In 1991, specialist services were introduced to the Cape communities as the Far North Regional Obstetric and Gynaecological Service (FROGS).1 Specialist staff and registrars from Cairns Base Hospital (CBH) travel to eight of the Cape communities four to six times per year. Since 2006, outreach midwives have accompanied the FROGS teams. After transfer to Cairns, women attend the Outreach Antenatal Clinic, which is staffed by the same midwives and, where possible, are cared for in labour by one of the Outreach team to provide continuity of care.
In the time that FROGS has been operating, the perinatal mortality rate for infants of Indigenous women in the region has decreased. In 1990, the perinatal mortality rate for Indigenous births in Queensland was 28 per 1000 births; in 2006, it was 20.3/1000 for Aboriginal births and 12.6/1000 for Torres Strait Islander births.2,3 Unpublished data from CBH show a perinatal mortality rate of 15/1000 for births among Indigenous women from the Cape York region in 2006.
During the study period, 172 women were transferred from 14 Far North Queensland communities (Box 1). This represented 7.4% of births at CBH (total births, 2328). Most women were Aboriginal (119; 69.2%) or Caucasian (34; 19.8%), with a minority from the Torres Strait Islands (12; 7.0%), Asia (5; 2.9%), and Papua New Guinea or New Zealand (2; 1.2%). The women’s mean age (range) was 26.8 years (14.8–45.3 years). The parity of the women ranged from zero to 12. One-hundred and 30 women had an ultrasound for dating at or before 22 weeks’ gestation.
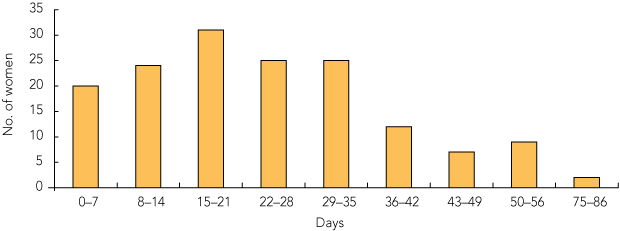
For 55 women (31.9%), the date of travel was known from accurate records. For the remainder, the date of the first antenatal appointment was used and their calculated length of stay is probably underestimated, as many women arrive in Cairns some days before their first appointment (Box 2).
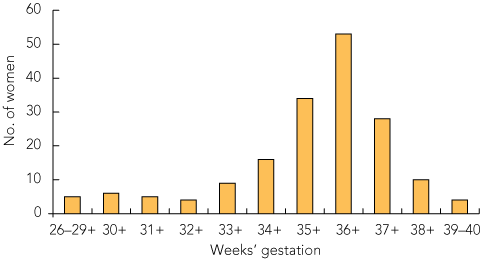
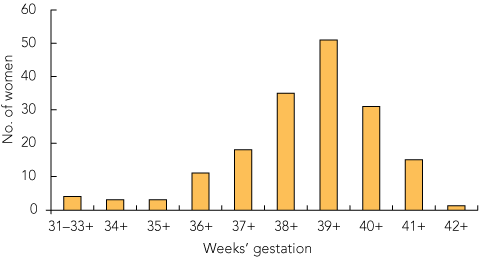
All transfers that occurred after 34 weeks were for routine care. The latest transfer occurred at 39 weeks and 3 days. Most women gave birth after 36 weeks, with the mode value in the 39th week (ie, between 39 weeks and 39 weeks and 6 days [51 women, 29.7%; Box 3]). Ten women (5.8%) gave birth before 36 weeks, 11 (6.4%) in the 36th week, 18 (10.5%) in the 37th week, 35 (20.3%) in the 38th week and 47 (27.3%) after 40 weeks (Box 3). The average length of stay in Cairns was 24 days (range, 0–86 days) (Box 4).
Most women (120/172; 69.8%) experienced normal vaginal births (Box 5). There were 27 emergency caesarean sections and 21 elective caesarean sections; the caesarean section rate was comparable to the background rate at CBH. There were very few instrumental deliveries (two forceps, one vacuum extraction). There were 11 births in the communities; six of these were before 36 weeks’ gestation. Four women were over 36 weeks’ gestation and had decided not to move to Cairns. The remaining woman had received no antenatal care, so gestational age at birth was unknown.
The wider issue is whether we are providing a satisfactory midwifery and obstetric service to the women in Cape York. There is much anecdotal evidence acquired from obstetric and midwifery practice in CBH, and in the available literature, which suggests that the model of care involving transfer of women to a regional centre in late pregnancy for women living in remote communities may not be acceptable to the women or their health care workers.4-6 It is postulated that this is the reason that some women avoid presenting for antenatal care, as this will ultimately separate them from their support network later in the pregnancy.4 Similar findings have been reported from studies in south-western Queensland, the Indian Ocean Territories, Canada and rural Scotland.7-10 Feelings of isolation and loneliness, poor social support and significant financial hardship have been reported among Queensland women giving birth preterm in units geographically distant from their homes.7
There is a paucity of published work regarding obstetric care in Far North Queensland. A 1989 study that reported high rates of preterm labour and pregnancy and labour complications among Indigenous women also noted that women appreciated the safety of transfer to Cairns for delivery.5
Although perinatal outcomes are improving, there is undoubtedly considerable social and psychological stress associated with moving to Cairns to give birth. Women who travel to Cairns must stay in hostels or with relatives. They are often separated from the rest of their families for prolonged periods (Box 6). Only women 16 years of age or younger can have an escort funded to accompany them for support during their antenatal stay and labour (CBH Patient Travel Office Manager, personal communication).11 There are anecdotal reports of financial hardship, particularly when the woman’s partner and family also stay in Cairns with limited financial support. Other concerns are the loss of customary cultural practices, decreased bonding with the father, and sibling jealousy due to the absence of the mother at this time.6
Midwives and GP–obstetricians face barriers if they wish to provide obstetric services in rural settings. These include constantly being on call and difficulty in maintaining skills.4 CBH trains four doctors in advanced general practice obstetrics each year, but the declining numbers of GPs or salaried doctors with obstetric skills have long been in evidence in the medical workforce.12 There are not enough new midwives in training, and the midwifery workforce is an “ageing population”.4 Little has been done to recruit or retain skilled doctors (either salaried doctors or private GPs) in these communities.
- Joanna L Arnold1
- Caroline M de Costa2
- Paul W Howat1
- 1 Cairns Base Hospital, Cairns, QLD.
- 2 Department of Obstetrics and Gynaecology, James Cook University, Cairns, QLD.
We thank Rose Hogan, James Cook University School of Medicine and Dentistry, and Lisa Gardiner, Clinical Benchmarking, CBH, for their assistance in preparing this study.
None identified.
- 1. Humphrey MD, Dudgeon M, Smith WJ. FROGS — the development of a specialist outreach service. Aust Health Rev 1993; 16: 268-272.
- 2. Queensland Council on Obstetric and Paediatric Morbidity and Mortality. Trends in maternal, perinatal and paediatric mortality in Queensland. Brisbane: Queensland Health, 1995.
- 3. Queensland Health. Health Statistics Centre Perinatal Statistics 2006. Perinatal deaths. http://www.health.qld.gov.au/hic/peri2006/Deaths.pdf (accessed Jun 2008).
- 4. Kildea S. Risk and childbirth in rural and remote Australia. 7th National Rural Health Conference; 2003 Mar 1–4; Hobart, Tas. http://nrha.ruralhealth.org.au/conferences/docs/7thNRHC/Papers/refereed%20IO%20papers/kildea.pdf (accessed Jun 2008).
- 5. Fitzpatrick J. Obstetric health services in Far North Queensland: is choice an option? Aust J Public Health 1995; 19: 580-588.
- 6. Kildea S. Risky business: contested knowledge over safe birthing services for Aboriginal women. Health Sociol Rev 2006; 15: 387-396.
- 7. Smith M, Askew DA. Choosing childbirth provider location — rural women’s perspectives. Rural Remote Health 2006; 6: 510. Epub 2006 Aug 23.
- 8. Roach SM, Downes S. Caring for Australia’s most remote communities — obstetric services in the Indian Ocean Territories. Rural Remote Health 2007; 7: 699. Epub 2007 Apr 11.
- 9. Kornelsen J, Grzybowski S. The reality of resistance — the experiences of rural parturient women. J Midwifery Womens Health 2006; 51: 260-265.
- 10. Pitchforth E, Watson V, Tucker J, et al. Models of intrapartum care and women’s trade-offs in remote and rural Scotland — a mixed-methods study. BJOG 2008; 115: 560-569.
- 11. Queensland Health. The patient travel subsidy scheme. Information for patients and their carers. http://www.health.qld.gov.au/services/community/ptss/www11399doc.pdf (accessed Apr 2009).
- 12. Innes K, Strasser RP. Why are general practitioners ceasing obstetrics [letter]? Med J Aust 1997; 166: 276-277.





Abstract
Objective: To determine whether the current planned transfer of pregnant women from Cape York communities to Cairns at 36 weeks’ gestation for birthing is medically appropriate.
Design and setting: Retrospective audit of travel details and demographic and obstetric outcome data on all women from Cape York communities who travelled to Cairns for late pregnancy care and birth at Cairns Base Hospital in 2006.
Main outcome measures: Length of stay in Cairns; gestational age at birth.
Results: In 2006, 172 women from 14 Cape communities travelled to Cairns to give birth. Of these, 76% identified as Aboriginal or Torres Strait Islander, 20% as Caucasian and 4% were from other ethnic groups. The mean time of stay in Cairns before birth (range) was 24 (0–86) days. Eleven women (6%) gave birth between 36 and 37 weeks of pregnancy; this point marked the beginning of a significant rise in births for increasing gestational ages.
Conclusion: Aiming for 36 weeks’ gestation for transfer is medically appropriate, but results in long periods of separation of women from Cape communities from family and friends, with detrimental social, cultural and financial consequences. Reopening maternity units in towns serving the Cape communities could reduce the number of women from the region having to travel to Cairns for pregnancy care and birth.