Dementia is the second greatest source of disability burden in Australia,1 with around 37 000 new diagnoses made each year.2 Early, accurate diagnosis of dementia has many benefits — treatable causes can be dealt with, interventions to slow progression can be implemented, and future planning can commence while the patient is still competent.3 Engagement of family and carers with support services and networks can reduce carer burden3 and in some cases delay institutionalisation.4
The time between onset of dementia symptoms and diagnosis is often prolonged, leading to years of uncertainty for patients and their families.5 Overseas studies have estimated the average time from first symptoms to diagnosis, as reported by informants, to be between 1 and 3 years,6,7 with symptoms recorded in general practitioners’ medical records as early as 5 years before diagnosis.8 Factors contributing to this delay include the insidious onset of the disease; under-recognition or uncertainty by families about the path to diagnosis; the stigma associated with dementia; and uncertainty about, a lack of knowledge about or a negative attitude to earlier diagnosis by health professionals.5,9,10
Identifying where diagnostic delays occur is one link in the chain towards timely diagnosis and support for patients and their carers. We aimed to describe the steps taken and delays encountered in the pathway to dementia diagnosis.
The survey was developed from the literature3,11 and included open and closed questions about the carer’s and patient’s demographic details; first dementia symptoms, actions, and consultations; diagnosis and use of any of a list of 22 resources (eg, support, respite and chronic illness services; medical services; advocacy organisations; and advisory services). Carers recorded the year these steps occurred.
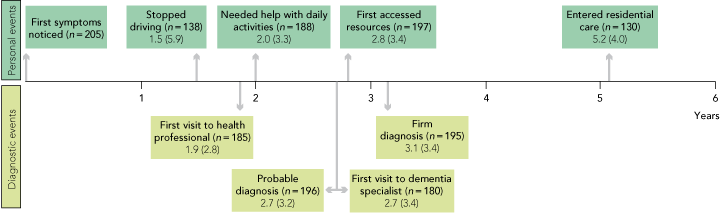
Mean intervals from the time first symptoms were noticed to personal and diagnostic events are shown in Box 1. The mean time reported by carers from first symptoms to a firm diagnosis was 3.1 years. At the time of the survey, a mean of 7.8 years (SD, 5.1 years) had elapsed since symptoms had first been noticed.
The most common first actions that carers or patients took after the onset of symptoms were consulting a health professional or service (64%) and increasing family support (15%); 18% took no immediate action (Box 2).
In most cases (84%), a GP was the first health professional patients saw about their symptoms; others saw a specialist (8%) or another health professional (8%). Most carers (64%) stated that a memory test was performed by the first health professional (Box 3).
The mean intervals from symptom onset to attending the first health professional about the symptoms (1.9 years), and receiving a firm diagnosis of dementia (3.1 years) are consistent with those found in overseas studies.6-8 The consequence of this delay is a lost opportunity for earlier medical and social interventions for patients and their families, and prolonged diagnostic uncertainty. The timeline we observed suggests that levels of daily functioning were substantially impaired well before a diagnosis was made or resources were used.
The first delay in the diagnosis of dementia occurred before seeing the first health professional. Some carers arranged support in the first instance rather than seeking medical advice, but in other cases, stigma and misinterpretation of symptoms contributed to the delay. Other studies have reported that carers may be uncertain about the significance of early symptoms or may gradually adapt to the changes.5,10
The second delay occurred after the first health professional was consulted. Some carers reported that the first health professional did not act on symptoms or perform a memory test, and, as in other studies,5,12,13 some carers reported that their concerns were dismissed or referral was delayed. In some cases, health professionals might not have considered dementia a likely diagnosis, may have been hesitant to suggest dementia as a possible diagnosis because of uncertainty or the stigma associated with the disease,9 or may have believed tests would not change patient management.14 Additionally, GPs might prefer a specialist to take on the responsibility of diagnosis and disclosure.9,15 The complexity of the consultation itself can also contribute, given the multiple diagnoses, comorbidities, agendas and social issues to consider.9
Community education about early symptoms and how and when to act on them could aid earlier recognition of symptoms and, possibly, earlier presentation to a health professional.5,16 Health professionals, especially GPs, need to be able to address the needs of patients presenting with possible dementia symptoms and their families with sensitivity and to accelerate diagnosis.5,9,15 Acknowledgement by the health professional that a problem exists, even if uncertainty surrounds the diagnosis in the early stages, might allow families earlier access to resources and information that can assist them in their caring roles.5,9 GPs may also wish to consider earlier referral to a dementia specialist. The Primary Dementia Collaborative Research Centre is currently investigating ways to improve dementia detection in primary care.17
1 Timeline of mean time (SD) in years for personal and diagnostic events on the pathway to dementia diagnosis
 | |||||||||||||||
2 First actions taken by carers or patients after the onset of possible dementia symptoms
- Catherine M Speechly1
- Charles Bridges-Webb2
- Erin Passmore3
- Projects, Research and Development Unit, NSW and ACT Faculty, Royal Australian College of General Practitioners, Sydney, NSW.
We thank the family members and carers for their detailed responses, AANSW staff, and the participating GPs and residential aged care facilities. We thank Julie Wang at the Burnet Institute for critically reviewing the manuscript.
This study was funded by the Family Medical Care, Education and Research Grant through the Royal Australian College of General Practitioners Research Foundation. The conduct of the study remained independent of the funding bodies at all stages.
- 1. Access Economics. The dementia epidemic: economic impact and positive solutions for Australia. Canberra: Alzheimer’s Australia, 2003. http://www.alzheimers.org.au/upload/EpidemicFullReportMarch2003.pdf (accessed Jun 2008).
- 2. Australian Institute of Health and Welfare. Dementia in Australia: national data analysis and development. Canberra: AIHW, 2006. (AIHW Cat. No. AGE 53.)
- 3. Bridges-Webb C, Wolk J, Pond D, Britt H. Care of patients with dementia in general practice: guidelines. Sydney: NSW Department of Health, 2003.
- 4. Mittelman MS, Haley WE, Clay OJ, Roth DL. Improving caregiver well-being delays nursing home placement of patients with Alzheimer disease. Neurology 2006; 67: 1592-1599.
- 5. Teel CS, Carson P. Family experiences in the journey through dementia diagnosis and care. J Fam Nurs 2003; 9: 38-58.
- 6. Cattel C, Gambassi G, Sgadari A, et al. Correlates of delayed referral for the diagnosis of dementia in an outpatient population. J Gerontol A Biol Sci Med Sci 2000; 55: M98-M102.
- 7. Fiske A, Gatz M, Aadnøy B, Pedersen NL. Assessing age of dementia onset: validity of informant reports. Alzheimer Dis Assoc Disord 2005; 19: 128-134.
- 8. Ramakers IH, Visser PJ, Aalten P, et al. Symptoms of preclinical dementia in general practice up to five years before dementia diagnosis. Dement Geriatr Cogn Disord 2007; 24: 300-306.
- 9. Iliffe S, Manthorpe J, Eden A. Sooner or later? Issues in the early diagnosis of dementia in general practice: a qualitative study. Fam Pract 2003; 20: 376-381.
- 10. De Lepeleire J, Heyman J, Buntinx F. The early diagnosis of dementia: triggers, early signs and luxating events. Fam Pract 1998; 15: 431-436.
- 11. Sano M, Devanand DP, Richards M, et al. A standardized technique for establishing onset and duration of symptoms of Alzheimer’s disease. Arch Neurol 1995; 52: 961-966.
- 12. Millard F. GP management of dementia — a consumer perspective. Aust Fam Physician 2008; 37: 89-92.
- 13. Downs M, Ariss SMB, Grant E, et al. Family carers’ accounts of general practice contacts for their relatives with early signs of dementia. Dementia 2006; 5: 353-373.
- 14. van Hout HP, Vernooij-Dassen MJ, Stalman WA. Diagnosing dementia with confidence by GPs. Fam Pract 2007; 24: 616-621.
- 15. Turner S, Iliffe S, Downs M, et al. General practitioners’ knowledge, confidence and attitudes in the diagnosis and management of dementia. Age Ageing 2004; 33: 461-467.
- 16. Werner P. Knowledge about symptoms of Alzheimer’s disease: correlates and relationship to help-seeking behavior. Int J Geriatr Psychiatry 2003; 18: 1029-1036.
- 17. Primary Dementia Collaborative Research Centre. The GP Study. Sydney: University of New South Wales, 2007. http://www.dementia.unsw.edu.au/DCRCweb.nsf/page/GPStudy (accessed Jun 2008).





Abstract
Objective: To describe the steps taken by health professionals to diagnose dementia and the timeframes for these steps, as reported by carers.
Design, setting and participants: A cross-sectional, anonymous survey was mailed or distributed by Alzheimer’s Australia New South Wales, six Sydney residential aged care facilities and 13 Sydney general practitioners to 415 carers or family members of patients with dementia between May and August 2007.
Main outcome measures: First symptoms noticed and actions taken; time to first health professional consultation and diagnosis; reported actions of first health professional; satisfaction with first consultation; and use of dementia and chronic illness resources.
Results: 209 surveys were returned. Family members noticed the first symptoms of dementia at a mean of 1.9 years before the first health professional consultation about dementia, and 3.1 years before a firm diagnosis. Resource use first occurred 2.8 years after the first symptoms. Most carers (72%) were satisfied with the first consultation, which was usually with a GP (84%). Two-thirds of carers (64%) reported that the first health professional had performed a memory test.
Conclusions: Delays in presentation, diagnosis and resource use may have clinical and social implications for people with dementia and their families, in addition to the challenges of the process of obtaining a firm diagnosis.