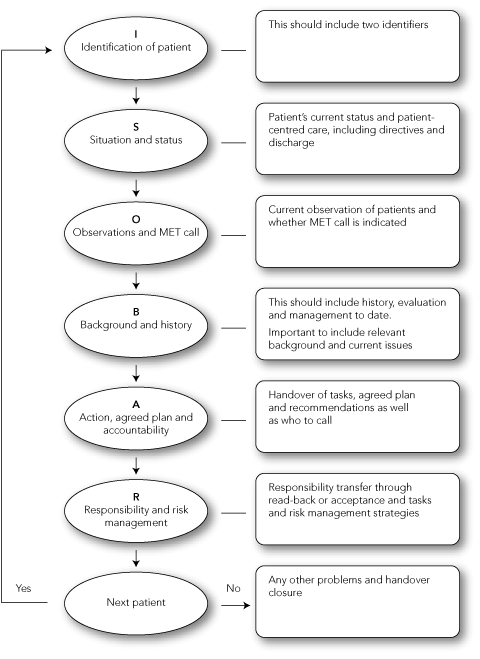
The overarching SOP and MDS that we developed was given the acronym “HAND ME AN ISOBAR”. This represents a four-step evidence-based approach to clinical handover. The steps and their constituent phases are summarised in Box 2 and Box 3 and explained in detail below.
O Observations of patient and call to medical emergency team (if indicated)
We acknowledge that there are ongoing conceptual arguments regarding the possibility of actually transferring accountability for patient care during clinical handover.2 We accept that there are certain handover circumstances in which the responsibility and accountability for patient care cannot be explicitly stated and transferred. Nevertheless, our model does support continuity of patient care from one team of practitioners to another.
- Kwang C Yee1,2
- Ming C Wong2
- Paul Turner2
- 1 Department of Gastroenterology, Royal Hobart Hospital, Hobart, TAS.
- 2 eHealth Services Research Group, School of Computing and Information Systems, University of Tasmania, Hobart, TAS.
We acknowledge the support of Craig White, Chief Executive Officer of Royal Hobart Hospital; members of the Steering Committee and reference groups; and all participants in the study. We also specifically thank the following members of the project team: Helen Courtney Pratt, Diana Coombes, Sharee Eldridge and Jo Robinson. Finally, we acknowledge the valuable feedback provided on the development and revisions of the SOP and MDS by Christine Jorm, Senior Medical Advisor, Australian Commission on Safety and Quality in Health Care.
None identified.
- 1. World Health Organization Collaborating Centre for Patient Safety Solutions. Communication during patient hand-overs. Patient Saf Solut 2007; 1 (Solution 3). http://www.ccforpatientsafety.org/common/pdfs/fpdf/presskit/PS-Solution3.pdf (accessed Feb 2009).
- 2. Australian Nurse Registering Authorities Conference. Report to the Australian Nurse Registering Authorities Conference. Canberra: Australian Nursing Council Inc, 1990.
- 3. Yee KC, Wong MC, Turner P. Medical error management and the role of information technology — a new approach to investigating medical handover in acute care settings. Stud Health Technol Inform 2006; 124: 679-684.
- 4. Bomba DT, Prakash R. A description of handover processes in an Australian public hospital. Aust Health Rev 2005; 29: 68-79.
- 5. Sherlock C. The patient handover: a study of its form, function and efficiency. Nurs Stand 1995; 9: 33-36.
- 6. Manias E, Street A. The handover: uncovering the hidden practices of nurses. Intensive Crit Care Nurs 2000; 16: 373-383.
- 7. Australian Council for Safety and Quality in Health Care. Clinical handover and patient safety: literature review report. Canberra: ACSQHC, 2005. http://www.safetyandquality.gov.au/internet/safety/publishing.nsf/Content/F3D3F3274D393DFCCA257483000D8461/$File/clinhovrlitrev.pdf (accessed Feb 2009).
- 8. Wong MC, Yee KC, Turner P. A structured evidence-based literature review regarding the effectiveness of improvement interventions in clinical handover. eHealth Services Research Group, University of Tasmania, for the Australian Commission on Safety and Quality in Health Care, 2008. http://www.safetyandquality.gov.au/internet/safety/publishing.nsf/Content/PriorityProgram-05 (accessed Feb 2009).
- 9. Arora V, Johnson J. A model for building a standardized hand-off protocol. Jt Comm J Qual Patient Saf 2006; 32: 646-655.
- 10. Bourne C. Intershift report: a standard for handovers. Nurs Times Res 2000; 5: 451-459.
- 11. Fenton W. Developing a guide to improve the quality of nurses’ handover. Nurs Older People 2006; 18: 32-36.
- 12. McCann L, McHardy K, Child S. Passing the buck: clinical handovers at a tertiary hospital. N Z Med J 2007; 120: U2778.
- 13. Wilson MJ. A template for safe and concise handovers. Medsurg Nurs 2007; 16: 201-206.
- 14. Mikos K. Monitoring handoffs for standardization. Nurs Manage 2007; 38: 16-20.
- 15. Agency for Healthcare Research and Quality, US Department of Health and Quality. TeamSTEPPS: national implementation. http://teamstepps.ahrq.gov/index.htm (accessed Feb 2009).
- 16. Coiera EW, Westbrook JI, Callen JL, Aarts J, editors. Information technology in health care 2007: Proceedings of the 3rd International Conference on Information Technology in Health Care: socio-technical approaches. Amsterdam: IOS Press, 2007. (Studies in Health Technology and Informatics Vol. 130.)
- 17. Clegg CW. Sociotechnical principles for system design. Appl Ergon 2000; 31: 463-477.
- 18. Land FF. Evaluation in a socio-technical context. In: Baskerville R, Stage J, DeGross JI, editors. Organizational and social perspectives on information technology. Boston: Kluwer Academic Publishers, 2000: 115-126.
- 19. Glaser B, Strauss AL. The discovery of grounded theory. New York: Aldine Publishing, 1967.





Abstract
Objective: To develop, using an evidence-based approach, a standardised operating protocol (SOP) and minimum dataset (MDS) to improve shift-to-shift clinical handover by medical and nursing staff in a hospital setting.
Design, setting and participants: A pilot study conducted in six clinical areas (nursing and medical handovers in general medicine, general surgery and emergency medicine) at the Royal Hobart Hospital between 1 October 2005 and 30 September 2008. Data collection and analysis involved triangulation of qualitative techniques; 120 observation sessions and 112 interviews involving nurses and junior medical officers were conducted across the six clinical areas; information on more than 1000 individual patient handovers was analysed.
Results: We developed an overarching four-step SOP and MDS for clinical handover, summarised by the acronym “HAND ME AN ISOBAR”. This standardised solution supports flexible adaptation to local circumstances.
Conclusion: A standardised protocol for clinical handover can be developed and validated across professional and disciplinary boundaries. It is anticipated that our model will be transferable to other sites and clinical settings.